* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Nosocomial Respiratory Syncytial Virus Infections: The “Cold War
2015–16 Zika virus epidemic wikipedia , lookup
Orthohantavirus wikipedia , lookup
Clostridium difficile infection wikipedia , lookup
Sarcocystis wikipedia , lookup
Cryptosporidiosis wikipedia , lookup
Herpes simplex wikipedia , lookup
Ebola virus disease wikipedia , lookup
Anaerobic infection wikipedia , lookup
Trichinosis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
Carbapenem-resistant enterobacteriaceae wikipedia , lookup
Antiviral drug wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
West Nile fever wikipedia , lookup
Hepatitis C wikipedia , lookup
Herpes simplex virus wikipedia , lookup
Oesophagostomum wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Marburg virus disease wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Henipavirus wikipedia , lookup
Hepatitis B wikipedia , lookup
Lymphocytic choriomeningitis wikipedia , lookup
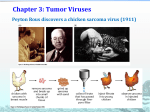
590 SPECIAL SECTION: HEALTHCARE EPIDEMIOLOGY Robert A. Weinstein, Section Editor Nosocomial Respiratory Syncytial Virus Infections: The “Cold War” Has Not Ended Caroline Breese Hall Departments of Pediatrics and Medicine, University of Rochester School of Medicine and Dentistry, Rochester, New York Respiratory syncytial virus (RSV) is a major nosocomial hazard on pediatric wards during its annual outbreaks. It produces significant morbidity in young children and is most severe in those with underlying conditions, especially cardiopulmonary and immunosuppressive diseases. In older patients, RSV may exacerbate an underlying condition or pulmonary and cardiac manifestations. On transplant units, of RSV may be occult and is associated with high mortality rates. The manifestations of nosocomial RSV infections may be atypical, especially in neonates and immunosuppressed patients, resulting in delayed or missed diagnosis and adding appreciably to the costs of hospitalization. RSV is primarily spread by close contact with infectious secretions, either by large-particle aerosols or by fomites and subsequent selfinoculation, and medical staff are often instrumental in its transmission. Thus, integral to any infection control program is the education of personnel about the modes of transmission, the manifestations, and the importance of RSV nosocomial infections. Hand washing is probably the most important infection control procedure. The choice of barrier controls should be decided by individual institutions depending on the patients, the type of ward, and the benefit relative to cost. In days of old the scourge of colds was thought a wen Of evil humors wrought on hands by sins of men. A curse for acts we should have done they still may be, But more, they teach both lords and serfs all risk this fee. The morbidity engendered by respiratory syncytial virus (RSV) infections has been recognized now for decades but not necessarily appreciated. Perhaps the first published description of nosocomial RSV infections was that of Adams [1], who in 1937 identified outbreaks of pneumonia in the nurseries of 2 Minneapolis hospitals. Thirty-two infants, mostly aged 4–12 weeks, developed pneumonia, and 28% died. All of the infants who died had cytoplasmic inclusions in the bronchial epithelium. These findings and the distinctive epidemiology and clinReceived 1 May 2000; revised 22 May 2000; electronically published 14 September 2000. Financial support: This study was supported by grants from the National Institutes of Health (AI-45248 and RR-00044). Publication of the Special Section on Healthcare Epidemiology has been made possible by an educational grant from Pfizer Pharmaceuticals Group, Pfizer, Inc. Reprints or correspondence: Dr. Caroline Breese Hall, University of Rochester Medical Center, 601 Elmwood Ave., Box 689, Rochester, NY 14642 ([email protected]). Clinical Infectious Diseases 2000; 31:590–6 q 2000 by the Infectious Diseases Society of America. All rights reserved. 1058-4838/2000/3102-0033$03.00 ical presentation of the outbreaks led Adams to suggest that they were caused by a virus. Two decades later, Adams et al. [2] studied a markedly similar outbreak of illness in infants and were able to identify it as being caused by the newly discovered RSV. Comparing this to the carefully documented clinical and pathological findings in the earlier nursery outbreaks led Adams to propose that the agent of both was the “chimps coryza agent,” later rechristened RSV. Epidemiological and Clinical Characteristics of Nosocomial RSV Infection Impact of Nosocomial RSV Infections In the decades since the study of Adams et al. [2], RSV has been shown during its yearly appearance to be a major nosocomial hazard for patients of all ages. On pediatric wards, RSV has been the most frequent cause of nosocomial infection [3–5]. The resulting morbidity and costs