* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download OUTLINE
Polycystic ovary syndrome wikipedia , lookup
Menstrual cycle wikipedia , lookup
Mammary gland wikipedia , lookup
Xenoestrogen wikipedia , lookup
History of catecholamine research wikipedia , lookup
Triclocarban wikipedia , lookup
Congenital adrenal hyperplasia due to 21-hydroxylase deficiency wikipedia , lookup
Breast development wikipedia , lookup
Bioidentical hormone replacement therapy wikipedia , lookup
Hormone replacement therapy (male-to-female) wikipedia , lookup
Neuroendocrine tumor wikipedia , lookup
Hyperandrogenism wikipedia , lookup
Endocrine disruptor wikipedia , lookup
Hyperthyroidism wikipedia , lookup
Graves' disease wikipedia , lookup
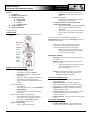
Endocrine Module Overview of the Endocrine System 29 January 2010 Dr. Ruben G. Kasala o OUTLINE I. Introduction II. Five Major Hormone Classes III. Functions of Hormones A. Pituitary Gland B. Adrenal Gland C. Pancreas D. Parathyroid Gland IV. Hormone Receptors V. Endocrine dysfunction **audio = italicized I. INTRODUCTION ENDOCRINOLOGY – study of glands and the hormones they produce Started endocrinology by coining the term: HORMONE - internal secretion of endocrine glands MacCallum and Voetlin o discovered the link between the parathyroid glands and calcium metabolism The impart of advances in organic chemistry and radioisotopes in endocrinology o 1904: Stolz was able to synthesize EPINEPHRINE o 1927: Harrington and Barger synthesized THYROXINE o 1930s: Joliot-Curies – discovered isotopes that can be used for the evaluation of the thyroid gland ** In the evolution of endocrinology, the introduction of radioimmunoassay help pave the way in measuring the hormones secreted by endocrine gland Highlights of History of Endocrinology 1889 – Charles Edouard Brown-Sequard o professor of College de France o introduced the concept of chemical messengers - secreted into the blood exert systemic effects o Experiment: Self-administration of extracts of animal testes, he discovered that he got stronger and improved intellectual and sexual potency 1891 –George Murray o English Physician o achieved the first success in treating myxedema (hypothyroidism) o Experiment: gave the patient an extract of the thyroid gland 1894 – Sharpey-Schafer and George Oliver o demonstrated that in the extracts of adrenal glands, there is a substance that raises the blood pressure: EPINEPHRINE and NOREPINEPHRINE (catecholamines) 1905 – Ernest H. Sterling o brilliant pupil of Sharper-Schafer Group 6 1956 – Rosalyn Yalow, Solomon Berson observed antibodies to insulin that led to development of radioimmunoassay for measuring insulin level o Within a short period, sensitive RIA of high specificity were developed for many peptide, thyroid, and steroid hormones ENDOCRINE vs. EXOCRINE Endocrine: hormones secreted internally then goes into the circulation Exocrine: hormones secreted externally into a lumen such as in the GIT o that’s why hormones secreted by the pancreas goes into the GIT for absorption or for processing food taken Hormone – Greek phrase meaning “to set in motion”, when it is secreted, it sets into motion a lot of physiological activities in the body II. FIVE MAJOR HORMONE CLASSES 1. Amino Acid derivatives – dopamine, catecholamine, thyroid hormone (TH) 2. Small neuropeptides – secreted by the pituitary Gonadotropin Releasing Hormone (GnRH) , Thyroid Releasing Hormone (TRH), somatostatin, vasopressin 3. Large proteins – insulin, Leuteinizing Hormone (LH), Parathyroid Hormone (PTH) 4. Steroid hormones – from the adrenal glands and gonads cortisol and estrogen that are synthesized form cholesterol precursors 5. Vitamin derivatives - retinoids, Vitamin D, protein growth factors III. FUNCTIONS OF HORMONES Three general areas: 1. Growth and differentiation – Insulin Growth Factor 1 (IGF-I), TH, sex hormones: testosterone and estrogen CALUAG, CARAMAT, CASTRO, CREENCIA, DELA CRUZ, DY, GRUTAS, LIM UY, SEE, UY, Page 1 of 5 BATCH 2014 Overview of the The Endocrine System 2. 