* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download File
Survey
Document related concepts
Transcript
Lecture №1
General Anatomy and Development of the Digastive System.
Clinical Anatomy of the Digestive Organs.
Digestion - physiological process, as a result of which the nutrition in a digestive tube
is exposed to physical and chemical processing, and the nutrient materials, keeping in
it, are soaked up in a blood and lymph.
Functions of a digestive tube:
1. Mechanical and chemical treatment of food.
2. Motor - the mastication, swallowing, agitating both moving on a digestive tube and
evacuation of unnecessary oddments is provided by presence of a specific
musculation.
3. Absorstion of the treated nutrients.
4 Excretion of undigested remnants of the food.
1. Protective - lymphoid device.
The human alimentary canal is about 8-10m long and is subdivided into the
following parts: the cavity of the mouth, the pharynx, the oesophagus, the stomack and the
small and large intestine. The small intestine consists of duodenum, jejunum and illeum.
The large intestine consists of the caecum with vermiform process the ascending,
transverse, descending, and sigmoid colon and finally, the rectum. The upper three part
located in the head, neck and chest maintain a relatively straight direction. In the pharynx
the alimentary canal intersects with the respiratory tract. Organs of the digestive system
are located in the thorasic and in the abdominal cavity and the pelvic cavity.
Features of a constitution of walls of the alimentiry canal:
1. Mucous membrane (tunica mucosa) is the internal layer of the digestive tube. The
mucosa is named so, because in it is produced and is mucified of complex
2
composition - digestive juices. In structure the mucous membrane consists of:
1)epithelium and 2)lamina propria mucosae. The mucos coat is concerned with absorption
and secretion
2. The submucosa bridges mucous with muscle. It consists of a quaggy connected tissue
and contains plexuses of large veins. Their elastic fibers attach an elastance to an
environment as a whole.
3. Muscle layer{tunica muscularis} situated between the external serous and the internal
mucous membranes is formed of smooth muscular tissue; the superior and inferior parts
of the alimentary canal also contain striated fibres. The muscular coat accomplishes the
motor function. In some parts of the digestive canal striate fibers are developed very
well, thus parts are called sphincters.
4. Connective tissue covers the alimentary tube from the outside. In the thoracic and
abdominal cavity it is called tunica serosa but in the head and neck it is called
adventitia.
Development of members of an alimentary system
The digestive tube is developed from Primitive digestive tube, which is the interna
embryonic part of archenteron or primary yolk sac after the formation of foldings of the
embryo. Primitive digestive tube is divided into three parts: 1) anterior (the foregut), from
which develop the posterior part of the mouth, pharynx, oesophagus, stomack, duodenum,
liver and its excretory apparatus, gall bladder, larynx;
2) middle part (the midgut) communicating with the yolc sac. Derivatives of midgut:
duodenum, jejunum, ilium, coecum and appendix, ascending colon,right two third of
transversae colon.
3
3) the posterior part (hindgut) from which the parts of large intestine develops.
Mucous membrane of gastro-intestinal tract is endodermal but the membrane of the
mouth and lower part of anal canal is ectodermal and form stomodeum and proctodeum
respectivelt.
The musculature and rest of the wall is mesodermal and from splanchnic mesoderm.
PARTS OF THE DIGESTIVE TUBE
1. Cavity of the mouth (cavitas oris) is divided into two parts: vestibulum oris and
cavitas oris propria. The vestibulum of the mouth is the space bounded by the
lips ans cheeks externally and by the teeth and gingivae internally. Cavitas oris
proprium extends from the teeth anterioly and laterally to the entry into the
pharynx posterioly through the fauces. The oral cavity is bounded superioly by
the hard palate and the anterior part of the soft palate; the floor is formed by the
diapfragm of the mouth and is occupied by the tongue.
2. The pharynx is that part of the alimentary canal and respiratory tract, which is a
connecting link between the cavity of the nose and mouth and the oesophagus
and trachea. The pharynx is divided into three parts: nasal part of the pharynx
(pars nasalis),oral part (pars oralis),laryngeal part (pars laryngea).
At the entry into the pharynx some oval-shaped mass of lymphoid tissue are
founded: the lingual tonsil, located at the root of the tongue, two palatine tonsil,
located in the depression between two arches of the soft palate, two tube tonsil,
situated near the auditory tube of the nasopharynx and one pharyngel tonsil,
located at the posterior wall of the pharynx. Thus,
4
almost a complete ring of
lymphoid structures is called Pirogov,s
lymphoepithelial ring.
3. The oesophagus is a narrow and long actively functioning tube inserted between
the pharynx and the stomach.
THE ABDOMINAL CAVITY
4. Begining with the stomach, the parts of the digestive tract with its large glands
are located in the abdominal cavity.
The abdominal cavity is the space in the trunk below the diaphragm; it is
completely filled with the abdominal organs. The anterior wall of the abdominal cavity is
formed by the tendinous expansions of the three broad abdominal muscles and the straight
abdominal muscles. The components of the lateral walls are the muscular portions of the
three broad muscles of the abdomen. The posterior wall is formed by the lumbar segment
of the spine and the psoas major and quadratus lumborum muscles.
The abdominal cavity is subdivided into the abdominal cavity proper and the pelvic
cavity. The pelvic cavity is bounded posterioly by the piriform muscles, anterioly and
laterally by parts of the hip bones with the overlying internal obturator muscles which are
lined with fasciae. The floor of the pelvic cavity is formed by the pelvic diaphragm.
Internally of the muscular layers, the abdominal cavity is lined with the subperitoneal
fascia, which is divided into the following parts according to the regions: the transverse
fascia lines the inner surface of the transverse abdominal
muscle and is then continuous with the pelvic fascia on the walls of the pelvis. The
abdominal cavity is lined with a serous membrane called the peritoneum, which also
covers to a lesser or greater extent the abdominal viscera. When the peritoneum
5
covers the walls of the abdominal cavity it is called parietal peritoneum, if it covers the
visceral organs it is called peritoneum visceralis. Both layers are in close contact and in
an intact abdominal cavity there is only а narrow space between them called the
peritoneal cavity (cavum peritonei) that contains а small amount of serous fluid; this fluid
moistens the surface of the organs and so makes easier their movement against one
another. An organ invested in the peritoneum is said to have an intraperitoneal position
(stomack, jejunum, ileum, coecum, colon transversus, colon sygmoideum);
a
mesoperitoneal position is that when an organ is covered by the peritoneum on three sides
(colon ascendens, colon descendens, liver). If an organ is covered by the peritoneum only
in front its position is called extraperitoneal (pancreas, duodenum, kidneys).
Between the peritoneum and the abdominal walls is а connective- tissue layer
containing а greater or lesser amount of fatty tissue. This space is called spatium
retroperitoneale.
5. The small intestine (intestinum tenue) begins at the pylorus, and ends at the beginning
of the large intestine. Mechanical and further chemical treatment of food under
conditions of an alkaline reaction occurs in the small intestine as well as absorption of
the nutriens.
Three parts are distinguished in the small intestine: 1) the duodenum, the part nearest to
the stomach; 2) the jejunum wich accounts for two fifth of the small intestine with the
exception of the duodenum; 3) the ileum, composing the remaning three fifth. There is no
clearly manifest anatomical boundary between the jejunum and ileum and their separation
is therefore relative.
6. The large intestine (intestine crassum) exteneds from the end of the small intestine to
the anus and is divided into the following parts: 1) caecum with
6
the vermiformis process; 2) ascending colon (colon ascendens) 3) transverse colon
(colon transversum); 4) descending colon (colon descendens); 5) sigmoid (pelvic)
colon (colon sigmoideum) and 6) rectum.
There are two large glands in the digestive tube: liver and pancreas.
The liver is primarily a large digestive gland secreting bile, which flows along the
efferent duct into the duodenum. It is weighing about 1500 g. The pancreas is
situated behind the stomach. Two components are distinguished in it: the main bulk
of the gland is concerned with external secretion and excretes its secretions into the
duodenum by way of the ducts; the smaller part of the gland consists of the islets of
Langerhans is an endocrine structure secreting insulin into the blood. Insulin
regulates the blood sugar content. There are indications that the pancreas
contributes to haemopoiesis and regulation of blood pressure.
The Digestive System 471
pancreaticus) receives numerous branches draining into'it almost at а right angle. It joins
the ductus choledochus and both open by means of а common orifice on the greater
duodenal papilla. This constructive connection of the pancreatic duct with the ductus
choledochus is determined by its functional significance (treatment of the duodenal
contents with the pancreatic juice) as well as by the development of the pancreas from the
part of the primary gut from which the duodenum also arises. In addition Со the main
duct, there is usually an accessory pancreatic duct (ductus pancreaticus accessorius),
which opens on the smaller duodenal papilla (about 2 cm above the greater duodenal
papilla). An accessory pancreas (pancreasaccessorium) is sometimes encountered, mostly
in the jejunal wall, less frequently in the wall of the stomach or ileum under the mucous or
serous coat; its size varies from several millimetres to 4-5 сш (such is the normal position
of the pancreas in some lower vertebrates). An annular pancreas is sometimes found, it
causes compression of the duodenum.
Structure. According Со structure, the pancreas is related to the group of acinar ог acinartubular glands.
Two components are distinguished in it: the main bulk of the gland is concerned with
external secretion and excretes its secretions into the duodenum Ьу way of the ducts; the
smaller part of the gland consists of the islets of Langerhans (insulae pancreaticae) and
is an endocrine structure secret- ing insulin ( insula island) into the blood; insulin
regulates the blood sugar content. There are indications that the pancreas contributes Со
haemopoiesis and regulation of blood pressure.
As а gland of mixed secretion, the pancreas receives numerous sources of nutrition,
namely the superior and inferior pancreaticoduodenal arteries, the splenic and left gastroepiploic arteries, etc. The veins of the нате name drain into the portal vein and small
veins draining into it. The lymph flows to the nearest nodes: coeliac, pancreaticolienal,
and others.
Innervation is accomplished from the solar plexus.
ТНЕ PERITONEUM
The peritoneum is а closed serous sac, which communicates with the external
environment only in females by means of а чету small abdominal opening of the uterine
tubes. Like any serous sac, it consists of two layers, parietal (peritoneum parietale) and
visceral (peritoneum visceral
e). The parie- tal layer lines the abdominal wall, while the visceral layer invests the viscera
and forms their serous covering for а shorter or longer distance. Both layers are in close
contact and in an intact abdominal cavity there is only а nar- row space between them
called the peritoneal cavity (cavum peritonei) that contains а small amount of serous
fluid; this fluid moistens the surface of the organs and so makes easier their movement
against one another. When air enters the cavity during operation or postmortem
examination or when pathological fluids accumulate in it, it acquires the lappearance of а
true, more or less large cavity.
The parietal peritoneum forms а continuous lining on the anterior and lateral walls of the
abdomen and passes on to the diaphragm and the
posterior abdominal wall. Неге it is reflected on the viscera and is directly continuous with
the visceral peritoneum investing them (Fig. 223).