have been striking, especially in infants. About 40% of nosocomial RSV infections are associated with lower respiratory tract disease in this young age group. Risk factors for acquiring RSV infection while hospitalized during the often-prolonged RSV season, in addition to young age, also include underlying or chronic disease, long hospitalization, and crowded, busy wards. Increases in the duration and costs of hospitalization have been significantly correlated with the nosocomial acquisition of RSV infection. CID 2000;31 (August) Nosocomial RSV Infections Clinical Findings in Populations at Risk Neonates. Nosocomial outbreaks of RSV in neonatal intensive care units, as illustrated by those described by Adams [1], may be particularly severe, with unexpected clinical manifestations and a high mortality [6–8]. The potential severity may be aggravated in neonatal units by the difficulty of recognizing an outbreak from an infectious agent or RSV specifically. In neonates, RSV infection is frequently atypical in its presentation, manifest as nonspecific, nonrespiratory signs that premature infants develop characteristically from multiple causes, such as apnea, bradycardia, and changes in feeding and ventilation. Medical personnel. RSV infections in medical staff, both community-acquired and nosocomially acquired, also frequently are not recognized, because they may be mild or manifest as “colds” or flu-like illnesses. More than 50% of staff on pediatric wards have been shown to become infected with RSV during periods when RSV is prevalent in the community. Acquisition of RSV infections by medical personnel is of particular concern. Because the infection lacks distinctive signs and initially sometimes lacks severity, its importance may not be recognized, and staff may become effective but occult vectors for transmission on the ward. Furthermore, RSV infection may result in ∼40% of those infected being absent from work during one of the busiest seasons on hospital wards [9]. Although the great majority of RSV infections in staff are symptomatic, asymptomatic infection accompanied by appreciable shedding of RSV in respiratory secretions occurs in 15%–20% of infected personnel. Medical students and staff new to pediatric wards are at highest risk of acquiring symptomatic RSV infection and may be least likely to recognize the etiology or significance of their respiratory illness. Older adults with underlying conditions. Nosocomial infections from RSV, once thought to be mainly a problem on pediatric wards, are now being recognized on units that house patients of all ages and are of particular concern for the elderly and patients with underlying cardiopulmonary and immunosuppressed conditions. Among the institutionalized populations of older adults, RSV has been shown to be the most commonly identified viral pathogen associated with respiratory illness, accounting for 27% of such illnesses [10]. Furthermore, in these groups, RSV-associated illness resulted in significantly greater morbidity than did infections with other agents, such as rhinovirus. Children with underlying conditions. As in the population at the other end of the age spectrum, in neonates in intensive care units the recognition and diagnosis of RSV infection is problematic. Frequently it presents primarily as cardiac or pulmonary decompensation or as a mimic of influenza [11–13]. Similarly, children with underlying cardiopulmonary disease, especially those with uncorrected congenital heart disease, may have predominantly cardiac or pulmonary manifestations and 591 are at particularly high risk for subsequent complications [14–16]. Immunocompromised patients. Of increasing recent interest and importance is RSV’s potential to become an opportunistic pathogen in immunocompromised patients [17, 18]. A 3-year survey of adult cancer patients with respiratory infection at the M. D. Anderson Cancer Center in Houston identified a respiratory virus in 27%–33% of the illnesses [18]. RSV was the most frequently isolated agent, accounting for 31% of the infections. About one-half to three-fourths of these infections were nosocomially acquired. Characteristically a nosocomial outbreak of RSV on a transplant unit is initiated by RSV being introduced unrecognized onto the ward by family members or medical personnel with upper respiratory tract infections, followed by the initially occult spread among the immunocompromised patients. Circulation of RSV tends to continue for prolonged periods on these units, even when RSV is no longer present in the community. In part this may relate to the long duration of shedding of RSV usually observed with immunocompromised patients. In these patients, both the amount and length of shedding appear to correlate with the degree of immunosuppression. In a prospective study of hospitalized immunocompromised children, those receiving corticosteroid therapy alone