* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Document
Survey
Document related concepts
Transcript
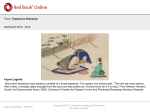
Critical Care of Kidney Transplant Dr yekehfallahphd of nursing Introduction Renal transplantation is the preferred treatment for patients with end-stage renal disease. It offers better quality of life and confers greater longevity than long-term dialysis. 5/25/2017 Dr yekehfallah-phd of nursing -2015 2 History of Kidney Transplantation 1950’s First successful kidney transplant Total body irradiation for immunosuppression Steroids 1960’s Azathioprine 1970’s Polyclonal anitbodies – anti-lymphocyte globulin (now Atgam, Thymoglobulin) 1980’s Cyclosporine (Sandimmune ), “triple drug therapy” Monoclonal antibody, OKT3 (Orthoclone ) in 1985 5/25/2017 Dr yekehfallah-phd of nursing -2015 3 Definitions Allograft : graft between genetically dissimilar individuals of the same species. Autograft : graft in which donor and recipient are the same individual. Xenograft : Donor and recipient belong to different species. 5/25/2017 Dr yekehfallah-phd of nursing -2015 4 Contraindications To Renal Transplantation Absolute : Severe vascular disease. Infection Cancer Relative : Recent malignancy. Coronary artery disease. Active bacterial, fungal, or viral disease. HIV positivity. Social conditions. Others. 5/25/2017 Dr yekehfallah-phd of nursing -2015 5 Kidney Donor Living related. Living unrelated (emotionally motivated). Cadaveric (Brain-dead) Beating and non-beating heart. 5/25/2017 Dr yekehfallah-phd of nursing -2015 6 CRITERIA FOR LIVING DONOR SELECTION - Blood relative. - Highly motivated. - ABO blood group-compatible. - HLA-identical or haploidentical with negative cross-match. - Excellent medical condition with normal renal function. 5/25/2017 Dr yekehfallah-phd of nursing -2015 7 CRITERIA FOR CADAVER DONOR SELECTION - - Irreversible brain damage. Normal renal function appropriate for age. No evidence of preexisting renal disease. No evidence of transmissible diseases. ABO blood group-compatible. Negative cross-match. Best HLA match possible, particularly at the DR and B loci. 5/25/2017 Dr yekehfallah-phd of nursing -2015 8 Matching between Recepient And Donor A- Tissue typing Determined by 6 antigens located on cell surface encoded for by the HLA gen located on the short arm of chromosom 6. Class I antigens (HLA-A and HLA-B) are expressed on the surface of most nucleated cells. Class II antigen (HLA-DR) are expressed on surface of APC and activated lymphocytes. These 6 antigens are refered to as major transplant antigens. The match between donor and recepient can range from 0 to six. 5/25/2017 Dr yekehfallah-phd of nursing -2015 9 Matching between Recepient And Donor B- Cross matching A laboratory test that determines weather a potential transplant recepient has preformed antibodies against the HLA antigens of the potential donor. (Donor Lymphocytest +Recepient Serum) A Final CM is mandatory C- Compatible ABO blood group. 5/25/2017 Dr yekehfallah-phd of nursing -2015 10 Effect Of HLA Matching On The Graft Outcome Data from large registries indicate that, the better the HLA-match, the better the long-term survival of the allograft. The benefits of matching are particularly notworthy in recipients of kidneys from donors with zero missmatch. The benefits of lesser degrees of matching have become less obvious with the use of newer and more potent immunosuppressive drugs. Matching for DR antigens are more favorable than others. 5/25/2017 Dr yekehfallah-phd of nursing -2015 11 Factors Influencing The Longivity Of Renal Allograft Age HLA matching Delayed graft function Ischemia time. Number of acute rejection episodes. Native kidney disease. Ethnicity. Others 5/25/2017 Dr yekehfallah-phd of nursing -2015 12 Major Causes Of Long-Term Allograft Failure Chronic rejection. Death with functioning graft. 5/25/2017 Dr yekehfallah-phd of nursing -2015 13 Most Common causes Of Death After Kidney Transplantation Cardiovascular disease. Infection. 