* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Aging of Cardiac Muscle and Cardiac Failure
Survey
Document related concepts
Management of acute coronary syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Saturated fat and cardiovascular disease wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Jatene procedure wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Rheumatic fever wikipedia , lookup
Electrocardiography wikipedia , lookup
Heart failure wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Transcript
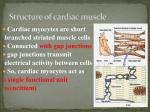
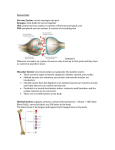
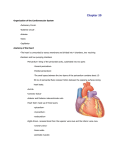
Today 3/20/06 1. Exercise 2. Aging of Skeletal Muscle 3. Aging of Heart Exercise and Aging • EXERCISE SLOWS AGING AND COMPENSATES FOR EFFECTS OF AGING • WHAT DOES EXERCISE DO? – – – – – Cardiovascular Fitness Metabolic Fitness—Obesity and diabetes protection Muscular Strength Anti-oxidant defenses Freedom from Injury—bones and muscles, osteoperosis – Sense of Well Being Measuring CV fitness • Cardiovascular Fitness – Exercising prevents CV disease and death from disease – VO2 Max (Maximal oxygen consumption) declines with aging and is increased by regular exercise – VO2 Max is higher in trained elderly person. – VO2 Max declines with age in both a trained and untrained elderly person to become almost equal. Metabolic Fitness – – – – Control age related increases in body fat Decrease risk of diabetes Maintain Ideal BMI Exercise at 45-50% of VO2 Max to facilitate fat loss and then start to metabolize carbohydrates (cross-over concept) Muscles There are 660 skeletal muscles in adult humans These constitute 45% to 50% of the normal body weight Their primary purpose is to provide “MOTILITY” In addition, they represent the major site for: - energy transduction - energy storage - primary support system Anatomy • 2 membranes surround the muscles: – outer membrane: the basement membrane (very permeable to solutes and proteins or to other metabolites) – inner membrane: SARCOLEMMA is located just beneath the plasma membrane (a true cell boundary) • An intact sarcolemma is critically important: – it maintains a proper acid-base balance of the fibers – propagates the action potential (starting at the neuromuscular plaque leading to the muscle contraction) Contraction The actors: • Ca++ passes through the sarcolemma; in its presence there is hydrolysis of ATP (ADP+P) which releases energy • ADP binds to ACTIN: meanwhile, a regulatory protein (enzyme) TROPONIN (activated by this energy) binds to MYOSIN forming TROPOMYOSIN--shifting the ACTIN helix and leading to CONTRACTION End result: the ACTOMYOSIN complex • Contraction could involve lengthening or shortening mechanisms, depending on the movement pattern • MEMO the TETANIC contraction SARCOPENIA: Loss of muscle tissue Most significant physiological change in muscle is with AGE Looking at muscles, fat and bones, we see that: At age 20, muscles are 45%, fat 20% and bones 12% of the total weight At age 75, muscles are 15%, fat 40% and bones 8% After age 49, there is a loss of 1.2 kg (3lbs) of muscle per decade DURING SARCOPENIA: The loss appears to be more significant for the FAST FIBERS type 1 and 2 (or FO and FOG) while the SLOW FIBERS (or SO) are more stable. This fact clarifies at least in part why a 9-year-old grandson can beat grandpa easily in a 100m run but will tire much sooner in a 10km hike. Reminder: The fast fibers (normally more pale) fatigue more easily while the slow (more red) are more resistant to FATIGUE. THE ETIOLOGY of SARCOPENIA due to a) inactivity b) decreased protein synthesis c) plus neural, hormonal and nutritional factors SARCOPENIA is aggravated: by the relative deficiency of the anabolic hormones (GH, Insulin-like GH, DHEA) BUT and AGAIN of greater importance is the DECREASE of VIGOROUS MUSCULAR WORK Any acute illness forcing elderly persons to bed rest is provoking a loss of muscle mass of about 1.5% per day Hence for 1 day of bed rest, up to 2 weeks of intense reconditioning is necessary. Sarcopenia harder for the FAST PALE FIBERS, but why? WE DO NOT KNOW but… fiber characteristics can be modified by different modalities like hormonal administration and/or by specific exercises or activities The change in the fiber characteristic is defined as MYOPLASTICITY MYOPLASTICITY May occur with different clinical effects, namely: -muscles enlarge with resistance type of exercise -increase their contractility (and the number of mitochondria) with endurance type of exercises -all these changes are due to stimulations and variations in the characteristics of the MYOSINS (protein isoforms) CLINICAL significance of Myoplasticity: RESISTANCE training: increases amount of contractile proteins permitting increasing efforts. As a consequence, muscles do ENLARGE (a decrease in Ca++ concentration is needed to elicit 50% of maximal tension). ENDURANCE training: increases the velocity of contraction, increases the number of mitochondria, and increases the capacity to oxidize substrate •Increase the Vmax (velocity of contraction) of the SO (slow) fibers •Decreases the Vmax of the FO (fast) fibers •Vmax = velocity of shortening of a fiber BENEFITS OF EXERCISE TRAINING (see lecture by Prof. Brooks) • Prevention of bone loss • Improvement of postural stability • Psychological benefits are to be added like preservation of cognitive functions, reduced incidence of depression