had no worse clinical manifestations of RSV infection than did control subjects. Shedding, however, was significantly more in quantity and longer in duration, up to 3 weeks [19]. In those with greater degrees of immunosuppression, larger quantities of virus were shed, and the duration of shedding was documented for up to 47 days. Of further concern is the observation that the shedding in these patients may be detected only intermittently and may not be associated with the presence of respiratory tract signs or symptoms. The diagnosis of RSV infection and the initiation of control measures are frequently delayed for these populations, because the presenting signs accompanying RSV infection are often indistinguishable from those caused by opportunistic pathogens that are more classically associated with the immunocompromised host. Yet it is important to be constantly aware of the possibility of RSV infection; the reported mortality due to RSV infection on transplant units is 20%–100% [18]. Characteristics of RSV that Augment the Chance of Nosocomial Transmission RSV’s considerable capability to become a major cause of nosocomial infection arises from several of its singular characteristics. First, RSV’s epidemiological pattern underscores its ubiquity and the speed that it spreads: outbreaks of RSV infection occur every year and spread throughout the country. Second, persons of all ages, both healthy and with underlying conditions, are potentially susceptible to RSV infection. In contrast to most bacterial agents that cause nosocomial illness, nosocomial RSV infections are not observed primarily in patients with chronic or 592 compromising conditions. Immunity to RSV is incomplete, resulting in repeated infections throughout life, often within short intervals, even weeks or months [20, 21]. Third, the shedding of RSV in the respiratory secretions of young children tends to be for long periods and at high titer. Even adults shed appreciable quantities of virus for 3 to >7 days [6, 9, 22]. Fourth, RSV in secretions may remain contagious in the environment for periods long enough for inadvertent transmission on hands and fomites [23] (figure 1). Secretions from young children frequently contaminate the objects surrounding their beds, such as crib railings, table tops, and toys, and may remain viable and contagious for hours, depending on the type of surface, environmental temperature, and humidity. The usual winter conditions on a ward of low humidity enhances the duration of RSV’s viability, allowing it to survive on nonporous surfaces for 6–12 h or more. Furthermore, hand contact with these contaminated surfaces has been shown to result in transfer of viable, infectious virus to the skin [23]. Possible Modes of Spread of RSV Respiratory viruses may be transmitted by any of 3 possible mechanisms. The first is transmission by small-particle aerosols (!10 mm mass median diameter), usually generated by coughing or sneezing, which may traverse distances >1.8 m. Transmission by small-particle aerosols, therefore, does not require close or direct contact with the infected subject or with infectious se- Hall CID 2000;31 (August) cretions. Typically, viruses spread by small-particle aerosols cause explosive outbreaks of infection in a susceptible population, such as occur with measles, varicella, and sometimes influenza. The second mechanism is transmission by droplets or large particles. In contrast to aerosols of small particles, aerosols of large particles require close person-to-person contact, usually at a distance of <0.9 m, for infection to occur. Third, the virus can also be transmitted via fomites; that is, by self-inoculation after touching contaminated surfaces. For this to occur, the virus must be able to remain infectious on environmental surfaces, to be transferred to the skin, and to remain infectious for a time sufficient to allow self-inoculation into the respiratory tract. Studies have indicated that RSV is primarily transmitted by the latter 2 methods, both of which require close contact with contagious secretions [24]. In one study, young adult volunteers working on a pediatric ward were exposed in 3 different manners to infants with RSV infection. The first group, called “cuddlers,” were exposed to an infected infant by caring for the baby 2–4 h in the usual manner, including feeding, diaper changing, and playing with the infant. These staff wore gowns but no mask or gloves. The second group, called “touchers,” touched with ungloved hand surfaces likely to be contaminated with the baby’s secretions when the infant was out of the room. They then gently rubbed the mucous membranes of their nose or eye, mimicking the manner in which we all unconsciously rub our eyes or nose. The most effective portals of inoculation Figure 1. Modes of nosocomial spread of respiratory syncytial virus. Dashed lines, routes of transmission most