Between the peritoneum and the abdominal walls is а connective- tissue layer containing а
greater or lesser amount of fatty tissue. This is the extraperitoneal tissue (tela subserosa),
which is developed irregularly. It is absent, for instance, in the region of the diaphragm but
is developed best on the posterior abdominal wall where it surrounds the kidneys, ureters,
adrenal glands, the abdominal aorta and vena cava inferior and their branches. On а
greater area of the anterior abdominal wall the extraperitoneal tissue is poorly developed,
but in the pubic region the amount of fat increases in it and the peritoneum is joined here
loosely with the abdominal wall. As а result, а distended urinary bladder pushes the
peritoneum away from <» ~~t~rinr яЫопппа1 wall and at а distance of about 5 cm above
the pubis
474 The Science of Vtscera
its anterior surface comes in ЙгесС contact with the abdominal wall. In the lower part of
the anterior abdominal wall the peritoneum forms йче folds converging on the umbilicus:
one unpaired medial umbilical fold (plica umbilicalis mediana) and two paired medial and
lateral umbilical folds (plicae umbilicales mediales and plicae umbilicales laterales) (Fig.
224).
These folds bound on each side two inguinal fossae (fossae inguinales) above the inguinal
ligament, which 'аге related to the inguinal canal. Immediately below the medial part of
the inguinal ligament is the femoral fossa, which corresponds to the position of the ring of
the femoral canal. Above the umbilicus the peritoneum passes from the anterior abdominal
wall and diaphragm Со the diaphragmatic surface of the liver to form the falciform
ligament of the liver between the two layers of which, at its free edge is lodged
ligamentum teres hepatis (obliterated umbilical vein).
Posteriorly of the falciform ligament the peritoneum is reflected from the inferior surface
of the diaphragm onto the diaphragmatic surface of the liver to form the coronary
ligament of the liver (lig. coronarium hepatis) whose edges have the shape of triangular
plates, which are known as the right and left triangular ligaments of the liver (lig.
triangulare dextrum and a'- nistrum). From the diaphragmatic surface of the liver the
peritoneum folds over its sharp border Со the visceral surface; then from the right lobe it
развея to the upper end of the right kidney as the hepatorenstl ligament (lig.
hepatorenale), from the hepatic porta Со the lesser curvature of the stomach as а thin
hepatogastric ligament (lig. hepatogastricum), and Со the рагС of the duodenum nearest
Со the stomach as the hepatoduodenal ligament (lig. hepatoduodenale). The
hepatogastric and hepatoduodenal ligaments are duplications of the peritoneum because
two peritoneal layers are encoun- tered in the region of the porta hepatis, one passing Со
the porta from the anterior рагС of the visceral surface of the liver and the other from the
poste- rior рагС. The hepatoduodenal and hepatogastric ligaments are а continua- tion of
one another and form together the lesser omentum (omentum minus). On the lesser
curvature of the stomach both layers of the lesser omentum separate, one to cover the
anterior and the other the posterior surface of the stomach. On the greater cur
vature they again join and descend in front of the transverse colon and the loops of the
small intestine to form the ante- rior lamina of the greater omentum (omentum majus).
On some level both layers fold over to ascend and form its posterior lamina (the greater
omentum consists, therefore, of four layers). On reaching the transverse colon the two
layers forming the posterior lamina of the greater omentum blend with the transverse
colon~ and its mesentery and together with the last патей pass posteriorly Со the anterior
border of the pancreas; here they separate, one passes upward and the other downward.
One covers the anterior surface of the pancreas and then ascends onto the diaphragm, the
other, having covered the inferior surface of the pancreas, is continuous with the
mesentery of the transverse colon, transverse mesocolon (тезосо1оп transversum).
~ In total adhesion of the anterior and posterior laminae of the greater omentum with the
transverse colon in an adult, five peritoneal layers (four omental layers and the visceral
peritoneum of the intestine) are thus fused on the tenia mesocolica.
The Digestive System 475
We shall now trace the course taken by the peritoneum, proceeding from the same layer on
the anterior abdominal wall, but not upward Со the dia- phragm, but in the transverse
direction. From the anterior abdominal wall the peritoneum extends Со line the lateral
walls of the abdominal cavity, passes to the posterior wall on the right and thus surrounds
completely the caecum and its vermiform process, which acquires а mesentery, the
mesentery of the vermiform appendix (mesenteriolum appendicis vermiformis). The peritoneum covers the ascending colon in front and on the sides, then the lower part of the
anterior surface of the right kidney, passes medially over the psoas muscle and ureter, and
at the root of the mesentery of the small intestine (radix mesenterii) is reflected to be
continuous with the right layer of this mesentery. Having supplied the small intestine with
а complete serous covering, the peritoneum is continuous with the left layer of the
mesentery. At the root of the mesentery the left layer of the mesentery is continuous with
the parietal peritoneum on the posterior abdominal wall. Then the peritoneum on the left
covers the lower part of the left kidney and approaches the descending colon, which is
related to the peritoneum in the same manner as the ascending colon. Still further laterally,
on the lateral abdominal wal), the peritoneum is again reflected on the anterior abdominal
wall. For easier understanding of the complex relations, the whole peritoneal cavity can be
separated into three regions, or storeys: (1) an upper storey bounded superiorly by the
diaphragm, and inferiorly by the mesocolon transversum; (2) а middle storey extending
downward from the mesocolon transversum to the entry into the true pelvis; the posterior
margin of the mesocolon transversum is attached to the posterior abdominal wall on а line
passing from the upper part of the right kidney through the beginning of the descending
part of the duodenum and the head of the pancreas and along the anterior border of the
pancreas to the upper part of the left kidney. On the anterior margin of the mesocolon
transversum stretches the transverse colon, which comes in contact with the anterior
abdominal wall. As а result, the upper storey of the abdominal cavity, for the whole
distance from the anterior to the poste- rior abdominal wall, is separated from the middle
storey by the mesocolon and the tra
nsverse colon suspended on it (the separation is not complete, however, because the two
storeys communicate by а narrow space between the transverse colon and the anterior
abdominal wall); (3) the lower storey begins at the line of entry into the true pelvis and
corresponds to the cavity of the true pelvis which is the lowest part of the abdominal
cavity.
1. The upper storey of the peritoneal cavity separates into three sacs: hepatic bursa (bursa
hepatica), pregastric bursa (bursa pregastrica), and omental bursa (bursa omentalis). The
hepatic bursa is related to the right lobe of the liver and is separated from the pregastric
bursa by the falciform 1щатепС of the liver; it is bounded posteriorly by the coronary
ligament of the liver. The upper end of the sight kidney with the adrenal. gland is palpated under the liver deep in the hepatic bursa. The pregastric bursa is related to the left lobe
of the liver, anterior surface of the stomach, and the spleen; the left part of the coronary
ligament passes on the posterior border of the left lobe of the liver; the spleen is
completely invested with the peritoneum except
The Science of Viecera
for the hilus, where the peritoneum passes from the spleen to the stomach as the
gastrosplenic ligament (ligamentum gastrolienale) and to the diaphragm as the lienorenal
ligament (ligamentum phrenicolienale).
The omental bursa, lesser sac of the peritoneum (bursa omentalis), is part of the general
peritoneal cavity lying behind the stomach and the lesser omentum. As it is indicated
аЬоче, the lesser omentum consists of two peri- | toneal ligaments, the hepatogastric
ligament passing from the visceral sur-] face of the liver and the porta hepatis to the lesser
curvature of the stomach, ' and the hepatoduodenal ligament connecting the hepatic porta
with the superior рагС of the duodenum. Between the layers of the hepatoduodenal
ligament pass the сотптлоп bile duct (on the right), the common hepatic artery (on the
left) and the portal vein (posteriorly and between these structures), as well as lymphatic
vessels, nodes and nerves.
The cavity of the omental bursa communicates with the general perito- neal cavity only by
means of а relatively narrow epiploic foramen, opening into the lesser гас (foramen
epiploicum). The foramen is bounded above by the caudate lobe of the liver, in front by
the free margin of the hepatoduode- nal ligament, below by the superior part of the
duodenum, behind by the peritoneal layer covering the vena cava inferior, which passes
here, and more laterally it is bounded by а ligainent passing from the posterior border of
the liver to the right kidney, the hepatorenal ligament (lig. hepatorenale). Part of the
omental bursa directly adjoining the epiploic foramen and situat- ed behind the
hepatoduodenal ligament is known as the vestibule of the omental bursa (vestibulum
bursae omentalis); it is bounded by the caudate lobe of the liver above and by the
duodenum and head of the pancreas below. The upper wall of the omental bursa is formed
by the inferior surface of the caudate lobe, with the papillary process suspended in the
bursa itself. The parietal peritoneum forming here the posterior wall of the omental bursa
covers the abdominal aorta, vena cava inferior, and the pancreas; it leaves the anterior
border of the pancreas and continues forward and downward as the anterior layer of the
mesocolon transversum, 'or, to ~Ье more Iprecise, the posterior lamina of the greater
omentum, fused with the шеяосо1оп transversum.
The greater omentum (omentum majus, s.
epiploon) hangs like an apron from the transverse colon and covers the loops of the small
intestine for а greater or lesser distance; it is thus пашей because fat is present in its
tissues (L omentum fat skin). It is formed of four peritoneal layers fused Со form two
laminae. The anterior lamina of the greater omentum consists of two peritoneal layers
descending from the greater curvature of the stomach in front of the transverse colon with
which they are fused; the рагС between the' stomach and the transverse colon is called the
gastrocolic ligament (liga- mentum gastrocolicum). These two layers of the omentum шау
descend |а
,front of the loops of the small intestine almost Со the level of the pubic bones and are
then reflected Со be continuous with the posterior lamina of
~ Galen described the omentum as а peritoneal fold swimming (epipleo) on the inte- stine.
The Digestive System
477
the omentum so that the entire thickness of the greater omentum consists of four layers.
Normally, the omental layers do not fuse with the loops of the small intestine. There is а
slit-like cavity between the anterior and poste- 'rior layers of the omentum, which
communicates above with the cavity of the omental bursa. In an adult, however, the layers
usually adhere one to
. another and the cavity of the greater оп~епЫш is obliterated on а conside- rable
distance, though in some cases it exists for some length between the layers of the greater
omentum along the greater curvature of the stomach.
2. The middle storey of the peritoneal cavity can be visualized when the greater omentum
and transverse colon are raised. Using as the bound- aries the ascending and descending parts of the colon on the sides апй the . mesentery of
the small intestine in the middle, this storey can be subdivided
into four compartments; between the lateral abdominal walls and the colon ascendens and
colon descendens are the right and left lateral canals (canales laterales dexter and
sinister); the space bounded by the colon is divided by the mesentery of the small
intestine, descending obliquely from left to right, into the right and left mesenteric sinuses
(sinus mesentericus dexter and sinus mesentericus sinister).