3. Maintenance of homeostasis – TH: controls 85% of the basal metabolism in most tissues - Cortisol: exerts a permissive action for many hormones in addition to its direct effects - PTH: important for homeostasis of Calcium and phosphorus - Vasopressin (Antidiuretic hormone): secreted by the posterior pituitary, regulates the osmolality and water balance - Mineralocorticoids: regulates vascular volume and electrolytes - Insulin: regulates blood sugar Reproduction – LH, GnRH, inhibin, Epidermal Growth Factor and vascular epithelial growth factor, prolactin, oxytocin 2. Oxytocin – important for stimulation of smooth muscles of the uterus and milk ejection/let-down *interrelationship that interconnects the master endocrine organ: pituitary and other endocrine organs 1909 Tandler and Grosz described pituitary enlargement after castration of men Carl R. Moore and Dorothy Price: o First experimental evidence for feedback control of gonadotrophins - showing a reciprocal relationship between the testes and the anterior pituitary o Subsequently, similar reciprocal relationship between ovaries and pituitary gland A.PITUITARY GLAND 1. Anterior Pituitary – secretes most of the hormones which stimulate the adrenal gland. (TSH, ACTH, FSH, GH, PRL, Endorphins) 1. thyrothropin-releasing hormone stimulates the thyroid gland to produce TH 2. prolactin is under the control of dopamine of the ant. pituitary; for the mammary gland 3. adrenocorticotropin hormone stimulates adrenal gland 4. growth hormone – for the adipose tissue, bone and muscles 5. follicle stimulating hormone and leutenizing hormone – for the testes and ovaries 6. melanocyte stimulating hormone “corticotrophic” – coming from pituitary gland “trophic” – stimulates Adrenocorticotrophic = coming from the pituitary to simulate the adrenal gland Gonadotrophic (FSH and LSH) – from the pituitary to stimulate the gonads 2. Posterior Pituitary 1. Antidiuretic hormone (ADH) – protects the kidney and maintains water balance and volume Group 6 ** negative feedback - important in the evaluation of the hyper/ hypofunction of endocrine glands - releasing hormones from the hypothalamus which stimulate the pituitary gland to release trophic hormones which then stimulate endocrine organs to produce the endocrine hormones -endocrine hormones send a negative signal to the pituitary and hypothalamic area to maintain normal levels of hormones if there is no negative feedback, continuous stimulation of endocrine organs will lead to hypersecretion of endocrine hormones that will have adverse effects ** Dopamine is a derivative of the amino acid tyrosine. Its principal function in the hypothalamus is to inhibit the release of prolactin (PRL) from the anterior lobe of the pituitary. Clinical Application: If a tumor blocks the pituitary stalk, adrenal hormones (cortisol) will be low, thyroid hormones will be low BUT prolactin will have high levels because there will be no inhibitory effect. Why do you think the blood sugar of a patient is elevated when given steroids? -due to stimulation of gluconeogenesis, protein metabolim and glycolysis (in the adipose tissue) ________________________________________________ CALUAG, CARAMAT, CASTRO, CREENCIA, DELA CRUZ, DY, GRUTAS, LIM UY, SEE, UY, Page 2 of 5 BATCH 2014 Overview of the The Endocrine System B. ADRENAL GLAND Adrenal Cortex Zona Glomerulosa – aldosterone Zona Fasciculata – cortisol Zona Reticularis – androgens **GFR is ACA or ACT(testosterone, an androgen) Adrenal Medulla – Epinephrine and Nor-epinephrine **glucose is transported by GLUT2 Glycolyisis produces ATP (36), ATP stimulates potassium sensitive channels, where diabetes medication attaches OBESITY Too much adipose tissue secretes leptin. RENIN – ANGIOTENSIN ALDOSTERONE SYSTEM ** Aldosterone - helps in the maintenance of volume and electrolyte levels. 