* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download CHEST PAIN Introduction
Survey
Document related concepts
Heart failure wikipedia , lookup
Saturated fat and cardiovascular disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Echocardiography wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Coronary artery disease wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
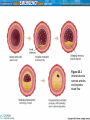
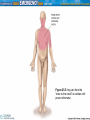
CHEST PAIN Introduction • Chest pain (angina) may not be heart attack but other cardiac event • Cardiac events have potential to progress to cardiac arrest • EMT must treat cardiovascular events as emergencies • Accurate assessment and quick management are keys to survival Anatomy and Physiology Review • The left heart – Left ventricle pumps blood around systemic circuit – Function of left ventricle estimated by blood pressure – Left ventricle not pumping adequately: low systolic blood pressure Anatomy and Physiology Review (cont’d.) • The right heart – Right ventricle pumps blood to lungs – Resistance is relatively low – Requires less work than left ventricle Anatomy and Physiology Review (cont’d.) • Coronary circulation – Coronary arteries: supplies heart with oxygenated blood – Two main arteries branch off into several smaller vessels Coronary Artery Disease • Pathophysiology of heart disease – Atherosclerosis: process of fat buildup in blood vessels – Plaques or atheromas: deposits of fat – Thrombus: blood clot – Unstable angina: chest pains with little exertion – Acute myocardial infarction (AMI): myocardial cell death Figure 25.3 Atherosclerosis narrows arteries and impedes blood flow Coronary Artery Disease (cont’d.) • Risk factors – Modifiable • Smoking, obesity, cocaine, lack of exercise, diet, high cholesterol – Non-modifiable • Sex, diabetes, age, hypertension, heredity Signs and Symptoms • • • • • Tachycardia: heart beats too fast Bradycardia: heart beats too slow Weakness and nausea Diaphoretic Chest pain Figure 25.5 Any pain from the “nose to the navel” is cardiac until proven otherwise Signs and Symptoms (cont’d.) • Noncardiac chest pain (see Table 25-3): – Esophageal spasm – Pleurisy – Pneumonia – Pneumothorax – Rib fractures – Gastric ulcer disease Assessment • Rule of thumb: – “Any pain from nose to navel is cardiac until proven otherwise” • Primary assessment – Unresponsive cardiac patient • Begin CPR immediately – Responsive cardiac patient • History and focused physical examination Assessment (cont’d.) • History – Onset – Provocation – Quality – Radiation – Severity – Time/duration Assessment (cont’d.) • Preexisting medical conditions – Ask about risk factors – Hypertension • Take blood pressure in both arms • Difference of more than 20 mmhg may indicate active dissection • Hypotension may be sign of several disorders Assessment (cont’d.) • Baseline vital signs – Helps determine speed at which condition is changing • Secondary assessment – Focused physical examination – Body’s effort to compensate Assessment (cont’d.) • Management – Place patient in position of comfort – Loosen constricting clothing – Aspirin – Nitroglycerin Assessment (cont’d.) • Reassessment – Repeat vital signs as needed – Review history – Be alert to possibility of sudden cardiac death and need to do CPR Transport • Never allow patient to walk to ambulance or stretcher • Carry patient if necessary • Ensure patient is comfortably seated • Continuously monitor patient • Avoid use of sirens and flashing lights Transport (cont’d.) • Aeromedical transportation – For remote areas lacking specialized heart centers – Avoids traffic in urban areas • ALS intercept – Traditional emergency department functions in field Fibrinolytics • Class of drugs used to treat AMI • “Fibrinolytic”: to divide the fibrin • Opens blocked arteries and reestablishes blood flow • Most effective within first few hours • EMT must quickly transport patient for rapid treatment Interventional Cardiology • Mechanically remove blockage • Angioplasty • Interventional cardiology techniques are best first option • Bottom line: blocked vessel must be opened as quickly as possible Conclusion • Chest pain is one of most common reasons EMS is called • Ever-present possibility of sudden cardiac death creates challenge • Skills and knowledge put to ultimate test • Thoughtful consideration and deliberate action will improve chance for survival