The mesentery (mesenterium) is а fold of two peritoneal layers by means of which the
small intestine is attached Со the posterior abdominal wall (Fig. 225). The posterior
margin of the mesentery attached to the abdom- inal wall is the root of the mesentery
(radix mesenterii). It is relatively short (f5-17 cm), whereas the opposite free end related to
the mesenteric part of the small intestine (jejunum and ileum) is the length of these two
segments. The line of attachment of the root passes obliquely from the left side of the
second lumbar vertebra to the right iliac fossa, transecting the
, terminal рагС of the duodenum, the aorta, vena cava inferior,,right ureter and psoas
major muscle. With а change in the position of the alimentary canal and growth of the
adjacent organs, the root of, the mesentery changes from а vertical position in the
embryonic period to an oblique position by the time of birth. Blood vessels, nerves,
lymphatic vessels and lymph nodes pass in the thickness of the mesentery between the two
serous layers con- taining more or less fatty tissue.
А series of peritoneal recesses are se
en on the posterior parietal perito- neum; these have practical importance because they
may be the place where retroperitoneal hernias form. Small pockets form at the junction of
the duo- denum and jejunum; they are the superior and inferior duodenal recesses
(recessus duodenalis superior and inferior). They are bounded on the right by the
duodenojejunal flexure, on the left by а peritoneal fold, the duode- nojejunal plica, passing
from the apex of the flexure to the posterior abdom- inal wall directly below the body of
the pancreas and containing the inferior mesenteric vein.
At the junction of the small intestine and the colon are two recesses, the inferior and
superior ileocaecal recesses (recessus ileocecalis inferior and superior), situated below
and above the ileocaecal fold passing from the ileum to the medial surface of'the caecum..
А recess in the parietal peritoneum lodging the caecum is called the
Lecture № 1
The Introduction of the General Anatomy. Methods of Investigation. Anatomy of
Locomotor System. The Human Skeleton. Development of Bones, Structural Features
and the Function of the Bones
The plan of lecture:
1. Subject of Anatomy. Approaches to Studing Anatomy.
2. Definition of a Skeleton (brief characteristics of components the skeleton).
Functions of a Skeleton.
3. Bone. Chemical Structure of Bone. Periosteum. Endosteum. Bone marrow.
Compact and Spongy Bones. Mechanical properties of Bones, their Form and
Peculiarities of the Structure.
4. Development of Bones (the ways of ossification, growth of bones in length and
thickness). Anatomy of Bone development.
5. Age features of bones.
Definition of a Skeleton (brief characteristics of components the skeleton).
Functions of a Skeleton
Skeleton - is anatomical structure. It consists of bones, skeletal cartilage, some
periarticular tissues, bone marrow and liquids (blood, lymph and intertissue liquid).
There are two parts in a skeleton:
- the axial part, including skull, vertebrae, ribs, breastbone, pelvis. It surrounds and
protects the important soft tissue - brain and spinal marrow, internal organs;
- the supplimentary skeleton is the skeleton of extremities.
The functions of a skeleton are as follows: supporting, protective, locomotor
(support of the body in space), metabolic, bloodmaking.
The bone consists of bone tissue and is covered with periosteum, involving bone
marrow.
There are different types of bones: tubular they are short and long, spongy (short),
flat (wide), mixed and pneumatic.
4
Bone. Chemical Structure of Bone. Periosteum. Endosteum. Bone marrow. Compact
and Spongy Bones. Mechanical properties of Bones, their Form and Peculiarities of
the Structure
Bones are specialised type of connective tissue undergoing various changes and
consists of cells and solid intercellular substance containing calcium salts.
Characteristics:
1. It is highly vascular
2. It is mineralised
3. It is hard and rigid and also somewhat resilient
4. It is constantly changing
5. It is regenerating capasity
6. It has a canalicular system for transport of nutrition
It may develop either by direct transformation of condenses mesenchyme or through
formation of a cartilaginous model which is later replaced by bone.
Functions:
1. It provides rigid structural framework of the body.
2. It provides area for attachment of muscles, and ligaments and also form a lever for
muscle movements.
3. It concerns protection of certain vital organs of body.
4. It contains bone marrow which manufactures blood cells.
5. It can act as store house for calcium and phosphorus.
Sructure of bone: Periosteum, Compact part, Spongy part, Medullary cavity.
I.
Periosteum – is a thick fibrous membrane covering the suface of bone exept the
articular surface. Structurally it consists of two layers: outer fibrous layer
consisting of white fibrous tissue, few osteoblasts and fat cells; inner
5
osteogenetic layer consists of elastic fibers. It contains osteoblasts in young bones and
help in subperiosteal bone formation.
II.
Compact Bone:
It is made of a number of cylindrical units called typical Secondary Osteones or
Haversian system which have a longitudinal orientation.
Each Haversian system consists of:
1.Haversian Canals – is a centrally located canals running parallel to long axis of
bone and contains nerves, blood vessels and lymphatics.
2.Concentric bony lamellae – It is made up of fine collagen bundles of calcified
matrix which surrounds the Haversian canal.
3.Lacunae- These are oval spaces between the lamellae and contain osteocytes.
III.Spongy Bone: It consists of irregular trabeculae of bone with bone cells but without
any Haversian systems. They form large narrow spaces.
IY. Endosteum: It is a vascular membrane which lines the medullary cavity and the
spaces of bongy bone.
Y. Bone Marrow: It is a soft vascular tissue found in the medullary cavity and spaces of
spongy bone. Two types 1.Red – It is blood cell formation marrow usually found in
middle of young bone and in flat bones. In the adult red bone marrow is contained
in the bones of the skull, in the ribs, in the thorax, the shoulder blade and clavicule,
in the spine, in the pelvis bones, and a small quantity of it can be found in tubular
bones. Reticular tissue forms the basis of the bone marrow. It is the predcessor of
blood elements- leucocytes, erithrocytes, and thrombocytes.2. Yellow (fatty)
marrow- It is mostly fat.
6
The histological structure of bone consists of two parts: 1.Bone cells, 2. Intercellular
substance or Matrix.
I Bone Cells: Osteoblasts, Osteocytes, Osteoclasts.
Osteoblasts – Bone forming cells. It is derived from undifferentiated mesenchym. They
secrete inorganic matrix around the cells. After ossification it becomes matured and
converted into osteocyte.
Osteocytes – Matured bone-cells.They have flattened body whith multiple processes and
live for 25 years. It get renewed every year in compact bone 2-2,5%, in spongy bone - up
to 10 % of cells.
Osteoclasts – Bone destroying cells.
II. Intercellular substance:
1. Organic – collagen fibes and cement substence.
2. Inorganic – important elements as bone salts – Calcium, magnesium, phosphate,
carbonate, fluoride and citrate.
Different types of Bone:
I.
Long Bone. They have two ends: Epiphysis and one shaft- Diaphysis They are
covered with cartilage and serve for connection with other bones. The part between
diaphysis and epiphysis is called metaphysis. On a surface of bone foramina nutricia are
located. ( Humerus, radius, ulna, femur,tibia and fibular.)
I.
Short Bones ( examples are Carpals and Talus).
II.
Flat Bones- plate-like and actually consists of two outer plates of compact bone
within which lie spongy bone and marrow.( examples are scapula, sternum, ribs, and
bones of vault of scull.
7
III.
Pneumatic Bones: Special type of irregular bones containing air sinus, i.e. air filled
spaces within it. Examples: Maxillar, Frontal, Sphenoid and Ethmoid.
IV.
Sesamoid Bones: are those bones which are formd in the tendons of muscles.
Mechanical characteristics of the bone. The bone is a very strong tissue. It is
capable of maintaining large mechanical loads. It is experimentally proved, that the
tension strenght of the bone is 10-12 кg per mm2, and compression strength is 12-16 кg
per mm2. The bone is 5 times as strong as concrete, and is well adapted to various loads.
Development and growth of theBones
The skeleton develops from germ connective tissue - mesenhima. Then the large part
of the skeleton becomes cartilaginous. Then cartilage is destroyed and becomes the bone.
In this way the bones of the body, extremities and the basis of the scull are developted.
The bones of the fornix of the scull and some face bones develop insted of mesenchimal
germ. They are called connective tissue. Such as parietalis,
frontalis, occipitalis, squama and tympany of temporalis bone, and also lacrimalis, nasalis ,
and vomer.
The process оf the bone ossification begins with the formation of ossification
points, where the centres of future bones are located.
The development and growth of the bones in the place of the cartilage occurs at the
process of periosteal and enhondral ossification.
8
The growth of the bone in length take place from metaphysis. In the end of growth
of the body the cartilage is completely оssified. Growth in width take place by
appositional growth and subperiosteal bone deposition occurs in succesive layer.
Factors for Bone growth
I.Metabolic factors: 1.Diet – should consist of calcium, phosphorous 2. Hormonens
II. Genetic factors
III. Mechanical factors
Аge features of the bone
The skeleton is a very labile formation. It adopts to physical loads increased and its
structure changes.
Many human bones are originated and developed as several parts. Then they are
joined and form a single bone. For example, pelvis develops as three big parts: pubis,
ischii, ileum.
The bones of the skull are originally separeted bordered with the sutures
and then become closed..
In children up to 4-5 years of age only red bone marrow can be found in the bonemarrow chanel.
In the course of years the content of mineral substances increase resulting in their
fragility. The connection of the bones to occurs the skull bone sutures close, red bone
marrow in tubular bone channels becomes yellow. The bones become
lighter and atrophied because of the decrease muscle extertion. Thus, to maintain physical
condition one should do physical exercises throughout his life.
Lecture №3
The Structures Composing the Joints. Classification of Joints.
Plan of the Lecture:
1. The Structures Composing the Joints.
2. Classification of the Joints.
3. The Kinds of Movement admitted in Joints.
4. Different Kinds of the Joints.
The various bones of the Skeleton are connected together at different parts of their surfaces, and
such a connection is designated by the name of Joint or Articulation. If the Joint is immovable as
between the cranial and most of the facial bones, the adjacent margins of the bones are applied in
almost close contact, a thin layer of fibrous membrane, the sutural ligament, and at the base of the
skull. But in certain situations, a thin layer of cartilage is interposed.Where slight movement is
required, combined with great strength, the osseous surfaces are united by tough and elastic fibrocartilages, as in the joints between the vertebral bodies and in the interpubic articulation. But in the
movable joints, the bones forming the articulation are generally expanded for greater convenience of
mutual connection, covered by cartilage, held together by strong bands or capsules of fibrous tissue,
called ligaments, and partially lined by a membrane, the synovial membrane, which secrets a fluid to
lubricate the various parts of which the joints is formed: so that the structures which enter into the
formation of a movable joint are bone, cartilage, fibro-cartilage, ligament, and synovial membrane.
And so, a joint is an articulation – the place of union or junction between two or more bones
or parts of bones of the skeleton. Joints exibit a variety of form and functions. Some
2
joints have no movement; others allow only slight movement, and some are freely movable, such as
the shoulder joint.
The three types of joint are classified according to the maner or type of material by which the
articulating bones are united.
Classification of the Joints
The articulations are divided into three classes: synarthrosis, or immovable; amphiarthrosis, or
mixed; and diarthrosis, or movable joints.