5/25/2017 Dr yekehfallah-phd of nursing -2015 14 GENERAL PRINCIPLES Renal transplant is the most common solid organ transplant Improves quality of life and survival compared to dialysis therapy for patients with chronic kidney disease Diabetic and hypertensive nephropathy are the most common causes of chronic kidney disease leading to transplant Underlying disease and its pathophysiology must be considered in pretransplant evaluation and postoperative management 5/25/2017 Dr yekehfallah-phd of nursing -2015 15 Basics of Transplantation Kidney transplantation is the most effective therapy for end-stage renal disease. The transplanted organ can come from either a live donor or deceased donor. Most deceased donor organs come from brain dead donors. Non-standard criteria donors: Expanded criteria donors (ECD). Donation after cardiac death (DCD). 5/25/2017 Dr yekehfallah-phd of nursing -2015 16 Recipient Selection Very few contraindications. General medical condition. Cardiovascular screening. Age-appropriate routine cancer screening (pap smear, mammography, colonoscopy, PSA). Infection (HIV, Hepatitis, TB). Presence of preformed antibody (PRA). Pregnancy, prior transplant, blood transfusion Psychosocial evaluation, including compliance. 5/25/2017 Dr yekehfallah-phd of nursing -2015 17 Benefits of Transplantation Life expectancy Cardiovascular benefits Quality of life Socioeconomic benefits 5/25/2017 Dr yekehfallah-phd of nursing -2015 18 Quality of Life Numerous studies have detailed improved quality of life. Life satisfaction, physical and emotional wellbeing and ability to return to work higher in transplant recipients. Uremic complications more fully reversed. Fertility returns. 5/25/2017 Dr yekehfallah-phd of nursing -2015 19 Socioeconomic Benefits Increased rates of return to work. Cost to society Mean cumulative costs of dialysis and transplantation are equal for first 3-4 years, then lower for transplantation. 5/25/2017 Dr yekehfallah-phd of nursing -2015 20 PRETRANSPLANT EVALUATION Cardiovascular Assessment: -History of coronary artery disease - symptoms of angina or congestive heart failure -recent change in exercise tolerance - new ischemic changes on ECG - Decreased pulse or bruit on peripheral vascular examination - new murmur on cardiac examination. Prevention: - Preoperative and postoperative B²-blocker therapy (atenolol 5 mg intravenously preoperatively and 50 to 100 mg orally daily for at least the first postoperative week) -monitoring for hyperkalemia, bradycardia, and hypotension - Consider continuing or starting aspirin for patients with multiple risk factors. 5/25/2017 Dr yekehfallah-phd of nursing -2015 21 PRETRANSPLANT EVALUATION Infection Assessment: -Signs or symptoms of active infection -assessment of indwelling hemodialysis or peritoneal dialysis catheters and hemodialysis access grafts - Culture and cell count of peritoneal fluid from Tenckhoff catheter. Prevention: -Postpone transplant until active infection has been treated. -Cephalosporin therapy for perioperative antibacterial prophylaxis 5/25/2017 Dr yekehfallah-phd of nursing -2015 22 PRETRANSPLANT EVALUATION Preoperative dialysis Assessment : - hypervolemia - Determine daily urine output - hyperkalemia or severe metabolic acidosis. Acute dialysis treatment to: - correct electrolyte abnormalities and volume status - avoiding excessive volume removal 5/25/2017 Dr yekehfallah-phd of nursing -2015 23 INTRAOPERATIVE CARE Careful attention to volume status is critical to avoid hypovolemia that will impair renal perfusion and contribute to delayed graft function (need for dialysis therapy during the first week after transplant, a risk factor for acute rejection). 