likely to be interrupted by infection control; solid lines, routes of transmission unlikely to be affected appreciably by infection control procedures. CID 2000;31 (August) Nosocomial RSV Infections for RSV have been shown experimentally to be the nose and eyes, in contrast to the mouth, which is a relatively insensitive site for inoculation [25]. The third group, called “sitters,” was exposed to an infected baby by sitting at a distance of 11.8 m from the bed. They wore gowns and gloves, but no masks, and were allowed to touch only the book they were reading. Cuddlers, therefore, could potentially acquire RSV infection by any of the 3 routes, whereas touchers could become infected only by means of fomites and self-inoculation, and sitters only by small-particle aerosols. Only the cuddlers and touchers became infected, which suggests that routes that require close or direct contact with infectious secretions and self-inoculation were the major or most effective means of transmission. RSV RNA has been detected by PCR-based methods in air samples from the rooms of infected patients at distances as far as 7 m from the patient’s bed and for up to 7 days of hospitalization [26]. This suggests that small-article aerosol transmission may be possible but is less efficient than the other routes, considering the lack of infection in the “sitters” [24]. The RSV detected by polymerase chain reaction in air samples may be largely noninfectious virus. Controlling the Spread of RSV How then should we control the spread of nosocomial RSV infections? First, and probably most importantly, all staff must understand that they need to be aware of RSV’s capricious character and covert circulation. Key to any infection control program is compliance, which will not be forthcoming unless staff understand that the imposed infection control procedures are important for their patients’ and their own health. Educational sessions at the beginning of each RSV season are usually helpful. Many studies, however, indicate that compliance tends to dwindle with time, even over one season, suggesting the need for educational updates. Second, surveillance and suspicion of RSV’s presence are important. Detecting the arrival and disappearance of RSV by community surveillance will define and limit the time that the special RSV infection control procedures need to be used. Educational programs should be initiated before the expected RSV season and the infection control procedures implemented when RSV is first detected in the community or when the first RSV admission occurs and the number of infant cases of bronchiolitis and pneumonia begin to rise. For communities that do not have their own virus surveillance system, the Centers for Disease Control and Prevention (CDC) now monitors RSV activity around the country on a weekly basis; reports are available on their Web site (http://www.cdc.gov/). Without this knowledge of RSV’s activity in the community, determining when RSV infection control procedures can be discontinued is difficult. Continuation for ∼2 weeks after the last infant admission for RSV or when the number of bronchiolitis admissions has returned to baseline may be a reasonable guideline. In units with 593 immunocompromised patients in whom RSV infection has been documented, precautions should be discontinued only after repeatedly negative cultures spaced over >2 weeks, and vigilance should be reinstated during periods of enhanced immunosuppression. The current availability of simple, rapid tests for RSV antigen has allowed most institutions a means of more specifically diagnosing patients with respiratory illness during the RSV season and may help define the duration of the community outbreak of RSV. These tests also have been beneficial in determining which patients need to be isolated. However, several caveats should be kept in mind. First, these are generally screening tests that may miss an appreciable proportion of infections. Their sensitivity and specificity tend to vary according to the quality of the specimen, the individual product, and the laboratory, and their positive predictive value markedly declines when the prevalence of RSV in the community is very low [27]. The third method to control the spread of nosocomial RSV infections is planning and implementation of control measures that are both effective and feasible. To have effective measures that are also feasible is often problematic and necessitates some degree of variability among individual institutions. The CDC advises the use of contact precautions, in addition to standard precautions, for RSV infections (table 1) [28]. Contact precautions are recommended for microorganisms that can be spread by direct patient contact (as occurs during care procedures that involve touching the dry skin of the patient) or by indirect contact, that is, touching surfaces or items in the patient’s environment that