1. Synarthrosis. Immovable Articution.
Synarthrosis includes all those articulationis in which the surfaces of the bones are in almost direct
contact, fastened together by an intervening mass of connective tissue or hyaline cartilage, and in
which there is appreciable motion, as the joints between the bones of the cranium and face,
excepting those of the lower jaw.
Sutura (a seam) is that form of articulation where the contiguous margins of flat bones are united
by a thin layer of fibrous tissue. It is met with only in the skull. When the articulating surface are
connected by a series of processes and indentations interlocked together, it is termed a true suture (
sutura vera); of which there are three varieties: sutura dentata, serrata, and limbosa.
Gomphosis (a nail) is an articulation formed by the insertion of a conical process into a socket, as a
nail is driven into a board; this is not illustrated by any articulation between bones, properly so
called, but is seen in the articulation of the teeth with the alveoli of the maxillary bones.
Synchondrosis.-Where the connecting medium is cartilage the joint is termed a synchondrosis. This
is a temporary form of joint, for the cartilage becomes converted into
3
bone before adult life. Such a joint is found between the epiphyses and shafts of long bones, and in
the junction between the occipital bone and the sphenoid and between the petrous portion of the
temporal bone and the jugular procces of the occipital bone.
2. Amphiarthrosis. Mixed Articulations.
In this form of articulation only a slight amount of movement is possible, the contiguous
osseous surfaces being either connected together by broad flattened discs of fibro-cartilage, of a
more or less complex structure, which adhere to each bone, as in the articulation between the bodies
of the vertebrae, and in the pubic symphysis. This is termed Symphysis. Or, secondly, the bony
surfaces are united by an interosseous ligament, as in the inferior tibio-fibular articulation. To this
the term Syndesmosis is applied. The interosseus membrane is the forearm is a sheer of fibrous
tissue that joint the radius and ulna is a syndesmosis.
3. Diartrosis. Movable Articulations or Synovial joints.
This form of articulation includes the greater number of the joints in the body, mobility being their
distinguishing character. They are formed by the approximation of two contiguous bony surfaces,
covered with cartilage, connected by ligaments, and lined by synovial membrane.
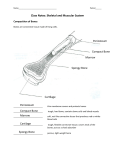
The synovial joints – name – comes from the labricating substance (synovial fluid) that is in the
joint cavity or synovial cavity, which is lined with a synovial membrane consists of vascular
connective tissue that produces synovial fluid (fig. 1).
The three distinguishing features of a synovial joint are:
-
a joint cavity;
-
bone ebds covered with articular cartilage;
-
articulating sufaces and joint cavity enclosed by an articular capsule
(fibrous capsule lined with synovial membrane).
Synovial joints are usually reinforced by accessory ligaments that are either separete (extrinsic)
or are a thickening of a portion of the articular capsule (intrinsic).
4
Some synovial joints have other distinguishing features such as fibrocartilating articular disc,
which are present when the articulating surfaces of the bones are incongruous.
The six major types of synovial joint are classified according to the shape of the articulating
surfaces and (or), the type of movement they permit.
Plane joints (for exsampule the acromioclavicular joint between the acromin of the scapula and
the clavicle) are numerous and are nearly aways small. They permit gliding or sliding movements.
The opposed sufaces of the bones are flat or almost flat. Most plane joints allow movement in only
one plane (axis); hence joints uniaxial joints. Movement of plane joints is limited by their tight
articular capsules.
Hinge joints move in one plane (sagittal) around only one axis (uniaxial) that runs transversely
between the bones involved (the elbow joint). Hinge joints permit flexion and extensoin, only. The
artiular capsule of these joints is thin and lax anteriorly and posteriorly where movement occurs;
however, the bones are joined by strong, laterally placed collateral ligaments.
Sadlle joints are biaxial with opposing surfaces shaped like a saddle. The carpometacarpal joint
at the base of the 1st digit (thumb) is a saddle joint.
Codyloid joints are also biaxial and allow movement in two planes, sagittal and frontal (coronal)
(the metacarpophalangeal joints); however, movement in one axis (sagittal) is usually greater (freer)
than in the other. Their two axes lie at right angles to each other. Condyloid joints permit flexion and
extension; abduction and adduction, and circumduction.
Ball and socket joints are multiaxial (polyaxial); they move in multiple axies and in mulitple
planes. In these highly movable joints (the hip joint), the spheroidal surface of one bone moves
within the socket of another (the head of the femur in the acetabulum of the hip bone). Flexion and
extension, abduction and adduction, medial and lateral rotation, and circumduction can occur at ball
and socket joints.
5
Pivot joints are uniaxial and allow rotation. In these joints, around process of bone of bone
rotates within a sleeve or ring. Examples include the rotation of the radius during pronation and
supination of the atlas (C1 vertebra) around the dens (odontoid process) of the axis (C2 vertebra)
during rotation of the head at the atlantoaxial joint.
The Kinds of Movement admitted in Joints
The movements admissible in joints may be divided into four kinds: gliding, angular,
circumduction, and rotation. However, these movements are often, more or less combined in the
various joints, so as to produce an infinite variety, and it is seldom that we find only one kind of
motion in any particular joint.
Gliding movement is the simplest kind of motion that can take place in a joint, one surface gliding
or moving over another without any angular or rotatory movement.
Angular movementjccurs only between the long bones, and by it the angle between the two
boners is increased or diminished. It may take place in four directions: forwards and baskwards,
constituting flexion and extension, or inwards and outwards, from the mesial line of the body,
constituting adduction and abduction.
Circumduction is that degree of motion which takes place between the head of a bone and its
articular cavity, while the limb is made to circumscribe a conical space, the base of which
corresponds with the inferior extremity of the limb, the apex with the articular cavity; this kind of
motion is best seen in the shoulder-and hip-joints.
Rotation is the movement of a bone around an axis; the latter may be formed by a separate
bone, as in the case of the pivot formed by the odontoid process of the axis around which the atlas;
or a bone may rotate around its own longitudinal axis, as in the rotation of the
6
humerus and femur at the shoulder-and hip-joints respectively and other. Such movements are called
supination and pronation.
Different Kinds of the Joints
1. Temporomandibular Joint (TMJ).
The TMJ is a modified hinge type of joint. The articular surface involved are the condyle of the
mandible, the articular tubercle of the temporal bone, and the mandibular fosse. The articular
capsule of the TMJ is loose. The fibrous capsule attaches to the margins of the articular area on the
temporal bone and around the neck of the mandible. The joint has two synovial membranes:
the superior synovial membrane lines the fibrous capsule superior to the articular disc;
The inferior synovial membrane lines the capsule inferior to the dick.
The articular disk divides the joint into two separate compartments. The thick part of the articular
capsule forms the intrinsic lateral ligament (ligamentum temporomandibularis), which strengthens
the TMJ laterally and, with the postglenoid tubercle, acts to prevent posterior dislocation of the
joint.
Two extrinsic ligaments and the lateral ligament connect the mandible to the cranium. The
stylomandibular ligament – runs from the styloid process to the angle of the mandible. The
sphenomandibular ligament runs from the spine of the sphenoid to the lingula of the mandible.
The movements of the mandible at the TMJ are as follows: Depression (open mouth), Elevation
(closed mouth), Protrusion (protraction of chin).
2. Joints of the Vertebral Bodies.
7
The joints of the vertebral bodies are secondary cartilaginous joints (symphyses) designed for
weightbearing and strength. The articulating surfaces of adjacent vertebrae are connected by IV
discs and ligaments. Each IV disc consists of:
An anulus fibrosus – an outer fibrous part – composed of concentric lamellae of fibrocartilage;
A gelatinous central mass – the nucleus pulposus.
There are two ligaments in the joints of the vertebral bodies: the anterior longitudinal lig. Is a strong
and connects the anterolateral aspects of the vertebral bodies and IV discs.The posterior
longitudinal lig. Somewhat weacer bend then the anterior longitudinal lig. It runs within the
vertebral canal along the posterior aspect of the vertebral bodies.
3. Joints of the Vertebral Arches.
These articulations are plane synovial joints between the superior and inferior articular processus
of adjacent vertebrae.
Ligaments of the intervertebral joints are as follows:the ligament flava (yellow elastic fibrous
tissue), the interspinous lig., the supraspinous lig., the nuchal lig., the intertransverse lig.
Joints of the Lower Limb.
1.Hip Joint.
The hip joint forms the connection between the lower limb and the pelvis girdle. It is a strong and
stable multiaxial ball – and socket type of synovial joint – the femoral head is the ball and the
acetabulum is the socket. The round head of the femur articulates with the cuplike acetabulum of the
hip bone. Because the depth of the acetabulum is increased by the fibrocartilaginous acetabular
labrum, which attaches to the bony rim of the acetabulum and the transverse acetabular lig., more
than half of the head fits within the acetabulum. The central and inferior part of the acetabulum, the
acetabular fossa, is thin, nonarticular, and often translucent.
8
The ligaments of the hip joint are as follows: the iliofemoral lig.; the pubofemoral lig.; the
ischiofemoral lig.; the lig. of the head of the femur.
Movements of the hip joint are as follows: flexion, extension, abduction, adduction, rotation.
2. Knee Joint (KJ).
The articular surfaces of the KJ are characterized by the large size and their complicated and
incongruent shapes. The KJ consists of three articulations:
lateral and medial articulations between the femoral and tibial condyles;
intermediate articulation between the patella and femur.
The fibula is not involved in the KJ.
Extracapsular Ligaments of the Knee Joint. The fibrous capsule is strengthened by five
extracapsular lig.: the patellar lig., the tibial collateral lig., the fibular collateral lig., the oblique
popliteal lig., the arcuate popliteal lig.
Intracapsular Ligaments of the Knee Joint: there are two cruciate ligaments in the KJ - anterior
and posterior. The cruciate ligaments are locatied in the center of the joint and cross each other
obliquely like letter X, providing stability to the KJ.The coronary lig. are capsular fibers that attach
the margins of the menisci to the tibial condyles, and also transverse lig. of the KJ.
There are two menisci in the KJ: the medial men. and lateral men. The menisci of the KJ are
crescentic plates of fibrocartilage on the articular surface of the tibia that deepen the surface and act
like shock absorbers. The Greek word meniskos means crescent.
Movements of the KJ: flexion, rotation, extension.
3. Ankle Joint (AJ) .
The ankle joint (talocrural articulation) is located between the distal ends of the tibia and fibula
and the superior part of the talus. The tibia articulates with the talus in two places:
9
its inferior surface forms the roof of the mortise;
its medial malleolus articulates with the medial surface of the talus.
Ligaments of the AJ: the lateral lig. consists of the anterior talofibular lig., the posterior talofibular
lig., and the calcaneofibular lig. Medial lig.(deltoid lig.) consists of tibionavicular lig., anterior and
posterior tibiotalar ligg. and tibiocalcaneal lig.
Movements of the AJ: dorsiflexion, plantarflexion.
Joints of the Upper Limb.
