* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Myocardial Infarction
Survey
Document related concepts
Heart failure wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Electrocardiography wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Cardiac surgery wikipedia , lookup
Drug-eluting stent wikipedia , lookup
Jatene procedure wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
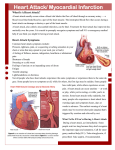
Myocardial Infarction
• Myocardial Infarction
Myocardial Infarction
blood vessels that supply blood to the heart are
blocked, preventing enough oxygen from getting
to the heart.
Insufficient blood supply to the myocardium can
result in
myocardial ischemia,
myocardial injury or
myocardial infarction, or
all three.
Myocardial Infarction
Myocardial ischemia
generally appears first in the subendocardial region and is more
extensive
farthest from the blood supply
greater intramural tension and
More need for oxygen.
Myocardial Infarction
Subendocardial ischemia:
repolarization normally from
Epicardium-to-Endocardium.
delayed recovery in the Subendocardial
region due to ischemia merely
lengthens repolarization.
results in prolonged QT interval or
increased amplitude of T wave or both
Myocardial Infarction
Subepicardial or transmural ischemia
ischemia extends subepicardially.
more visible effect on recovery of subepicardial
cells.
Recovery is more delayed
the subendocardial muscle fibers seem to recover
first.
Repolarization is endocardial-to-epicardial,
resulting in inversion of the T waves in leads
overlying the ischemic regions.
Myocardial Infarction
Injury
to the myocardial cells results when the ischemic
process is more severe.
Subendocardial injury - ST segment depression,
subepicardial or transmural injury - ST segment
elevation.
ischemia, injury and myocardial infarction
frequently coexist
producing mixed and complex ECG patterns.
Myocardial Infarction
Myocardial infarction
necrosis or death of myocardial cells.
The left ventricle - predominant site
right ventricular infarction occasionally coexists.
pathological Q waves in transmural myocardial infarction
initial downward deflection of 40 msec or more in any
lead except III and aVR.
infracted muscle is electrically inert
vector directed away from the site of infarction
seen as a negative Q wave
Myocardial Infarction
Transmural Infarction - Rupture
Myocardial Infarction
During acute myocardial infarction various stages of
myocardial damage can coexist
the central area of necrosis
surrounded by an area of injury
surrounded by an area of ischemia.
Transient myocardial ischemia produces T wave,
and sometimes ST segment abnormalities
can be reversible without producing permanent
damage
not accompanied by serum enzyme elevation.
Causes
blood clot that blocks one of the coronary
arteries.
atherosclerosis
• The slow buildup of plaque, almost block one of
your coronary arteries, more likely during exercise
• The plaque itself develops cracks, platelets form a
blood clot, that can completely blocks the passage
of oxygen-rich blood to the heart.
• sudden, significant emotional or physical stress,
including an illness, can trigger a heart attack.
Atherosclerosis
Atherosclerosis –Hardening of Artery
Atherosclerosis
Infarction
Atherosclerosis
Infarction
Infarction
Risk factors
•
•
•
•
•
•
•
•
•
•
for heart attack and coronary artery disease include:
Increasing age (over age 65)
Male gender
Diabetes
Family history of coronary artery disease - genetic
High blood pressure
Smoking
Too much fat in your diet
high LDL ("bad") cholesterol and low HDL ("good")
Chronic kidney disease
Risk factors
Risk factors
Symptoms
• Chest pain major symptom, may move from your chest
to your arms, shoulder, neck, teeth, jaw, belly area, or
back.
• severe or mild. It can feel like:
• A tight band around the chest
• Bad indigestion
• Something heavy sitting on your chest
• Squeezing or heavy pressure
• usually lasts longer than 20 minutes.
• Rest and a medicine called nitroglycerin may not
completely relieve the pain.
• Symptoms may also go away and come back.
sudden cardiac arrest
•
•
•
•
•
•
•
•
•
•
Symptoms
Other symptoms of a heart attack include:
Anxiety
Cough
Fainting
Light-headedness, dizziness
Nausea or vomiting
Palpitations
Shortness of breath
Sweating - extreme
"silent heart attack" is a heart attack with no symptoms elderly, people with diabetes, and women, no chest pain
but unusual symptoms
unusual symptoms
Exams and Tests
•
•
•
•
A heart attack is a medical emergency.
seek immediate medical help.
DO NOT try to drive yourself to the hospital.
DO NOT DELAY - greatest risk of sudden cardiac
death in the early hours of a heart attack.
• You may have a rapid pulse.
• Your blood pressure may be normal, high, or low.
Exams and Tests
Tests to look at your heart include:
• Coronary angiography
• CT scan
• Echocardiography
• Electrocardiogram (ECG) -- once or repeated
• MRI
• Nuclear ventriculography
• Blood tests - show if heart tissue damage
• Troponin I and troponin T
• CPK and CPK-MB
• Serum myoglobin
Tests EKG
TESTs
Echocardiography
CT Scan
Angiography
Treatment
• need to stay in ICU.
• arrhythmias - leading cause of death in the first
few hours -medications or electrical cardioverson
/defibrillation.
• oxygen
• An intravenous line, urinary catheter
Treatment
ANGIOPLASTY AND STENT PLACEMENT
called percutaneous coronary intervention
(PCI)
preferred emergency procedure, within 90
minutes but not later than 12 hours after MI
open narrowed or blocked blood vessels.
A stent is often placed after angioplasty.
prevent the artery from closing up again.
