* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download learning zone
Heart failure wikipedia , lookup
Coronary artery disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Myocardial infarction wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Jatene procedure wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Atrial fibrillation wikipedia , lookup
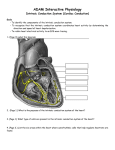
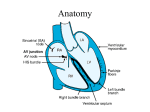
p50-57w12 19/11/09 13:17 Page 50 learning zone CONTINUING PROFESSIONAL DEVELOPMENT Page 58 ECG interpretation multiple choice questionnaire Page 59 Read Laura Demmen’s practice profile on care after death Page 60 Guidelines on how to write a practice profile An introduction to electrocardiogram interpretation:part 1 NS520 Woodrow P (2009) An introduction to electrocardiogram interpretation: part 1. Nursing Standard. 24, 12, 50-57. Date of acceptance: July 24 2009. Summary Introduction This article describes how to interpret the single-lead electrocardiogram (ECG). The author also describes cardiac electrophysiology and how this is represented by ECG graphs. Part 2 of this article, to be published next week, will describe 12-lead ECGs and acute coronary syndromes. Cardiac changes can be sudden and devastating, and while some changes may not always be preventable or treatable, patients in acute hospitals experience significant morbidity and mortality that is avoidable (National Institute for Health and Clinical Excellence (NICE) 2007). ECGs are the most common cardiovascular diagnostic procedure (Kligfield et al 2007). Nurses who are able to recognise abnormal ECGs are well placed to initiate early action to improve patient outcomes. ECGs contain much information in relatively little space. A framework is provided in this article for systematic interpretation and applied to normal sinus rhythm and the most commonly encountered dysrhythmias. Once the nurse is confident with the core aspects, his or her knowledge and skills can be developed further through more advanced texts and resources. Normal sinus rhythm is also described, together with common conduction problems and treatments. Tracings (views) of cardiac electrical activity taken from electrodes are called ‘leads’; however, in daily language ‘lead’ is usually used to describe a wire. In this article, leads are used to describe views of electrical activity and ‘electrodes’ to identify sites on the body from which wires transmit electrical information to ECG machines. Bedside monitors usually only display one or sometimes two leads, so this article describes limb lead II, the usual default lead displayed on monitors, and the usual ‘rhythm strip’ on 12-lead ECGs, which should be recorded when there are specific concerns. More information can be found on 12-lead ECGs in Part 2 of this article, which also describes acute coronary syndromes. Author Philip Woodrow, practice development nurse in critical care, Intensive Therapy Unit, Kent & Canterbury Hospital, Kent. Email: [email protected] Keywords Atrial fibrillation, atrioventricular blocks, dysrhythmias, electrocardiograms These keywords are based on subject headings from the British Nursing Index. This article has been subject to double-blind review. For author and research article guidelines visit the Nursing Standard home page at nursingstandard.rcnpublishing.co.uk. For related articles visit our online archive and search using the keywords. Aims and intended learning outcomes This article aims to improve the reader’s ability to interpret single-lead electrocardiogram (ECG) monitoring. After reading this article and completing the time out activities you should be able to: Explain normal cardiac conduction. Identify components of the normal sinus rhythm complex and what they signify. Recognise atrial fibrillation and atrioventricular blocks. Use a systematic approach to ECG interpretation. 