5/25/2017 Dr yekehfallah-phd of nursing -2015 24 INTRAOPERATIVE CARE Intravascular volume status should be maintained at adequate central venous pressure without predisposing to pulmonary edema. Central venous pressure monitoring is recommended to maintain pressure approximately between 5 and 10 cm H2O 5/25/2017 Dr yekehfallah-phd of nursing -2015 25 INTRAOPERATIVE CARE Consider pulmonary artery catheterization to assess hemodynamics in patients with significantly decreased left ventricular function 5/25/2017 Dr yekehfallah-phd of nursing -2015 26 5/25/2017 Dr yekehfallah-phd of nursing -2015 27 5/25/2017 Dr yekehfallah-phd of nursing -2015 28 5/25/2017 Dr yekehfallah-phd of nursing -2015 29 Anatomy of Renal Transplantation 5/25/2017 Dr yekehfallah-phd of nursing -2015 30 An adult donor kidney transplanted to the left iliac fossa of an adult recipient 5/25/2017 Dr yekehfallah-phd of nursing -2015 31 Graft Prognosis Directly related to source of donor kidney. Recipients of cadaveric kidneys have more episodes of rejection and lower graft survival rates. Graft survival rates for kidneys from living donor is 95% 1 yr and 76% 5 yrs vs graft survival from a cadaveric kidney donor is 89% 1 yr and 61% 5 yrs. 5/25/2017 Dr yekehfallah-phd of nursing -2015 32 Morbidity Infection (most common cause of M&M in first year post transplantation) and graft failure occur. HT occurs in 75-85% of all renal transplant recipients. Hyperlipidaemia 60% CVS disease 15.8 – 23% DM 16.9 – 19.9% (more likely to be present before transplantation and new onset DM after transplantation is related to corticosteriod use.) Osteoporosis 60% Malignant neoplasm 14% - related to the degree of immunosupression 5/25/2017 Dr yekehfallah-phd of nursing -2015 33 Mortality Survival of pts after transplantation from a liver donor is 98% at 1 yr and 91% 5 yrs. Survival of pts who receive cadaveric organs is 95% 1 yr and 81% 5 yrs. 5/25/2017 Dr yekehfallah-phd of nursing -2015 34 POSTOPERATIVE CARE Postoperative management is determined by initial allograft function: - Chest radiograph - frequent electrolyte monitoring to assess volume and metabolic status (sodium, potassium, calcium, and magnesium levels are essential 5/25/2017 Dr yekehfallah-phd of nursing -2015 35 POSTOPERATIVE CARE Oliguria (urine output <20 mL/h) requires careful attention to intravascular volume status. If euvolemic or hypervolemic, then aggressive fluid resuscitation should be avoided and complications such as urinary obstruction, vascular thrombosis, and acute tubular necrosis must be considered. Hyperkalemia must be identified and treated 5/25/2017 Dr yekehfallah-phd of nursing -2015 36 POSTOPERATIVE CARE With immediate graft function, urine output can reach 1 L/h. Careful fluid and electrolyte replacement is required to avoid hypovolemia and electrolyte depletion 5/25/2017 Dr yekehfallah-phd of nursing -2015 37 POSTOPERATIVE CONSIDERATIONS Surgical complications 1/Hemorrhage Risk of occurrence 1.9% to 12%. Increased risk for patients requiring preoperative reversal of chronic Coumadin anticoagulation. Frequently due to vascular anastomotic bleeding, but in half of cases no obvious source is identified 5/25/2017 Dr yekehfallah-phd of nursing -2015 38 POSTOPERATIVE CONSIDERATIONS Surgical complications 2/Allograft thrombosis Risk factors (1) Hypotension and hypovolemia (2) Hypercoagulable state (antiphospholipid antibody syndrome; factors C, S, or antithrombin III deficiency; factor V Leiden mutation; acute humoral rejection). (3) Severe peripheral vascular disease (increased risk of intimal flap and other anastomotic complications). (4) Multiple small renal arteries 5/25/2017 Dr yekehfallah-phd of nursing -2015 39 POSTOPERATIVE CONSIDERATIONS Presentation, diagnosis, and treatment (1) Sudden oligoanuria (arterial thrombosis), gross hematuria, allograft pain and swelling (venous thrombosis). (2) Doppler ultrasound including visualization of flow in renal artery and vein confirms diagnosis. (3) Almost always requires allograft nephrectomy 5/25/2017 Dr yekehfallah-phd of nursing -2015 40 POSTOPERATIVE CONSIDERATIONS Prevention (1) Maintain adequate blood pressure and intravascular volume. (2) Aspirin for severe peripheral vascular disease. (3) IV heparin for hypercoagulable state. No definitive evidence-based guidelines are available, but therapeutic target partial thromboplastin time (PTT) of 1.5 to 1.9 times the upper limit of normal PTT range has been suggested with low risk of bleeding 5/25/2017 Dr yekehfallah-phd of nursing -2015 41 POSTOPERATIVE CONSIDERATIONS Surgical complications 3/Urologic a/Significant hematuria with passage of