* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Nurs 1100 LAB
Survey
Document related concepts
Baker Heart and Diabetes Institute wikipedia , lookup
Heart failure wikipedia , lookup
Saturated fat and cardiovascular disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Electrocardiography wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Cardiac surgery wikipedia , lookup
Jatene procedure wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Coronary artery disease wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
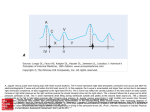
Nurs 1100 LAB Jarvis Unit 7 Pg 488-495 Chapter 19: Heart and Neck Vessels The Neck Vessels - See Fig 19-10 - Carotid artery pulse o Carotid artery located in groove between trachea and sternomastoid muscle, medial to and alongside that muscle o Carotid artery = central artery; close to heart; timing closely coincides with ventricular systole o Characteristic of waveform- smooth rapid upstroke, a summit that is rounded and smooth, and a downstroke that is more gradual and that has a dicrotic notch caused by closure of the aortic valve (marked as D in Fig 19-11 below) o Arterial pulse caused by forward propulsion of blood - Jugular venous pulse and pressure o Jugular veins = empty unoxygenated blood directly into superior vena cava o Jugular vein gives info about activity on the right side of heart o Reflect filling pressure and volume changes o Jugular vein exposes volume and pressure increase when right side of heart fails to pump efficiently o 2 jugular veins present in each side of neck (See Fig 19-10) o Larger internal jugular = deep and medial to the sternomastoid muscle Usually not visible Diffuse pulsations may be seen in sterna notch when person is supine o External jugular = more superficial; lies lateral to sternomastoid muscle, above clavicle o Jugular pulse different from arterial o Jugular pulse results from a backwash, a waveform moving backward caused by events upstream o Jugular pulse has 5 components (Fig 19-12 below) A wave reflects atrial contraction because some blood flows backward to the vena cava during right atrial contraction C wave (or ventricular contraction), is backflow from the bulging upward of the tricuspid valve when it closes at the beginning of the ventricular systole (not from neighbouring carotid artery pulsation) X descent shows atrial relaxation when right ventricle contracts during systole and pulls the bottom of the atria downward V wave occurs with passive atrial filling because of the increasing volume in the right atria and increase pressure Y descent reflects passive ventricular filling when tricuspid valve opens and blood flows from the RA to the RV Developmental Care - Infants and Children o Fetal heart begins to beat at the end of 3 weeks’ gestation o Lungs are nonfunctional, but fetal circulation compensates for this o Oxygenation takes place at placenta o Arterial blood is returned to right side of heart o No point in pumping all freshly oxygenated blood through the lungs, so it is rerouted in 2 ways: First, 2//3 of blood is shunted through an opening in the atrial septum, the foremen ovale, into the left side of the heart, where it is pumped out through the aorta Second, the rest of the oxygenated blood is pumped by the right side of the heart out through the pulmonary artery, but it is detoured through the ductus arteriosus to the aorta Because both are pumping into systemic circulation, the right and left ventricles are equal in weight and muscle wall thickness o Inflation and aeration of lungs at birth produces circulatory changes Blood is oxygenated now through lungs instead of placenta Foremen ovale closes within first hour because of new lower pressure in right side of heart than in left side Ductus arteriosus closes later, within 10-15 hours of birth LV has greater workload of pumping into the systemic circulation When baby has reached 1 year, the LV’s mass increases to reach the adult ratio of 2:1. LV to RV o Heart’s position in chest is more horizontal in infant than adult >> apex is higher, located at fourth left intercostals space; reaches adult position when 7 years old - The Pregnant Female o Blood volume increases by 30-40% o Most rapid change during second trimester o Creates an increase in stroke volume and cardiac output and increase pulse rate of 10-15 beats/minute o Arterial blood pressure decreases as a result of peripheral vasodilation o Blood pressure drops most during second trimester and then rises after that - The Aging Adult o Aging process of cardiovascular system depends on lifestyle, habits, and diseases o Lifestyle- smoking, diet, alcohol use, exercise patterns, and stress >> influence on coronary artery disease o Cardiac changes partially due to sedentary lifestyle accompanying aging o Hemodynamic Changes with Aging From 20-60, systolic blood pressure increases about 20 mm Hg From 60-80, systolic blood pressure increases another 20 mm Hg because of stiffening of large arteries which is due to calcification of vessel walls (arteriosclerosis) Stiffening creates increase in pulse wave