50 november 25 :: vol 24 no 12 :: 2009 NURSING STANDARD p50-57w12 19/11/09 13:17 Page 51 An ECG is a time/voltage graph of electrical activity in the heart. Cardiac muscle conducts can also generate electrical impulses. Usually, muscular contraction, which creates the pulse, follows electrical activity. There are many factors that can influence cardiac function, but measuring the time of electrical conduction and viewing the voltage involved usually indicate function, while different parts of the ECG complex represent different stages of conduction (Houghton and Gray 2008). ‘Normal’ healthy adult time ranges are suggested, but as with other observations and vital signs, what is normal for each individual patient may vary slightly. Names of abnormalities sometimes vary between texts and practitioners so, where appropriate, this article includes variants – the nurse should therefore be able to recognise whatever terms he or she encounters in practice. This article uses the term dysrhythmias for abnormal (non-sinus) rhythm rather than the more commonly used term arrhythmias. While ECGs may contain abnormal (ectopic) beats, initial interpretation should focus on the underlying rhythm. Polarisation Muscular electrical activity occurs through the movement of ions (sodium, calcium, potassium) across cell membranes. Ion movement changes the cell membrane’s charge from its resting –90 millivolts (mV), so polarity is lost and the cell becomes electrically excitable (depolarisation). When normal ion balance and cell membrane polarity are then restored, electrical excitability ceases (repolarisation). To summarise: Depolarisation = electrical activity. Repolarisation = end of electrical activity. Higher control Heart rate is regulated by the cardiac centre, one of the vital centres in the brainstem. The cardiac centre sends signals via the sympathetic and parasympathetic fibres of the autonomic nervous system. Sympathetic stimulation increases the heart rate, while parasympathetic stimulation decreases it. Most nerve impulses that reach the heart are parasympathetic, slowing down intrinsically fast heart rates (Marieb and Hoehn 2007). Parasympathetic impulses travel through a branch of the vagus nerve, the tenth cranial nerve. Therefore, stimulating the vagus nerve in another part of the body can slow the heart rate (vagal stimulation). This can be exploited therapeutically, using carotid massage, but this should only be attempted if users have been trained to perform it safely. Vagal stimulation can occur unintentionally. For example, people who are constipated and strain when passing a stool might induce bradycardia and NURSING STANDARD myocardial infarction by stimulating vagal nerve fibres in the gut. Conduction pathway Impulses are conducted through a specialised pathway (Figure 1). If one pacemaker fails, the next part of the conduction pathway might initiate impulses to fill the gap. This is referred to as an escape ectopic/rhythm (Hampton 2008). Sinoatrial node Normally, the sinoatrial (SA) node is the pacemaker – it initiates electrical impulses and sets the heart rate. Any rhythm not originating from the sinoatrial node is therefore not sinus. Sometimes the term ‘sinus rhythm’ is used incorrectly to describe a rate between 60 and 100 beats per minute (bpm), which is a normal heart rate for adults. Impulses from the SA node spread out across atrial muscle, conducted from one muscle cell to the next. Without specialised conduction pathways, this makes conduction across the atria relatively slow. Atrioventricular node The atrioventricular (AV) node acts like a gateway into the ventricular conduction system, delaying impulses for approximately 0.1-0.2 seconds (Marieb and Hoehn 2007). This creates a short period of electrical standstill between the end of atrial depolarisation (P wave) and ventricular depolarisation (QRS wave), limiting the number of impulses that can be conducted by the AV node to approximately 230bpm (Ganong 2005). If the AV node does not receive impulses, it might become the pacemaker, typically with rates of 50-60bpm (Marieb and Hoehn 2007). FIGURE 1 Conduction pathway Sinoatrial node Atrioventricular node Bundle of His Left bundle branch Right bundle branch Purkinje fibres november 25 :: vol 24 no 12 :: 2009 51 p50-57w12 19/11/09 13:17 Page 52 learning zone cardiology focus Ventricular conduction Impulses travel quickly from the AV node through specialised conduction pathways: the bundle of His, which splits into the left and right bundle branches. The left bundle branch further splits into anterior and posterior fasicles. From the three fasicles (right bundle branch, left anterior hemibranch, left posterior hemibranch) impulses spread into the ventricular muscle mass through the Purkinje fibres (Hampton 2008). This