clots may require continuous bladder irrigation. Avoid excessively high intravesical pressures that can lead to rupture of the ureteroneocystotomy 5/25/2017 Dr yekehfallah-phd of nursing -2015 42 POSTOPERATIVE CONSIDERATIONS b/Urinary leak (1) Occurs at the ureteroneocystostomy due to anastomotic complication or distal ureteral ischemia and necrosis. Patient may present with sudden oligoanuria or significant increase in wound drainage. (2) Ultrasound may identify perigraft fluid collection (urinoma), nuclear medicine scan may identify extravasation of tracer from ureter, and increased creatinine level of wound drainage (when compared to serum creatinine) will confirm urine leak. (3) In some cases, replacement of Foley catheter with bladder decompression is sufficient. Surgical reexploration with ureteral reimplantation and stent placement may be required 5/25/2017 Dr yekehfallah-phd of nursing -2015 43 POSTOPERATIVE CONSIDERATIONS Surgical complications 4/Wound a/Infection and dehiscence are infrequent complications (less than 5%). Risk is increased with obesity (body mass index >30) and combined use of sirolimus and steroids for immunosuppression, which both impair wound healing 5/25/2017 Dr yekehfallah-phd of nursing -2015 44 POSTOPERATIVE CONSIDERATIONS b/Lymphoceles requiring therapy occur in approximately 5%. Patients present with ureteral or venous obstruction of the graft, which are often associated with ipsilateral lower extremity edema. Treatment: laparoscopic internal drainage through a peritoneal window. External drainage and sclerotherapy are less effective 5/25/2017 Dr yekehfallah-phd of nursing -2015 45 POSTOPERATIVE CONSIDERATIONS MEDICAL COMPLICATIONS 1/Cardiovascular Because of the increased risk of myocardial infarction in patients with end-stage renal disease (ESRD), a high index of suspicion is required, especially with prolonged intraoperative hypotension or postoperative pulmonary edema. Pericarditis occurs in approximately 2%. Causes include uremia and infection, especially cytomegalovirus (CMV; unusual in the immediate postoperative period). 5/25/2017 Dr yekehfallah-phd of nursing -2015 46 POSTOPERATIVE CONSIDERATIONS MEDICAL COMPLICATIONS 2/Metabolic Hyperkalemia can occur with delayed graft function. Immediate therapy is required with calcium chloride, insulin and dextrose, and bicarbonate. Kayexalate or dialysis is required if diuresis to eliminate potassium cannot be induced. Hypokalemia may occur with large-volume diuresis early postoperatively, requiring frequent monitoring and repletion. Hypocalcemia, hypophosphatemia, and hypomagnesemia can occur with large-volume diuresis and early renal tubular dysfunction. Frequent electrolyte monitoring (at least every 12 hours) and repletion are required 5/25/2017 Dr yekehfallah-phd of nursing -2015 47 POSTOPERATIVE CONSIDERATIONS MEDICAL COMPLICATIONS 3/Infection in the early postoperative period is due to bacterial etiology similar to that for other surgical patients. Risk is greatest in patients with diabetes or those over 60 years old. Prophylactic antibiotic therapy with cephalosporins is required 5/25/2017 Dr yekehfallah-phd of nursing -2015 48 POSTOPERATIVE CONSIDERATIONS MEDICAL COMPLICATIONS 4/Neurologic Stroke is a rare early postoperative complication. Risk is greatest in patients with any significant vascular disease. Stroke should be considered in the setting of a postoperatively unexplained altered level of consciousness or with other neurologic changes. New onset seizure is also uncommon. Uremia in the setting of delayed graft function, stroke, or drug toxicity with OKT-3 is a common cause 5/25/2017 Dr yekehfallah-phd of nursing -2015 49 Immunosuppressive Medications Induction: Corticosteroids Anti-thymocyte globulin (ATG) IL-2 receptor antagonists Maintenance: Corticosteroids Calcineurin inhibitors (CNIs) mTOR inhibitors Antimetabolites 5/25/2017 Dr yekehfallah-phd of nursing -2015 50 Immunosuppressive Medications Treatment of Rejection: Corticosteroids Anti-thymocyte globulin Intravenous Immunoglobulin (IVIG) Rituximab Plasmapheresis 5/25/2017 Dr yekehfallah-phd of nursing -2015 51 Corticosteroids Used for induction, maintenance and treatment of rejection. Mechanism of action: Inhibit function of dendritic cells. Inhibit translocation to nucleus of NF-κB. Suppress production of IL-1, IL-2, IL-3, IL-6, TNF-α, and γ-IFN. Adverse effects numerous and well-known. 