* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download 11Brucella,Francisella,Bordetella2012
Survey
Document related concepts
Neglected tropical diseases wikipedia , lookup
Lyme disease microbiology wikipedia , lookup
Neonatal infection wikipedia , lookup
Transmission (medicine) wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Onchocerciasis wikipedia , lookup
Chagas disease wikipedia , lookup
Hepatitis B wikipedia , lookup
Marburg virus disease wikipedia , lookup
Infection control wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
Germ theory of disease wikipedia , lookup
Schistosomiasis wikipedia , lookup
Globalization and disease wikipedia , lookup
Transcript
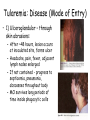
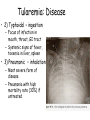
Brucella, Francisella, Bordetella, Fastidious Gram-Negative Rods Genera of Uncertain Affliation • Gram(-), small, coccobacilli • Strict aerobe, nonfermenter • Most nonmotile • Fastidious, enriched media for culture • Slow culture growth, prolong incubation • Brucella - brucellosis • Francisella - tularemia • Bordetella – pertussis, important pediatric disease Brucella: Zoonotic Pathogen • Worldwide - >500,000 cases/year • USA - <100 cases/year, control disease in animals • Usually mild, AS disease in natural animal host • Infect animal tissue rich in erythritol; localize infection of breast, uterus, placenta, fetus, epididymus • Intracellular parasite of macrophage • Cause of sterility, abortion, AS carriage of infected animals Brucella: Genera • Four species infect humans – wide disease spectrum: – B. melitensis (goats, sheep) - most common cause of brucellosis, causes severe disease – B. suis (swine) – destructive lesions, prolonged disease – B. abortus (cattle) – mild disease – B. canis (dog) – mild disease • DNA studies show one species – B. melitensis, others are biovars Brucella: Lab Culture • Brucella Blood agar - fastidious, requires enriched media, CBA containing meat infusion or tryptone • Growth on CBA or chocolate agar, slow and may take 72 hours • Colonies start as tiny pinpoint, translucent colonies, become gray with age • Most clinical isolates obtained from blood culture Brucella: Lab ID • Collect patient blood specimen, inoculate directly into blood culture bottle • Serum serology for Brucella antibodies to test for infection • Extreme care required for safe handling of specimen and culture in lab • Biosafety Level-3 pathogen - transmitted by respiratory route, produce serious disease; handle in biological safety cabinet Brucella melitensis: Brucellosis (Undulant Fever) • “Malta (Island of Melita) Fever” • In humans, ingestion of unpasteurized milk or cheese from goats, cows; also acquire MO via direct contact with infected animals, inhalation • At risk are veterinarians, slaughterhouse workers, farmers, lab microbiologists • CDC category B Select Biological Agent – Easy to disseminate – Moderate morbidity, low mortality Brucellosis (Undulant Fever) • Localized abcesses at site on inoculation; bacteremia, MO phagocytized; localized in RES tissues (spleen, liver, bone marrow, lymph nodes, kidneys) • Infection ranges from: – Asymptomatic, subclinical – Subacute - malaise, chills, sweats, fatigue, myalgia, weight loss, nonproductive cough – Acute infection – fever, chills, endotoxic disease • Fever in all patients and intermittant: – Typically spikes each evening – Coincides with release of MO from phagocytes – “Undulant” fever Brucella: Treatment and Prevention • Chemotherapy difficult, intracellular survival of MO in macrophages • Combination doxycycline + rifampin • Tetracycline toxic for pregnant moms and young kids (<8 yr.) - SXT drug of choice • Control by ID (serology) infected animals: – Eliminate infected herds – Animal vaccine to prevent infection • Pasteurization of dairy products kills MO • Biohazard safety precautions in the lab Francisella tularensis: Zoonotic Pathogen • Tulare county – infected rodent transmit to humans by tick bite • Tularemia – glandular fever, rabbit fever, tick fever, deerfly fever • Worldwide; USA - low incidence ~100 cases/year • Intracellular parasite – survive prolonged periods in macrophage of RES (lymph nodes, bone marrow, spleen, liver, kidneys) F. tularensis: Lab Culture • Fastidious, require