* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Lung Scan
Survey
Document related concepts
Transcript
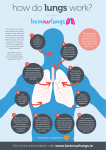
Respiratory System VNSG 1420 Anatomy & Physiology Chapter 16 Respiration Process by which oxygen is obtained from the environment & delivered to the cells (scientific definition) Carbon dioxide is transported to outside of body in a reverse pathway 3 phases of respiration Pulmonary ventilation External exchange of gases Internal exchange of gases See Figure 16-1, p 306 Three Phases of Respiration Pulmonary Ventilation air exchanged between atmosphere & air sacs of lungs by inspiration & expiration External exchange of gases oxygen passes from air sacs into blood & carbon dioxide passes out of blood by diffusion (lungs & environment) Internal exchange of gases oxygen carried to cells & carbon dioxide carried from tissue cells to lungs in circulating blood (blood & body cells) Cellular Respiration Oxygen is taken into cell & used in breakdown of nutrients with the release of energy Carbon dioxide is waste product of cellular respiration Respiratory System Conducts air into lungs Exchange of oxygen & carbon dioxide between atmosphere & blood Components (anatomy) Nasal cavities Pharynx - throat Larynx - voice box Trachea - windpipe Bronchi Nasal Cavities Nostrils (nares) - initial site of air entry Nasal cavities - 2 spaces inside nostrils - separated by septum Septum & walls - mucous membrane covering with blood vessels to deliver heat & moisture Secrete up to 1 quart of liquid per day Mucous membranes filter out foreign bodies, warm & moisten air More on Nasal Cavities . . . Conchae 3 paired bony projections in lateral walls - increase surface for travel of air Air changes with contacting lining of nose Foreign bodies filtered by nostril hairs or surface mucus Air warmed by vascular membrane blood Air moistened by liquid secretions Sinuses small mucous membrane lined cavities in bones of skull - communicate with nasal cavities Pharynx Pharynx / throat - carries air to respiratory tract & carries food & liquids to digestive system Nasopharynx - superior (upper) part behind nasal cavity Oropharynx - middle section behind mouth Laryngeal pharynx – inferior (lowest) portion opens into larynx (voice box) toward front & toward esophagus in back See Figure 16-2, p 307 Pharynx Larynx Larynx / voice box - cartilage framework between pharynx & trachea Adam’s apple - projection of thyroid cartilage Vocal cords - paired mucous membrane folds - for producing speech - air flow cause vibrations Glottis - space between vocal cords Epiglottis - leaf shaped cartilage - covers larynx during swallowing See Figures 16-3 & 16-4, pp 308 & 309 Larynx Trachea Trachea / windpipe - conducts air between larynx & lungs Tubular - from lower larynx edge to upper chest above heart C- shaped (horseshoe) frame of cartilage - to keep structure open Framework of separate cartilages Open sections in cartilage lined up in back so esophagus can bulge into area when swallowing See Figures 16-2 & 16-3, pp 307 & 308 Trachea Main Stem Bronchi Main Stem Bronchi branches off trachea enter lungs then subdivide into secondary bronchi Walls contain cartilage - to keep airways open Right bronchus - larger diameter than left - extends down in vertical direction (inhaled foreign bodies usually enter right bronchus) Each bronchus enters lung at hilum - notched depression Blood vessels & nerves also connect with lungs at hilum region of each lung Bronchi / Bronchioles Lining of Air Passages Simple columnar epithelium - appear stratified, but are not Pseudo-stratified - falsely stratified See Figure 16-6, page 310 Epithelial cells have cilia to filter out impurities & to move fluids toward throat Impurities eliminated by coughing, sneezing or blowing nose Lungs Organs of gas exchange - diffusion of gases occurs through thin delicate tissues Left lung indented to accommodate heart Right lung - 3 lobes with 3 secondary bronchi Left lung - 2 lobes with 2 secondary bronchi Bronchi divide like tree branches Bronchioles - smallest conducting tubes - no cartilage - mostly smooth muscle Bronchial tree – bronchi & bronchioles Lung Structures & Related Structures Lobes Bronchi Bronchioles Alveoli Lung cavities Pleura Mediastinum Diaphragm Alveoli Clusters of tiny air sacs where gases are exchanged located at end of terminal bronchioles Single squamous cell epithelium wall easy passage of gases entering & leaving blood circulating through millions of capillaries covering alveoli Surfactant reduces alveoli surface tension - eases expansion of lungs & prevents collapse of alveoli Lung Cavities & Pleura Lungs occupy thoracic cavity Diaphragm - muscular partition between thoracic & abdominal cavities Pleura - doubled membrane sac - encloses each lung Visceral pleura - attached to lung surface Parietal pleura - attached to chest wall Pleural space - between layers of pleura allows lung surfaces to slide easily & enlarge effortlessly as thoracic volume changes during breathing More on Lung Cavities . . . Mediastinum - space & organs between lungs Contains heart, great blood vessels, esophagus trachea & lymph nodes See Figure16-2, page 307 Process of Respiration Respiration - exchange of gases in lungs & transport of gases in blood Pulmonary ventilation / breathing movement of air in & out of the lungs 2 phases of ventilation Inhalation (inspiration) – active phase Drawing of air into lungs Exhalation Expulsion (expiration) - passive phase of air from lungs Inhalation Respiratory muscles contract – active phase Diaphragm flattens & presses abdominal organs down & forward - rib cage rises up & out Thoracic cavity size increases