may be contaminated [28]. They class the evidence for these recommendations as “category I-B,” which is based “on strong rationale and suggestive evidence” and is strongly recommended and “reviewed as effective by experts in the field” [28]. Included are recommendations to wash hands, to wear gloves, masks, eye protection, and gowns, and to house patients infected with RSV in private rooms or in a cohort isolated from other patients (table 1). Studies evaluating the smorgasbord of possible infection control procedures are confusing and often conflicting [28]. The differing reported efficacy and permutations of procedures available make it difficult, if not impossible, to conclude that a single combination of procedures is most effective and evidence-based. The possible exception to this is hand washing. Hand washing. Most experts concur that hand washing is central to any infection control program, and the CDC also labels hand washing as category I-B [28]. However, no methods have been developed to ensure continued compliance with hand washing or to monitor how effectively and assiduously hospital staff wash their hands. Important in promoting frequent and effective hand washing are the convenience and number of sinks, the acceptability of the soap or cleansing agent and towels, and their accessibility. For these reasons, the newer alcoholbased hand rub agents, which do not require a sink and water, may be useful [29]. Although studies have not examined the 594 Hall CID 2000;31 (August) Table 1. Infection control procedures, both standard precautions and contact precautions, for prevention of respiratory syncytial virus (RSV) infection. Recommendation category, procedure Comment(s) a Category I-B recommendations Hand washing b Wearing gloves b Wearing gowns b Wearing masks plus eye protection Housing patients in private rooms or in a cohort isolated b from other patients Use of dedicated patient-care equipment Sometimes recommended with less or no supporting evidence Staff assigned according to patient’s RSV status b Visitor restrictions during RSV season Screening visitors for illness during RSV season Water with soap or antibacterial agent or waterless antiseptic hand rub Combined with hand washing before and after each glove change; may diminish self-inoculation When direct contact with patient or patient secretions is likely Eyes and nose are major sites for inoculation Patients with documented infection can be grouped and isolated from other patients; beds should be separated by 10.9 m Equipment, including toys, assigned to specific patients Specific staff care only for patients with RSV infection Some qualify by restricting young children only Visitors assessed by trained personnel and/or advised by use of an educational patient information sheet a Centers for Disease Control and Prevention recommendations based “on strong rationale and suggestive evidence” and strongly recommended and “reviewed as effective by experts in the field” [28]. b See text for further qualifications and alternatives. comparative efficacy of these products for RSV, experiments in our laboratory have shown RSV to be a labile virus that is quickly rendered noninfectious by a variety of agents, including alcohol and mild soaps with water [23]. Gloves. The use of gloves along with gowns has been shown to reduce the rate of nosocomial RSV infections [30]. However, gloves should be changed and the hands washed between tasks involving the same patient, as well as between patients [28]. Bacterial contamination on the hands of gloved personnel has been demonstrated [29, 31], and RSV survives on gloves for longer than on the skin of the hands [23]. Nevertheless, gloves may be effective in the control of RSV because few persons will pick their noses or rub their eyes while gloved, and therefore the chance for self-inoculation is diminished. Gowns. The use of gowns is advisable if the staff member is to have direct contact with the infected patient such that contamination of clothing with patient secretions is likely, on the basis of evidence that RSV in secretions on clothing may remain infectious for 1 h [23]. The expense associated with gown use can be considerable; it can be diminished by not requiring the use of gowns by all persons entering the room but only by those who have intimate contact with the patient, and also sometimes by allowing the reuse of a gown kept by the patient’s bedside. Of note, but unexplained, is the finding that no particular isolation policy in a multivariate model was associated with a decreased rate of RSV nosocomial infections in 9 Canadian pediatric hospitals, but gowning to enter the room was actually associated with an increased risk of RSV transmission [5]. Masks. It has not been clearly shown that wearing masks has any additional benefit. Most studies use of masks do so as part of multiple infection control procedures, not