1. Glenohumeral (Shoulder) Joint (GJ)
The GJ is a ball-and-socket type of synovial joint that permits a wide range of movement;
however the mobility it the relatively unstable. The large, round humeral head articulates with the
relatively shallow glenoid cavity of the scapula, which is deepened slightly but effectively by the
ringlike, fibrocartilaginous glenoid labrum. The synovial membrane lines the fibrous capsule and
reflects from it onto the glenoid labrum and neck of the humerus, as far as the articular margin of the
head. The synovial memrane also forms a tubular sheath for the tendon of the long head of the
biceps brachii, where it passes into the joint cavity and lies in the intertubercular groove, extending
as far as the surgical neck of the humerus.
Ligament of the GJ is the coracohumeral.
Movements of the GJ: Flexion-extensjon, abduction-adduction, rotation, circumduction.
Elbow Joint (EJ).
The EJ – a hinge type of synovial joint – is located 2 to 3 cm inferior to the epicondyles of the
humerus. The spool-shaped trochlea and spheroidal capitulum of the humerus articulate with the
trochlear notch of the ulna and the slightly concava superoir aspect of the head of the radius,
respectively; therefore, there are humeroulnar and humeroradial articulations.The articular capsule is
weak anteriorly and posteriorly but is strengthened on each side by collateral ligaments.
10
Ligaments of the EJ are the radial collateral lig. and the ulnar collateral lig.
Movements of the EJ are flexion and extension.
Wrist Joint.
The wrist joint (radiocarpal) is a condiloid type of synovial joint. The position of the joint is
indicated approximately by a line joining the styloid processus of the radius and ulna. The distal
ends of the radius and the articular disc of the distal radioulnar joint articulate with the proximal
row of carpal bones, except for the pisiform.
Ligaments of the wrist joint are the palmar radiocarpal lig., the dorsal radiocarpal lig., ulnar
collateral lig., radial collateral lig.
Movements of the wrist joint are flexion-extension, abduction-adduction and circumduction.
Lecture №5
Muscles and Fasciae of the Head and Neck. Triangles of the Neck
Muscles of the head are divided into two groups: chewer muscles and mimic
muscles.
Chewer Muscles
The Masseter – is a short thick muscle consisting of two portions: superficial and
deep.
The Temporal – is a broad radiating muscle, situated at the side of the head and
occupying the entire extend of the temporal fossa.
The External pterygoid – is a short, thick muscle somewhat conical in form, which
extends almost horisontally between the zygomatic fossa and the condyle of the jaw.
The Internal pterygoid – is a thick, quadrilateral muscle and resembles the
masseter in form. It arises from the pterigoid fossa.
The Temporal, Masseter and Internal pterygoid rise the lower jaw against the upper
with great force. The superficial portion of the Masseter assists the External pterygoid
in drawing the lower jaw.
All Chewer muscles are supplied by the third branch of the n.trigemins (trigeminal
nerve). Contracture of all chewer muscles and at least one of them inevitably causes the
immobility of the lower jaw. This is termed as trismus (lock jaw) in stomatology.
There are many spaces, which are filled with fatty tissue. These spaces play an
important role in spreading inflametion processes and hematomas. These spaces are
limited by facies:
1. Parotid fascia (f.parotidea). It covers parotid glands. In front of this gland parotid
fascia covers masseter muscle and is called masseteric fascia (f. masseterica).
2. Masseteric f. F. covering the masseter muscle, part of which attaches below the
parotid gland at the upper end of the zygomatic arch.
3. Buccopharyngeal fascia. It lies on the buccinator muscle and expends from the
angel of the mouth.
4. Temporal F. It consists of the two layers.
a) superficial layer. It attached to the outer margin of the zygomatic arch;
b) deep layer. Layer of the temporal f., attached to the inner margin of the
zygomatic arch.
Mimic muscles ( Muscles of Facial Expression)
There are muscles of facial expression around the eyes, ears,nose and mouth
blending into the upper lip,lower lip chin and cheek.
The muscles of the face are in the subcutaneous tissue; most of them attach to the
skull bones and the skin or mucous membrane. They move the skin and change facial
expressions to convey mood. These muscles are in the anterior and posterior scalp,
face, and neck. All muscles of facial expression develop from the 2 nd pharyngeal arch
and are supplied by its nerve, the 7th cranial nerve.
Muscles of the Forehead
The frontalis is the anterior part of the scalp muscle – the occipitofrontalis. The
frontal belly of this muscle aries from the anterior part of the epicranial aponeurosis and is
attached to the skin of the eyebrows. The frontalis has no bony attachments; it elevates
the eyebrows, giving the face a suprised look, and produced transverse wrinkles in the
forehead when one frowns.
Muscles of the Mouth, Lips, and Cheeks
Several muscles alter the shape of the mouth and lips. The shape of the mouth and
lips is controlled by a complex three-dimensional group of muscllar slips:
elevators, retractors, and evetors of the upper lip;
- depressors, retractors, and evertors of the lower lip;
- a compound sphincter around the mouth;
- the buccinator in the cheek.
At rest lips are in gentle contact and the teeth are close together.
The muscles: m. Orbicularis oris, dilator muscles, m. Mentalis, mm. Levator labii
superioris alaeque nasi, m. Buccinator, m. Depressor anguli oris, m. Levator
anguli oris, mm. Zigomaticus major et minor, mm. Levator labii superioris and
inferioris, m. Depressor labii superioris, m. Depressor labii inferioris, m Risorius.
Muscles Around the Orbital Opening
The function of the evelids is to protect the eye from injury and excessive light. The
eyelids also keep the cornea moist by spreading the tears.
The m. Orbital oculi closed the eye and wrinkles the forehead vertically. The m.
Orbicularis oculi consists of three parts;
- the lacrimal part;
- the palpebral part;
- the orbital part.
The m. Corrugator supercilii aries from the orbital part of the m. Orbicularis oculi and
nasal prominence and inserts into the skin of the eyebrow.
Muscles Around the Nose
All muscles around the nose are supplied by the facial nerve. The m.Procerus and m.
Depressor septi are reletively unimportant to most health care professionals. The
nasals. The main muscle of the nose, consists of transverse
and alar parts. The transverse part arises from the superior part of the canine ridge on
the anterior surface of the maxilla, superior to the incisor teeth. The alar
part arises from the maxilla superior to the transverse part and attaches to the alar
carilages of the nose.
All mimic muscles are supplied by facial nerve. When innervation of mimic muscles
is distored there appear a mask-like face.
Muscles of the Neck
The muscles of the neck may be arranged into groups corresponding to the region in
which they are situated:
1. Superficial region: 1.Platysma myoides 2.Sterno-cleido-mastoid
2. Suprahyoid region: 1.Digastric
2.Stylo-hyoid
3.Mylohyoid
4.Geniohyoid
3. Infrahyoid region: 1.Sternohyoid
2.Sternothyroid
3Thyrohyoid
4.Omohyoid
4. Anterior Vertebral region: 1.Rectus capitis anticus maior
2.Rectus capitis anticus minor
3.Rectus capitis lateralis
4.Longus colli
5. Lateral Vertebral region: 1. Scalenus anterius
2. Scalenus medius
3. Scalenus posterius
Superficial and Lateral Muscles of the Neck
Three superficial and lateral muscles are in the neck: platysma, sternoclaidomastoid
(SCM), and trapesius. The platysma, like the facial and skalp muscles, develops form a
continuous sheet of musculature that derives from mesenchyme in the 2 nd pharyngeal
arch of the embryo. The platysma and facial muscles are supplied by branches of the
facial nerve, which supplies the 2nd embryonic pharyngeal arch. Likewise, the trapezius
and sternomastoid muscles are derived from the same embryonic muscle mass and are
both supplied by the accessory nerve.
Deep Structures of the Neck
Prevertebral Muscles.
The anterior and lateral vertebral or prevertebral muscles, posterior to the
prevertebral layer of deep cervical fascia, lie in the floor of the anterior and posterior
triangles of the neck. The anterior vertebral muscles, consisting of the longus colli and
capitis and rectus capitis anterior and lateralis, are related to the anterior triangle, and
the lateral vertebral muscles, consisting of the splenius capitis, levator scapulae, and
scalene muscles (anterior, middle, and posterior), are related to the posterior triangle.
There are longus colli and capitis, rectus capitis anterior and lateralis, splenius
capitis, anterior middle, and posterior scalene, levator scapule muscles on the neck.
Triangles of the Neck
To facilitate description of cervical anatomy, each side of the neck is divided into
two triangles, anterior and posterior, by the obliquely placed SCM. The posterior
triangle of the neck has:
- an anterior boubdary, formed by the posterior border of the SCM ;
- a posterior boundary, formed by the anterior border of the trapezius;
- an inferior boundary, formed by the middle third of the clavicle between the trapezius
and SCM;
- its apex, where the SCM and trapezius meet on the superior nuchal line of the occipital
bone;
- a roof, formed by the investing leyer of deep cervical fascia;
- a floor, formed by muscles covered by the prevertebral layer of deep cervical fascia.
The posterior triangle is subdivided into the omoclavicular
and omo-trapesoid
triangles.( trigonum omoclaviculare and omotrapesoideum)
The anterior tiangle of the neck has:
- an anterior boundary, formed by the median line of the neck;
- a posterior boundary, formed by the anterior of the SCM;
- a superior boundary, formed by the inferior border of the mandible;
- its apex, at the jugular notch in the manubrium;
- a roof, formed by subcutaneous tissue containing the platyzma
- a floor, formed by the pharynx, laryx, and thyroid gland.
The anterior triangle is subdivided into three triangles: trigonum submandibulare,
caroticum and trigonum omotracheale.
Fascia of the Neck
Fascia is the collective term for connective tissue layers of the neck:
1. Superficial layer ( f. superficialis). It surrounds the platisma
2. Lamina superficialis f. colli propria is surround the sterno-cleido-mastoideus, and
trapezius muscle. It is attached to the anterior magin of the manubrium.
3. Lamina profunda f. colli propria. It is connective tissue investing the neurovascular
bundle (carotid artery, jugular vein, vagus nerve) and continuos with the pretracheal
layer.
4. F. endocervicalis ( or pretracheal layer) consists of two layers ( parietal and
visceral). It spreads between the two omohyoid muscles and is attached to the
posterior margin of the manubrium and clavicle.
5. F. prevertebral is a layer that lies between the vertebral column and pharyngeal
constrictors.
Lecture №6
Clinical Anatomy of “ weak places” of the Body
Plan of the Lecture:
1. Abdominal Cavity.
2. Anterolateral Abdominal Wall:
a) Fascia of the Anterolateral Abdominal Wall;
b) Muscles of the Anterolateral Abdomenal Wall.
3. Abdominal Hernias.
The abdominal cavity is the lower part of the trunk between the thorax and pelvis. It
has musculotendinous anteriolateral wall, and posterior wall which is formed by bones,
muscles and fasciae. The diaphragm forms the roof of the abdominal cavity. Some
abdominal organs – the spleen, liver, part of the kidneys, and stomach – are protected
by the abdominal cavity.