1. When volume is low, it stimulates the juxta-glomerular apparatus (JGA) to release renin. 2. Renin then converts angiotensin I from angiotensinogen 3. Angiotensin I is then converted to angiotensin II 4. Angiotensin II stimulates aldosterone. ** Aldosterone stimulates potassium, renal excretion, and renal sodium retention which maintain the volume. ** when you are dehydrated you stimulate RAA system and ADH release = water retention C. Pancreas **In obesity, there is leptin resistance. **Adipose tissue leptin neg feedback hypothalamus decreased Neuropeptide Y decreased hunger, increased activity, increased thermogenesis, increased sympathetic activity Central Effect of Leptin ** Diabetes and abnormalities in glucose-simulated insulin secretion. (Glucose and other nutrients regulate insulin secretion by pancreatic beta cell. Glucose is transported by GLUT2 glucose transporter; subsequent glucose metabolism by the beta cell alters ion channel activity leading to insulin secretion.) Group 6 CALUAG, CARAMAT, CASTRO, CREENCIA, DELA CRUZ, DY, GRUTAS, LIM UY, SEE, UY, Page 3 of 5 BATCH 2014 Overview of the The Endocrine System D. PARATHYROID GLAND Found in the posterior aspect of the thyroid gland (usually 4) Secretes PARATHYROID HORMONE o maintains calcium metabolism by calcium resorption from the bone or stimulating the kidney 1,25-Dihydroxyvitamin D _____________________________________________________ 2. Intracellular nuclear receptors – lipid soluble steroids, TH, vit D and retinoids Example: Thyroid Hormone receptors Hormone receptors CROSS-TALK (cross reactions) **Hormone A specifically attaches to Hormone A receptor and produces a specific signal, but sometimes Hormone B attaches to Hormone A receptor and produces the same effect as Hormone A. 1. IV. HORMONE RECEPTORS ** Endocrine hormones exert their effects on hormone receptors **endocrine hormones always attach to SPECIFIC receptors 2. 1. Cell-surface membrane receptors – amino acid derivatives and peptide hormones Example: INSULIN SIGNAL TRANSDUCTION in SKELETAL MUSCLE 3. 4. ** The insulin receptor has intrinsic tyrosine kinase activity and interacts with insulin receptor substrates ** insulin exerts its effect through the membrane receptor, Eventual outcome = stimulation of GLUT 4, transporter of glucose. This opens up the plasma membrane for absorption of glucose for glycolysis and ATP production. Human Chorionic Gonadotropin(HCG) and Thyroid Stimulating Hormone(TSH) - when there is a lot of HCG, it can stimulate TSH receptors and cause hyperthyroidism Parathyroid Hormone related peptide (PTHrp) and PTH – as in certain tumors, they produce PTHrp, which can stimulate PTH receptors = patient develops hypercalcemia Insulin Growth Factor II (IGF-II) precursor and insulin and IGF 1 receptor ACTH and MSH ** NELSON SYNDROME If you remove both adrenal glands, ACTH levels would rapidly increase, ACTH stimulates melanocyte stimulating hormone = patient gets darker Hormones are also bound to Serum-binding proteins in the circulation 1. Thyroxine (T4) and triiodothyronine (T3): Thyroxine Binding Globulin and Albumin and Thyroxine Binding PreAlbumin (TBPA) 2. Cortisol: Cortisol Binding Globulin (CBG) 3. Androgen and estrogen: Sex Hormone Binding Globulin(SHBG) or Testosterone binding globulin (TeBG) 4. IGF-I and II : IGF-binding proteins (IGFBPs) 5. GH : GH-binding protein (GHBP) V. ENDOCRINE DYSFUNCTION Causes of endocrine dysfunction Type of Endocrine Disorder HYPERFUNCTION Neoplastic Benign Malignant Ectopic Autoimmune Group 6 CALUAG, CARAMAT, CASTRO, CREENCIA, DELA CRUZ, DY, GRUTAS, LIM UY, SEE, UY, Examples Can be iatrogenic (cushing’s syndrome), thyrotoxicosis Tumor in the pituitary gland *Pituitary adenomas, *hyperparathyroidism, *autonomoius thyroid or adrenal nodules – nodule will secrete excess thyroid hormone = hyperthyroidism, *pheochromocytoma – tumor in the adrenal gland = excessive secretion of epinephrine = patient is hypertensive (tumors that secrete