* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download The Immune System
Complement system wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Molecular mimicry wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Lymphopoiesis wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Immune system wikipedia , lookup
Adaptive immune system wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
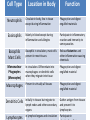
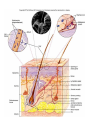
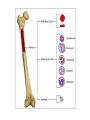
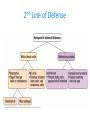
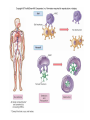
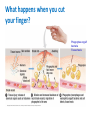
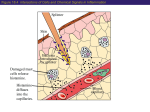
The Immune System Introduction Immune system The body’s defenses against pathogens that produce disease 2 types of immunity 1. Nonspecific defenses (Innate defense) • Provide general protection against invasion by a wide range of pathogens • Present at birth–innate 2. Specific Defenses • Specific lymphocytes combat particular pathogens Overview of the body’s defense Three lines of defense protect us from pathogens Nonspecific Defenses A set of physical barriers and chemicals that prevent foreign invaders from getting inside our bodies 1st Line of Defense External Barriers 1. PHYSICAL BARRIERS: An outer layer of skin Hair in the nostrils Mucous membranes of the digestive and respiratory tracts Cilia lining the upper respiratory tract propel trapped particles up and out Goblet cells secrete mucus, which coats the epithelial cells. Mucus contains lysozyme, that breaks down bacterial cell walls. Bacteria and other debris become trapped in the thick mucus. Cilia sweep it up and out of the respiratory tract, where it is expelled from the body by coughing, sneezing, or even swallowing! The Skin I. Epidermis - outer layer of skin that provides a barrier against infection. Any microbes attached to outer layer of dead cells will be shed with those cells. II. Dermis contains : a. sweat glands – they produce salty perspiration to flush microbes and other contaminants out of the pores. – Sweat also contains a special enzyme called lysozyme,. . b. sebaceous glands that coat the skin with sebum, which is an oily substance that contains fatty acids that lower the pH of the skin surface to inhibit microbial growth 2. Chemical defenses (barriers) Sweat, saliva, and tears contain enzymes that kill bacteria. Glands produce oils and acids The acid pH of the stomach kills many bacteria 3. Resident Bioflora Beneficial microbes living on our skin and in our bodies that help block infection by disease-causing microbes Where does all the dead skin go? • Dead skin cells can be found on our sheets, pillows, clothes, and even in the dust particles that form in our homes. • Dead skin cells are broken down by dust mites, which are microscopic parasites that live on our skin, hair, and eyelashes. 2nd Line of Defense • Acts when an invader penetrates the body’s external barriers • Nonspecific – combats all invading microbes • Depend on white blood cells and defensive proteins. White Blood Cells (cells that fight infection) 2nd Line of Defense Leukocytes – “Warriors of the immune system” AKA white blood cells Produced in the bone marrow Include: basophils, eosinophils, mast cells, neutrophils, monocytes, macrophages Lymphocytes (specific immunity) 2nd Line of Defense 2nd Line of Defense • When the external barriers fail, a set of nonspecific internal defenses stands ready – the second line of protection • Antimicrobial proteins Interferon Complement • WBCs: phagocytic cells and natural killer cells • Inflammation • Fever Antimicrobial proteins– Interferons (IFNs) • Protect body against viral infection • Cells infected by viruses produce interferon • IFNs stimulate healthy cells to produce proteins that inhibit viral reproduction Antimicrobial proteins– the complement system complement • A group of ~20 proteins in blood plasma and cell Membranes • “Complement” proteins cause invading cells to lyse – Form a “membrane attack complex” that makes holes in some microbes – Causes the microbe to lyse proteins membrane attack complex fluids fluids The 2nd line of defense: WBCs • Phagocytes • Engulf microbes or other particles (by phagocytosis) • Phagocytes migrate to infected area by chemotaxis (attracted to chemicals released by invading microbes and host cells) A Macrophage in action • White blood cells have specialized receptors on their surface that enable them to determine what is "self" and "non-self” • When "non-self" proteins are encountered, an immune response is mounted to destroy the foreign (non-self) substance. Cell Type Location in Body Function Neutrophils Circulate in body, few in tissue except during inflammation Phagocytize and digest engulfed materials Eosinophils Mainly in blood except during inflammation and allergies Participate in inflammatory reaction and immunity to some parasites Basophils Mast Cells Basophils in circulation, mast cells present in most tissues Release histamine and other inflammation causing chemicals In circulation. Differentiate into macrophages or dendritic cells when they migrate into tissue Phagocytize and digest englulfed material Macrophages Present in virtually all tissues Phagocytize and digest englulfed material Dendritic Cells Initially in tissues but migrate to lymph nodes and other secondary organs Gather antigen from tissues and present it to lymphocytes Lymphocytes In lymphoid organs and circulation Participate in Mononuclear Phagocytes (Monocytes) Natural Killer (NK) cells • Destroy infected body cells and cancerous cells • NK cells bind to infected cells • Release perforins that penetrate the plasma membrane of infected cells causing them to lyse (similar effect as complement) Chemical Messengers Cytokines – Include: • • • • • Interleukin I and II Histamine Prostaglandins Complement Interferons The 2nd line of defense: Inflammation • Occurs when tissue is damaged • Inflammation • an attempt to dispose of microbes • prevent their spread to other tissues • prepare the site for tissue repair • 4 hallmark symptoms of the inflammatory response: • Redness • Pain • Swelling • Heat (warm to the touch) What happens when you cut your finger? Phagocytes engulf bacteria Tissue heals Steps in the Inflammatory Response 1. Tissue damage 2. Mast cells release Histamine Histamine increases blood flow (by vasodilation) to damaged area (redness). Causes capillaries to become leaky (swelling). 3. Damaged cells in area produce other chemicals that attract phagocytic cells to site. Inflammatory Response 4. Prostaglandins produced – induces pain, and important in production of fever. 5. Chemicals released attract neutrophils which “stick” to capillary walls (margination), eventually “squeezing” through the leaky capillaries (extravasation). 6. Neutrophils and other phagocytes attracted to damaged site via cytokines. 7. Ingest and destroy bacteria. 8. Platelets and clotting factors help to heal wound and confine infectious agents at wound site. (McGraw Hill video)