Constituent Layes of Abdominal Wall from outside on wards:
1. Skin, 2. Superficial Fascia, which consists of two layers in many regions a)
Superficial – fatty, b) Deep membranous. 3. Muscles in some regions covered by
fasciae. 4. F. abdominal propria which surrounded muscles of the abdominal. 5. The
deep layer of f. endoabdominalis covered abdominal cavity inside.
2
Muscles of the Anterolateral Abdomenal Wall
Trere are five muscles in the anterolateral abdominal wall: three flat mucles and two
vertical muscles.
The three flat muscles of the anterolateral abdomenal wall are the:
- external oblique;
- internal oblique;
- transverse abdominal.
The two vertical muscles of the anterolateral abdomenal wall are within the rectus
sheath:
- rectus abdominis;
- pyramidalis.
The aponeurouses of three lateral muscles form Linea alba (white line). It is a fibro
tendinous raphe situated in the median line in front of abdominal wall and extends from
xiphoid process to symphysis pubis.
The aponeuroses of External, Internal oblique and Transversus abdominis form
Rectus sheath ( Vagina m. recti abdominis). At different levels it is formed in different
ways. Upper umbilicus:
Anterior wall: 1. Aponeurosis of External oblique muscle of abdomen.
2.Anterior lamella of Internal oblique muscle of abdomen.
Posterior wall: 1. Posterior lamella of aponeurosis of Intern. oblique
2. Aponeurosis of Transversus abdominis
3. Fascia Transversalis
3
Region below umbilicus
Anterior wall:
1. Aponeurosis of External oblique.
2. Aponeurosis of Internal oblique
3. Aponeurosis of Transversus abdominis
Posterior wall – deficient and Rectus abdominis lies directly on transversalis fascia
Arcuate line – is the lower free concave margin of posterior wall of wall of rectus
sheath situated at the mid point of umbilicus and symphysis pubis. Below this level the
posterior wall of rectus sheath is deficient.
The linea alba contains the umbilical ring, a defect in the linea alba through which
the fetal umbilical evssels pass to and from the umbilical cord and placenta.
Lumbul triangle is weak area of the back borded by the latissimus dorsi, external
oblique and iliac crest.
Inguinal canal situated in lower part of anterior abdominal wall about half an inch
above and parallel to medial half of inguinal ligament. Length of this canal-4cm.
Contents:
In male – Spermatic cord; ilioinguinal nerve.
In Female – Round ligament of Uterus; Ilioinguinal nerve.
Walls of Inguinal canal:
1.Inguinal ligament – inferiorly
2.External oblique aponuerosis– anterioly
3.Internal oblique and transversus abdom. muscle – upper
4
4.Transversalis fascia – posteriorlly.
Superficial inguinal ring ( annulus ingvinalis superfis) – external opening
of the inguinal canal
2. Crus mediale – group of fibers of the external oblique aponuerosis ascending
obliquely medial to the superficial inguinal ring
3. Lateral crus – group of fibers of the external oblique aponeurosis ascending lateral
to the superficial inguinal ring
4. Reflected ligament ( lig.reflexum) – Curved band of fibers passing upward from the
medial attechment of the inguinal ligament and forming the medial lining of the
superficial inguinal ring.
5. Intercrural fibers ( f. intercrurales) – curved fibers between the medial and lateral
crura.
Deep inguinal ring ( annulus inguinalis profundus) – inner inguinal ring at the
transition of the transversalis fascia into the internal spermatic fascia.
Abdominal Hernias
The anterolateral abdominal wall may be the site of hernias. Most hernias occur in
the inguinal, umbilical, and epigastric regions. Umbilical hernias are common in
newborns because the anterior abdominal wall is relatively weak in the umbilical ring,
especially in low-birth-weight infants. Umbilical hernias are usually small and result
from increased intra-abdominal pressure in the presence of weakness and incomplete
closure of the anterior abdominal wall after ligation
of the umbilical cord at birth. Herniation occurs through the umbilical ring – the
oppening in the linea alba. Acquired umbilical hernias occur most commonly in
5
women and obese people. An epigastric hernia – a hernia in the epigastric region
through the linea alba – occurs in the midline between the xiphoid process and the
umbilicus. Epigastric hernias tend to occur in people older than 40 years and are
usually associated with obesity. Inguinal hernia may form in the region of superficial
inguinal ring or deep inguinal ring.
Lecture №7
The Types of Muscles of the Extremities and their Functions. Surface Forms of
Muscles of Extremities and their Clinical Role
Plan of the Lecture:
1. Anterior Thoracoappendicular Muscles of the Upper Limb.
2. Muscles of the Arm, of the Forearm, and of the Hand.
The upper limb (extremity) is characterized by its mobility and ability to grasp and
manipulate. These characteristics are especially marked in the hand (manus) when
performing manual activities such as buttoning a shirt. Because the upper limb is not
usually involved in weightbearing, its stability has been sacrificed to gain mobility. The
digits (fingers including the thumb) are the most mobile, but other parts are still more
mobile than comparable parts of the lower limb.
The upper limb consists of four segments:
- pectoral girdle – the bony ring, incomplete posteriorly, formed by the scapulae and
clavicles, which is completed anteriorly by the manubrium of the sternum;
- arm –the part between the elbow containing the humerus, which connects the shoulder
and the elbow;
- forearm – the part between the elbow and wrist containing the ulna and radius, which
connect the elbow and wrist;
2
- hand – the part of the upper limb distal to the forearm containing the carpus,
metacarpus, and phalanges, which is composed of the wrist, palm, dorsum of hand, and
finges including the thumb.
Anterior Thoracoappendicular Muscles of the Upper Limb
Four anterior thoracoappendicular (pectoral) muscles move the pectoral girdle:
pectoral major, pectoral minor, subclavius, and serratus anterior.
The pectoral major, large and fan shaped, covers the superior part of the thorax. The
latter head is much larder, and its lateral border is responsible for the muscular mass that
forms most of the anterior wall of the axilla, with its inferior border fopming the anterior
axillary fold. The pectoralis major and adjacent deltoid form the narrow deltopectoral
groove, in which the cephalic vein runs. The pectoralis major is a powerful adductor of the
arm and a medial rotatot of the humerus.
The pectoral minor lies in the anterior wall of the axilla, where it is lardely covered
by the much larder pectoralis major. The pectoralis minor stabilizes the scapula and is
used when stretching the arm forward to touch an object that is just out of reach. The
pectoral minor is a useful anatomical and surgical landmark for structures in the axilla.
The subclavius lies almost horizontally when the arm is in the anatomical position.
This muscle is located inferior to the clavicle and affords some protection to the suclavian
artery when the clavicle fractures.
3
The serratus anterior overlies the lateral part of the thorax and forms the medial wall
of the axilla.
Scapulohumeral Muscles.
The six scapulohumeral muscles (deltoid, teres major, teres minor, supraspinatus,
and subscapularis) are relatively shot muscles that pass from the scapula to the humerus
and act on the glenohumeral (shoulder) joint.
Axilla.
The axilla (armpit) is the pyramidal space inferior to the scapulohumeral joint and
superior to the axially fascia at the junction of the arm and thorax. The axilla has an apex,
a base, and four walls, three of which are muscular:
- anterior wall of axilla is formed by the pectoralis major and pectoralis minor and the
pectoral and clavicopectoral fascia associated with them;
- posterior wall of axilla is formed by the scapula and subscapularis on its anterior
surface and inferiorly by the teres major and latissimus dorsi;
- medial wall of axilla is formed by the thoracic wall and the overlying serratus anterior;
- lateral wall of axilla is a narrow bony wall formed by the intertubercular groove in the
humerus.
The axilla contains axillary blood vessels (axillary artery and its branches, axillary vein),
lymphatic vessels, and several groups axillary lymph nodes. The axilla also contains large
nerves of the brachial plexus.
4
Muscles of the Arm, the of Forearm, and of the Hand
The arm extends from the eblow. Two types of movement occur between the arm abd
forearm at the elbow joint: flexion-extension and pronation0supination. The muscles
perfoming these monements are clearly divided into anterior and posterior groups.
Of the four arm (brachial) muscles, three flexors (biceps brachii, brachialis,
coracobrachialis) are in the anterior compartments and one extensor (triceps brachii) is in
the posterior compartment. The anconeus muscle, at the posterior aspect of the elbow, is
partly blended with – and is essentially a distally placed continuation of – the triceps.
Cubital fossa.
The cubital fossa is the triangular hollow area on the anterior aspect of the elbow.
The boundaries of the cubital fossa are:
- superiorly – an imaginary line connecting the medial and lateral epicondyles;
- medially – the pronator teres;
- laterally – the brachioradialis.
The floor of the cubital fossa is formed by the brachialis and supinator muscles of the arm
and forearm, respectively. The roof of the cubital fossa is formed by deep fascia –
reiforced by the bicipital aponeurosis – subcutanel tissue, and skin.
The muscles of the forearm act on the joints of the elbow, wrist, and digits. In the proximal
part of the forearm, the muscles form fleshy masses extending inferiorly from the medial
and lateral epicondyles of the humerus. The tendons of
5
these muscles pass through the distal part of the forearm and cotinue into the wrist, hand,
and digits.
Flexor-Pronator Muscles of the Forearm are in the anterior compartment of the
forearm and are separated from the extensor muscles of the forearm by the radius and ulna
and the interosseus membrane that connects them.
The flexor muscles are arranged in four layers and are divided into two groups,
superficial and deep.
- a superficial group of five muscles (pronator teres, flexor carpi radialis, palmaris
longus, flexor carpi ulnaris, and flexor digitorum superficialis);
- a deep group of three muscles (flexor digitorum profundus, flexor pollicis longus, and
pronator quadratus).
Extensor Muscles of the Forearm are in the posterior (extensor-supinator) compartment
of the forearm. These muscles can be organized into three functional groups:
- muscles that extend and abduct the hand at the wrist joint (extensor carpi radialis
longus, extensor carpi radialis brevis, and extensor carpi ulnaris);
- muscles that extend and medial four digits (extensor digitorum, extensor indicis, and
extensor digiti minimi);
- muscles that extend or abduct the 1 st digit, or thumb (abductor pollicis longus, extensor
pollicis brevis, and extensor pollicis longus.
Muscles of the Hand
The intrinsic muscles of the hand are in four compartments:
- thenar muscles in the thenar compartment: abductop pollicis brevis, flexor pollicis
brevis, and opponens pollicis;
6
- adductor pollicis in the adductor compartment;
- hypothenar muscles in the hypothenar compartment: abductor digiti minimi, flexor
digiti minimi, and opponens digiti minimi;
- short muscles of the hand: the lumbricals are in the central compartment and
interossei are between the metacarpals.
Lecture №8
Biomechanics of Human Locomotor System
Plan of the Lecture:
1. Organization of Thigh Muscles.
2. Gluteal Region.
1. Popliteal Fossa.
2. Muscles of the Leg and of the Foot.
Organization of Thigh Muscles
The thigh muscles are organized into three compartments by intermuscular septa
that pass between the muscles from the fascia lata to the femur. The compartments are
anterior, medial, and posterior,so named on the basis of their location, and actions.
Anterior Thigh Muscles.