allowing delineation of any additional possible benefit from masks alone. However, masks without eye protection may offer only limited protection, given that the eyes are also effective portals of inoculation for RSV. Therefore masks, if appropriately used, may act as a barrier for 1 of the 2 most effective sites for inoculation of RSV. The use of eye-nose goggles has been shown to be beneficial [32]. Their use, however, may be limited by acceptability and additional expense, and much of their benefit could probably be achieved by strict hand washing. Isolation of patients. If feasible, patients with acute respiratory illness should be isolated during the RSV and influenza seasons until the etiology of the illness is determined. The use of rapid detection assays has been helpful in determining which patients may be housed together. However, during the busy RSV season, when pediatric wards tend to be overcrowded, there may not be enough single bedrooms available. Several observations suggest that isolation may not be essential. First, RSV is primarily spread by close or direct contact; that is, largeparticle aerosols and fomites. Because large-particle aerosols traverse distances of only 0.9 m, spacing beds by 10.9 m should prevent transmission by this route from patient to patient. Fomite-mediated transmission is probably controlled more effectively by strict hand washing and by education of staff and family members than by separating patients. A study by Wenzel et al. [33] questions whether single bedrooms are required for children with respiratory virus infections. They demonstrated that for a patient in a multibed room, the risk of becoming infected with a virus shed by a roommate was only 3%. Thus, when single-bed rooms are limited, it may be best to reserve them for patients with underlying conditions that put them at high risk for severe or complicated RSV infection. Assignment of personnel and equipment to specific patients. Assigning staff to care only for patients with or without RSV infection theoretically should limit the chance of staff acting as vectors of transmission of RSV from an infected to an uninfected patient by contamination of their hands from fomites. This policy, however, is unlikely to be feasible, and any additional benefit it may offer could be equaled by emphasizing strict hand washing. Transmission of RSV by infected person- CID 2000;31 (August) Nosocomial RSV Infections nel, even those with mild respiratory symptoms, however, is of concern. Ward personnel manifesting any respiratory symptoms should be reminded about the need for hand washing and good infection control procedures and, if possible, should avoid caring for high-risk patients. Equipment for patient care, including toys, should be assigned to use by individual patients. All reusable equipment should not be used for another patient until it is properly cleaned, even if the other patient is also infected and staying in the same room. Visitor restrictions. Family and other visitors during the RSV season frequently are infected with RSV and may transmit it to uninfected patients. Studies analyzing the antigenic and genomic diversity among isolates of RSV obtained during nosocomial outbreaks have shown that multiple strains tend to circulate during a single outbreak [34, 35]. A number of policies have been devised to guard against this possibility of visitors introducing RSV onto a ward. Some prohibit all young children from visiting during the RSV season. The relative benefit of this prohibition must be considered in each institution. In addition, such a policy does not recognize the frequent RSV infections that occur in older children and adults. One-third or more of the adult family members of a child infected with RSV may acquire the infection, and ∼15% of these infections are asymptomatic. Screening of visitors for acute respiratory symptoms, if feasible, may prevent some possible infections being transmitted, but many factors, such as the duration of symptoms and the accuracy and quality of the screening, make the effectiveness of this procedure variable. A reasonable policy, nevertheless, is to educate family members at the time of the patient’s admission about the risks visiting when ill and the importance of limiting their visit, especially if they bring young children. Precautions against introduction of infection by visitors, however, must be much more stringent on transplant units and other wards that house high-risk patients for whom the potential benefit of avoiding devastating nosocomial infection outweighs the extra educational and monitoring efforts of the staff. Other means of controlling RSV in the hospital. There is currently no vaccine or generally feasible and effective means of prevention of RSV infection in or out of the hospital setting. The first means of prophylaxis for some high-risk infants only became available in 