velocity because less compliant arteries cannot store the volume ejected Overall size of heart doesn’t change with age But left ventricular wall thickness increases o Adaptive mechanism to accommodate for vascular stiffening (that creates an increased workload on heart) No significant change in diastolic pressure with aging No change in resting heart rate with aging Cardiac output at rest if not changed with aging Decreased ability of heart to augment cardiac output with exercise Shown by decreased maximum heart rate with exercise and diminished sympathetic response Non-cardiac factors also cause decrease in max work performance with aging- decrease in skeletal muscle performance, increase in muscle fatigue, increased sense of dyspnea Exercising can help modify aging changes in cardiovascular function Arrhythmias Presence of supraventricular and ventricular arrhythmias increases with age Ectopic beats common in aging population Tachyarrhythmias not tolerated well by older adults o Myocardium is thicker and less compliant and early diastolic filling is impaired at rest o Can’t tolerate tachycardia because of shortened diastole o Can further compromise vital organs whose function has already been affected by aging/disease o i.e. ventricular tachycardia produces a 40-70% decrease in cerebral blood flow older person can experience syncope because of this ECG Change in conduction system: o Prolonged P-R interval (first degree AV block) and prolonged Q-T interval, but QRS interval is unchanged o Left axis deviation from age related mild LV hypertrophy and fibrosis in left bundle branch o Increased incidence of bundle branch block Cardiovascular disease increases with age Coronary artery disease increases siginificantly Account for about half of deaths in older adults Hypertension and heart failure increases Lifestyle habits play huge role Increased physical activity associated with reducing risk of death from cardiovascular diseases and respiratory illnesses Cultural and Social Considerations - In Canada, death by cardiovascular disease is decreasing - - - - - - - Reasons for decrease: early intervention, public health awareness, better medications, etc Canada, men and women have almost equal death rates from CVD (cardiovascular disease) Cancer rates have increase (29.5%) Prevalence of heart disease and stoke higher in adults of African descent o 44.6% for men and 40% for women o (37.2% for men and 35% for women of European desecent) o Need to improve early detection and screening and treatment for people of African descent Socioeconomic factors influence CVD in Canadians Factors that influence people with CVD to complement comprehensive treatment plan: income, employment, ability to afford nutritious diet, access to resources, extended healthcare plans 2004, income differences accounted for 6400 premature deaths from CVD Major risk factors for heart disease and stroke- high blood pressure, smoking, high cholesterol, obesity, physical inactivity, and diabetes For women, risk factors include use of oral contraceptives and presence of post menopausal hormones High Blood Pressure (HBP) o Over 1/5 of Canadians have HBD/hypertension o Increase in past 10 years Smoking o Estimated 5.1 million Canadians or 20% of population aged 15 and older reported smoking daily or occasionally in 2004 o More men than women smoke (22% vs. 17%) Serum Cholesterol o Children (4-19) and adolescents of African descent have higher total cholesterol, high low-density lipoprotein (LDL) cholesterol, and higher high-density lipoprotein (HDL) cholesterol (the “good” cholesterol) than children/adolescents of European descent o Differences reverse during adulthood (ppl of African descent have lower serum cholesterol levels than do Euro-Canadians) Obesity o Overweight = BMI of 25 kg/m(squared) or higher o Obesity = BMI of 30 kg/m(squared) or higher o Canadian women are more overweight than men, 64% vs. 53% o Children ages 2-17 are overweight and obsess- 25% of females and 29% of males Diabetes o Over 2 million Canadians have diabetes o 77% of new Canadians, including Hispanics, Asians, South Asians, and those of African descent, come from populations that are at higher risk for type 2 diabetes o In Canada, diabetes is more common in men than women o 80% of people with diabetes die of heart disease or stroke Subjective Data Chest Pain - Any chest pain or tightness? o When did it start? How long have you had it this time for? Had this type of pain before? How often? o Where did it start? Does it pain to any other spot? o How would you describe it? Crushing, stabbing, burning, viselike, etc? o What is pain brought on by? Activity, emotional upset, after eating… o Associated symptoms? Sweating, ashen grey/pale skin, heart skips… o Pain made worse by moving the arms/neck, breathing, lying flat? o Pain relieved by rest or nitroglycerine? How many? Dyspnea - Any shortness of breath? o What type of activity brings it on and how much bring on shortness of breath? o Does shortness come unexpectedly? o Is it constant or does it come and go? o Does it seem to be affected by