specific endocrine hormones) *Adrenal cancer, *medullary thyroid cancer, *carcinoid *Ectopic ACTH (lung carcinoma) = increased ACTH = Cushing’s syndrome, *SIADH Secretion *Antibody cross talks with the endocrine hormone receptor: Grave’s disease – secretes a TSH receptor antibody = stimulates excess TH = Hyperthyroidism Page 4 of 5 BATCH 2014 Overview of the The Endocrine System HYPOFUNCTION Autoimmune Iatrogenic Infectious/inflammatory Hormone mutations Enzyme defects Developmental defects Nutritional/vitamin deficiency Hemorrhage/infarction Hormone Resistance Receptor Mutations Membrane Nuclear Signalling pathway mutations Postreceptor Hashimoto’s thyroiditis, type I diabetes mellitus, Addison’s disease, polyglandular tissue Radiation-induced hypopituitarism, hypothyroidism, surgical, radioactive iodine Adrenal insufficiency, hypothalamic sarcoidosis GH Iodine deficiency = hypothyroidism Hemorrhage in the pituitary = shehan’s syndrome GH, vasopressin, LH, FSH, ACTH, ENDOCRINE DISEASES 1. Hyperthyroidism o Gigantism o Acromegaly o Exopthalmos in Graves’ disease – TSH receptor antibodies exert its effect = excess TH production = negative feedback on pituitary = increase ACTH o Subacute Thyroiditis o Toxic Adenoma 2. Hypothyroidism o Cretinism – from infancy o Multinodular Goiter – thyroid is normal but abnormality in the anatomy (can also be autonomous and cause hyperthyroidism) o Thyroid Cold Nodule – nodule that is not functioning o Hypervascular Thyroid Nodule – detected through ultrasound o Metastatic thyroid carcinoma 3. CUSHING’S SYNDROME – tumor in adrenal gland o Hypersecretion of ACTH by the pituitary gland o Protein depletion o Thin skin with abnormal reddish striae o Weak muscles o Poor wound healing o osteoporosis o Hyperglycemia o Body fat redistribution (not symmetrical) o Moon facies o Hirsutism o CNS, symptoms o Water retention increased BP 4. ADDISON’S DISEASE – opposite of Cushing’s 5. ANDROGENITAL SYNDROME 6. SECONDARY HYPERTENSION due to endocrine problem o Pheochromocytoma o Primary hyperaldosteronism – tumor of the adrenal cortex o Congenital adrenal hyperplasia 7. Chromosomal abnormalities o Klinefelter’s syndrome o Turner’s Syndrome Group 6 Common Endorcine disorders and screening tests Disorder Approximate Screening/testing prevalence in recommendations adults Hyperlipidemia 20-25% Cholesterol screening at least every 5 years More forten in highrisk groups Hypothyroidism TSH screening test *when hypothyroidism is not severe(subclinical hypothyroidism) T3 and T4 can be normal Graves’ disease Thyroid nodules and neoplasia Osteoporosis Hyperparathyroidism TSH and T3 and T4 Ultrasound, physical examination, Fine needle aspiration Bone mineral density screen with TSH, Serum Calcium, and random Cortisol Infertility Polycystic ovarian syndrome Hirsutism Menopause Klinefelter syndrome Turner syndrome CALUAG, CARAMAT, CASTRO, CREENCIA, DELA CRUZ, DY, GRUTAS, LIM UY, SEE, UY, RESEARCH: (this was discussed in class in passing) MEN stands for "Multiple Endocrine Neoplasia". The MEN syndromes are conditions which cause overactivity and enlargement in certain endocrine glands. MEN syndromes are usually (but not always) inherited conditions and therefore they run in families. When they are inherited, they are passed from one generation to the next. THREE MAIN TYPES OF MEN Each type of MEN is associated with a specific cluster of illnesses. The main health problems in each of the MEN syndromes are: MEN 1 = Parathyroid tumors, pancreatic tumors, and pituitary tumors. MEN 2a = Medullary thyroid cancers (MTC), pheochromocytoma, and parathyroid tumors. MEN 2b = Medullary thyroid cancers, pheochromocytoma and neuromas. There are specific genetic causes for each of the three types of MEN. Any particular MEN family will have only one type of MEN, either MEN 1, MEN 2a or MEN 2b. Therefore, families with one type of MEN do not have an increased risk of developing an other type of MEN. Page 5 of 5