5/25/2017 Dr yekehfallah-phd of nursing -2015 52 Corticosteroids Component of >80% of transplant protocols. Given IV at high doses (250-500 mg/day) for induction or treatment of rejection. Tapered to maintenance dose of 5-10 mg/day in early post-transplant phase. Should NOT be tapered off: increased risk of rejection and graft loss! Steroid free regimen: overall some benefits but graft survival likely worse. 5/25/2017 Dr yekehfallah-phd of nursing -2015 53 Anti-thymocyte Globulin (Thymoglobulin) Used for induction and treatment of rejection. Prepared by immunization of rabbits with human lymphoid tissue. Causes depletion of peripheral blood lymphocytes. Administered generally via central line for 3-10 days. Premedication required: acetaminophen, corticosteroids and antihistamine. 5/25/2017 Dr yekehfallah-phd of nursing -2015 54 Anti-thymocyte Globulin: Adverse Effects Infusion-related reactions: chills, fevers, arthralgias. Lymphopenia. Thrombocytopenia. Prolonged immunosuppression: increased risk of opportunistic infections (PCP, CMV, fungal). Possibly increased risk of BK virus nephropathy. 5/25/2017 Dr yekehfallah-phd of nursing -2015 55 IL-2 Receptor Blockers Basiliximab (Simulect®) and Daclizumab (Xenapax®). Block CD25 (IL-2 receptor) on activated T cells. Used for induction only. Almost no side effects, but also much less potent. 5/25/2017 Dr yekehfallah-phd of nursing -2015 56 Calcineurin Inhibitors Used for maintenance immunosuppression. Two agents in clinical practice: Cyclosporine (Sandimmune, Gengraf, Neoral, generic; CysA) Tacrolimus (Prograf, generic; FK506). Generics NOT clinically therapeutically equivalent. At present are key to maintenance immunosuppression and a component of the majority of transplant protocols. 5/25/2017 Dr yekehfallah-phd of nursing -2015 57 Calcineurin Inhibitors: Dosing and Monitoring Both medications are generally dosed twice per day, 12 hrs apart. Trough levels monitored: check approximately 12 hrs after last dose. In some cases C2 levels might be checked 2 hrs after administration. Cyclosporine is 35-40% bioavailable, tacrolimus approximately 25%. Oral to IV conversion 3-4:1. Both are metabolized by cytochrome P450 3A4 & 3A5. 5/25/2017 Dr yekehfallah-phd of nursing -2015 58 Calcineurin Inhibitors: Interactions 5/25/2017 Dr yekehfallah-phd of nursing -2015 59 Calcineurin Inhibitors: Interactions Drugs to use with caution: NSAIDs—avoid. Amphotericin B & Aminoglycosides– worsened nephrotoxicity. ACEi & ARBs– use with caution. Statins– avoid lovastatin, start others at lowest possible dose. 5/25/2017 Dr yekehfallah-phd of nursing -2015 60 Calcineurin Inhibitors: P-Glycoprotein P-Glycoprotein (P-gp, also known as MDR1) is an ABC-transporter found among other places, in the intestine. It is thought to have evolved as a defense mechanism against harmful substances. It acts as an efflux pump for many substances including drugs (CNIs, colchicine, some cancer chemotherapeutic agents, digoxin, corticosteroids, antiretrovirals). Decreased P-gp expression, such as in diarrhea, leads to elevated drug levels. 5/25/2017 Dr yekehfallah-phd of nursing -2015 61 Calcineurin Inhibitors: Adverse Effects Nephrotoxicity: Functional decrease in blood flow from afferent arteriolar vasoconstriction. Thrombotic microangiopathy (rare). Chronic interstitial fibrosis. Hyperkalemia, hypomagnesemia and type IV renal tubular acidosis. Cyclosporine thought to be more nephrotoxic. 