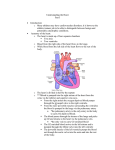
* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Left ventricle
Cardiac contractility modulation wikipedia , lookup
Heart failure wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Aortic stenosis wikipedia , lookup
Electrocardiography wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Coronary artery disease wikipedia , lookup
Artificial heart valve wikipedia , lookup
Myocardial infarction wikipedia , lookup
Cardiac surgery wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Atrial septal defect wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
PowerPoint® Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College CHAPTER 18 The Cardiovascular System: The Heart: Part A © Annie Leibovitz/Contact Press Images © 2013 Pearson Education, Inc. The Pulmonary and Systemic Circuits • Heart is transport system; two side-by-side pumps – Right side receives oxygen-poor blood from tissues • Pumps to lungs to get rid of CO2, pick up O2, via pulmonary circuit – Left side receives oxygenated blood from lungs • Pumps to body tissues via systemic circuit © 2013 Pearson Education, Inc. The Pulmonary and Systemic Circuits • Receiving chambers of heart: – Right atrium • Receives blood returning from systemic circuit – Left atrium • Receives blood returning from pulmonary circuit © 2013 Pearson Education, Inc. The Pulmonary and Systemic Circuits • Pumping chambers of heart: – Right ventricle • Pumps blood through pulmonary circuit – Left ventricle • Pumps blood through systemic circuit © 2013 Pearson Education, Inc. Figure 18.1 The systemic and pulmonary circuits. Capillary beds of lungs where gas exchange occurs Pulmonary Circuit Pulmonary arteries Aorta and branches Venae cavae Right atrium Right ventricle Oxygen-rich, CO2-poor blood Oxygen-poor, CO2-rich blood © 2013 Pearson Education, Inc. Pulmonary veins Left atrium Heart Left ventricle Systemic Circuit Capillary beds of all body tissues where gas exchange occurs Heart Anatomy • Approximately size of fist • Location: – In mediastinum between second rib and fifth intercostal space – On superior surface of diaphragm – Two-thirds of heart to left of midsternal line – Anterior to vertebral column, posterior to sternum © 2013 Pearson Education, Inc. Heart Anatomy • Base (posterior surface) leans toward right shoulder • Apex points toward left hip • Apical impulse palpated between fifth and sixth ribs, just below left nipple © 2013 Pearson Education, Inc. Figure 18.2a Location of the heart in the mediastinum. Midsternal line 2nd rib Sternum Diaphragm © 2013 Pearson Education, Inc. Location of apical impulse Figure 18.2b Location of the heart in the mediastinum. Mediastinum Heart Left lung Body of T7 vertebra Posterior © 2013 Pearson Education, Inc. Figure 18.2c Location of the heart in the mediastinum. Superior vena cava Pulmonary trunk Aorta Parietal pleura (cut) Left lung Pericardium (cut) Apex of heart Diaphragm © 2013 Pearson Education, Inc. Coverings of the Heart: Pericardium • Double-walled sac • Superficial fibrous pericardium – Protects, anchors to surrounding structures, and prevents overfilling © 2013 Pearson Education, Inc. Pericardium • Deep two-layered serous pericardium – Parietal layer lines internal surface of fibrous pericardium – Visceral layer (epicardium) on external surface of heart – Two layers separated by fluid-filled pericardial cavity (decreases friction) © 2013 Pearson Education, Inc. Figure 18.3 The pericardial layers and layers of the heart wall. Pulmonary trunk Fibrous pericardium Pericardium Parietal layer of serous pericardium Myocardium Pericardial cavity Epicardium (visceral layer of serous pericardium) Myocardium Endocardium Heart chamber © 2013 Pearson Education, Inc. Heart wall Homeostatic Imbalance • Pericarditis – Inflammation of pericardium – Roughens membrane surfaces pericardial friction rub (creaking sound) heard with stethoscope – Cardiac tamponade • Excess fluid sometimes