* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Abstract: Eperythrozoonosis is a zoonosis transmitted from animals
Creutzfeldt–Jakob disease wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Yellow fever wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Chagas disease wikipedia , lookup
West Nile fever wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Typhoid fever wikipedia , lookup
Sarcocystis wikipedia , lookup
Neonatal infection wikipedia , lookup
Hepatitis B wikipedia , lookup
Brucellosis wikipedia , lookup
Hepatitis C wikipedia , lookup
Marburg virus disease wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Rocky Mountain spotted fever wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Trichinosis wikipedia , lookup
Plasmodium falciparum wikipedia , lookup
Schistosomiasis wikipedia , lookup
Oesophagostomum wikipedia , lookup
Fasciolosis wikipedia , lookup
Lymphocytic choriomeningitis wikipedia , lookup
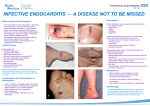
Abstract: Eperythrozoonosis is a zoonosis transmitted from animals to humans. It is caused by Eperythrozoon, Which was divided into Rickettsia In Bergey's Manual, but it’s generally considered to be part of mycoplasma according to 16sRNA sequence. Eperythrozoon is a parasitic bacteria that invades erythrocytes, plasma, and bone marrow. It has high infection rate and can cause varying degrees of damage. The more serious symptoms appear when more than 60% of total erythrocytes are infected. It’s the first case report of infective endocarditis caused by Eperythrozoon. The gold standard for diagnosis is the blood smear, It should be considered in the cases of a fever of unknown origin that does not improve with empiric antibiotic therapy as well as endocarditis with negative blood cultures. Key words: Eperythrozoonosis, Eperythrozoon, Infective Endocarditis, Blood smear Introduction Infective endocarditis (IE) is the disease which has long term therapy and high cost, and its’clinical diagnosis is relatively difficult. Cases of IE associated with negative blood culture up to 31% of all endocarditis cases(1), and there is not yet report of Eperythrozoon in the present pathogens related to endocarditis in China, not only is it largely because the deficiency of the current detection methods, but it's also because of our insufficient clinical cognition. Eperythrozoonosis was a zoonosis in many kind of animals, which parasite on erythrocytes, plasma and marrow. Formerly, Eperythrozoon was classified as the rickettsial agent, recently phylogenetic analysis of 16S rRNA gene showed that Eperythrozoon was closely related to mycoplasma (Haemotrophic Mycoplasma)(2, 3). Blood smear examination was the mainly method of diagnosis. It confirmed hemoplasma infection in humans showing fever, malaise, drowsiness, splenohepatomegalia, decrease of red cell, hemoglobin and platelet, increasing of bilirubin. 1. Case Report: A 37-year-old woman with no significant past medical history presented to an outside hospital with a 30 day history of remittent fever that gradually worsened during the first week. The fever would fluctuate daily, rising as high as 41 degrees Celsius and decreasing to afebrile levels without any medical intervention. She also reported chills and progressive weakness. She has no previous history of heart disease. Six months earlier, she had eaten roasted lamb. Thirty days ago, she spent one week in Hainan, China’s only tropical province, where she ate raw seafood. Laboratory investigations revealed an initial hemoglobin of 14 g/dL that decreased to 10.7 g/dL(normal: 11-15g/dL) after one month, WBC ranged from 3.3-4.9 x109/L(normal: 3.5-10 x109/L) with normal neutrophil and lymphocyte counts. ESR and CRP were mildly elevated at 46-51mm/hr (normal: 1-15 mm/hr) and 8.7-18.4mg/L(normal: 0-5 mg/L) respectively. T-Spot test, antinuclear antibodies, viral antibody panel (Coxsackie, Epstein-Barr, Cytomegalovirus, Herpes), Widal’s reaction, blood smear for malarial parasites, agglutination test for brucellosis were all negative. Thyroid function tests, urine dipstick, ECG, and chest x-ray were unremarkable. At the outside hospital, the patient completed a four day course of amoxicillin/clavulanic acid, five days of levofloxacin, three days of ceftriaxone and three days of artemisinin. Despite this wide variety of antibiotics, the patient’s symptoms did not improve and was then transferred to our hospital. All antibiotic treatment was then discontinued for seven days to rule out druginduced fever. Three sets of blood cultures post-antibiotic therapy showed no growth(4), yet the patient continued to have a fever. A transthoracic echocardiogram performed about 20 days after onset of symptoms revealed a 0.97 x 0.65 cm vegetation on the non-coronary aortic cusp (Figure 1). The patient then completed a six day course of amoxicillin/clavulanic acid with no improvement of her fever(5). The final results from two separate blood smears sent to the CDC of Hangzhou were then obtained and were positive for Eperythrozoon (Figure 2). The patient was diagnosed with Eperythrozoon endocarditis according to the Modified Duke criteria(5). Combined with the treatment of endocarditis and Eperythrozoonosis respective, She was started on oral minocycline 200mg daily for six weeks(5, 6). Her fever and weakness rapidly resolved within the first 3 days of treatment and blood smears were negative for Eperythrozoon after antibiotic therapy. A follow up transthoracic echocardiogram at six months revealed that the vegetation became smaller in size and more stable. The patient remained afebrile and her hemoglobin normalized. 