* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Special Senses
Survey
Document related concepts
Transcript
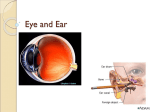
Special Senses Chapter 8 The Special Senses Touch Taste Smell Sight Hearing Equilibrium (Balance) Special Sense Receptors Receptors can be large complex sensory organs such as the eye and ear Or they can be localized clusters of receptors such as the taste buds and olfactory system The Eye and Vision Anatomy of the Eye 70% of your sensory receptors are in the eye. It is the sense that requires the most learning External and Accessory Structures: The eye is a sphere about 1 inch in diameter Only the anterior 1/6th of the eye is visible the rest is cushioned with fat and bony structures Eyelid: Anterior protection of the eyes which meet at the lateral and medial canthus (corner) of the eye Eyelashes: projections on the border of the eyelid Anatomy of the Eye External & Accessory Structures: Meibomian glands: modified sebaceous glands on the eyelid edges. They produce an oily secretion which lubricates the eye. Ciliary glands: modified sweat glands which lie between the eyelashes Conjunctiva: delicate membrane lining the eyelid and covering part of the outer surface of the eyeball. Secretes mucus which helps to lubricate the eye and keep it moist. Conjunctivitis: inflammation of the conjunctiva. Eyes become red, irritated and when infected becomes pinkeye – caused by a bacteria or virus and is highly contagious. Anatomy of the Eye Lacrimal Apparatus: Consists of lacrimal gland and ducts which drain the lacrimal sections of the nasal cavity. Lacrimal Glands: Located above the lateral end of each eye. They release a diluted salt solution (tears) onto the anterior surface of the eye through ducts Tears: contain antibodies, lysozomes, and enzymes which destroy bacteria. They cleanse and protect the eye surface as well as moisturize and lubricate it. Lacrimal canals: Tiny canals through which the tears drain into. When the lacrimal mucosa is inflamed due to infection they swell and do not allow proper drainage of the tears from the eye surface causing watery eyes. Anatomy of the Eye Lacrimal Apparatus: Lacrimal sac: another stop for the tears before they drain into the … Nasolacrimal duct: empties tears into the nasal cavity. When tears spill over the eyelids they fill the nasal cavity and cause congestion. This can occur because of irritation to the eyes or when we are emotionally upset. Anatomy of the Eye Extrinsic/External Eye Muscles: Attach to the outer surface of the eye The muscles provide gross movement of the eye and make it possible to follow moving objects. Anatomy of the Eye Internal Structures: The Eyeball Eyeball: Hollow sphere that’s wall contain tunics and its interior is filled with fluids called humors which maintain its shape. Tunics: Sclera: Outermost tunic Made up of thick, white, connective tissue It is sometimes referred to as the fibrous tunic and can be seen anteriorly as the white of the eye. Cornea: Central anterior portion of the sclera Is a transparent window through which light enters the eye It has many nerve endings which when it is touched blinking and increased tears begin It has a great ability to heal itself and is the only tissue inn the body that can be transplanted without worry of rejection. Anatomy of the Eye Internal Structures: The Eyeball Choroid: Middle tunic of the eye Is blood rich and contains a dark pigment which prevents light from scattering inside the eye Anteriorly it forms the ciliary body Cilialry Body: Anterior formation of the choroid Attaches to the lens and the iris Anatomy of the Eye Internal Structures: The Eyeball Lens: Main focusing apparatus of the eye Cataracts: As we age the lens becomes increasingly hard and opaque causing vision to become hazy and eventually causing blindness Special glasses or removal of the lens and putting a new one in are the most common treatments. Aqueous Humor: Is Anterior to the lens and contains a clear water-like fluid similar to blood plasma It is continually secreted by a special area of the choroids It helps with internal pressure of the eye and provides nutrients for the lens and cornea which have NO blood supply Anatomy of the Eye Interior Structures: The Eyeball Vitreous Humor: Canal of Schlemm: Gel-like fluid which is contained within the posterior segment. Helps prevent the eyeball from collapsing inward by reinforcing the internal aspect Reabsorbs the aqueous humor and is located between the sclera and cornea Glaucoma Result of blocked drainage of the aqueous humor which compresses the retinal and optic nerve Pain and possible blindness will occur Common in the elderly and tends to occur without any obvious signs Signs that develop