compresses heart limited pumping ability © 2013 Pearson Education, Inc. Layers of the Heart Wall • Three layers of heart wall: – Epicardium – Myocardium – Endocardium • Epicardium – Visceral layer of serous pericardium © 2013 Pearson Education, Inc. Layers of the Heart Wall • Myocardium – Spiral bundles of contractile cardiac muscle cells – Cardiac skeleton: crisscrossing, interlacing layer of connective tissue • Anchors cardiac muscle fibers • Supports great vessels and valves • Limits spread of action potentials to specific paths © 2013 Pearson Education, Inc. Layers of the Heart Wall • Endocardium continuous with endothelial lining of blood vessels – Lines heart chambers; covers cardiac skeleton of valves © 2013 Pearson Education, Inc. Figure 18.3 The pericardial layers and layers of the heart wall. Pulmonary trunk Fibrous pericardium Pericardium Parietal layer of serous pericardium Myocardium Pericardial cavity Epicardium (visceral layer of serous pericardium) Myocardium Endocardium Heart chamber © 2013 Pearson Education, Inc. Heart wall Figure 18.4 The circular and spiral arrangement of cardiac muscle bundles in the myocardium of the heart. Cardiac muscle bundles © 2013 Pearson Education, Inc. Chambers • Four chambers: – Two superior atria – Two inferior ventricles • Interatrial septum – separates atria – Fossa ovalis – remnant of foramen ovale of fetal heart • Interventricular septum – separates ventricles © 2013 Pearson Education, Inc. Figure 18.5e Gross anatomy of the heart. Aorta Superior vena cava Right pulmonary artery Pulmonary trunk Right atrium Right pulmonary veins Fossa ovalis Pectinate muscles Tricuspid valve Right ventricle Chordae tendineae Trabeculae carneae Inferior vena cava Frontal section © 2013 Pearson Education, Inc. Left pulmonary artery Left atrium Left pulmonary veins Mitral (bicuspid) valve Aortic valve Pulmonary valve Left ventricle Papillary muscle Interventricular septum Epicardium Myocardium Endocardium Chambers and Associated Great Vessels • Coronary sulcus (atrioventricular groove) – Encircles junction of atria and ventricles • Anterior interventricular sulcus – Anterior position of interventricular septum • Posterior interventricular sulcus – Landmark on posteroinferior surface © 2013 Pearson Education, Inc. Atria: The Receiving Chambers • Auricles – Appendages that increase atrial volume • Right atrium – Pectinate muscles – Posterior and anterior regions separated by crista terminalis • Left atrium – Pectinate muscles only in auricles © 2013 Pearson Education, Inc. Atria: The Receiving Chambers • Small, thin-walled • Contribute little to propulsion of blood • Three veins empty into right atrium: – Superior vena cava, inferior vena cava, coronary sinus • Four pulmonary veins empty into left atrium © 2013 Pearson Education, Inc. Ventricles: The Discharging Chambers • • • • Most of the volume of heart Right ventricle - most of anterior surface Left ventricle – posteroinferior surface Trabeculae carneae – irregular ridges of muscle on walls • Papillary muscles – anchor chordae tendineae © 2013 Pearson Education, Inc. Ventricles: The Discharging Chambers • Thicker walls than atria • Actual pumps of heart • Right ventricle – Pumps blood into pulmonary trunk • Left ventricle – Pumps blood into aorta (largest artery in body) © 2013 Pearson Education, Inc. Figure 18.5b Gross anatomy of the heart. Brachiocephalic trunk Superior vena cava Right pulmonary artery Ascending aorta Pulmonary trunk Right pulmonary veins Left common carotid artery Left subclavian artery Aortic arch Ligamentum arteriosum Left pulmonary artery Left pulmonary veins Auricle of left atrium Right atrium Right coronary artery (in coronary sulcus) Anterior cardiac vein Right ventricle Circumflex artery Right marginal artery Great cardiac vein Anterior interventricular artery (in anterior interventricular sulcus) Apex Small cardiac vein Inferior vena cava Anterior view © 2013 Pearson Education, Inc. Left