conduction tissue enables rapid transmission from the AV node to ventricular myocytes – normally no more than 0.1 seconds (the minimum AV node delay) (Marieb and Hoehn 2007). If no impulses are received from the AV node, the ventricular conduction pathway can become the pacemaker, but its rate is often about 30bpm, which is likely to compromise the patient’s blood pressure and might lead to cardiac arrest. Time out 1 Think of some patients you have cared for and list the reasons why bedside cardiac monitors have been used. Time out 2 Continue reading and focus on the section on regularity. Use the methods described to calculate the heart rate in the ECG below. Find at least one ECG in a patient’s notes and calculate his or her heart rate at the time it was taken. failure to detect electrical activity, such as poor electrode contact (Houghton and Gray 2008). Electrical activity causes a vertical deflection from the isoelectric line. Deflections above the baseline are described as positive, while deflections below the baseline are described as negative. Positive and negative deflections are discussed further in the second article. ECGs measure voltage, detected in mV. Standard calibration is 1mV = 10mm (two large squares) in height. Some monitors or machines display voltage by a calibration box (either on the far left or far right), and often add: 10mm/mV. Voltage is described in more detail in the second article. Regularity Normal sinus rhythm is regular, but some regular rhythms can be abnormal and life-threatening, such as ventricular tachycardia. Irregular rhythms are usually abnormal, although slight variations can be caused by breathing and other factors (Houghton and Gray 2008). Staff should know whether or not patients have regular heart rates by checking the pulse, but ECG interpretation should begin by assessing whether or not the rhythm is regular. Regularity can be assessed by seeing if the distance between R waves (peaks of complexes) is constant. The easiest way to do this is usually by: Placing some paper over a printout so that only R waves are visible. Marking a few consecutive R waves. Moving the paper along a few complexes. If the distance between R waves remains (approximately) constant, then the ECG is regular. If not, it is irregular (Houghton and Gray 2008). Provided the ECG is recorded using the standard speed of 25mm/second, heart rate can be calculated either by (Jevon 2009): Counting the number of R waves in six seconds (30 large boxes) and multiplying by ten. Putting it on paper The ECG is a time/voltage graph. Time is represented horizontally, and voltage vertically. In the UK, ECG machines (including bedside monitors) run at a standard speed of 25mm/second. ECG graph paper is divided into millimetre squares, with larger squares each measuring 5mm. Twenty five small squares (or five large squares) pass each second. So on the horizontal axis, each large square represents 0.2 seconds, and each small square represents 0.04 seconds. Many screens and printouts display the time in words: 25mm/s. If no electrical activity is detected, machines display a horizontal line, called the isoelectric line. Asystole will usually produce a slightly wavy line, so a straight line is more likely to indicate 52 november 25 :: vol 24 no 12 :: 2009 Counting the number of large squares between two consecutive R waves and dividing 300 by that number. If ECGs are irregular, then assess whether or not a pattern can be seen to the irregularity, for example regularly missed beats. If there is a pattern, it may be called regularly irregular. If there is no pattern, it is irregularly irregular. With irregular rhythms, the first method suggested above is usually better, although it may be difficult. The second method is usually easier for calculating regular rhythms (Houghton and Gray 2008). Normal adult heart rates are between 60 and 100bpm – rates below 60bpm are known as bradycardias, while those above 100bpm are NURSING STANDARD 19/11/09 13:17 Page 53 tachycardias. Mild tachycardias (up to about 130bpm) are usually compensatory and seldom compromise blood pressure (Hinds and Watson 2008), so treatments should focus on the underlying causes. However, faster tachycardias (more than 130bpm at rest) may become imminently life-threatening and require urgent treatment. Treatment of supraventricular