are: halos around lights, headaches, and blurred vision Treated with eyedrops which increases the rate of drainage of aqueous humor Anatomy of the Eye Interior Structures: The Eyeball Iris: Pigment color of the eye which contains a rounded opening allowing light to enter Pupil: Rounded opening of the iris where the light enters. Made of smooth muscle fibers which regulate the amount of light entering the eye so that you can see clearly in the available light Close vision/Bright light = pupils contract Distant vision/dim light = pupils dilate Anatomy of the Eye Interior Structures: The Eyeball Retina: Inner most tunic of the eye Extends anteriorly to the ciliary body Contains receptor cells called rods and cones Rods & Cones: Photoreceptors which respond to light Electrical signals go to the photoreceptors then to the retina through the optic nerve and then are transmitted to the optic cortex to create what we see (VISION) Rods are most dense and on the periphery and decrease in number as you get closer to the center of the retina. They allow us to see gray tones in dim light and provide peripheral vision. Anatomy of the Eye Interior Structures: The Eyeball Rods & Cones con’t: Night Blindness: Result of damage or injury to the rods Can be caused by a prolonged deficiency of vitamin A which will eventually result in total deterioration of the retina Supplements can be taken to restore the damage before degenerative changes occur. Cones: Discriminatory receptors which allow us to see details in color under bright light They are found near the center of the retina and decrease in number as you get closer to the outer edge. Anatomy of the Eye Internal Structures: The Eyeball Optic Nerve: Contains ganglionic cells and is the point where senses leave the eye. Optic Disk/Blind Spot: When light from an object focuses on the optic disk then the object disappears from sight and we can no longer see it. Fovea Centralis: Lies lateral to the blind spot and is a tiny pit that contains only cones It is the area of greatest visual acuity (sharpest vision) and when we are viewing things critically this is the area we use. Anatomy of the Eye Three Types of Cones: Responds to Blue Light Responds to Green Light Responds to a range of light including green and red wavelengths of light. These are most commonly referred to as the cones because they are the only ones that can respond to a red light When all three cones are stimulated we see white. If you were to shine a red light into one eye and a green light into the other eye you will see yellow. This allows us to see things in multiple colors. Anatomy of the Eye Color Blindness: Lack of all three types of cones Lack of one type of cone will lead to partial color blindness Most common is the lack of red or green receptors which leads to two types of color blindness: Red and green are seen as the same color = you see only red or only green Color blindness is a sex linked condition and occurs in males because genes that regulate color are linked to the X chromosome. Ophthalmoscope: Instrument used to illuminate the interior of the eye and allows the retina, optic disk and internal blood vessels to be viewed and examined. Pathway of Light through the Eye and Light Refraction When light passes from one substance to another substance with a different density the rays are bent/refracted. Light enters the cornea, then through the aqueous humor, then through the lens and into the vitreous humor = a bend in the rays The lens can change the bend in the light by changing its shape so that incoming light can properly focus in the retina The more concave the lens is the more bend there will be in the light The less concave the lens is the less bend there is in the rays Pathway of Light through the Eye and Light Refraction Light from a distance greater than 20 ft away does not require as much bend in the rays meaning the lens can be flatter or less concave Light from a closer object scatters and the lens must bulge, causing it to become more concave, in order to make close vision possible. When the ciliary body contracts the lens becomes more convex (rounded) = Accommodation: the ability to focus on close objects Real Image The result of light bending activities of the lens from the retina The real image is reverse from left to right and upside down and smaller than the actual object Vision problems occur when the lens is too strong or too weak to make the adjustment to the real image. Pathway of Light through the Eye and Light Refraction Emmetropia: Lens which focuses images correctly on the retina Myopia: Nearsightedness Occurs when parallel rays from distant objects fail to reach the retina and are focused in front of it. The distant objects appear