coronary artery (in coronary sulcus) Left ventricle Figure 18.5a Gross anatomy of the heart. Left subclavian artery Left common carotid artery Brachiocephalic trunk Aortic arch Ligamentum arteriosum Ascending aorta Pulmonary trunk Right atrium Right coronary artery (in coronary sulcus) Right ventricle Auricle of left atrium Anterior interventricular artery (in anterior interventricular sulcus) Additional branch off left coronary artery, normal variation Left ventricle Apex of heart (left ventricle) Anterior aspect (pericardium removed) © 2013 Pearson Education, Inc. Figure 18.5f Gross anatomy of the heart. Superior vena cava Ascending aorta (cut open) Pulmonary trunk Aortic valve Right ventricle anterior wall (retracted) Opening to right atrium Pulmonary valve Interventricular septum (cut) Left ventricle Chordae tendineae Papillary muscles Trabeculae carneae Right ventricle Photograph; view similar to (e) © 2013 Pearson Education, Inc. Heart Valves • Ensure unidirectional blood flow through heart • Open and close in response to pressure changes • Two atrioventricular (AV) valves – – – – Prevent backflow into atria when ventricles contract Tricuspid valve (right AV valve) Mitral valve (left AV valve, bicuspid valve) Chordae tendineae anchor cusps to papillary muscles • Hold valve flaps in closed position © 2013 Pearson Education, Inc. Figure 18.7 The atrioventricular (AV) valves. 1 Blood returning to the heart fills atria, pressing against the AV valves. The increased pressure forces AV valves open. Direction of blood flow Atrium 2 As ventricles fill, AV valve flaps hang limply into ventricles. Cusp of atrioventricular valve (open) Chordae tendineae 3 Atria contract, forcing additional blood into ventricles. Ventricle Papillary muscle AV valves open; atrial pressure greater than ventricular pressure Atrium 1 Ventricles contract, forcing blood against AV valve cusps. 2 AV valves close. 3 Papillary muscles contract and chordae tendineae tighten, preventing valve flaps from everting into atria. AV valves closed; atrial pressure less than ventricular pressure © 2013 Pearson Education, Inc. Cusps of atrioventricular valve (closed) Blood in ventricle Heart Valves • Two semilunar (SL) valves – Prevent backflow into ventricles when ventricles relax – Open and close in response to pressure changes – Aortic semilunar valve – Pulmonary semilunar valve © 2013 Pearson Education, Inc. Figure 18.8 The semilunar (SL) valves. Aorta Pulmonary trunk As ventricles contract and intraventricular pressure rises, blood is pushed up against semilunar valves, forcing them open. Semilunar valves open As ventricles relax and intraventricular pressure falls, blood flows back from arteries, filling the cusps of semilunar valves and forcing them to close. Semilunar valves closed © 2013 Pearson Education, Inc. Figure 18.6a Heart valves. Pulmonary valve Aortic valve Area of cutaway Mitral valve Tricuspid valve Myocardium Mitral (left atrioventricular) valve Tricuspid (right atrioventricular) valve Aortic valve Pulmonary valve Cardiac skeleton © 2013 Pearson Education, Inc. Anterior Figure 18.6b Heart valves. Pulmonary valve Aortic valve Area of cutaway Mitral valve Tricuspid valve Myocardium Mitral (left atrioventricular) valve Tricuspid (right atrioventricular) valve Aortic valve Pulmonary valve © 2013 Pearson Education, Inc. Figure 18.6c Heart valves. Pulmonary valve Aortic valve Area of cutaway Mitral valve Tricuspid valve Chordae tendineae attached to tricuspid valve flap © 2013 Pearson Education, Inc. Papillary muscle Figure 18.6d Heart valves. Pulmonary valve Aortic valve Area of cutaway Mitral valve Tricuspid valve Opening of inferior vena cava Tricuspid valve Mitral valve Chordae tendineae Myocardium of right ventricle Interventricular septum Papillary muscles © 2013 Pearson Education, Inc. Myocardium of left ventricle Homeostatic Imbalance • Two conditions severely weaken heart: – Incompetent valve • Blood backflows so heart