tachycardia (originating above the ventricles) and ventricular tachycardia is (usually) different, so rapid identification may be life saving. They can be distinguished by the width of the QRS complex (Davey 2008): Narrow complex tachycardias are supraventricular. Broad complex tachycardias are usually ventricular. FIGURE 2 Sinus rhythm complex Atria 2 Ventricles RR interval Millivolts (mV) p50-57w12 R 1 S-T segment T P 0 Q S Q-T interval P-R interval = 0.16 sec –1 0 0.2 0.4 0.6 0.8 1.0 1.2 BOX 1 P wave. A systematic approach to ECG interpretation PR interval. Regularity Is the rate regular? If not, is the rate: Regularly irregular – is there a pattern? Irregularly irregular – is there no pattern? QRS complex. ST segment. T wave, and sometimes a U wave. Following this sequence using a structured framework, such as the one shown in Box 1, helps interpretation. Normal timings, described in each section, are summarised in Table 1. Whereas timings should apply to all ECG leads, the shapes often differ, so the descriptions below are for limb lead II. P wave The P wave represents atrial depolarisation. P waves are relatively broad and shallow. The normal P wave timing is 0.08 seconds (two small squares) (Marieb and Hoehn 2007). P waves are often difficult to see, but should have a rounded (hump-back bridge) shape. P wave abnormalities indicate atrial (that is, supraventricular) abnormalities (Hampton 2008). Common P wave abnormalities are listed in Table 2. If P waves are missing, other atrial activity may be seen, for example: Fibrillation waves (a wavy baseline, which may be coarse or fine) – atrial fibrillation is discussed below. Flutter waves (sharp upstroke – ‘saw-tooth’ or ‘sharks tooth’ (Figure 3)). Pacing spikes – vertical lines, indicating an artificial pacemaker (temporary or permanent); pacing is not discussed further in these two articles. NURSING STANDARD 1.6 Time (s) Normal ECG complex The normal sinus rhythm complex comprises (Figure 2) : Q wave. 1.4 P wave Does the P wave appear before the QRS? Is there one P wave before every QRS? Is the shape normal? Are P waves missing? Check to see if they are replaced by pacing spikes, for example. PR interval Does the PR interval cover three to five small squares? QRS complex Is the QRS width within three small squares? Is the QRS positive or negative? Is the axis normal?* Does the QRS look normal? ST segment Does the isoelectric line return between the S and the T? If not, is it: Elevated (>1mm above the isoelectric line)? Depressed (<0.5mm below the isoelectric line)? T wave Does the T wave look normal? Is the QT interval less than half the preceding R-R interval, with a maximum length of 0.4 seconds? Tachycardia (>100 beats per minute) Narrow complex (usually with P waves) = atrial (supraventricular). Wide complex (without P wave) = ventricular. *The QRS axis is discussed in Part 2 of this article. (Reproduced with permission from Moore and Woodrow 2009) Atrial conduction, and therefore contraction, precedes ventricular activity. Stroke volume – the amount of blood ejected from a ventricle when it contracts – is reduced by 20-30% if november 25 :: vol 24 no 12 :: 2009 53 p50-57w12 19/11/09 13:17 Page 54 learning zone cardiology focus atrioventricular synchronisation is lost (Novak et al 2002), so making pulses weaker. Therefore, any rhythm lacking atrial-ventricular synchronisation, that does not have P waves preceding ventricular depolarisation, may result in smaller stroke volumes. Unless compensatory mechanisms such as increased right-sided filling (preload) or tachycardia occur, blood pressure will be compromised. PR interval The PR interval is measured from the start of the P wave to the Q wave (the first negative deflection) (Guyton and Hall 2006) or, in the absence of Q waves, to the start of the R wave. So it includes the P wave and the period of electrical standstill created by impulses crossing the AV node. Normal PR time is 0.12-0.2 seconds (three to five small squares, or no more than one large square) (Hampton 2008). TABLE 1 Normal timings of the electrocardiogram (ECG) complex Time Width* P wave 0.08 seconds Two small squares PR interval 0.12-0.2 seconds Three to five small squares (no more than one large square) QRS Maximum 0.12 seconds Maximum three small squares ST segment Not significant T wave 0.16 seconds