* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Surgical Management of Ischaemic Heart Disease
Survey
Document related concepts
Saturated fat and cardiovascular disease wikipedia , lookup
Cardiovascular disease wikipedia , lookup
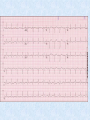
Electrocardiography wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Drug-eluting stent wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Cardiac surgery wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
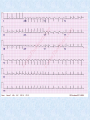
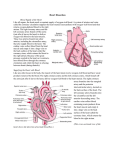
Surgical Management of Ischaemic Heart Disease By Dilshan Udayasiri HMO2 Introducing Mrs Anne Gina • You’re the intern working in Western Hospital ED. • 52yo female presents with Chest Pain. What do you do next!!!! History • Pain came on one hour ago on a background of having similar pain on exercise over the last 3 weeks. • Central and crushing • Radiates up the Jaw • Associated with SOB, palpitations, presyncope, diaphoresis. • Did not go away with rest, still present • WHAT DO YOU DO NEXT!! Management • • • • • • • • • • Obs sats 95%, BP 145/70, HR 100, afebrile ECG O2 15L via Hudson Mask 300mcg of anginine sublingually 300mg of asprin Monitored Bed 2 large bore cannula. Heparin infusion commenced Pain relieved. Bloods and CXR request sent, Cardiology registrar on the way Further History • PHx (Cardiac Risk factors) – – – – – Exsmoker (40 pack year history) Hypertension Hyperlipidaemia T2DM – diet controlled FHx – Father AMI 50 • SHX – Lives at home with Husband • Medications – Ramipril 2.5mg daily – Atorvastatin 20mg nocte • NKDA • Cardiology Registrar arrives. Is very Happy with your work. Takes the patient off for angiography. The Coronaries • 2 main coronary arteries – Right Coronary Artery (RCA) • Gives of a Posterior Descending artery branch in approx 70% of patients • 20% of patients the PDA comes of the left circumflex and are hence Left dominant • 10% PDA comes off both and are then Codominant. • Supplies 25% - 35% of the left ventricle and the SA node in 60% of cases (otherwise LCx artery) • Left Main coronary artery – Divides early into the • Left anterior descending artery – Supplies the anterolateral myocardium, interventricular septum and the apex of the heart. In total it supples 45%55% of the left ventricle. – Gives off septal (run straight into the intaventricular septum at 90degrees to surface, and diagonals that supply the lateral myocardium) • Left Circumflex – Gives off obtuse marginals (OMs) as it curves around the posterior aspect of the heart. – Supples the SA node in 40% of cases. If nonDominant supplies 15%-20% of LV, if dominant 40%-50%. Also supples anterolateral papillary muscles. Patients Angiography • LMCA – Short left main with ostial 90% stenosis • LAD – Medium calibre vessel with mild dease throughout • LCx – Medium calibre, non-dominant vessel with mild disease. OM1 is tortuous and mildly diseased. Small AV branch diffusely diseased distally. • RCA – Dominant. Small calibre vessel with diffuse disease proximally and totally occluded mid vessel. • Ventriculogram – Lv Function is severely impaired. There is no mitral regurgitation Some common indications for Coronary Artery Bypass Grafting • • • • • • • • • Left main artery disease or equivalent Triple vessel disease Abnormal Left Ventricular function. Failed PTCA. Immediately after Myocardial Infarction (to help perfusion of the viable myocardium). Life threatening arrhythmias caused by a previous myocardial infarction. Occlusion of grafts from previous CABGs. Coronary artery disease with valvular disease Angina not controlled by maximal medical therapy Pt arrives at RMH PAC • Note History – Meds are now • • • • • Ramipril 2.5mg daily Atorvastatin 20mg nocte Metoprolol 25mg BD Asprin 100mg daily GTN spray 400mcg PRN O/E • Comfortable, no chest pain • Obs, BP 140/75, HR 80, sats 98%RA, afeb • Pulse: ulna and radial present bilaterally, strong and regular • Allens test – negative bilaterally • No carotid Bruits • No previous scars on chest. Heart sounds are dual with no added sounds. Chest sounds are vesicular. • Lower limb pulses are present. No varicose veins • Right Handed What do you want to do before the operation? • Consent patient for surgery • Optimise medical management – increase metoprolol to 50mg BD • W/H asprin 7/7 prior to surg • Tests – – – – TTE CXR Bloods (FBE, UEC, Ca/Mg/Phos, Coags, G&S) Carotid U/S not required Complications of CABGs • • • • • • • Bleeding Infection Stroke AMI Arrythmias Postperfusion syndrome (pumphead) Sternal dehiscence Graft Patency Rates Conduit 5 year 10 year left internal thoracic artery 96% 95% right internal thoracic artery 93% 90% Radial artery 90% 80% Saphenous vein 75% 50% In Theatre • Pt prepared by anaesthetics (peripheral lines, CVC, arterial lines inserted.) • Once anaesthetised, TOE inserted. • Body prepped. • Conduits harvested • Heparin commenced • Chest opened and canulated ready for bypass. • Aorta clamped and cardioplegia started to stop heart. • Anastomosis performed. • Drains and pacing wires inserted • Cardioplegia ceased pt taken off bypass • T/fed to ICU Post Op • Pt extubated day 1. Weaned off ionotropes and t/fed to ward. • First few days post op need to – – – – Continuous cardiac monitoring. Monitor drain outputs Daily bloods + ECGs + CXR + weight Pt normally commenced on frusemide + iv Abs + nebulisers on top of normal meds. – On day 3 post op you are paged by the nurse stating the patient is tachycardic rate 160, (BP 130/75, sats 95% 2L, no CP) – ECG is as follows ECG What would you do • Send off bloods • Think of and treat reversible causes – Electrolytes – Ischaemia – Hyperthyriodsim • Rate vs Rhythm control