repumps same blood over and over – Valvular stenosis • Stiff flaps – constrict opening heart must exert more force to pump blood • Valve replaced with mechanical, animal, or cadaver valve © 2013 Pearson Education, Inc. Pathway of Blood Through the Heart • Pulmonary circuit – Right atrium tricuspid valve right ventricle – Right ventricle pulmonary semilunar valve pulmonary trunk pulmonary arteries lungs – Lungs pulmonary veins left atrium © 2013 Pearson Education, Inc. Pathway of Blood Through the Heart • Systemic circuit – Left atrium mitral valve left ventricle – Left ventricle aortic semilunar valve aorta – Aorta systemic circulation © 2013 Pearson Education, Inc. Figure 18.9 The heart is a double pump, each side supplying its own circuit. Both sides of the heart pump at the same time, but let’s Oxygen-poor blood follow one spurt of blood all the way through the Oxygen-rich blood Pulmonary system. Tricuspid semilunar valve Superior vena cava(SVC) valve Right Right Pulmonary Inferior vena cava(IVC) atrium ventricle trunk Coronary sinus SVC Pulmonary arteries Tricuspid valve Coronary sinus Pulmonary trunk Right atrium Pulmonary semilunar valve Right ventricle IVC To heart Oxygen-poor blood returns from the body tissues back to the heart. Oxygen-poor blood is carried in two pulmonary arteries to To lungs the lungs (pulmonary circuit) to be oxygenated. Systemic capillaries To body Pulmonary capillaries Oxygen-rich blood returns To heart to the heart via the four pulmonary veins. Oxygen-rich blood is delivered to the body tissues (systemic circuit). Aorta Pulmonary veins Aorta © 2013 Pearson Education, Inc. Aortic semilunar valve Left atrium Mitral valve Left ventricle Aortic semilunar valve Left ventricle Mitral valve Left atrium Four pulmonary veins Slide 1 Pathway of Blood Through the Heart • Equal volumes of blood pumped to pulmonary and systemic circuits • Pulmonary circuit short, low-pressure circulation • Systemic circuit long, high-friction circulation • Anatomy of ventricles reflects differences – Left ventricle walls 3X thicker than right • Pumps with greater pressure © 2013 Pearson Education, Inc. Figure 18.10 Anatomical differences between the right and left ventricles. Left ventricle Right ventricle Interventricular septum © 2013 Pearson Education, Inc. Coronary Circulation • Functional blood supply to heart muscle itself – Delivered when heart relaxed – Left ventricle receives most blood supply • Arterial supply varies among individuals • Contains many anastomoses (junctions) – Provide additional routes for blood delivery – Cannot compensate for coronary artery occlusion © 2013 Pearson Education, Inc. Coronary Circulation: Arteries • Arteries arise from base of aorta • Left coronary artery branches anterior interventricular artery and circumflex artery – Supplies interventricular septum, anterior ventricular walls, left atrium, and posterior wall of left ventricle • Right coronary artery branches right marginal artery and posterior interventricular artery – Supplies right atrium and most of right ventricle © 2013 Pearson Education, Inc. Figure 18.11a Coronary circulation. Aorta Pulmonary trunk Left atrium Superior vena cava Anastomosis (junction of vessels) Left coronary artery Right atrium Right coronary artery Right ventricle Right marginal artery Circumflex artery Posterior interventricular artery The major coronary arteries © 2013 Pearson Education, Inc. Left ventricle Anterior interventricular artery Coronary Circulation: Veins • Cardiac veins collect blood from capillary beds • Coronary sinus empties into right atrium; formed by merging cardiac veins – Great cardiac vein of anterior interventricular sulcus – Middle cardiac vein in posterior interventricular sulcus – Small cardiac vein from inferior margin • Several anterior cardiac veins empty directly into right atrium anteriorly © 2013 Pearson Education, Inc. Figure 18.11b Coronary circulation. Superior vena cava Anterior cardiac