QT interval < half preceding R-R interval Four small squares *If ECG speed is 25mm/second TABLE 2 Common P wave abnormalities Shape Likely cause Peaked Right atrial enlargement, from lung disease, for example chronic obstructive pulmonary disease. Broad or notched Left atrial enlargement, from left-sided strain, for example left ventricular failure, mitral valve disease. Inverted From an ectopic pacemaker. (Jowett and Thompson 2007) FIGURE 3 Atrial flutter 54 november 25 :: vol 24 no 12 :: 2009 The only possible PR abnormalities are that the intervals are too long or too short. Short PR intervals are fairly rare and are usually caused by abnormal conduction pathways such as that of the bundle of Kent, an extra conduction pathway, which causes Wolff-Parkinson-White syndrome (Hampton 2008). Long PR intervals, caused by prolonged delay at the AV node, are more common. Prolonged PR intervals are variously called first-degree block, first-degree heart block or first-degree AV node block – all terms mean the same thing. Q wave The Q wave, the first negative deflection, is caused by depolarisation through the septum (muscle wall) that separates the left and right ventricles, and through which the ventricular conduction pathway passes. Q waves are usually small or absent, depending on the electrical view (or lead used). Deep Q waves (bigger than 0.2 small squares) often indicate myocardial infarction (Meek and Morris 2008). However, deep Q waves do not always appear following infarction, so a diagnosis of infarction cannot be excluded if deep Q waves are not present. Generally it is more useful to look at the QRS complex in its entirety. QRS complex The QRS complex represents ventricular depolarisation. Much voltage is needed for ventricular depolarisation, making the QRS the tallest part of these complexes. However, the specialised conduction pathway (bundle of His, bundle branches and hemibranches, and Purkinje fibres) ensures that impulses travel quickly from the AV node to ventricular muscle. Normal QRS width is within 0.12 seconds (three small squares) (Jevon 2009) and is often half this width. In limb lead II (the lead most often shown on single-lead ECGs), and in most other leads, the QRS is normally positive. This is discussed in more detail in Part 2. Wide QRS complexes indicate ventricular abnormalities (Jevon 2009). Although there are also other less frequent causes, likely causes of wide QRS complexes include (Hampton 2008): Bundle branch block (discussed in Part 2 of this article). Ventricular ectopics or rhythms. Artificial pacemakers. ST segment After a negative deflection at the S wave, the QRS should return to the isoelectric line quickly, followed by some electrical standstill (horizontal isoelectric line) before the T wave. Timing of the ST segment is not significant. What is important is that there is no elevation or depression (Hampton 2008). Although ST abnormality may be suspected from a single-lead ECG, a 12-lead ECG is necessary to confirm the NURSING STANDARD p50-57w12 19/11/09 13:17 Page 55 abnormality. ST elevation and depression, and acute coronary syndromes are discussed in Part 2. T wave The T wave represents ventricular repolarisation, the end of the cardiac conduction. The normal T wave time is 0.16 seconds (four small squares) (Marieb and Hoehn 2007). However, height is more important than T wave length. Jowett and Thompson (2007) suggested that normal T wave height is less than 5mm, but Houghton and Gray (2008) suggested there is no normal height. It should be taller than the P wave. T wave abnormalities are non-specific, which is usually all the information given by machine diagnosis. Although there may be various causes for T wave abnormalities, a common cause is abnormal potassium levels in blood (Houghton and Gray 2008): High T wave = (probably) high potassium levels. Low T wave = (probably) low potassium levels. T wave inversion is usually abnormal (unless QRS complexes are negative). T wave inversion can also have various causes, including hypertrophy, but a newly inverted T wave may be the result of ischaemia or infarction (Hampton 2008). QT interval The QT interval from the beginning of the Q wave to the end of the T wave represents total ventricular depolarisation and repolarisation time. It should be less than half the time of the preceding R-R