Treatment
THROMBOLYTIC THERAPY (CLOT-BUSTING DRUGS)
• drugs to break up the clot.
• Best if given within 3 hours of first felt chest pain.
Contraindications :
• intracranial hemorrhage
• Brain tumors or blood vessel malformations
• Stroke within past 3 months
• Head injury within past 3 months
• Pregnant women
• Severe high blood pressure
Angioplasty
Treatment
• OTHER MEDICINES FOR HEART ATTACKS
• Nitroglycerin helps reduce chest pain.
• Antiplatelet medicines help prevent clots. Aspirin,
clopidogrel (Plavix), daily for at least one year
• Beta-blockers - atenolol help reduce the strain on
the heart and lower blood pressure.
• ACE inhibitors - enalapril, or captopril, to prevent
heart failure and lower blood pressure.
• Lipid-lowering medications, statins, lovastatin,
Treatment
• CORONARY ARTERY BYPASS SURGERY
• narrowing of the left main coronary artery emergency CABG).
CABG
Management
Healthy Diet
Regular Exercise
Possible Complications
•
•
•
•
•
•
•
•
•
Cardiogenic shock
Congestive heart failure
infarct extension - rupture of the heart
Damage to heart valves or the wall
pericarditis)
ventricular tachycardia and ventricular fibrillation
pulmonary embolism
Stroke - Blood clot to the brain
Side effects of drug treatment
Stroke - CVA
Prevention
• BP, blood sugar, and cholesterol under control.
• Don't smoke.
• 1 glass of alcohol each day. larger amounts does more
harm than good.
• low-fat diet rich in fruits, vegetables and low in animal
fat. fish twice a week.
• Exercise daily or several times a week.
• Lose weight if you are overweight.
• one or more risk factors Aspirin therapy
• regular follow-up cardiac rehabilitation program
• Always follow the exercise, diet, and medication plan
Myocardial Infarction
Two types of myocardial infarction on EKG:
1. Q wave infarction - presence of pathological Q
waves, also called transmural infarction.
2. Non-Q wave infarction - presence of ST
depression and T wave abnormalities.
• Elevation of serum enzymes is expected in both
types of infarction.
• In the absence of enzyme elevation, ST and T
wave abnormalities - due to injury or ischemia
rather than infarction.
Site of infarction
Fairly accurately from analysis of the 12-lead ECG.
• Inferior (or diaphragmatic) wall: II, II and aVF
• Septal: V1 and V2
• Anteroseptal: V1, V2, Vf3 and sometimes V4
• Anterior: V3, V4 and sometimes V2
• Apical: V3, V4 or both
• Lateral: I, aVL, V5 and V-6
• Extensive anterior: I, aVL and V1 through V6
Posterior wall infarction - tall R waves in V1 and
V2.
Site of infarction
The classic changes seen during acute infarction.
necrosis (Q waves)
injury (ST elevation), and
ischemia (T wave inversion)
In recovery
the ST segment that normalizes earliest,
then the T wave;
the Q wave usually persists.
the age of the infarction, roughly estimated from
appearance of ST segment and T wave.
Q wave in the absence of ST and T wave generally
indicates prior or healed infarction.
ST segment elevation and T wave
abnormalities
Other causes of ST segment elevation
• Acute pericarditis: ST elevation is generally diffuse
and not accompanied by reciprocal depression of
the ST segment in other leads.
• Early repolarization: particularly young patients
without known disease.
• Ventricular aneurysm: persistent aneurysm in the
region of infarction, ST segment elevation may
persist indefinitely.
Abnormal T waves
conditions other than myocardial ischemia:
•
•
•
•
•
•
•
•
•
•
Hyperventilation
Cerebrovascular disease
Mitral valve prolapse
Right or left ventricular hypertrophy
right or left bundle branch block
Ventricular preexcitation
Myocarditis
Electrolyte imbalance
drugs - digitalis and antiarrhythmic agents
No obvious cause, particularly in women
Myocardial infarction
• the death of a portion of heart muscle in an area
where there is sudden loss of blood supply.
• Death of the heart muscle often causes chest pain
• electrical instability of the heart muscle tissue
• rapid and disorganized heartbeat - ventricular
fibrillation.
• cannot pump/deliver oxygenated blood to brain.
• Permanent brain damage and death can occur
unless oxygenated blood flow is quickly resumed
Myocardial infarction
• usually by complete blockage of coronary artery
by blood clot.
• advanced coronary artery disease, having fatty
deposits, is damaged.
• blood clot on the damaged surface
• Chest pain or pressure is a common symptom.
• Cardiac chest pain is often vague, dull, pressure or
constricting band-like sensation, squeezing,
heaviness, or discomfort.
Consequences
A heart attack is potentially very serious, can lead to
full recovery
chronic disabling condition
permanent brain damage, rapidly fatal and
Death, unless blood flow is quickly resumed.
Invasive Procedures
• Coronary (balloon) angioplasty: A thin catheter is
inserted into the blocked artery with a tiny balloon on
the end. it is expanded to keep the artery open and the
catheter is removed.
• Stents: The insertion of a stent is similar to coronary
angioplasty except that over the balloon is a small
metallic tube (a stent) that stays in place to keep the
artery open while the catheter and the balloon are
removed.
• Atherectomy: laser cuts away the plaque
• Brachytherapy: Radiation to the blockages to remove
them from recurring after angioplasty.
Coronary Blood Flow