* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download J Thorac Cardiovasc Surg
Survey
Document related concepts
Saturated fat and cardiovascular disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Heart failure wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Coronary artery disease wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
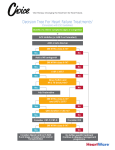
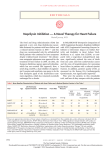
THE TREATMENT OF ADVANCED HEART FAILURE ROSS ZIMMER MD, FACC DIRECTOR, HEART FAILURE PROGRAM CLINICAL ASSOCIATE PROFESSOR OF MEDICINE PENN PRESBYTERIAN MEDICAL CENTER 2 Traditional Therapies Beta Blockers Reduce catecholamine effects Decrease myocardial O2 demand Antiarrhythmic ACE/ARBs Reduce afteroad Prevent remodeling Reduce RAAS impact on heart and vascular Aldosterone Inhibitors Prevent myocardial hypertrophy Reduce fibrosis Decrease arrhythmia potential Diuretics Decrease after/preload Reduce dyspnea Decongest splanchnic circulation 3 Ivabradine First-in-class to selectively inhibit hyperpolarization-activated cyclic nucleotide (HCN) gated (If current) channel within the SA node that lowers heart rate Dose-dependent reduction in heart rate Degree of effect is dependent on the baseline heart rate 4 The SHIFT (Systolic Heart Failure Treatment with the If Inhibitor Ivabradine) trial Chronic stable HF with LVEF ≤35 percent In sinus resting heart rate ≥70 bpm On max dose (or maximally tolerated dose) Beta-blocker Primary end point: composite of cardiovascular death or hospital admission for worsening HF Swedberg K, et al. SHIFT Study. Lancet 2010;376:875-85. 5 SHIFT STUDY Randomized, double-blind, placebo-controlled, parallel group study 6558 patients with systolic HF followed for 23 months NYHA class II, III, IV symptoms In stable condition for >4 weeks On guideline-based HF medication regimen without changes in meds or doses for >4 weeks HF exacerbation admission within 12 months 6 Swedberg K, et al. SHIFT Study. Lancet 2010;376:875-85. Ivabradine vs. Placebo Reduced primary events (24% vs. 29%, 95% CI 0.75-0.90; p<0.0001; NNT=20) Decreased HF deaths (3% vs. 5%; p=0.014) Decreased HF admissions (16% vs. 21%; p<0.0001) Did not significantly reduce cardiovascular/allcause deaths (p=0.128) Swedberg K, et al. SHIFT Study. Lancet 2010;376:875-85. 7 (all comparisons are versus enalapril 20 mg daily, not versus placebo) Neprilysin Inhibition Promotes Action of Endogenous Vasoactive Peptides that Benefit the Failing Heart Endogenous vasoactive peptides (natriuretic peptides, adrenomedullin, bradykinin, substance P, calcitonin gene-related peptide) Neprilysin Inactive metabolites Neurohormonal activation Vascular tone Cardiac fibrosis, hypertrophy Sodium retention Neprilysin inhibition PARADIGM-HF Randomized double-blind trial sacubitril-valsartan vs. enalapril 8442 patients LVEF ≤40 percent NYHA functional class II, III, or IV 10 PARADIGM-HF: Cardiovascular Death or Heart Failure Hospitalization (Primary Endpoint) Kaplan-Meier Estimate of Cumulative Rates (%) 4 0 Enalapril 3 2 (n=4212) 914 2 4 LCZ696 (n=4187) 1 6 HR = 0.80 (0.73-0.87) P = 0.0000002 Number needed to treat = 21 8 0 0 180 360 540 720 900 1080 1260 896 853 249 236 Days After Randomization Patients at Risk LCZ696 Enalapril 1117 4187 4212 3922 3883 3663 3579 3018 2922 2257 2123 1544 1488 PARADIGM-HF Sacubitril-valsartan reduced risk of: Primary outcome of death from cardiovascular causes or HF hospitalization (21.8 vs 26.5%; HR 0.80; 95% CI 0.73-0.87) All-cause mortality (17.0 vs 19.8%; HR 0.84; 95% CI 0.76-0.93) Death from cardiovascular causes (13.3 vs 16.5%; HR 0.80; 95% CI 0.71-0.89) HF hospitalization (12.8 vs 15.6%; HR 0.79; 95% CI 0.71-0.89). 