2. Discussion: Eperythrozoonosis is a zoonosis transmitted from animals to humans. More than 30 countries worldwide, mainly China, have reported the disease in sheep, cattle, pigs, humans, etc. Patients with Eperythrozoonosis and animals carriers of Eperythrozoon are the sources of this infectious disease. The infection rates vary from 0 to 97% in China, and the incidence rate is significantly higher in the summer and autumn compared to winter and spring(7). Survey data from the Hangzhou CDC showed that the average infection rate of Hangzhou was 9.31%, of 580 people including controls, meat processing workers, slaughter operators, veterinarians, farm workers. And further found that it has significant difference in the infection rates of those wash their hands or not after contact with animal fur, feces, raw meat, etc. And it also has significant difference in the infection rates of using antibacterial soap to wash hands or not. Eperythrozoon is a parasitic bacteria that invades erythrocytes, plasma, and bone marrow. They are diversiform and mostly spherical, fusiform and short rod. The clinical manifestations of eperythrozoonosis vary from asymptomatic subclinical infection to fever, weakness, scleral icterus, and anemia depending on the ratio of infected erythrocytes. The more serious symptoms appear when more than 60% of total erythrocytes are infected(8). Similar to malaria, Eperythrozoonosis typically manifests as a remittent fever. It can be difficult to identify since its nonspecific clinical signs belong in a wide differential diagnosis that includes influenza, malaria, and anemia. The gold standard for diagnosis is the blood smear; DNA testing continues to be imprecise due to incomplete knowledge of the gene sequence for Eperythrozoon(9), and the hemoplasmas have highly dynamic genomes, and the lack of standards regarding genus circumscription, etc. There is still no correct classification of these organisms. Therefore, a blood smear should be considered in the cases of a fever of unknown origin that does not improve with empiric antibiotic therapy as well as endocarditis with negative blood cultures(1). It has high infection rate and can cause varying degrees of damage. And no one had reported Eperythrozoonosis case involving the endocardium before this in China. References 1.Houpikian P, Raoult D. Blood Culture-Negative Endocarditis in a Reference Center. Medicine (Baltimore). 2005 May;84(3):162-73. 2.Guimaraes AM, Santos AP, do Nascimento NC, Timenetsky J, Messick JB. Comparative genomics and phylogenomics of hemotrophic mycoplasmas. PloS one. 2014;9(3):e91445. 3.Neimark H, Johansson KE, Rikihisa Y, Tully JG. Proposal to transfer some members of the genera Haemobartonella and Eperythrozoon to the genus Mycoplasma with descriptions of 'Candidatus Mycoplasma haemofelis', 'Candidatus Mycoplasma haemomuris', 'Candidatus Mycoplasma haemosuis' and 'Candidatus Mycoplasma wenyonii'. Int J Syst Evol Microbiol. 2001 May;51(Pt 3):891-9. 4.Gould FK, Denning DW, Elliott TS, Foweraker J, Perry JD, Prendergast BD, et al. Guidelines for the diagnosis and antibiotic treatment of endocarditis in adults: a report of the Working Party of the British Society for Antimicrobial Chemotherapy. J Antimicrob Chemother. 2012 Feb;67(2):269-89. 5.Habib G, Hoen B, Tornos P, Thuny F, Prendergast B, Vilacosta I, et al. Guidelines on the prevention, diagnosis, and treatment of infective endocarditis (new version 2009): the Task Force on the Prevention, Diagnosis, and Treatment of Infective Endocarditis of the European Society of Cardiology (ESC). Endorsed by the European Society of Clinical Microbiology and Infectious Diseases (ESCMID) and the International Society of Chemotherapy (ISC) for Infection and Cancer. Eur Heart J. 2009 Oct;30(19):2369-413. 6.Messick JB. Hemotrophic mycoplasmas (hemoplasmas): a review and new insights into pathogenic potential. Vet Clin Pathol. 2004;33(1):2-13. 7.Huang DS, Guan P, Wu W, Shen TF, Liu HL, Cao S, et al. Infection rate of Eperythrozoon spp. in Chinese population: a systematic review and meta-analysis since the first Chinese case reported in 1991. BMC Infect Dis. 2012 Jul 31;12:171. 8.Zhao M, Wang C. One case report of eperythrozoonosis and literature review. Chin J Infect Chemother. 2009;Mar. Vol.9, No.2:3. 9.Jianbiao W, Qishi F, Lin N, Peihua N, Yufeng Y. Establishment of diagnostic methods to detect eperythrozoon in human. Laboratory Medicine. 2011;Vol 26,No 11.:784-90.