The anterior thigh muscles – the flexors of the hip and extensors of the knee – are
in the anterior compartments of the thigh. For attachments,main actions of these
muscles. The anterior thigh muscles are:
- pectineus;
- iliopsoas;
- tensor of fascia lata;
- sartorius;
2
- quadriceps femoris.
The pectineus is a flat quadrangular muscle located in the anterior part of the
superomedial aspect of the thigh. The pectineus adducts and flexes the thigh and assists in
medial rotation of the thigh.
The iliopsoas is the chief flexor of the thigh. Its board lateral part , the iliacus, and its
long medial part, the psoas major , arise from the iliac fossa and lumbal vertebrae,
respectively.
The tensor of fascia lata is a fusiform muscle approximately 15 cm long that is
enclosed between two layers of fascia lata. The tensor of fascia lata is a flexor of the thigh.
It also tenses the fascia lata and iliotibial tract.
The sartorius is a long muscle that passes obliquely across the superoanterior part of
the thigh. The sartorius, the longest muscle in the body, acts across two joints : it flexes
the hip joint and participates in flexion of the knee.
The quadriceps femoris (L. Four-haeded femoral muscle) forms the main bulk of the
anterior thigh muscles and collectively constitutes the largest and one of the most
powerful muscles in the body. It covers almost all the anterior aspect and sides of the
femur. The quadriceps cosists of four parts:
- rectus femoris;
- vastus lateralis;
- vastus intermedius;
- vastus medialis.
The quadriceps is an important muscle during climbing, running, jamping, rising from the
siting position, and walking up and down stairs.The tendons of the four parts of the
quadriceps unite in the distal portion of the thigh to form a single,
3
strong, broad quadriceps tendon. This tendon is traditionally discribed as attaching to the
base of the patella, a large sesamoid bone in the tendon, which in turn is attached through
the patellar ligament to the tibial tuberosity.
Vastus lateralis lies on the lateral side of the thigh; vastus medialis covers the
medial side of the thigh; vastus intermedius lies deep to the rectus femoris, between the
vastus medialis and vastus lateralis.
Medial Thigh Muscles.
The medial thigh muscles – the adductor group – are in the medial compartment of
the thigh. It consists of:
- adductor longus;
- adductor brevis;
- adductor magnus;
- gracilis;
- obturator externus.
Collectivelly, these muscles are the adductors of the thigh; however, the actions of
some of these muscles are more complex.
Femoral Triangle – a junctional region between the trunk and lower limb is a
triangular fascial space in superoanterior third of the thigh. It appears as a triangular
depression inferior to the inguinal ligament when the thigh is flexed, abducted, and
laterally rotated. The femoral triangle is bounded:
- Superiorly by the inguinal ligament;
- Medially by the adductor longus;
- Laterally by the sartorius.
4
The femoral canal – the smallest of the three femoral sheath compartments – is the
short (1.25 cm), conical medial compartment of the femoral sheath that lies between the
medial edge of the femoral sheath and the femoral sheath and the femoral vein. The base
of the femoral canal ( its abdominal end) is directed superiorly and , although oval shaped,
is called the femoral ring.
The femoral ring – the small proximal opening of the femoral canal ( 1cm wide) – is
closed by extraperitoneal fatty tissue that forms the femoral septum. The abdominal
surface of this septum is covered by parietal peritoneum. The femoral septum is pierced by
lymphatic vessels connecting the inguinal and external iliac lymph nodes. The boundaries
of the femoral ring are:
- Laterally, the partition between the femoral canal and femoral vein;
- Posteriorlly, the superior ramus of the pubis covered by the pectineus and its fascia;
- Medially, the lacunar ligament;
- Anteriorlly, the medial part of the inguinal ligament.
The adductor canal (Hunter,s canal) – 15 cm long, is a the thigh running from the
apex of the femoral triangle to the adductor hiatus in the tendon of the adductor magnus.
The contents of the adductor canal are the:
- femoral artery and vein;
- saphenous nerve;
- nerve to vastus medialis;
The adductor canal is bounded:
- anteriorly and laterally by the vastus medialis;
- posteriorly by the adductors longus and magnus;
5
- medially by the sartorius.
Gluteal Region
The gluteus region lies posterior to the pelvis between the level of the iliac crests
and the inferior borders of the gluteus maximus muscles.
Gluteus Ligaments.
The part of the bony pelvis – hip bones, sacrum, and coccyx – are bound together by
dense ligaments. The sacrotuberous and sacrospinous ligaments convert the sciatic
notches in the hip bones into the greater and lesser sciatic foramina. If is helful to think
of the greater sciatic foramen as the “door” through which all lower limb arteries and
nerves leave the pelvis and enter the gluteal region.
Posterior Thigh Muscles.
The three muscles in the posterior aspect of the thigh are the hamstring:
- semitendinosus;
- semimembranosus;
- biceps femoris.
The hamstrings are extensors of the thigh and flexors of the leg.
Popliteal Fossa
The popliteal fossa is the diamond-shaped depression of the posterior aspect of the
knee. The fossa is bounded superiorly by the hamstring and inferiorly by the two neads of
the gastrocnemius and the plantaris. All important vessels and nerves from the thigh to the
leg pass through this fossa. The popliteal fossa is formed:
6
- superolayerally by the bicips femoris (superolateral border);
- superomedially by the semimembranosus, lateral to which is the semitendinosus
(superomedial border);
- inferolaterally and inferomedially by the lateral and medial heads of the gastrocnemius
(inferolateral and inferomedial borders).
Muscles of the Leg and of the Foot
The leg is divided into three fascial compartmenrs – anterior, lateral, and posterior –
by the anterior and posterior intermuscular septa and the interosseous membrane. The
anterior septum separates the anterior and lateral leg muscles, and the posterior septum
separates the lateral and posterior muscles; thus, each group has its own compartment.
Anterior Compartment of the Leg.
The anterior compartment is bounded anteriorly by crural fascia and skin.
The four muscles in the anterior compartment are the:
- tibialis anterior;
- extensor digitorum longus;
- extensor hallucis longus;
- fibularis tertius.
Lateral Compartment of the Leg.
The lateral compartment is bounded by the lateral surface of the fibula, the anterior
intermuscular septa, and the crural fascia.
The lateral compartment contains the fibularis longus and brevis muscles.
7
Posterior Compartment of the Leg.
The posterior compartment is the largest of the free leg compartments. The calf
muscles in the posterior compartment are divided into superficial and deep groups by the
trasverse intermuscular septum.
The superficial group of muscles – gastrocnemius, soleus, and plantaris – forms a
powerful mass in the calf of the leg that plantar flexes the foot. Together, two-headed
gastocnemius and soleus form the three-headed triceps surae. This large muscle has a
common tendon
- the calcaneal tendon (Achilles tendon) – which attaches to the
calcaneus.
Deep Muscles Group in the Posterior Compartment.
Four muscles comprise the deep group in the posterior compartment of the leg:
- popliteus;
- flexor digitorum longus;
- flexor hallucis longus;
- tibialis posterior.
The popliteus acts on the knee joint, whereas the other muscles act on the ancle and
foot joints.
Muscles of the Foot.
The four layers in the sole of the foot help maintain the arches of the foot and
enable one to stand on uneven ground.
The 1st layer of plantar muscles consists of:
- abductor hallucis;
- flexor digitorum brevis;
- abductor digiti minimi
8
The 2nd layer of plantar muscles consists of:
- quadratus plantae;
- tendons of flexor hallucis longus and flexor digitorum longus;
- lumbricals.
The 3rd layer of plantar muscles consists of:
- flexor hallucis brevis;
- adductor hallucis;
- flexor digiti minimi brevis.
The 4th layer of plantar muscles consists of:
- three plantar interossei;
- four dorsal interossei.
The lateral plantar artery and nerve course laterally between the muscles of the 1 st
and 2nd layers of plantar muscles. Their deep branches course medially between the
muscles of the 3rd and 4th layers.
Lecture № 1
Functional Anatomy of the Skull.
The skull ( or cranium in Latin) is the skeleton of the head.It consists of two parts,
the neurocranium and fasial skeleton. The neurocranium (“brain box” or cranial
vault) provides a case for the brain and cranial meninges. The facial skeleton consists
of the bones surrounding the mouth and nose and contributing to the orbits (eye
sockets, orbital cavites).
The neurocranium in adults is formed by a series of eight bones:
-
a frontal bone;
-
two parietal bones;
-
two temporal bones;
-
an occipital bone;
-
a sphenoid bone;
-
an ethmoid bone.
The facial skeleton consists of 14 bones:
-
lacrimal bones (2);
-
nasal bones (2);
-
maxillae (2);
-
zygomatic bones (2);
-
palatine bones (2);
-
inferior nasal conchae (2);
-
mandible (1);
-
vomer (1).
The cranium has a domelike roof – the calvaria (skullcap) – and a floor or cranial
base (basicranium) consisting of the ethmoid bone and parts of the occipital and
temporal bones.
Development of the Skull
The bones forming the calvaria and some parts of the cranial base develop by
intramembranous ossification. These bones is called primary bones. Whereas most parts
of the cranial base develop by endochondral ossification. Thus bones are called secondary
bones.
The structure of the calvaria bones differs from the other bones of the skull.
Most of these bones are largely flat, curved, and united by fibrous interlocking
sutures. These bones are composed of two layers of compact tissue enclosing between
them a variable quantity of cancellous tissue. In the cranial bones the outer layer is thick
and tough, the inner one thinner, denser and more brittle. The intervening cancellous
tissue is called diploe(layer of spongy bone) Large venous canals are situated in the
diploe.
In the anatomical position, the skull is oriented so that the inferior margin of the
orbit and the superior margin of the external acoustic meatus of bouth sides lie in the same
horizontal plane. This standard craniometric reference is the orbitomeatal plane.
The other important feature of the skull is the presence of pneumetic bones. They
are the bones with air-containing cells or sinuses. They are needed to make the skull bone
lighter and they give timbre to the voice. All sinuses of the pneumatic bone open in the
meatus of nasal cavity. S.sphenoidal and posterior cells of ethmoid open in superior nasal
meatus, frontal, maxillary sinuses and anterior and medial cells of the ethmoid open in the
middle nasal meatus.
Connections of the bones of the skull
The bones of the skull, with the exeption of the Mandible are connected to each
other by means of Sutures. They are closely adapted to each other.
There are four sutures in the skull, they are: sagittal, coronal, lambdoid and sguamous.
1The Sagital Suture is formed by the junction of the two parietal bones.
1. The Coronal Suture extends transversely across the vertex of the skull and
connects the frontal with the parietal bones.
2. The Lambdoid S. is so called from its resemblance to the Greek latter, and it
connects the occipital with the parietal bones
3. The Squmous S is the joints between squamous part of temporal bone and parietal
bone.
There is only one movable articulation in the head. It is Temporomandibular Joint
(TMJ).
The TMJ is a modified hinge type of joint. The articular surface involved are the
condyle of the mandible, the articular tubercle of the temporal bone, and the mandibular
fosse. The articular capsule of the TMJ is loose. The fibrous capsule attaches to the
margins of the articular area on the temporal bone and around the neck of the mandible.