interval (Jevon 2009). Prolonged QT intervals represent delayed repolarisation, which may cause tachydysrhythmias (dysrhythmias with rates over 100bpm, and often considerably faster than this) and sudden cardiac death (Straus et al 2006). Some people are genetically susceptible to long QT syndrome, and need to avoid drugs that might aggravate the problem – this is an extensive list, but it includes many commonly used drugs such as salbutamol, many psychotropic drugs and paradoxically many cardiac drugs such as beta blockers. As high heart rates decrease the QT interval, cardiologists might calculate the QTc – the QT interval corrected to what it would be if the heart rate was 60bpm (Davey 2008). Time out 3 Ask your ward or department pharmacist which drugs, that are commonly used in your clinical area, patients with long QT syndrome should avoid. (Hampton 2008). Unless staff are very skilled at ECG interpretation, U waves are usually best forgotten about. Atrial fibrillation So far this article has focused on the normal sinus rhythm. However, ECGs are generally recorded because of cardiac abnormalities or concerns. Many ECGs seen in practice are abnormal. The most common abnormal rhythm is atrial fibrillation (AF) (Royal College of Physicians (RCP) and NICE 2006). AF affects about 5% of people over the age of 65 in the UK, and incidence increases with age, to about 9% in people over the age of 80 years (RCP and NICE 2006). AF causes chaotic atrial activity, with no co-ordinated conduction or contraction occurring in the atria (Jevon 2009). There will therefore be no P waves, but some erratic atrial activity may appear as a ‘wavy’ isoelectric line (Figure 4). AF may be ‘fine’ (little or no activity is seen between T waves and QRS complexes) or ‘coarse’ (chaotic activity is visible between T waves and QRSs) (Jevon 2009). Consensus classification (RCP and NICE 2006) defines AF as one of the following: An initial event. Paroxysmal: spontaneous termination, recurrent, for less than seven days, and often for less than 48 hours. Persistent: not self-terminating. Permanent (accepted): not terminated. The first three groups are sometimes termed acute AF, while permanent AF is sometimes called chronic AF. Acute AF often occurs in response to a trigger, such as illness or surgery. Treatment aims for acute AF are to control heart rate and restore sinus rhythm, using drugs such as amiodarone and/or electrical cardioversion (Zimetbaum 2007, Musco et al 2008). With sinus rhythm, atria contract before ventricles, causing active flow of blood into ventricles. AF lacks this active part to atrial bloodflow, leaving only passive flow, which may result in thrombi and therefore emboli that may cause strokes. Anticoagulants may therefore be needed to the reduce the risk of stroke. Permanent or chronic AF cannot be cured, but should be controlled (RCP and NICE 2006). As with acute AF, the two aspects that should be controlled are heart rate and coagulation. FIGURE 4 Atrial fibrillation U wave While U waves are frequently described in texts, they are seldom seen in practice. Often they are not present. If they are present they are often too small to see on ECGs, and may be a sign of good health or problems (often hyperkalaemia) NURSING STANDARD november 25 :: vol 24 no 12 :: 2009 55 p50-57w12 19/11/09 13:17 Page 56 learning zone cardiology focus Time out 4 Ask your medical team what drugs they prescribe to control heart rate and coagulation. Also discuss what alternative drugs they might use, and factors that would influence their choice. AF usually causes tachycardia. The target for heart rate control is usually below 100bpm. Although the RCP and NICE (2006) suggest that amiodarone or other rhythm-control drugs are preferable to the rate-control drug digoxin, established AF is still often treated with digoxin. Passive blood flow through the atria increases the risk of thrombi, and therefore strokes and other thrombotic events (Hart et al 2003). Anticoagulation, usually with warfarin (Mant et al 2007, Waldo 2008), reduces stroke risk by 60% (Shannon 2009), and is usually given to achieve a target international normalisation ratio of 2-3 (RCP and NICE 2006). Warfarin has a narrow therapeutic range, so serum levels need to be monitored frequently. ECGs (and pulses) where the rate is irregularly irregular (no