veins Great cardiac vein Coronary sinus Small cardiac vein The major cardiac veins © 2013 Pearson Education, Inc. Middle cardiac vein Figure 18.5d Gross anatomy of the heart. Aorta Superior vena cava Left pulmonary artery Right pulmonary artery Right pulmonary veins Left pulmonary veins Auricle of left atrium Left atrium Great cardiac vein Posterior vein of left ventricle Left ventricle Apex Posterior surface view © 2013 Pearson Education, Inc. Right atrium Inferior vena cava Coronary sinus Right coronary artery (in coronary sulcus) Posterior interventricular artery (in posterior interventricular sulcus) Middle cardiac vein Right ventricle Homeostatic Imbalances • Angina pectoris – Thoracic pain caused by fleeting deficiency in blood delivery to myocardium – Cells weakened • Myocardial infarction (heart attack) – Prolonged coronary blockage – Areas of cell death repaired with noncontractile scar tissue © 2013 Pearson Education, Inc. Figure 18.12a Microscopic anatomy of cardiac muscle. Nucleus Intercalated discs © 2013 Pearson Education, Inc. Cardiac muscle cell Gap junctions Desmosomes Microscopic Anatomy of Cardiac Muscle • Intercalated discs - junctions between cells - anchor cardiac cells – Desmosomes prevent cells from separating during contraction – Gap junctions allow ions to pass from cell to cell; electrically couple adjacent cells • Allows heart to be functional syncytium – Behaves as single coordinated unit © 2013 Pearson Education, Inc. Figure 18.12b Microscopic anatomy of cardiac muscle. Cardiac muscle cell Intercalated disc Mitochondrion Nucleus Mitochondrion T tubule Sarcoplasmic reticulum Z disc Nucleus Sarcolemma I band © 2013 Pearson Education, Inc. A band I band PowerPoint® Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College CHAPTER 18 The Cardiovascular System: The Heart: Part B © Annie Leibovitz/Contact Press Images © 2013 Pearson Education, Inc. Energy Requirements • Cardiac muscle – Has many mitochondria • Great dependence on aerobic respiration • Little anaerobic respiration ability – Readily switches fuel source for respiration • Even uses lactic acid from skeletal muscles © 2013 Pearson Education, Inc. Heart Physiology: Electrical Events • Heart depolarizes and contracts without nervous system stimulation – Rhythm can be altered by autonomic nervous system © 2013 Pearson Education, Inc. Sequence of Excitation • Cardiac pacemaker cells pass impulses, in order, across heart in ~220 ms – Sinoatrial node – Atrioventricular node – Atrioventricular bundle – Right and left bundle branches – Subendocardial conducting network (Purkinje fibers) © 2013 Pearson Education, Inc. Heart Physiology: Sequence of Excitation • Sinoatrial (SA) node – Pacemaker of heart in right atrial wall • Depolarizes faster than rest of myocardium – Generates impulses about 75X/minute (sinus rhythm) • Inherent rate of 100X/minute tempered by extrinsic factors • Impulse spreads across atria, and to AV node © 2013 Pearson Education, Inc. Heart Physiology: Sequence of Excitation • Atrioventricular (AV) node – In inferior interatrial septum – Delays impulses approximately 0.1 second • Because fibers are smaller diameter, have fewer gap junctions • Allows atrial contraction prior to ventricular contraction – Inherent rate of 50X/minute in absence of SA node input © 2013 Pearson Education, Inc. Heart Physiology: Sequence of Excitation • Atrioventricular (AV) bundle (bundle of His) – In superior interventricular septum – Only electrical connection between atria and ventricles • Atria and ventricles not connected via gap junctions © 2013 Pearson Education, Inc. Heart Physiology: Sequence of Excitation • Right and left bundle branches – Two pathways in interventricular septum – Carry impulses toward apex of heart © 2013 Pearson Education, Inc. Heart Physiology: Sequence of Excitation • Subendocardial conducting network – Complete pathway through interventricular septum into apex and ventricular walls – More elaborate on left side of heart – AV bundle and subendocardial conducting network depolarize 30X/minute in absence of AV node input • Ventricular contraction immediately follows from apex toward atria © 2013 Pearson Education, Inc. Figure 18.15a Intrinsic cardiac conduction system and action potential succession during one heartbeat. Superior vena cava Right atrium 1 The sinoatrial (SA) node (pacemaker) generates impulses. Internodal pathway 2 The impulses pause (0.1 s) at the atrioventricular (AV) node. 3 The atrioventricular (AV) bundle connects the atria to the ventricles. 