1996, when high-titer polyclonal immunoglobulin to RSV (RespiGam; MedImmune, Gaithersburg, MD) was licensed. This is approved only for high-risk premature infants and requires monthly iv administration [36]. The subsequent licensing of a humanized monoclonal antibody, palivizumab (Synagis; MedImmune), has offered the advantages of monthly im administration, which has fewer adverse effects and can be used for outpatients [36]. This product was produced from a mouse monoclonal antibody that recognizes a protective epitope of the immunologically important surface glycoprotein, the F protein. However, these products are approved for prophylaxis only for the small group of premature infants who are 595 !36 weeks’ gestational age and/or have chronic lung disease and still require medical therapy. The pivotal multicenter trial that led to approval for monthly prophylaxis for these highrisk infants was a placebo-controlled trial of 1502 premature infants, which demonstrated that the rate of subsequent hospitalization for RSV illness was 10.6% in the placebo group and 4.8% in the infants receiving prophylaxis, which was a 55% reduction in the rate of hospitalization [37]. The product is not approved for use in other groups, and the American Academy of Pediatrics advises against using it to prevent nosocomial RSV infection, preferring other traditional infection control procedures [36]. Furthermore, the effectiveness of this product as prophylaxis in other groups of patients or in other settings has not been adequately evaluated, and the significant expense, even for small infants, prohibits widespread use. Polyclonal RSV immunoglobulin has been evaluated in a relatively small group of infants as therapy and has not been shown to be of clear benefit. High-titer polyclonal immunoglobulin to RSV with or without ribavirin has also been suggested as prophylaxis for hospitalized patients beyond infancy who are at high risk for severe or complicated RSV infection, especially transplant recipients [19, 38]. No controlled studies, however, are yet available to support this use. Summary Although 60 years have elapsed since the Adams’ [1] initial description of a nosocomial outbreak of pneumonia among infants due to a virus that was subsequently identified as RSV, no truly effective means exists to control the capricious circulation of RSV in the hospital environment. The difficulty in evaluating and quantitating the benefit of any one or multiple infection control procedures does not allow recommendation of a single set of procedures from the array of available interventions. Based on many years of studies, we know that each has potential advantages and disadvantages and that each institution must judge which procedures are best to use based on their relative benefit, cost, feasibility, and acceptability. Nevertheless, an infection control policy to curb the spread of RSV is advisable, indeed essential, if we are to diminish the appreciable morbidity and mortality now recognized to be associated with nosocomial RSV infection in high-risk patients. Of prime importance is that each institution be prepared. Whatever prevention program an institution adopts, it needs to be fully developed and ready for implementation as soon as surveillance data indicate RSV’s annual arrival in the community. Central to any such program is the education and reeducation of all staff about the characteristics, transmission, and risk of nosocomial RSV infection for patients and for themselves, because compliance depends on it. The choice of which infection control procedures to use is best based on understanding the mechanisms by which RSV spreads. Good hand washing is probably the single most important procedure. 596 Hall CID 2000;31 (August) References 1. Adams J. Primary virus pneumonitis with cytoplasmic inclusion bodies; a study of an epidemic involving thirty-two infants with nine deaths. JAMA 1941; 116:925–33. 2. Adams J, Imagawa D, Zike K. Epidemic bronchiolitis and pneumonia related to respiratory syncytial virus. JAMA 1961; 176:1037–9. 3. Hall C, Douglas RJ, Geiman J, et al. Nosocomial respiratory syncytial virus infections. N Engl J Med 1975; 293:1343–6. 4. Hall C. The nosocomial spread of respiratory syncytial virus infections. Annu Rev Med 1983; 34:311–9. 5. Langley J, LeBlanc J, Wang E, et al. Nosocomial respiratory syncytial virus infection in Canadian pediatric hospitals: a pediatric investigators collaborative network on infections in Canada study. Pediatrics 1997; 100:943–6. 6. Hall C, Kopelman A, Douglas RJ. Neonatal respiratory syncytial viral infections. N Engl J Med 1979; 300:393–6. 7. Forster J, Schumacher R. The clinical picture presented by premature neonates infected with the respiratory syncytial virus. Eur J Pediatr 1995; 154:901–5. 8. Gouyon J, Pothier P, Guignier F, et al. Outbreak of respiratory syncytial virus in France. Eur J Clin Microbiol 1985; 4:415–6. 