enriched media • Chocolate, MTM + antimicrobials • BCYE (buffered charcoal-yeast extract) – selective media for Legionella • Colonies may grow in 24 hours, or 5-7 days • Specimen – ulcer scrape, lymph node biopsy, sputum • Collection and processing specimen extremely hazardous: – MO highly contagious (<100 MO) – Penetrate skin and mucous membranes – Inhale aerosols F. tularensis: Lab ID • Best done by serology: – No previous infection - antibody titer ≥1:160 – Patient with previous antibody - 4x increase in paired serum (acute, convalescent) • Culture done under biological safety cabinet (Biosafety Level-3 pathogen) • Laboratory infection common Tularemia: Transmission • MO in wild animals, domestic animals, birds, fish, ticks, water • Acquired by: – Direct contact infected animals – Ingestion contaminated meat or water – Inhalation • Infectious dose low ~10 • A disease mostly in rabbits, rodents • Most often transmitted to human by ticks or deer flies fed on infected rodents, or pet catching infected rabbit Tularemia: Disease (Mode of Entry) • 1) Ulceroglandular – through skin abrasions: – After ~48 hours, lesion occurs at inoculated site, forms ulcer – Headache, pain, fever, adjacent lymph nodes enlarged – If not contained - progress to septicemia, pneumonia, abscesses throughout body – MO survives long periods of time inside phagocytic cells Tularemia: Disease • 2) Typhoidal – ingestion – Focus of infection in mouth, throat, GI tract – Systemic signs of fever, toxemia in liver, spleen • 3) Pneumonic – inhalation – Most severe form of disease – Pneumonia with high mortality rate (30%) if untreated F. tularensis: Bioterrorism Agent • CDC category A Select Biological Agent • Risk to national security • Spread person-to-person, or easily disseminated • Result in high mortality • Lead to great public health impact and public panic F. tularensis: Treatment and Prevention • Streptomycin drug of choice, however not readily available, high toxcity • Gentamycin good alternative • Attenuated, live vaccine protects against inhalation form of disease; for at risk (farmer, hunter, veterinarian, lab microbiologist) • Avoid reservoirs and vectors of infection • Wear protective clothing, use insect repellant (DEET) to reduce risk of tick, fly bite Case Study 5 - Francisella • A 27-year-old man was mowing his field when he ran over two young rabbits. • When he stopped his mower, he realized that two other rabbits were dead in the unmowed part of the lawn. • He removed all the rabbits and buried them. • Three days later he developed a fever, muscle aches, and a dry, nonproductive cough. • Over the next 12 hours he got progressively sicker and was transported by his wife to the area hospital. Case Study 5 - Francisella • Results of a chest x-ray showed infiltrates in both lung fields. • Blood cultures and respiratory secretions were collected, and antibiotics were initiated. • Blood cultures became positive with small gram-negative rods after 3 days of incubation, and the same organism grew from the respiratory specimen that was incubated onto BCYE agar. Case Study - Questions • 1. What test should be performed to confirm the tentative diagnosis of Francisella tularensis? • 2. This infection was presumably acquired by inhalation of aerosolized contaminated blood. What are the most common sources of F. tularensis infections and the most common routes of exposure? • 3. What are the different clinical manifestations of F. tularensis? Bordetella: Pertussis • Endemic disease worldwide - >60 million cases annually, >200,000 deaths • Incidence reduced with Diphtheria, Pertussis, Tetanus vaccine (DPT) • Pertussis in USA: – Inadequately immunized children (5 doses) – Child not vaccinated due to parental fear of vaccine-related neurologic toxcity – Increase infections in adolescents and adults (reservoir) due to waning immunity, no booster vaccination – Recent resurgence and outbreaks estimated ~3 million Bordetella: Genera • Three medically important species: – B. pertussis – “severe cough”, pertussis (whooping cough) in humans – B. parapertussis – “resembling”, milder pertussis in humans – B. bronchoseptica – “trachea, septic”, respiratory disease in animals; occasional respiratory or wound infection in humans Bordetella pertussis: Lab Culture • No growth on common lab media: – Additional nutrients needed – Use of adsorbents to remove media substances (fatty acids, sulfides) toxic to B. pertussis • Bordet-Gengou media – glycerol, potato infusion, albumin (binds fatty acids), up to 50% sheep RBCs • Charcoal agar supplemented with 10% horse blood, with or without cephalexin • Usually 3-7 days for growth, 370 C B. pertussis: Virulence Factors Toxins • Pertussis toxin (PT): – Increase in cAMP; increase respiratory secrections, mucus leads to coughing stage of disease • Adenylate cyclase/hemolysin toxin: – Increase in cAMP; inhibits phagocytes – Protect MO during infection, early stages of disease • Tracheal cytotoxin: – Due to bacterial peptidoglycan – Killing, sloughing of ciliated cells – Interferes with cell DNA synthesis, repair, regeneration – Disrupts normal clearance in RT – Damage leads to “whooping” cough B. pertussis: Virulence Factors (Cell Surface) • Filamentous hemagglutinin (FHA) – attaches to host cell cilia, antibody made against it protective (used for acellular vaccine) • Pertactin – adhesion, antibody made against it protective (used for acellular vaccine) • Lipooligosaccharide - surface of the bacteria, potent endotoxin activity B. pertussis: Whooping Cough • Infection by inhalation of infected droplets or direct contact with secretions • Highly infectious, 2º attack rate = 80% • MO attaches to RT ciliated cells • Incubation 1-2 weeks, MO multiplies liberates toxins Whooping Cough: Three Stages • 1) Catarrhal stage: – Resembles cold, mild cough and sneezing – Large number MO spread through respiratory secretions – Last ~2 weeks • 2) Paroxysmal stage: – Rapid, consecutive coughs, rapid intake of air (whooping sound) – 40-50 daily paroxysms; vomiting, exhaustion – Last 3-4 weeks • 3) Convalescent stage: – Symptoms gradually subside – Last 3-4 weeks – Complete recovery may need months Whooping Cough • B. pertussis rarely spreads to other sites, but lot of cell damage may occur: – Local tissue of RT – Systemic damage by spread of exotoxin • Secondary complications may occur – Pneumonia – Otitis media – CNS dysfunction - seizures, encephalopathy occurs ~10% cases; unknown cause B. pertussis: Treatment and Prevention • Primarily supportive care • Convalescence correlated with regeneration of ciliated epithelium • Erythromycin: – Effective early stage of disease before toxins – Reduces infectivity of patient • DTaP vaccine – subunit acellular pertussis: – PT toxoid, FHA hemagglutinnin, Pertactin – Lower incidence of side-effects – Children: five doses – 2, 4, 6, 18 months; booster at 4-6 years – Adolescents, adults: boosters – 12 years; 19-65 years Class Assignment • Textbook Reading: • Chapter 18 Haemophilus and Other Fastdious Gram-Negative Rods - Brucella, Francisella • Chapter 40 Zoonotic Diseases – Tularemia, Brucellosis (pgs. 941-943) • Chapter 32 Upper and Lower RTI – Pertussis (pgs. 782-783) • Key Terms • Learning Assessment Questions Case Study 6 - Bacillus • A 56-year-old female postal worker sought medical care for fever, diarrhea, and vomiting. • She was offered symptomatic treatment and discharged from the community hospital emergency department. • Five days later she returned to the hospital with complaints of chills, dry cough, and pleuritic chest pain. • A chest radiograph showed a small right infiltrate and bilateral effusions but no evidence of a widened mediastinum. Case Study 6 - Bacillus • She was admitted to the hospital, and the next day her respiratory status and pleural effusions worsened. • A computerized tomographic (CT) scan of her chest revealed enlarged mediastinial and cervical lymph nodes. • Pleural fluid and blood was collected for culture and was positive within 10 hours for gram-positive rods in long chains. Case Study - Questions • 1. The clinical impression is that this woman has inhalation anthrax. What tests should be performed to confirm the identification of the isolate? • 2. What are the three primary virulence factors found in B. anthracis? • 3. Describe the mechanisms of action of the toxins produced by B. anthracis. • 4. Describe the two forms of B. cereus food poisoning. What toxin is responsible for each form? Why is the clinical presentation of these two diseases different?