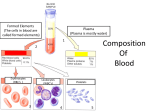
* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download CO - Moodle
Cardiac contractility modulation wikipedia , lookup
Heart failure wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Electrocardiography wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Artificial heart valve wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Cardiac surgery wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Myocardial infarction wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Responding to ill Health Life Science The Cardiovascular System Stanwhit607 (2007) https://commons.wikimedia.org/wiki/File:Humhrt2.jpg 1 Learning outcomes Explain in detail the coronary blood supply (coronary arteries and coronary veins). Discuss the events of the cardiac cycle. Explain the structure and function of the conduction system of the heart and how this relates to normal E.C.G. pattern. Discuss in detail the physiology of blood pressure and the factors which influence it. 2 The Cardiovascular System (revision) Function ?? maintains continuous blood flow to and from all body cells – supplies nutrients and removes wastes Components ?? Heart Blood vessels Blood - ‘CARDIO’ - ‘VASCULAR’ 3 Double Circulation (revision) Pulmonary circulation to and from lungs Systemic circulation to and from body blood from right side of heart only reaches left side via the lungs – i.e. blood in heart does not mix UWS Staff (2015) 4 Conducting System Heart = pump needs coordinated synchronised contractions of cardiac cells initiated and controlled by specialised cells i.e. conducting system: SA node - pacemaker AV node + ‘wiring’ - conduct & spread impulse 5 The pacemakers of the heart Madhero88 (2009) Electrical_conduction_system https://commons.wikimedia.org/wiki/File:Electrical_conduction_system_of_the_heart.svg?uselang=en-gb Lynch (2006) Heart right anatomy http://commons.wikimedia.org/wiki/File:Heart_right_anatomy.jpg?uselang=en-gb Sino-atrial (SA) node (pacemaker) in wall of right atrium impulse spreads from SA node to both atria causes atrial contraction Atrioventricular (AV) node node of neuromuscular cells at base of right atrium very near septum impulse from SA node reaches AV node There is a pause in conduction of impulse from AV node (until atrial contraction + filling of ventricles is complete) 7 impulse passes from AV node to septum & then across walls of both ventricles (Bundle of His, R & L bundle branches, Purkinje fibres) ventricle contracts NB co-ordination of heart beat – 2 atria then 2 ventricles 8 Cardiac cycle events of one heartbeat systole = period of contraction diastole = period of relaxation revise structure of heart & direction of blood flow in order to understand cardiac cycle 9 Cardiac cycle Events of cardiac cycle depend on heart structure, particularly: location & orientation of heart valves pressure of blood in different chambers blood vessels associated with heart Useful animation: http://library.med.utah.edu/kw/pharm/hyper_heart1.html 10 Josiño (2010) https://commons.wikimedia.org/wiki/File:Latidos.gif CARDIAC CYCLE LadyofHats (2008) https://commons.wikimedia.org/wiki/File:Human_healthy_pumping_heart_en.svg Cardiac cycle 1. passive ventricular filling 2. atrial systole 3. ventricular systole 4. ventricular diastole 13 1. Passive ventricular filling blood enters R & L atria, pours passively through open AV valves into ventricles atrioventricular valves open – semilunar (pulmonary & aortic) valves shut atria & ventricles in diastole, pressure in each remains constant pressure in ventricles does not rise, as walls expand to receive incoming blood accounts for 70% of ventricular filling 14 2. Atrial systole SA node discharges atrial contraction, ventricles in diastole 30% of ventricular filling AV valves open, semilunar valves shut pressure rises in both atria & ventricles 15 3. Ventricular systole impulse from AV node ventricular contraction, ventricular pressure rises , AV valves shut when ventricular pressure than BP in systemic & pulmonary arteries semilunar (pulmonary) valves open atria in diastole - filling passively, ventricles in systole AV valves open then shut, semilunar valves shut then open 16 4. Ventricular diastole ventricles relax, pressure falls, semilunar valves shut ventricular pressure falls below atrial pressure, AV valves open back to passive ventricular filling atria in diastole, ventricles in