position? Lying down… o Does it awaken you from sleep? o Does SOB interfere with ADL? Orthopnea - How many pillows do you use when sleeping/lying down? Cough - Do you have a cough? o How long have you had it? o Is it related to time of day? o Describe it- hacking, barky, hoarse, congested… o Do you cough up mucus? Color, odour, blood? o Is it associated with activity, position (lying down), anxiety, talking, etc? o Does activity make it better/worse? o Relieved by rest of medication? Fatigue - Do you seem to get tired easily? Are you able to keep up with your family and coworkers? o When did fatigue start? Sudden or gradual? Has any recent change occurred in energy level? o Is fatigue related to time of day? All morning, evening, afternoon? Cyanosis or Pallor - Have you ever noted your facial skin turn blue or ashen? Edema - Any swelling of your feet and legs? o What did you first notice this? o Any recent change? o What time of day does the swelling occur? Do your shoes feel right at the end of the day? o How much swelling would you say there is? Are both legs equally swollen? o Does the swelling go away with rest, elevation, after rest? o Are there any associated symptoms (i.e. SOB). If so, does this occur before or after the leg swelling? Nocturia - Do you awaken at night with an urgent need to urinate? o How long has this been occurring? Any recent change? Cardiac History - Any past history of hypertension, elevated cholesterol or triglycerides, heart murmur, congenital heart disease, rheumatic fever or unexplained joint pains as child or youth, recurrent tonsillitis, anemia? - Ever had heart disease? o When? o Treated by medication or surgery? - Last ECG, stress ECG, serum cholesterol measurement, other heart tests? Family Cardiac History - Any family history of hypertension, obesity, diabetes, coronary artery disease (CAD), sudden death at younger age? Personal Habits (cardiac risk factors) - Nutrition o Describe your usual daily diet o What is your usual weight Any recent change? - Smoking o Do you smoke cigarettes or other tobacco? What age did you start? How much per day? For how many years have you smoked this amount? Have you ever tried to quit? If so, how did this go? - Alcohol o How much do you usually drink each week/day? o When was your last drink? How many that time? o Have you ever been told you have a drinking problem? - Exercise o What is your usual amount of exercise each day/week? o What type of exercise and usual amount (light, moderate, heavy)? - Drugs o Do you take any antihypertensives, beta-blockers, calcium channel blockers, digoxin, diuretics, aspirin, and anticoagulants, over the counter drugs or street drugs? Additional History for Infants (for subjective data) - How was the mother’s health during pregnancy? o Any unexpected fever, rubella first trimester, other infection, hypertension, drugs taken? - Have you ever noted any cyanosis while nursing, crying? o Is baby able to eat, nurse, finish bottle without tiring? - Growth o Has the baby grown as expected by growth charts and about the same as siblings/peers? - Activity o Were baby’s motor milestones achieved as expected? Is the baby able to play without tiring? How many naps does the baby take each day and how long does each last? Additional History for Children (for subjective data) - Growth o Has child grown as expected by growth charts? - Activity o Is child able to keep with siblings or age mates? Is child willing or reluctant to go out to play? Is child able to climb stairs, ride a bike, walk a few blocks? Does child squat to rest during play or to watch TV, or assume a knee-chest position while sleeping? Have you noted “blue spells” during exercise? - Has child had any unexplained joint pains/unexplained fever? - Does child have frequent headaches, nosebleeds? - Does child have frequent respiratory infections? How many per year? How are they treated? Have any of these proved to be streptococcal infections? - Family History o Does child have a sibling with heart defect? o Is anyone in the child’s family known to have chromosomal abnormalities, such as Down syndrome? Additional History for the Pregnant Female (for subjective data) - Have you had any HBP during this or earlier pregnancies? - What was your usual blood pressure before pregnancy? - How has your BP been monitored during pregnancy? - If HBP, what treatment has been started? - Any associated symptoms: weight gain, protein in urine, swelling in feet/legs/face? - Have you had any faintness or dizziness with this pregnancy? Additional History for the Aging Adult (for subjective data) - Do you have any known heart or lung disease? (hypertension, CAD, chronic emphysema or bronchitis) o What efforts to treat this have been started? o Usual symptoms changed recently? Does illness interfere with ADL’s? - - Do you take any medications for your heart, such as water, blood pressure, or heart pills? Are you aware of the side effects? Have you recently stopped taking your med’s? why? Environment o Does your home have any stairs? o How often do you need to climb them? o Does this have any effect on ADL’s?