4 The bundle branches conduct the impulses through the interventricular septum. Left atrium Subendocardial conducting network (Purkinje fibers) Interventricular septum 5 The subendocardial conducting network depolarizes the contractile cells of both ventricles. Anatomy of the intrinsic conduction system showing the sequence of electrical excitation © 2013 Pearson Education, Inc. Slide 1 Figure 18.15b Intrinsic cardiac conduction system and action potential succession during one heartbeat. Pacemaker potential SA node Atrial muscle AV node Ventricular muscle Pacemaker potential Plateau 0 100 200 300 400 Milliseconds Comparison of action potential shape at various locations © 2013 Pearson Education, Inc. Homeostatic Imbalances • Defects in intrinsic conduction system may cause – Arrhythmias - irregular heart rhythms – Uncoordinated atrial and ventricular contractions – Fibrillation - rapid, irregular contractions; useless for pumping blood circulation ceases brain death • Defibrillation to treat © 2013 Pearson Education, Inc. Homeostatic Imbalances • Defective SA node may cause – Ectopic focus - abnormal pacemaker – AV node may take over; sets junctional rhythm (40–60 beats/min) • Extrasystole (premature contraction) – Ectopic focus sets high rate – Can be from excessive caffeine or nicotine © 2013 Pearson Education, Inc. Homeostatic Imbalance • To reach ventricles, impulse must pass through AV node • Defective AV node may cause – Heart block • Few (partial) or no (total) impulses reach ventricles – Ventricles beat at intrinsic rate – too slow for life – Artificial pacemaker to treat © 2013 Pearson Education, Inc. Extrinsic Innervation of the Heart • Heartbeat modified by ANS via cardiac centers in medulla oblongata – Sympathetic rate and force – Parasympathetic rate – Cardioacceleratory center – sympathetic – affects SA, AV nodes, heart muscle, coronary arteries – Cardioinhibitory center – parasympathetic – inhibits SA and AV nodes via vagus nerves © 2013 Pearson Education, Inc. Figure 18.16 Autonomic innervation of the heart. The vagus nerve (parasympathetic) decreases heart rate. Dorsal motor nucleus of vagus Cardioinhibitory center Cardioacceleratory center Medulla oblongata Sympathetic trunk ganglion Thoracic spinal cord Sympathetic trunk Sympathetic cardiac nerves increase heart rate and force of contraction. AV node SA node © 2013 Pearson Education, Inc. Parasympathetic fibers Sympathetic fibers Interneurons Electrocardiography • Electrocardiogram (ECG or EKG) – Composite of all action potentials generated by nodal and contractile cells at given time • Three waves: – P wave – depolarization SA node atria – QRS complex - ventricular depolarization and atrial repolarization – T wave - ventricular repolarization © 2013 Pearson Education, Inc. Figure 18.17 An electrocardiogram (ECG) tracing. Sinoatrial node Atrioventricular node QRS complex R Ventricular depolarization Ventricular repolarization Atrial depolarization T P Q P-R Interval 0 © 2013 Pearson Education, Inc. S 0.2 S-T Segment Q-T Interval 0.4 Time (s) 0.6 0.8 Figure 18.18 The sequence of depolarization and repolarization of the heart related to the deflection waves of an ECG tracing. SA node R R T P Q Q S S 4 Ventricular depolarization is complete. R R Q Q S 5 Ventricular repolarization begins at apex, causing the T wave. S 2 With atrial depolarization complete, the impulse