diastole AV valves shut then open, semilunar valves open then shut 17 Click slide to start animation Cardiac Cycle AV (inlet) valve SL (outlet) valve P ventricle contracting relaxing relaxed P PP UWS Staff (2015) 18 Electrocardiogram Diagnostic tool (powerful) Evaluates electrical events in heart via currents generated in body fluids Detects: Mis, Conduction blocks, Arrhythmias 3 recognised wave forms P wave = A contraction QRS complex = V contraction; A repolarization T wave = V repolarization 19 ELECTROCARDIOGRAM (ECG) Anthony Atkielski (2007) SinusRhythmLabels https://commons.wikimedia.org/wiki/File:SinusRhythmLabels.svg?uselang=en-gb Interpretation of ECG P wave: atrial depolarisation - atria about to contract Q, R, S waves: ventricular depolarisation – ventricles about to contract; and atrial repolarization (relaxation of atrial muscle) T wave: ventricular repolarization (relaxation of ventricular muscle) 21 ECG – examples of diagnosis Normal Bundle branch block Madhero88 (2010) https://commons.wikimedia.org/wiki/File:ECGbasic.svg https://commons.wikimedia.org/wiki/File:Bundle_branch_block.svg 22 Coronary Arteries Patrick J. Lynch, (2010) https://commons.wikimedia.org/wiki/File:Coronary_arteries.svg?uselang=en-gb 23 Coronary Arteries Anatomist90 (2011) https://commons.wikimedia.org/wiki/File:Coronary_arteries_1.jpg?uselang=en-gb 24 When does blood flow through coronary circulation? Only during diastole, when aortic valve ‘closes’, opening access to coronary circulation NOTE: increased heart rate > period of diastole shortens > decrease blood flow > conflict with the needs of the heart 25 PHYSIOLOGY OF BP BP pressure exerted by blood on vessel wall Where does this pressure come from ?? • BP drives blood flow – maintains oxygen supply to organs of the body – brain and heart in particular 26 Pressure in the Vascular System OpenStax College (2013) https://commons.wikimedia.org/wiki/File:2109_Systemic_Blood_Pressure.jpg 27 Clinically: BP = pressure in large arteries (~ same throughout body) BP is not constant PULSATILE: max. (systole) = ventricular contraction min. (diastole) = ventricular relaxation Icternol (2015) https://commons.wikimedia.org/wiki/File:Augmentation-index.PNG 28 Blood Pressure Values normal range: systolic: 90 - 140 mmHg diastolic: 60 - 90 mmHg BPs within this range NORMOTENSIVE if SP > 140 mmHg or DP > 90 mmHg HYPERTENSIVE if SP < 90 mmHg or DP < 60 mmHg HYPOTENSIVE Both dangerous 29 Blood Pressure Determinants 1. cardiac output (CO) 2. peripheral resistance (PR) 30 Note: Total Blood Volume also helps determine blood pressure ~ 5 Litres in average person does not vary greatly i.e. total blood vol. NOT used to control BP however: volume of blood in arteries does dictate BP 31 1. Cardiac Output (CO) volume of blood pumped out of ventricle per minute CO = heart rate x stroke volume (beats/min) (mL) SV - vol. of blood pumped out by ventricle per heart beat CO = 75 x 70 - typically 70 mL = 5250 mL/min = 5.25 L/min HR - typically 75 bts/min 32 1. Cardiac Output (CO) CO same for both left and right ventricles HR + SV can be rapidly changed, thus changing CO changes in CO can be used to rapidly control BP e.g. haemorrhage BP HR SV CO 33 2. Peripheral Resistance total vascular resistance to flow Can change with vessel length (doesn’t vary) and blood viscosity (may vary with disease) Vessel radius is the major mechanism determining peripheral resistance radius Resistance due mainly to: arterioles = chief resistance vessels arteriole resistance + hence peripheral resistance can be rapidly changed to control BP 34 Further Determinant Venous return ‘the heart can only pump out what it gets in’ i.e. ventricle must fill before it can pump – this is determined by the volume of blood returning via the veins to the heart i.e. venous return venous return CO 35 Factors Influencing BP BP = CO x p.resistance HR x ANS: sympathetic SV arteriolar resistance CO arteriolar resistance parasympathetic CO changes in BP are corrected for by the ANS (-ve feedback) some hormones e.g. Adrenaline CO arteriolar resistance 36 Factors Influencing BP (contd) temperature e.g. fever HR CO emotions (higher brain) anger CO fear arteriolar resistance anxiety BP • endocrine systems controlling blood volume can influence BP 37 Summary Conducting system Cardiac cycle Coronary circulation VITAL to maintain BP Main determinants: - CO -Blood volume (in arteries) - Peripheral resistance 38