12 VENTRICULAR ASSIST DEVICES Initially developed to address short term needs in patients who struggled coming off pump during cardiac surgery With new technology, subsequently used when needed to provide hemodynamic support for those patients who were clinically declining while awaiting transplant VENTRICULAR ASSIST DEVICES Bridge to recovery explant once clinically stabilized with expectation of acceptable native cardiac function (post MI) Bridge to transplant unable to wait until an organ is available Bridge to decision options unclear Destination Therapy non-transplant candidate 14 What is Destination Therapy? Refers to VAD implantation for long-term use, rather than as a bridge to transplantation or recovery Evolving technologies increase the horizon of time support can be sustained These are not artificial hearts REMATCH: A New Era “The use of a left ventricular assist device in patients with advanced heart failure resulted in a clinically meaningful survival benefit and an improved quality of life. A left ventricular assist device is an acceptable alternative therapy in selected patients who are not candidates for cardiac transplantation.” One-year survival: 52% vs. 25% (p=0.002) Two-year survival: 23% vs. 8% (p=0.09) N ENGL J MED 2001; 345:1435-1443 25% vs. 8% at 2 Years J Thor CV Surg 2006, 129: 6 1464 HeartMate XVE Continuous vs Pulsatile Flow vs OMM NEJM 2009, 361:2282 HMII Key Design Features Valveless Only one moving part, the rotor Blood immersed bearings designed for minimization of blood damage All motor drive and control electronics are outside of the implanted blood pump Length: 3 in. Weight: 10 oz. Speed: 6,000-15,000 rpm Flow range: 3 – 10 L/min VADs Improve Functional Status > 80% of patients tested improved to NYHA class I/II from NYHA class IIIB/IV by 6 months Sustained through 24 months Six-minute walk distance improved to 340 m by 6 months from 181+/-138 and 225 +/- 142 m Sustained through 24 months VADs Improve Quality of Life When surveyed about lifestyle changes, VAD patients highlight the ability to drive, exercise, travel, return to work or school, and engage in hobbies and sexual activity as major contributors to improved QOL J Thorac Cardiovasc Surg 2004;127:1432–5 J Thorac Cardiovasc Surg 2000;119:251–9 HeartWare HVAD HeartWare HVAD Pericardial placement – no pump pocket Eliminates the need for abdominal surgery and device pockets Provides up to 10 l/min of flow Centrifugal design, continuous flow Hybrid magnetic / hydrodynamic impeller suspension Optimizes flow, pump surface washing, and hemocompatibility Displaced volume = 50cc, Weight = 160g Thin (4.2 mm), flexible driveline with fatigue-resistant cables HEARTMATE 3 HEARTMATE 3 Fully Magnetically Levitated No bearings Large pump gaps reduce blood trauma Artificial pulse Reduces risk of bleeding, AI, thrombosis, stroke Textured blood contacting surfaces allow endothelialization Output 2 – 10 L/min Who is a VAD Candidate? Selection Criteria Inability to walk a block without shortness of breath Intolerant or refractory to ACE inhibitors, ARBs, Bblockers 1 HF–related admission in the past 6 months CRT nonresponder High diuretic dose (e.g., 120 mg/d furosemide) Serum sodium < 136 mmol/L BUN > 40 mg/dL Hematocrit < 35% Thoratec Issues to Assess Pre-operatively RV function – there is no DT RVAD Aortic insufficiency – may require AVR Anticoagulation - contraindications Insight/compliance – not a “quick fix” Family/social support – a total buy-in Financial – will insurance cover it? 29 When Should You Refer? Medication Repeat Can’t intolerance hospitalizations “bounce back” Failure to thrive 30 Before they get too sick A VAD is NOT a “Hail Mary Pass” Survival after LVAD implantation by the candidate’s operative risk Lietz K et al. Circulation 2007;116:497-505 Copyright © American Heart Association MERIT-HF