5/25/2017 Dr yekehfallah-phd of nursing -2015 62 Calcineurin Inhibitors: Adverse Effects Cyclosporine Tacrolimus Hypertension ++ + Pancreatic islet toxicity + ++ Neurotoxicity + ++ Hirsutism + - Hair loss - + Gum hypertrophy + - GI side effects - + Gastric motility - + Dyslipidemia + - Hyperuricemia ++ + +/↓Mg2+ ↑K 5/25/2017 + of nursing -2015 Dr yekehfallah-phd + 63 mTOR Inhibitors Target site is the mammalian target of rapamycin (mTOR), a key regulatory kinase in cell division. Sirolimus (Rapamune®) only available mTOR inhibitor in the US. Administered once daily, 24-hour trough levels monitored. Also metabolized by P450 3A system, with interactions similar to the CNIs. 5/25/2017 Dr yekehfallah-phd of nursing -2015 64 mTOR Inhibitors Target site is the mammalian target of rapamycin (mTOR), a key regulatory kinase in cell division. Sirolimus (Rapamune®) only available mTOR inhibitor in the US. Administered once daily, 24-hour trough levels monitored. Also metabolized by P450 3A system, with interactions similar to the CNIs. 5/25/2017 Dr yekehfallah-phd of nursing -2015 65 Antimetabolites Azathioprine (Imuran®, generic) is a purine analogue that is incorporated into RNA and inhibits cell replication. A mainstay of transplantation for 30 years, it has largely been replaced by the below drugs. Mycophenolate mofetil (Cellcept®) and enteric-coated mycophenolate sodium (Myfortic®) are prodrugs of mycophenolic acid (MPA), an inhibitor of inosine monophosphate dehydrogenase (IMPDH). 5/25/2017 Dr yekehfallah-phd of nursing -2015 66 Antimetabolites: Adverse Effects Azathioprine: Bone marrow suppression. Hepatitis. Azathioprine is inactivated by xanthine oxidase, therefore should not be used in combination with allopurinol. MPA prodrugs: GI toxicity: diarrhea, nausea, esophagitis. Leukopenia and anemia. Not different between formulations. 5/25/2017 Dr yekehfallah-phd of nursing -2015 67 Antimetabolites: Interactions Azathioprine: Allopurinol Other marrow suppressive drugs MPA prodrugs: Cyclosporine Antacids Cholestyramine Ferrous sulfate OK to use with allopurinol 5/25/2017 Dr yekehfallah-phd of nursing -2015 68 Antimetabolites: Interactions Azathioprine: Allopurinol Other marrow suppressive drugs MPA prodrugs: Cyclosporine Antacids Cholestyramine Ferrous sulfate OK to use with allopurinol 5/25/2017 Dr yekehfallah-phd of nursing -2015 69 Rituximab Used in the treatment of antibody-mediated rejection. Monoclonal antibody directed at CD20 antigen on B lymphocytes. Causes rapid and sustained depletion of B lymphocytes. Does not have direct activity against plasma cells and memory B cells, which do not express CD20. Adverse events: infusion reactions, and increased susceptibility to infection. 5/25/2017 Dr yekehfallah-phd of nursing -2015 70 Other Agents OKT3 Used for induction and treatment of rejection, now largely replaced by anti-thymocyte globulin. Monoclonal antibody against CD3 Severe infusion reactions (pulmonary edema & capillary leak syndrome). Alemtuzumab (Campath-1H) Monoclonal anti-CD52 antibody Toxicities include bone marrow suppression and severe infections Leflunomide (Arava) Dihyroorotate dehydrogenase (DHODH) inhibitor. Used in certain clinical settings as an adjunct immunosuppressive. 5/25/2017 Dr yekehfallah-phd of nursing -2015 71 Common Complications of Transplantation Early complications Surgical complications Delayed or slow graft function Lymphocele Acute rejection Acute cellular rejection Antibody-mediated rejection Infectious complications Cytomegalovirus BK virus Others Malignancy 5/25/2017 Chronic allograft dysfunction Dr yekehfallah-phd of nursing -2015 72 Surgical Complications Graft thrombosis: Caused by thrombosis of donor renal artery or vein. Usually happens in first week. Diagnosed by ultrasound with doppler studies. Almost always requires explant of kidney. Urine leak: Elevated creatinine. May or may not have abdominal pain. Diagnose with nuclear medicine scans (DTPA or MAG3). Surgical repair and/or relief of obstruction. 5/25/2017 Dr yekehfallah-phd of nursing -2015 73 Lymphocele Collection of lymph caused by leakage from iliac lymphatics. Presents several weeks post-operatively. Symptoms: Compression of kidney, ureter, bladder: obstructive uropathy and ARF. Compression of iliac vessels: unilateral lower extremity edema and DVT. Abdominal mass. Treatment is surgical. 