blurry and nearby objects are in focus because the lens accommodates Can result from an eye that is too long or a lens is too strong or a cornea that is too curved. Correction requires concave lenses Pathway of Light through the Eye and Light Refraction Hyperopia: Farsightedness Occurs when the parallel light rays from distant objects are focused behind the retina Results from an eye that is too short or a lazy lens People see distant objects clearly but cannot focus on objects that are nearby Correction requires a convex lens to converge the light rays before they enter the eye Astigmatism: Unequal curvatures in different parts of the cornea or lens. Blurry images occur because points of light are focused as lines on the retina Special cylindrical lenses or contacts are used to correct the problem Visual Fields and Visual Pathways to the Brain Axons which carry impulses from the retina are bundled together at the posterior aspect of the eye and arise from the back of the eye at the optic nerve. Optic Chiasma: Fibers from the medial side of each eye cross over to the opposite side. Optic Tracts: Fiber tracts that result from the optic chiasma. Each tract contains fibers from the lateral side of the eye on the same side and the medial side of the opposite eye. They synapse with neurons in the thalamus Visual Fields and Visual Pathways to the Brain Optic Radiation: Synapse of neurons in the thalamus and axons. Controls the occipital lobe of the brain They then synapse with cortical cells and visual interpretation (vision) occurs. Binocular vision: Two Eye vision which provides for depth perception and requires input from both eyes. Visual Fields and Visual Pathways to the Brain Hemianopia: Loss of the same side of the visual field of both eyes. Result of damage to the visual cortex on one side only. The person is unable to see things past the middle of his/her visual field on either the right or left side. Eye Reflexes Both internal and external eye muscles are necessary for proper function of the eye Internal muscles are controlled by the autonomic nervous system External muscles control eye movement and make it possible to follow a moving object. Convergence: Reflexive movement of the eye medially when we view close objects. Uses the extrinsic eye muscles Eye Reflexes Photopupillary reflex: When eyes are exposed to bright light the pupils will immediately constrict This is a protective reflex that prevents excessively bright light from damaging the delicate photoreceptors within the eye. Accommodation papillary reflex: Pupil constriction when viewing close objects. Provides more acute vision Reading requires the use of both reflexes. The EAR Hearing and Balance Hearing Fluid must be “stirred” to stimulate the receptors located within the ear. The sound vibrations move the fluid to stimulate the receptors Gross movement of the head disturbs the fluids surrounding the balance organs Mechanoreceptors then respond to these physical forces allowing us to hear while moving. Anatomy of the Ear Outer/External Ear: Composed of the pinna and external auditory canal and is responsible for hearing only. Pinna: Also called the auricle Is the “ear” the structure that surrounds the auditory canal opening. External Auditory canal: Short narrow chamber carved into the temporal bone of the skull Anatomy of the Ear Outer/External Ear: Ceruminous glands: Skin lined walls of the external auditory canal which secretes a waxy, yellow substance Cerumen: Earwax Substance secreted by the ceruminous glands Tympanic membrane/Eardrum: Eardrum Soundwaves enter and cause it to vibrate The eardrum separates the outer ear from the middle ear. Anatomy of the Ear Middle Ear: Tympanic Cavity: Small air filled cavity within the temporal bone It is surrounded by the eardrum laterally and the bony wall medially which has two openings. Oval Window: one of the openings Round Window: the other opening which is inferior and covered by a membrane. Anatomy of the Ear Middle Ear: Auditory Tube: Runs obliquely downward to link the middle ear cavity with the throat and mucosa lining the two are continuous Normally it is flattened and closed but swallowing or yawning can open it briefly to equalize pressure in the middle ear The eardrum does not vibrate freely unless pressure is equal on both sides If pressure is unequal the eardrum bulges and causes hearing difficulty Otitis Media: Inflammation of the middle ear. Common result of a sore throat – the eardrum bulges and becomes inflamed. Anatomy of the Ear Middle Ear: Myringotomy: Cutting of the eardrum to release pressure and inserting a tube into it to allow pus formed in the middle ear to drain into the outer ear. Ossicles: Three of the smallest bones in the body which are