pattern) are usually caused by AF or a mixture of various rhythms (one of which may be AF). Erratic times between pulses cause variable ventricular filling times, and so variable pulses. Some pulses may be too weak to be felt at the peripheries, which causes an apex-radial deficit. Digoxin, or other heart rate control drugs, should usually be omitted if the heart rate is below 60bpm. Recorded observations usually measure the brachial pulse rate (from automated blood pressure monitors). FIGURE 5 Atrioventricular node construction blocks a) First-degree block b) Second-degree block b) Third-degree block 56 november 25 :: vol 24 no 12 :: 2009 If the brachial pulse rate is below 60bpm, the apex rate should be checked before giving any drugs that slow down heart rate (such as digoxin), as tachycardia in AF can cause significant apex-radial deficits, with slow brachial pulses (Levine 2005). AV node blocks Electrical impulses will fail to be conducted through any tissue that is electrically unexcitable (or blocked). Blocks can occur in any part of the conduction system, but occur most often at or near the AV node. A block may be: A delay where all impulses are conducted, but more slowly than normal. Incomplete – some impulses are conducted, others are not. Complete – no impulses are conducted. AV node conduction blocks or AV heart blocks (Figure 5) are: first degree (delay), second degree (incomplete) and third degree (complete). Unless there are other diseases such as congenital defects or valve disease, blocks are usually caused by (Riley 2002): Age-related sclerosis of the AV node. Myocardial damage or infarction. Drugs, for example beta blockers. First-degree block A first-degree block does not usually cause problems or require treatment. If there are symptoms such as breathlessness or chest pain, then they should be treated. If it is caused by drugs, then the patient’s prescriptions should be reviewed. If it is symptomatic and persistent, permanent artificial pacing is sometimes necessary. Second-degree block A second-degree or incomplete block is more likely to cause symptoms. There are two types of second-degree block (Jevon 2009): Type 1 (also called Wenckebach or Mobitz type 1) and Type 2 (also called Mobitz type 2, and sometimes just Mobitz). Type 1, with progressively lengthening PR intervals until a P wave is not conducted, is the more common and less sinister type (Hatchett 2002). Type 2, where all PR intervals remain the same length, but some P waves (at regular intervals) are not conducted, is less common, but more likely to progress to complete (third-degree) block or asystole (Houghton and Gray 2008, Jevon 2009). Third-degree block A third-degree or complete block means that whatever happens in the atria is not conducted to the ventricles. The ventricles are therefore paced from a focus in the ventricles themselves, typically causing slow, wide QRS complexes – often the heart rate is about 30-40bpm (Jevon 2009). If the sinoatrial node is functional, there will be regular P waves (typically NURSING STANDARD p50-57w12 19/11/09 13:17 Page 57 60-100bpm) that are unrelated to the ventricular complexes, and which may be lost in any part of the QRS, ST segment or T wave. More often, third-degree blocks develop in patients with significant cardiac disease, who previously had established AF. The slow rate usually compromises cardiac output, causing hypotension and usually needs urgent pacing (Davey 2008). Conclusion ECGs are widely used, and might detect or confirm various cardiac problems. Some problems might necessitate urgent action, so nurses able to interpret ECGs are more likely to initiate actions or call for help. Interpreting ECGs is a skill which, like all skills, improves with practice. This article has provided a systematic means for interpreting ECGs, and described core aspects of single-lead normal sinus rhythm, together with some common dysrhythmias. Part 2 of this article in next week’s Nursing Standard will describe 12-lead ECGs and acute coronary syndromes NS Time out 5 Using the framework outlined in Box 1, practise interpreting some ECGs in your clinical area. Depending on individual patients, some aspects might involve advanced interpretation (not discussed in this article). Make a list of what you have found and discuss this list with your colleagues, or check