9. Hall C, Geiman J, Douglas RJ, et al. Control of nosocomial respiratory syncytial viral infections. Pediatrics 1978; 62:728–31. 10. Falsey AR, Treanor JJ, Betts RF, Walsh EE. Viral respiratory infections in the institutionalized elderly: clinical and epidemiologic findings. J Am Geriatr Soc 1992; 40:115–9. 11. Falsey AR, Cunningham CK, Barker WH, et al. Respiratory syncytial virus and influenza A infections in the hospitalized elderly. J Infect Dis 1995; 172:389–94. 12. Guidry GG, Black-Payne CA, Payne DK, Jamison RM, George RB, Bocchini JA Jr. Respiratory syncytial virus infection among intubated adults in a university medical intensive care unit. Chest 1991; 100:1377–84. 13. Walsh E, Falsey A, Hennessey P. Respiratory syncytial virus and other virus infections in persons with chronic cardiopulmonary disease. Am J Respir Crit Care Med 1999; 160:791–5. 14. MacDonald N, Wolfish N, McLaine P, et al. Role of respiratory viruses in exacerbations of primary nephrotic syndrome. J Pediatr 1986; 108:378–82. 15. Isaacs D, Dickson H, O’Callaghan C, et al. Handwashing and cohorting in prevention of hospital acquired infections with respiratory syncytial virus. Arch Dis Child 1991; 66:227–31. 16. Mahant S, Robinson F, Wang E. Hospital morbidity in patients with RSV lower respiratory illness (LRI) and underlying heart disease: analysis of PICNIC RSV database. Pediatr Res 1997; 41:78A. 17. Harrington RD, Hooton TM, Hackman RC, et al. An outbreak of respiratory syncytial virus in a bone marrow transplant center. J Infect Dis 1992; 165: 987–93. 18. Couch R, Englund J, Whimbey E. Respiratory viral infections in immunocompetent and immunocompromised persons. Am J Med 1997; 102:2–9. 19. Hall CB, Powell KR, MacDonald NE, et al. Respiratory syncytial viral 20. 21. 22. 23. 24. 25. 26. 27. 28. 29. 30. 31. 32. 33. 34. 35. 36. 37. 38. infection in children with compromised immune function. N Engl J Med 1986; 315:77–80. Hall C, Walsh E, Long C, et al. Immunity to and frequency of reinfection with respiratory syncytial virus. J Infect Dis 1991; 163:693–8. Henderson F, Collier A, Clyde WJ, et al. Respiratory syncytial virus infections, reinfections and immunity. N Engl J Med 1979; 300:530–4. Hall C, Douglas RJ, Geiman J. Respiratory syncytial virus infections in infants: quantitation and duration of shedding. J Pediatr 1976; 89:11–5. Hall C, Geiman J, Douglas RJ. Possible transmission by fomites of respiratory syncytial virus. J Infect Dis 1980; 141:98–102. Hall C, Douglas RJ. Modes of transmission of respiratory syncytial virus. J Pediatr 1981; 99:100–3. Hall C, Douglas RJ, Schnabel K, et al. Infectivity of respiratory syncytial virus by various routes of inoculation. Infect Immun 1981; 33:779–83. Aintablian N, Walpita P, Sawyer M. Detection of Bordetella pertussis and respiratory syncytial virus in air samples from hospital rooms. Infect Control Hosp Epidemiol 1998; 19:918–23. Kellogg JA. Culture vs. direct antigen assays for detection of microbial pathogens from lower respiratory tract specimens suspected of containing respiratory syncytial virus. Arch Pathol Lab Med 1991; 451–8. Garner JS. Guidelines for isolation precautions in hospitals. Infect Control Hosp Epidemiol 1996; 17:53–80. Larson EL. APIC guideline for hand washing and hand antisepsis in health care settings. Am J Infect Control 1995; 23:251–69. Leclair J, Freeman J, Sullivan B, et al. Prevention of nosocomial respiratory syncytial virus infections through compliance with glove and gown isolation precautions. N Engl J Med 1987; 317:329–34. Olsen RJ, Lynch P, Coyle MB, Cummings J, Bokete T, Stamm WE. Examination gloves as barriers to hand contamination in clinical practice. JAMA 1993; 270:350–3. Gala C, Hall C, Schnabel K, et al. The use of eye-nose goggles to control nosocomial respiratory syncytial virus infection. JAMA 1986; 256:2706–8. Wenzel R, Deal E, Hendley J. Hospital-acquired viral respiratory illness on a pediatric ward. Pediatrics 1977; 60:367–371. Storch GA, Hall CB, Anderson LJ, Park CS, Dohner DE. Antigenic and nucleic acid analysis of nosocomial isolates of respiratory syncytial virus. J Infect Dis 1993; 167:562–6. Mazzulli T, Peret T, McGeer A, et al. Molecular characterization of a nosocomial outbreak of human respiratory syncytial virus on an adult leukemia/lymphoma ward. J Infect Dis 1999; 180:1686–9. American Academy of Pediatrics, Committee of Infectious Diseases. Prevention of respiratory syncytial virus infections: indications for use of palivizumab and update on the use of RSV-IVIG. Pediatrics 1998; 102: 1211–6. IMpact-RSV Study Group. Palivizumab, a humanized respiratory syncytial virus monoclonal antibody, reduces hospitalization from respiratory syncytial virus infection in high-risk infants. Pediatrics 1998; 102:531–7. Whimbey E, Englund JA, Couch RB. Community respiratory virus infections in immunocompromised patients with cancer. Am J Med 1997; 102:10–8.