part of the tympanic cavity. They transmit vibrations of the eardrum to the fluids of the inner ear. Anatomy of the Ear Ossicles con’t: Hammer/Malleus: Named for its hammer like appearance When eardrum vibrates the hammer moves the vibration to the anvil. Anvil/Incus: Moves the vibration into the stirrup Stirrup/Stapes: Passes the vibration to the oval window of the inner ear. The movement of the window sets the fluid of thinner ear in motion. Anatomy of the Ear Inner Ear: Only part of the ear responsible for hearing and balance. Osseus/Labrynth: Maze of bony chambers in the ear Located deep within the temporal bone and just behind the eye socket. Cochlea: Subdivision of the bony labyrinth Vestibular: Located between the cochlea and the semicircular canal Semicircular canal: Canals within the bony labyrinth Anatomy of the Ear Inner Ear: Perilymph: Membranous Labyrinth: Plasma like fluid in the bony labyrinth System of membrane sacs within the perilymph which follow the shape of the bony labyrinth Endolymph: Thick fluid contained within the membranous labyrinth. Mechanism of Hearing Organ of Corti: Contained within the cochlea The organ of corti contains tiny hearing receptors called hair cells. Basilar Membrane: Contains receptor cells which are stimulated when the hair cells are bent or tweaked by the movement of the … Tectorial Membrane: Gel like fluid which lies over the hair cells. Mechanism of Hearing Cochlear Nerve: Division of the vestibulocochlear nerve where interpretation of sound occurs. Since sounds reach each ear at different times we hear in “stereo” and are able to determine where sound is coming from Hearing is the last sense to leave our awareness and the first to return. Mechanism of Equilibrium Equilibrium is a mechanism of response which often we do not even realize its occurring. Vestibular apparatus: The equilibrium receptors of the inner ear. They are divided into two arms: Static Equilibrium Dynamic Equilibrium Mechanism of Equilibrium Static Equilibrium: Maculae: Receptors within the membrane sacs of the vestibulae They report on the position of the head with the pull of gravity when the head is not moving They help us to stand up straight. Otolithic Membrane: Patch of receptor hair cells with hairs embedded into it. Mechanism of Equilibrium Static Equilibrium con’t: Otoliths: Tiny stones made up of calcium salts and when our head moves they roll in response to the changes in gravity This creates a pull on the gell which slides over the hair cells causing them to bend Once the hair cells are activated by this impulses are sent along the vestibular nerve. Vestibular Nerve: Informs the brain of the position of the head in space. Mechanism of Equilibrium Dynamic Equilibrium: Receptors are found in the semicircular canals and respond to angulatory or rotary movements of the head. These receptors work in all three planes so that any way we move they will detect it. Crista Ampularis: receptor region consisting of tufts of hair cells covered with a gelatin like cap called the … Capula: When your head moves in an angular direction the endolymph in the canal moves in the opposite direction pushing the capula into a direction that is opposite of your body movement. This stimulates the hair cells and transmits impulses up the vestibular nerve. Mechanism of Equilibrium Dynamic Equilibrium con’t: Vestibular Nerve: transmits impulses to the cerebellum. When angular motion stops the flow is in the opposite direction reversing the capula’s movement and causes the reversed motion you feel when stopping suddenly. The static and dynamic equilibrium work together along with sight and sound to keep us balanced. Hearing & Equilibrium Deficits Deafness: Hearing loss of any degree – from slight to total Conduction Deafness: Results when something interferes with the conduction of sound vibrations to the fluids of the inner ear. Buildup of earwax can be the cause of the fusion of the ossicles A ruptured eardrum or otitis media may also contribute. The person will be able to hear by bone conduction In most cases this can be fixed by the use of a hearing aid. Hearing & Equilibrium Deficits Sensorineural Deafness: Occurs when there is degeneration or damage to the receptor cells in the organ of corti, the cochlear nerve or neurons of the auditory cortex These people cannot hear by any conduction route. Meniere’s Syndrome: Cause is not fully known Suspected causes are arteriosclerosis, degeneration of the cranial nerve 8 and increased pressure of the inner ear fluids. Progressive deafness occurs and individuals experience nausea or vertigo which is so bad that they are unable to stand up without extreme discomfort. Anti-motion sickness medications may help with this discomfort.