your answers by using a textbook on ECGs. Make notes of how any problems were treated. If there are any treatments you do not understand, discuss them with more experienced colleagues, and what alternative treatments or management might have been used. Time out 6 Now that you have completed the article, you might like to write a practice profile. Guidelines to help you are on page 60. References Davey P (2008) ECG at a Glance. Wiley-Blackwell, Oxford. Hands-on Guide. Third edition. Edward Arnold, London. Ganong WF (2005) Review of Medical Physiology. Twenty second edition. McGraw Hill Medical, New York NY. Jevon P (2009) ECGs for Nurses. Second edition. Wiley-Blackwell, Oxford. Guyton AC, Hall JE (2006) Textbook of Medical Physiology. Eleventh edition. Elsevier Saunders, Philadelphia PA. Hampton JR (2008) The ECG Made Easy. Seventh edition. Churchill Livingstone, Edinburgh. Hart RG, Halperin JL, Pearce LA et al (2003) Lessons from the Stroke Prevention in Atrial Fibrillation trials. Annals of Internal Medicine. 138, 10, 831-838. Hatchett R (2002) Caring for the patient with a cardiovascular disorder. In Walsh M (Ed) Watson’s Clinical Nursing and Related Sciences. Sixth edition. Baillière Tindall, Edinburgh, 248-331. Hinds CJ, Watson JD (2008) Intensive Care: A Concise Textbook. Third edition. Saunders Elsevier, Edinburgh. Houghton AR, Gray D (2008) Making Sense of the ECG: A NURSING STANDARD Jowett NI, Thompson DR (2007) Comprehensive Coronary Care. Fourth edition. Baillière Tindall, London. Kligfield P, Gettes LS, Bailey JJ et al (2007) Recommendations for the standardization and interpretation of the electrocardiogram: part I. Circulation. 115, 10, 1306-1324. Levine BS (2005) History taking and physical examination. In Woods SL, Froelicher ESS, Motzer SU, Bridges EJ (Eds) Cardiac Nursing. Fifth edition. Lippincott Williams and Wilkins, Philadelphia PA, 229-264. Mant J, Hobbs JD, Fletcher K et al (2007) Warfarin versus aspirin for stroke prevention in an elderly community population with atrial fibrillation (the Birmingham Atrial Fibrillation Treatment of the Aged Study, BAFTA): a randomised controlled trial. The Lancet. 370, 9586, 493-503. Marieb EN, Hoehn K (2007) Human Anatomy and Physiology. Seventh edition. Benjamin/Cummings, San Francisco CA. Meek S, Morris F (2008) Introduction II-basic terminology. In Morris F, Brady WJ, Camm J (Eds) ABC of Clinical Electrocardiography. Second edition. Blackwell Publishing, Oxford, 5-8. Moore T, Woodrow P (2009) High Dependency Nursing Care: Observation, Intervention and Support for Level 2 Patients. Second edition. Routledge, Abingdon. Musco S, Conway EL, Kowey PR (2008) Drug therapy for atrial fibrillation. Medical Clinics of North America. 92, 1, 121-141. National Institute for Health and Clinical Excellence (2007) Acutely Ill Patients in Hospital: Recognition of and Response to Acute Illness in Adults in Hospital. NICE, London. Novak B, Filer L, Hatchett R (2002) The applied anatomy and physiology of the cardiovascular system. In Hatchett R, Thompson D (Eds) Cardiac Nursing: A Comprehensive Guide. Churchill Livingstone, Edinburgh, 43-66. Riley J (2002) The ECG: its role and practical application. In Hatchett R, Thompson D (Eds) Cardiac Nursing: A Comprehensive Guide. Churchill Livingstone, Edinburgh, 97-117. Royal College of Physicians, National Institute for Health and Clinical Excellence (2006) Atrial Fibrillation. National Clinical Guideline for Management in Primary and Secondary Care. RCP and NICE, London. Shannon MS (2009) Anticoagulation in practice. Medicine. 37, 3, 155-158. Straus SM, Kors JA, De Bruin ML et al (2006) Prolonged QTc interval and risk of sudden cardiac death in a population of older adults. Journal of the American College of Cardiology. 47, 2, 362-367. Waldo AL (2008) Anticoagulation: stroke prevention in patients with atrial fibrillation. Medical Clinics of North America. 92, 1, 143-159. Zimetbaum P (2007) Amiodarone for atrial fibrillation. New England Journal of Medicine. 356, 9, 935-941. november 25 :: vol 24 no 12 :: 2009 57 Copyright of Nursing Standard is the property of RCN Publishing Company and its content may not be copied or emailed to multiple sites or posted to a listserv without the copyright holder's express written permission. However, users may print, download, or email articles for individual use.