The joint has two synovial membranes:
- the superior synovial membrane lines the fibrous capsule superior to the articular disc;
- the inferior synovial membrane lines the capsule inferior to the disk.
The articular disk divides the joint into two separate compartments. The thick part of the
articular capsule forms the intrinsic lateral ligament (ligamentum temporomandibularis),
which strengthens the TMJ laterally and, with the postglenoid tubercle, acts to prevent
posterior dislocation of the joint.
Two extrinsic ligaments and the lateral ligament connect the mandible to the cranium.
The stylomandibular ligament – runs from the styloid process to the angle of the
mandible. The sphenomandibular ligament runs from the spine of the sphenoid to the
lingula of the mandible.
The movements of the mandible at the TMJ are as follows: Depression (open mouth),
Elevation (closed mouth), Protrusion (protraction of chin).
The next peculiarity of the skull structures is the presence of the strongest zones
(areas) of the skull. These zones counteract the mechanical influence during the process
mastication in normal conditions and in fractures and injuries.
They are called contrforces in the facial part of the skull.
They are called arches in the calvaria.
They are called trabecula in the bases of the skull.
They are all connected with each other.
Dr. Le Fort, a Paris surgeon classified the common variants of fractures of the
maxilla. There are 3 types of fracture, they are:
A Le Fort I is located just superior to the alveolar process, crossing the bony nasal
septum and the pterigoid plates of the sphenoid.
A Le Fort II passes from the maxillary sinuses, through the infraorbital foramina,
lacrimals or ethmoid to the bridge of the nose.
A Le Fort III passes through the superior orbital fissures, the ethmoid and nasal
bones and extends laterally through the greater wings of the sphenoid bone.
Fractures of the mandible
There are 4 types of mandible’s fractures, they are: Fractures of the coronoid process; fr.
of the neck of the mandible; fr.of the angle of the mandible; fr. of the body of the
mandible.
Age features of the Skull
At birth, the bones of the calvaria are smooth and unilaminar; no diploe is present. The
frontal and parietal eminences are especially prominent. The skull of a newborn infant is
disproportionately large compared with other parts of the skeleton; The large size of the
newborn, s calvaria results from precocious growth and development of the brain. The
smallness of the face results from the absence of erupted teeth, and the small size of the
nasal cavities.
A frontal suture separates the halves of the frontal bone, but the greater part of it
usually disappeared about the 15 or 16 year. The maxillae and mandibles are separated by
an intermaxillary suture and mandibular symphysis, respectively.
At an early period of life a thin plate of cartilage exists between the basilar surface
of the body of the occipital bone and the posterior surface of the body of the sphenoid. In
the adult they become fused and the basilar suture is formed.
The bones of the calvaria of a newborn infant are separated by areas of fibrous tissue
membrane – the fontaneless – which represent parts of unossified bones. There are six
fontanelles : two are in the median plane – anterior and posterior – and two pairs are on
each side – the anterolateral or sphenoidal fon. and the posterolateral or mastoid fon.
The anterior fon. is located at the junction of the sagital, coronal, and frontal
sutures, the future site of the bregma. By 18 months of age, the surrounding bones have
fused and the anterior fon. is no longer clinically palpable. The posteror fon. is triangular
and bounded by the parietal bones anteriorly and occipital bone posteriorly. It is located at
the junction of the lambda. The posterior fon. begins to close during the first few months
after birth, and by the end of the 1st year it is small and no longer clinically palpable.
The bones of the fetal skull are very resilient. The increase in the size of the calvaria
is greatest during the first 2 years, the period of most repid brain development. A person , s
calvaria normally increases in capacity until 15 or 16 years of age.
External Aspect of the skull has three thopografic features, three fossae: temporal
fossa, infratemporal fossa and pterygopalatine fossa.
Temporal fossa is a bony fossa located on the lateral aspect of the skull between
the temporal line and the zygomatic arch.
Contains: 1. Temporal muscle
2. Deep temporal nerve and vessels.
Infratemporal fossa – bony space situated below the middle cranial fossa of the
skull, behind body of maxilla and lateral to lateral pterygoid plate. It contains the
pterygoid muscles, the pterygoid plexus and the ramus of the mandibular nerve.
Pterygopalatine fossa – a small bony space situated deep to pterygomaxillary
fissure. This fossa communication with :
1.Orbit through inferior obital fissure
4. Middle cranial fossa – through f. rotundum
5. Oral cavity through canalis palatinus major
6. Nasal cavity through f. sphenopalatinum
7. F.Lacerum through pterygoid canal
Anterior, Lateral, Posterir, Superoir, External and Internal Aspects of the Skull
Anterior Aspect of the skull.
Features of anterior aspect of the skull are the frontal and zygomatic bones, orbits,
nasal region, maxillae, and mandible.
The frontal bone- specifically its squamous part – forms the skeleton of the forehead,
articulating inferiorly with the nasal and zygomatic bones. The supraorbital margin, the
angular boundary between the squamous and orbital parts, has a supraorbital notch or a
foramen in some skulls for passage of the supraorbital nerve and vessels. Just superior to
the supraorbital margin is a ridge – the superciliare arch – that extends laterally on each
side from the glabella. The prominence of this ridge, deep to the eyebrows, is generally
greater in males. Within the orbits are the superoir and inferior orbital fissures and optic
canals.
The maxillae form the upper jaw; their alveolar processes include the sockets
(alveoli) and constitute the supporting bone for the maxillare teeth. The maxillae have a
broad connection with the zygomatic bones laterally and have an infraorbital foramen
inferior to each orbit for the infraorbital nerve and vessels.
The mandible consists of a horizontal part, the body, and a vertical part, the ramus.
The mandible is a U-shaped bone with alveolar processes that hous the mandibular teeth.
Inferior to the second premolar teeth are the mental foramina for the mental nerve and
vessels. The mental protuberanse – forming the prominence of the chin – is a triangular
elevation of bone inferior to the mandibular symphysis, the region there the halves of the
fetal mandible fuse.
Lateral Aspect of the Skull.
Cranial and facial bones form the lateral aspect of the skull. The main features of
the cranial part include the temporal fossa, the opening of the external acoustic meatus,
and the mastoid region of the temporal bone. The main features of
the facial part include the infratemporal fossa, zygomatic arch, and lateral aspects of the
maxilla and mandible. The temporal fossa is bounded superiorly and posteriorly by the
temporal lines, anteriorly by the frontal and zygomatic bones, and inferiorly by the
zygomatic arch.
The external acostic meatus opening is the entrance to the external acoustic meatus,
which leads to the tympanic membrane. The mastoid proces of the temporal bone is
posteroinferior to the opening of the external acoustic meatus. Anteromedial to the
mastoid process is the slender styloid process.
Posterior Aspect of the Skull.
The posterior aspect of the skull, or occiput, is typically ovoid or round in outline. It
is formed by the occipital bone, parts of the parietal bones, and mastoid parts of the
temporal bones. The external occipital protuberance is usually an easily
palpable elevation in the median plane. The external occipital crest descends from the
external occipital protuberance toward the foramen magnum – the large opening
in the basal part of the occipital bone. The superior nuchal line, markes the superior limit
of the neck. In the center of the occiput, the lambda indicates the junction of the sagittal
and lambdoid sutures.
Superior Aspect of the Skull.
The superior aspect of the skull, usually somewhat oval in form, broadens
posterolaterally at the parietal eminences. The coronal suture separates the parietal bones,
and the lambdoid suture separates the parietal and temporal bones from the occipital bone.
The bregma is the landmark formed by the intersection of the sagittal and coronal sutures.
The vertex – the most superoir point of the skull – is near the midpoint of the sagittal
suture.
The inferior region or base of the skull has two surfaces an external or basilar and
internal or cerebra.
External Aspect of the Cranial Base.
The external surface of the cranial base shows the alveolar arch of the maxillae, the
palatine processes of the maxillae, and the palatine, sphenoid, vomer, tenporal, and
occipital bones.
Wedged between the frontal, temporal, and occipital bones is the sphenoid bone,
consists of the body, greater wings, lesser wings, and pterygoid process. Depression in the
temroral bone – the mandibular fossae – accommodate the condyles of the mandible when
the mouth is closed.
The cranial base is formed posteriorly by the occipital bone, which articulates with
the sphenoid bone anteriorly. The large opening between the occipital bone and the
petrous part of the temporal bone is the jugular foramen, from which the internal jugular
vein and several cranial nerves emerge from the skull. Superolateral to the
jugular foramen is the internal acoustic meatus.The entrance to the carotid canal for the
internal carotid artery is just anterior to the jugular foramen. The mastoid process is ridged
because it is designed for muscle attachment. The stylomastoid foramen, transmitting the
facial nerve and stylomastiod artery, lies posterior to the base of the styloid process.
Internal Aspect of the Cranial Base.
The internal surface of the cranial base has three large, depressions that lie at
different levels – the anterior, middle, and posterior cranial fossae – which form the bowlshaped floor of the cranial cavity.
Anterior Cranial Fossa. The inferior and anterior parts of the frontal lobes of the
brain occupy the anterior cranial fossae, the shallowest of the three fossae. The anterior
cranial fossa is formed by the frontal bone anteriorly, the ethmoid bone in the middle, and
the body and lesser wings of the sphenoid posteriorly. The crista galli (cock , s comb) is a
median ridge of ethmoid bone. The foramen caecum is anterially to the cock , s comb.
Middle Cranial Fossa. The middle cranial fossa is butterfly-shaped, composed of
large, deep depressions on each side of the much smaller sella turcica centrally on the
body of the sphenoid bone. The boundary between the middle and
posterior cranial fossae is the petrous crests of the temporal bones laterally and a flat plate
of bone, the dorsum sellae of the sphenoid, medially.
The sella turcica ( Turkish saddle)– is composed of three parts:
tuberculum sellae; hypophyseal fossa; dorsum sellae (“back of the saddle”).
In the middle cranial fossa on each side of the base of the body of the sphenoid bone
is a crescent of four foramina:
-
the superor orbital fissure is between the greater and lesser wings. This
fissure transmits the ophtalmic veins and nerves entering the orbit;
-
the foramen rotundum, it transmits the maxillary nerve;
-
the foramen ovale, it transmits the mandibular nerve;
-
the foramen spinosum, it transmits the middle meningeal vessels and the
meningeal branch of the mandibular nerve.
The foramen lacerum – not part of the crescent of foramina – is a ragged foramen
that lies posterolateral to the hypophysial fossa; it is an atrifact of a dried skull.
Posterior Cranial Fossa.
The posterior cranial fossa lodges the cerebellum, pons, and medulla
oblongata. The posterior cranial fossa is formed largely by the occipital bone, but
the dorsum sellae of the sphenoid marks its anterior boundary centrally and the
petrous and mastoid parts of the temporal bones contribute its anterolateral “walls".
From the dorsum sellae, the clivus is a marked incline in the center of the anterior
part of the posterior cranial fossa leading to the foramen magnum.