is delayed at the AV node. R T P Q S 3 Ventricular depolarization begins at apex, causing the QRS complex. Atrial repolarization occurs. © 2013 Pearson Education, Inc. R T P Q T P T P T P 1 Atrial depolarization, initiated by the SA node, causes the P wave. AV node Slide 1 6 Depolarization S Ventricular repolarization is complete. Repolarization Figure 18.19 Normal and abnormal ECG tracings. Normal sinus rhythm. Junctional rhythm. The SA node is nonfunctional, P waves are absent, and the AV node paces the heart at 40–60 beats/min. Second-degree heart block. Some P waves are not conducted through the AV node; hence more P than QRS waves are seen. In this tracing, the ratio of P waves to QRS waves is mostly 2:1. © 2013 Pearson Education, Inc. Ventricular fibrillation. These chaotic, grossly irregular ECG deflections are seen in acute heart attack and electrical shock. Heart Sounds • Two sounds (lub-dup) associated with closing of heart valves – First as AV valves close; beginning of systole – Second as SL valves close; beginning of ventricular diastole – Pause indicates heart relaxation • Heart murmurs - abnormal heart sounds; usually indicate incompetent or stenotic valves © 2013 Pearson Education, Inc. Figure 18.20 Areas of the thoracic surface where the sounds of individual valves can best be detected. Aortic valve sounds heard in 2nd intercostal space at right sternal margin Pulmonary valve sounds heard in 2nd intercostal space at left sternal margin Mitral valve sounds heard over heart apex (in 5th intercostal space) in line with middle of clavicle © 2013 Pearson Education, Inc. Tricuspid valve sounds typically heard in right sternal margin of 5th intercostal space Mechanical Events: The Cardiac Cycle • Cardiac cycle – Blood flow through heart during one complete heartbeat: atrial systole and diastole followed by ventricular systole and diastole – Systole—contraction – Diastole—relaxation – Series of pressure and blood volume changes © 2013 Pearson Education, Inc. Figure 18.21 Summary of events during the cardiac cycle. Left heart QRS P Electrocardiogram T 1st Heart sounds Dicrotic notch 120 Pressure (mm Hg) P 2nd 80 Aorta Left ventricle 40 Atrial systole Left atrium 0 Ventricular volume (ml) 120 EDV SV 50 ESV Atrioventricular valves Aortic and pulmonary valves Phase Open Closed Open Closed Open Closed 1 2a 2b 3 1 Left atrium Right atrium Left ventricle Right ventricle Atrial contraction Ventricular filling 1 © 2013 Pearson Education, Inc. Ventricular filling (mid-to-late diastole) Ventricular Isovolumetric contraction phase ejection phase 2a 2b Ventricular systole (atria in diastole) Isovolumetric relaxation 3 Early diastole Ventricular filling Cardiac Output (CO) • Volume of blood pumped by each ventricle in one minute • CO = heart rate (HR) × stroke volume (SV) – HR = number of beats per minute – SV = volume of blood pumped out by one ventricle with each beat • Normal – 5.25 L/min © 2013 Pearson Education, Inc. Autonomic Nervous System Regulation • Sympathetic nervous system activated by emotional or physical stressors – Norepinephrine causes pacemaker to fire more rapidly (and increases contractility) • Binds to β1-adrenergic receptors HR • contractility; faster relaxation – Offsets lower EDV due to decreased fill time © 2013 Pearson Education, Inc. Autonomic Nervous System Regulation • Parasympathetic nervous system opposes sympathetic effects – Acetylcholine hyperpolarizes pacemaker cells by opening K+ channels slower HR – Little to no effect on contractility • Heart at rest exhibits vagal tone – Parasympathetic dominant influence © 2013 Pearson Education, Inc. Autonomic Nervous System Regulation • Atrial (Bainbridge) reflex - sympathetic reflex initiated by increased venous return, hence increased atrial filling – Stretch of atrial walls stimulates SA node HR – Also stimulates atrial stretch receptors, activating sympathetic reflexes © 2013 Pearson Education, Inc. Figure 18.22 Factors involved