and enhanced self-efficacy. • Prevention of colonic cancer possibly due to increased GI transit time and stimulation by GH and IGF-1. CLEAR BENEFITS OBTAINED WITH EXERCISE: • Metabolic: increased insulin sensitivity and glucose tolerance. • Cardiovascular: reduces blood pressure, helps vasodilation, reduces incidence of arrythmias •Cerebral: enhanced brain blood supply and reduced episodes of thrombosis • Improved equilibrium hence fewer falls • Lower mortality rate • Higher HDL/LDL ratio Aging of Cardiac Muscle and Cardiac Failure In absence of specific disease the heart adjusts very well to advancing age. Physiological Changes with Age: exercise and diet are important! Parameter 20 years 60 years VO2 Max (mL x kg x min) 39 29 Maximum Heart Rate 194 162 Resting Heart Rate Max. Cardiac Output (L x min) EJECTION FRACTION 63 22 70-80% 62 16 50-55% Resting BP Total Lung Capacity (L) 120/80 6.7 130/80 6.5 Vital Capacity (L) 5.1 4.4 Residual Lung Volume (L) 1.5 2.0 Body Fat % 20.1 22.3 Blood Pressure Physiolgic Changes with Age Hypertension: most common treatable cardiovascular change in the elderly Definition: values above 140/190 In young, if standing BP but in elderly it may to 20 mmHg Orthostatic hypotension: drop of 20 mmHg in the systolic and 10 or more in the diastolic BP on standing upright Pathology of the Aging Heart Changes due to: • Normal Aging Processes • Superimposed Processes (i.e. endocarditis) • Residuals of other conditions (i.e. hypertension, bicuspid, aortic valve Pathological Changes of the Aging Heart • Size: can atrophy, remain unchanged or develop moderate hypertrophy. • Cardiac myocytes: in size, not numbers (some replaced with fibrous tissue). Cardiac myocytes effective in reentering the cell cycle & proliferating, partly offsetting cell loss due to necrosis or apoptosis. • Amyloid deposition: half of those +70 years have some amyloid deposits in the heart but mostly in small amount & confined to the atria. • Vasculature (atherosclerosis) Walls of large arteries thicken, vessels become dilated and elongated. Increase intimal thickness (due to cellular and matrix deposition) Pathological Changes Continued • Aortic Stenosis: Narrowing of the aortic orifice of the heart or of the aorta itself. Due to fatty alteration of collagen, calcification, rigidity and various degrees of aortic stenosis, amyloid infiltration of the valves • Valves of heart become thickened and calcified. Complications include heart block, infections and embolic events Heart Failure: Cardiac Output (CO) insufficient to meet physiologic demands In the elderly, heart failure due to: • Mostly systemic arterial hypertension • Coronary artery & valvular diseases (due to impaired cardiac filling & chronic volume overload) • Combined right & left cardiac failure most common, but isolated occurrence of left or right also probable Contributory Causes to Heart Failure in the Elderly • • • • • • • • Hypertension (poor elasticity of arterial system) Alcohol, but only if in excess Viral infections Autoimmunity Heredity (specially for the cardiomyopathies) Senile amyloid Diabetes (due to the microvascular disease) Arrhythmias and especially the TACHYCARDIAS Heart Failure in the Elderly • Symptoms: dyspnea, orthopnea, fatigue on exertion and dependent edema • Severity: classified according to the NY Heart Association Scale Cardiomyopathy: Any heart muscle disorder not caused by coronary artery disease, hypertension or congenital valvular or pericardial diseases. Prevalence of heart failure: 25-54 yrs: 1% 55-65 yrs: 3% 65-74 yrs: 4.5% +75 yrs: 10% • > 75% of patients with heart failure +60 years of age •Primary reason is Coronary Heart Disease (CHD) •Secondary reason is Hypertension •Third reason is cardiomyopathy Dilated Cardiomyopathy Normal Heart Hypertrophic Cardiomyopathy Normal Heart Restrictive Cardiomyopathy: The classic example is the senile cardiac amyloidosis of the elderly, especially over 95 years old. Normal Heart Sudden Death from a cardiomyopathy • In young athletes (also in middle aged men), SUDDEN DEATH can occur in patients with congenital hypertrophic cardiomyopathy – Usually due to severe arrythmia (ventricular fibrillation) – If diagnosis is made a cardiac defibrillator should be implanted. • The SUDDEN DEATH of runners are usually limited to 1 case per 15,000 runners per year-- hence, very rare. • MEMO: There is still the possibility of ANAPHYLACTIC SHOCK in runners or walkers, if stung by a bee. Syncope in Elderly Definition: temporary suspension of consciousness due to cerebral ischemia Causes • Orthostatic Hypotension • Vaso-Vagal Reflex (?) • Arrhythmias (brady- & tachyarrhythmias) • Drugs – Antihypertensives (vasodilators/diuretics) – Cardiac drugs: beta-blockers, digitalis, anti- arrhythmias, Ca+2 channel blockers, nitrates. – Recreational: alcohol, marijuana and cocaine. – Psychiatric: Antidepressants and phenothiazines Conduction System in Aged Heart • Sinoatrial Node: Increased fibrous tissue; seldom origin for arrythmias • Atrio-Ventricular Node: Slight increase in collagen fibers • Bundle of His: Increased fibrous tissue with higher frequency of First or Second degree heart block (the mobitz) • Also the possibility of: L or R BBB (Bundle Branch Block) -this is seldom a complete heart block. • In the conduction system fibrosis occurs: 40% – Coronary Artery Disease : 20% – Calcification : 10% Normal ECG Ventricular Fibrillation Atrial Fibrillation