gas pressure decreases with cavity Air drawn into lung by suction Compliance ease with which lungs & thorax can be expanded Exhalation Muscles of respiration relax – passive phase Thorax decreases in size Ribs & diaphragm return to usual positions Lungs become smaller during exhalation Forceful exhalation uses muscles of chest & abdomen See Figure 16-7, p 311 Lung Volume Lung volumes used to evaluate respiratory function Tidal volume - amount of air moved in & out of lungs in quiet relaxed breathing Residual volume - volume of air that is always in the lungs See Table 16-1, p 312 & Figure 16-9, p 313 Lung Capacity Lung capacity = tidal volume + residual volume Vital capacity - amount of air that can be expelled from lungs by maximum exhalation following maximum inhalation Total lung capacity - volume of air in lung after maximum inhalation Functional residual capacity - amount of air in lungs after normal inhalation Gas Exchange in the Lungs Gases move from area of higher concentration to area of lower concentration (diffusion) Respiratory membrane - thin & moist separates alveolar wall from capillary walls External exchange gases move between alveoli & capillary blood Internal exchange occurs between tissues and blood - oxygen leaves blood as carbon dioxide enters from tissue cells More on Gas Exchange . . . Inspired air = 21 % oxygen (O2) & 0.04 % carbon dioxide (CO2) Expired air = 16 % oxygen (O2) & 3.5 % carbon dioxide (CO2) Diffusion - 2 way process - takes place through wall of alveoli & capillaries around alveoli See Figure 16-10, p 314 Gas Transport Oxygen almost totally bound to heme portion of hemoglobin in RBCs Separates from hemoglobin when oxygen concentration is low (in tissues) Oxygen (O2) has to separate from hemoglobin to be able to enter cells Carbon dioxide (CO2) - most carried as bicarbonate ion Regulates pH of blood Partial Pressure of Gases Air is mixture of gases Gas concentrations - expressed as pressures Oxygen (O2) & carbon dioxide (CO2) exert only partial pressures PO2 - partial pressure of O2 PCO2 - partial pressure of CO2 Transport of Oxygen (O2) O2 bound to heme portions is released as concentrations (partial pressure) of O2 drops in tissues O2 must separate from hemoglobin to enter cells Arterial blood in systemic arteries & pulmonary veins - 97 % O2 saturation Venous blood in systemic veins & pulmonary arteries - 70 % O2 saturation - cells take up other 27 % Transport of Carbon Dioxide CO2 - constantly produced in tissues Byproduct of metabolism CO2 diffuses from cells into blood for transport to lungs in 3 ways 10 % dissolved in plasma & fluid in RBCs 15% combined with hemoglobin protein & plasma proteins 75% transported as bicarbonate ion – from CO2 dissolving in blood fluids More on Carbon Dioxide Transport . . . Bicarbonate ion formed slowly in plasma Carbonic anhydrase (enzyme) - aids rapid formation of bicarbonate ion in RBCs Carbonic acid - ionizes into bicarbonate & hydrogen ions Reactions reverse when blood reaches lungs & CO2 is exhaled CO2 + H2O ↔ H2CO3 ↔ H+ + HCO3carbonic acid hydrogen bicarbonate ion ion Carbon Dioxide & Acid-Base Balance CO2 - important in regulating blood pH (acid-base balance) Exhalation of CO2- in pH Blood becomes more base (alkaline) Retention of carbon dioxide - in pH Blood becomes more acid as blood CO2 increases Bicarbonate ion - buffer to keep pH of 7.4 Regulation of Respiration Primary control of respiration occurs in respiratory control centers located in medulla oblongata & pons of brain stem Centers respond to changes in hydrogen ion concentrations in cerebrospinal fluid Blood chemistry changes are detected by chemoreceptors outside medulla H+ ions related to blood CO2 concentration Nervous System Control Respiratory control center located partly in medulla & partly in pons of central nervous system Main part of control center in medulla - sets basic pattern of respiration - can be modified by pons centers Breathing - continuously regulated O2, CO2 & acid stay within normal limits Phrenic nerve - controls diaphragm More on Nervous System Control . . . Motor nerve fibers from medulla centers extend into cervical (neck) part of spinal cord On to phrenic nerve to diaphragm Respiratory centers in brain stem are under involuntary control Diaphragm & other breathing muscles can control breathing rate & depth by voluntary control of messages from cortex brain centers Chemical Control Central & peripheral chemorecptors detect changes in CO2, hydrogen ion, & O2 composition of blood to regulate breathing Central - located near medulla respiratory centers – respond to ↑ CO2 levels Peripheral – located in neck & aortic arch - respond to considerably low O2 levels CO2 is main controller of respiration Breathing must when CO2 levels Breathing / Respiratory Rates One cycle of inhalation & exhalation counts as 1 breath Normal adult = 12-20 per minute Children = 20-40 per minute Higher in infants Count for at least 30 seconds Best to count if patient is unaware Abnormal Ventilation Hyperventilation High O2 levels Low CO2 level (hypocapnia) Increase blood pH (alkalosis) Hypoventilation Insufficient air in alveoli Decrease blood pH (acidosis) Lung Scan Altered Breathing Terms Hyperpnea Hypopnea Tachypnea Apnea Dyspnea Orthopnea Results of Inadequate Respiration Cyanosis Hypoxia Anoxia Hypoxemia Suffocation Aging & Respiratory Tract Respiratory tract tissues lose elasticity & become more rigid with age Chest wall rigidity, arthritis & loss of strength in breathing muscles - lead to decrease lung capacity & compliance Increased susceptibility to infection Emphysema from smoking & other irritants activity & exercise can decrease capacity Emphysema