5/25/2017 Dr yekehfallah-phd of nursing -2015 74 Acute Rejection May present with ARF or proteinuria. Diagnosis made by biopsy. Pathology is reported according to Banff classification. Acute cellular rejection: treat with steroids or ATG based on severity Antibody-mediated rejection: may require steroids, ATG, rituximab, IVIG or plasmapheresis based on severity and setting. 5/25/2017 Dr yekehfallah-phd of nursing -2015 75 Cytomegalovirus Most common viral infection after transplantation. Various degrees of severity: Asymptomatic CMV viremia CMV syndrome (viremia plus constitutional symptoms) CMV end-organ or invasive disease (hepatitis, gastritis, colitis, pneumonitis) Risk factors: Use of antibody induction Donor seropositive, recipient seronegative status 5/25/2017 Dr yekehfallah-phd of nursing -2015 76 Cytomegalovirus Clinical presentation: Asymptomatic (detected on screening) Neutropenia Malaise & constitutional symptoms GI CMV: gastritis, colitis, esophagitis Clinical hepatitis, pneumonitis Prophylaxis: All patients at risk (D+/R+, D-/R+ or D+/R-) receive valganciclovir prophylaxis for 4.5-6 months. “Preemptive” strategy with CMV PCR monitoring. 5/25/2017 Dr yekehfallah-phd of nursing -2015 77 Cytomegalovirus CMV PCR assays have largely replaced pp65 antigenemia for diagnosis. Low-level viremia can be treated with full-dose oral valganciclovir (900 mg bid, dose-adjusted for renal function). High-grade viremia or invasive disease requires 2-4 week course of IV ganciclovir, which may be followed by oral valganciclovir. Ganciclovir-resistant cases might require foscarnet or cidofovir. 5/25/2017 Dr yekehfallah-phd of nursing -2015 78 BK Virus Disease BK virus is a member of the polyomavirus family. An increasingly important cause of allograft failure. Latent in genitourinary tract and reactivated by immunosuppression. Usually presents in first year after transplantation. Asymptomatic viruria or viremia BK-associated interstitial nephritis BK virus nephropathy 5/25/2017 Dr yekehfallah-phd of nursing -2015 79 BK Virus Disease Screening is by BK viral PCR in blood or urine. Presence of BK virus titers >10,000 is suggestive but not diagnostic of BK nephropathy. Diagnosis can only be established by biopsy. Options for therapy: Judiciously reduce immunosuppression Use of leflunomide IVIG (especially in simultaneous rejection & BK nephropathy). 5/25/2017 Dr yekehfallah-phd of nursing -2015 80 BK Virus Monitoring Algorithm 5/25/2017 Dr yekehfallah-phd of nursing -2015 81 Other Infections Transplant patients have increased susceptibility to all other common infections. Opportunistic infections can also be seen: Pneumocystis jirovicii pneumonia Candida infection Toxoplasmosis Nocardiosis Cryptococcus infections 5/25/2017 Dr yekehfallah-phd of nursing -2015 82 Malignancy Recipient of organ transplants are at higher risk of developing malignancy. May be related to impaired immune surveillance as a result of immunosuppression. Skin cancer most common: sun protection mandatory. Routine cancer screening. Specific malignancies: Kaposi sarcoma Post-transplant lymphoproliferative disorder (PTLD) 5/25/2017 Dr yekehfallah-phd of nursing -2015 83 Chronic Allograft Dysfunction Persistent rise in serum creatinine and worsening GFR over weeks to months is termed chronic allograft dysfunction. Histological counterpart is chronic allograft nephropathy (CAN). Characterized by nonspecific interstitial fibrosis and tubular atrophy. Usually irreversible and will lead to allograft failure and need for dialysis or retransplantation. 5/25/2017 Dr yekehfallah-phd of nursing -2015 84 Chronic Allograft Dysfunction: Why Do Grafts Fail? Chronic low-grade immune injury Long-standing hypertension Recurrent disease (diabetic nephropathy or glomerulonephritis) Repeated episodes of acute rejection Donor disease Calcineurin inhibitor nephrotoxicity 5/25/2017 Dr yekehfallah-phd of nursing -2015 85 Long Term Complications in Renal Transplantation 5/25/2017 Dr yekehfallah-phd of nursing -2015 86 INFECTIONS MALIGNANCY BONE DISEASE CARDIOVASCULAR DISEASE,HYPERTENTION POST TRANSPLANT D.M CATARACT POST TRANSPLANT ERYTHROCYTOSIS CHRONIC REJECTION 5/25/2017 Dr yekehfallah-phd of nursing -2015 87 ? 5/25/2017 Dr yekehfallah-phd of nursing -2015 88