in determining cardiac output. Exercise (by sympathetic activity, skeletal muscle and respiratory pumps; see Chapter 19) Heart rate (allows more time for ventricular filling) Venous return Physiological response Result © 2013 Pearson Education, Inc. Sympathetic activity Contractility EDV (preload) Initial stimulus Exercise, fright, anxiety Bloodborne epinephrine, thyroxine, excess Ca2+ Parasympathetic activity ESV Stroke volume Heart rate Cardiac output Chemical Regulation of Heart Rate • Hormones – Epinephrine from adrenal medulla increases heart rate and contractility – Thyroxine increases heart rate; enhances effects of norepinephrine and epinephrine • Intra- and extracellular ion concentrations (e.g., Ca2+ and K+) must be maintained for normal heart function © 2013 Pearson Education, Inc. Homeostatic Imbalance • Hypocalcemia depresses heart • Hypercalcemia increased HR and contractility • Hyperkalemia alters electrical activity heart block and cardiac arrest • Hypokalemia feeble heartbeat; arrhythmias © 2013 Pearson Education, Inc. Other Factors that Influence Heart Rate • Age – Fetus has fastest HR • Gender – Females faster than males • Exercise – Increases HR • Body temperature – Increases with increased temperature © 2013 Pearson Education, Inc. Homeostatic Imbalances • Tachycardia - abnormally fast heart rate (>100 beats/min) – If persistent, may lead to fibrillation • Bradycardia - heart rate slower than 60 beats/min – May result in grossly inadequate blood circulation in nonathletes – May be desirable result of endurance training © 2013 Pearson Education, Inc. Homeostatic Imbalance • Congestive heart failure (CHF) – Progressive condition; CO is so low that blood circulation inadequate to meet tissue needs – Reflects weakened myocardium caused by • • • • Coronary atherosclerosis—clogged arteries Persistent high blood pressure Multiple myocardial infarcts Dilated cardiomyopathy (DCM) © 2013 Pearson Education, Inc. Homeostatic Imbalance • Pulmonary congestion – Left side fails blood backs up in lungs • Peripheral congestion – Right side fails blood pools in body organs edema • Failure of either side ultimately weakens other • Treat by removing fluid, reducing afterload, increasing contractility © 2013 Pearson Education, Inc. Developmental Aspects of the Heart • Fetal heart structures that bypass pulmonary circulation – Foramen ovale connects two atria • Remnant is fossa ovalis in adult – Ductus arteriosus connects pulmonary trunk to aorta • Remnant - ligamentum arteriosum in adult – Close at or shortly after birth © 2013 Pearson Education, Inc. Developmental Aspects of the Heart • Congenital heart defects – Most common birth defects; treated with surgery – Most are one of two types: • Mixing of oxygen-poor and oxygen-rich blood, e.g., septal defects, patent ductus arteriosus • Narrowed valves or vessels increased workload on heart, e.g., coarctation of aorta – Tetralogy of Fallot • Both types of disorders present © 2013 Pearson Education, Inc. Figure 18.25 Three examples of congenital heart defects. Narrowed aorta Occurs in about 1 in every 500 births Ventricular septal defect. The superior part of the inter-ventricular septum fails to form, allowing blood to mix between the two ventricles. More blood is shunted from left to right because the left ventricle is stronger. © 2013 Pearson Education, Inc. Occurs in about 1 in every 1500 births Coarctation of the aorta. A part of the aorta is narrowed, increasing the workload of the left ventricle. Occurs in about 1 in every 2000 births Tetralogy of Fallot. Multiple defects (tetra = four): (1) Pulmonary trunk too narrow and pulmonary valve stenosed, resulting in (2) hypertrophied right ventricle; (3) ventricular septal defect; (4) aorta opens from both ventricles. Age-Related Changes Affecting the Heart • • • • Sclerosis and thickening of valve flaps Decline in cardiac reserve Fibrosis of cardiac muscle Atherosclerosis © 2013 Pearson Education, Inc.