* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download lecture 2-Cardiovascular Assessment
Management of acute coronary syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Coronary artery disease wikipedia , lookup
Rheumatic fever wikipedia , lookup
Heart failure wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Electrocardiography wikipedia , lookup
Artificial heart valve wikipedia , lookup
Myocardial infarction wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Aortic stenosis wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Jatene procedure wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
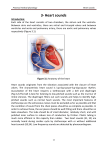
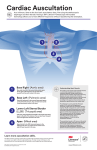
Assessment of the Heart, Great vessels of the neck, and Peripheral Vascular system Great vessels of the neck Jugular veins Carotid arteries JUGULAR VENOUS DISTENTION JVD Assessment Position client supine Then head elevated at 45 degrees INSPECTION: Lifts, heaves PMI (assess location) Inspection Chest for visible cardiac motion Estimate Jugular venous pressure Patient supine and head elevated to 15-30 degrees. JVP is the distance b/w highest point at which pulsation can be seen and the sternal angle Jugular venous pressure An indirect measure of right atrial pressure. Measured in centimeters from the sternal angle and is best visualized with the patient's head rotated to the left. Described for its quality and character, effects of respiration, and patient position-induced changes. Palpation Physical Landmarks Suprasternal notch Sternum Manubriosternal angle – Angle of Louis Intercostals Spaces palpations Palpate for PMI; easiest if patient sits up and leans forward has a diameter of 2cm and located with 10 cm of the midsternal line Palpate for general cardiac motion with fingertips and patient in supine position Palpate for radial, carotid, brachial, femoral, popliteal, posterior tibial And dorsalis pedis peripheral pulses palpations See figure 4-12 Rate strength of the pulse normal, diminished, or absent on a scale of 0 to +4, where 2+ is normal. See table 4-6 Auscultation: Auscultatory Sites Auscultation With a stethoscope Use diaphragm to assess higher pitched sounds Needs a lot of practice and experience Listen in a quiet area or to close eyes to reduce conflicting stimuli See also figure 4-10 for auscultatory Sites Auscultatory Sites: Cont. Auscultatory Sites The auscultatory Sites are close to but not the same as the anatomic locations of the valves. Aortic area2nd ICS at the right sternal border Pulmonic 2nd ICS at the left sternal border Tricuspid lt lower sternal border Mitral cardiac apex Heart Sounds Heart sounds are characterized by location, pitch, intensity, duration, and timing within the cardiac cycle Heart Sounds High-pitched sounds such as S1 and S2, murmurs of aortic and mitral regurgitation, and pericardial friction rubs are best heard with the diaphragm. The bell is preferred for low-pitched sounds such as S3 and S4. Heart Sounds – S1…(Lub)… S1: Closure of AV valves (mitral and tricuspid valves: M1 before T1) Correlates with the carotid pulse Loudest at the cardiac apex Can be split but not often Heart Sounds – S2…(Dub)… S2: Closure of Semilunar valves (aortic & pulmonic) Loudest at the base of the heart May have a split sound (A2 before P2) Heart Sounds – S2…(Dub)… S1 and S2 assessed in all four sites in upright and supine position S1 precedes and the S2 follows the carotid pulse Heart Sounds – Cont. Base (R/L 2nd ICS) – S2 louder than S1 Apex – S1 louder than S2 Normal physiologic S2 Split – Best heard at pulmonic area during inspiration Fixed split (no variation with inspiration) Extra Heart Sounds S3… S4… Due to volume overload Due to Rapid ventricular filling: ventricular gallop S1 -- S2-S3 (Ken--tuc-ky) Due to pressure overload Due to slow ventricular contraction: atrial gallop S4-S1 — S2 (Ten-nes—see) Extra Heart Sounds S3… S4… low-pitched sound usually heard at the apex of the heart. caused by rapid filling and stretching of the left ventricle when the left ventricle is somewhat noncompliant. characteristic of volume overloading, such as in CHF (especially left-sided heart failure), tricuspid or mitral valve insufficiency. a dull, low-pitched postsystolic atrial gallop usually caused by reduced ventricular compliance. best heard at the apex in the left lateral position. occurs with reduced ventricular compliance and is present in conditions such as aortic stenosis, hypertension, hypertrophic cardiomyopathies, and coronary artery disease. Murmurs Turbulent blood flow across a valve or a disease such as anemia or hyperthyroidism Listen for murmurs in the same auscultatory sites APETM Systolic b/w S1 & S2 Diastolic b/w S2 & S1 Characteristics of Heart Sounds Type of Murmur Midsystolic Pansystolic Diastolic Examples Location Pitch Radiation Aortic stenosis 2nd RICS Medium Neck, left sternal border Harsh Pulmonic stenosis 2nd and 3rd LICS Medium Left shoulder Harsh and neck Hypertrophic 3rd and 4th cardiomyopat LICS hy Medium Left sternal border to apex Harsh Mitral regurgitation Apex Medium to high Left axilla Blowing Tricuspid regurgitation Lower left sternal border Medium Right sternum, xiphoid Blowing Ventricular septal defect 3rd, 4th, and High 5th LICS Aortic regurgitation 2nd to 4th LICS Mitral stenosis Apex Quality Often harsh High Apex Low Little or none Blowing Murmurs They are classified by – timing and duration within the cardiac cycle (systolic, diastolic, and continuous), – location, – intensity, – shape (configuration or pattern), – pitch (frequency), – quality, and radiation Murmurs Grade I :barely audible Gr II : audible but quiet and soft Gr III : moderated loud, without thrust or thrill Gr IV : loud, with thrill Gr V : louder with thrill, steth on chest wall Gr VI : loud enough to be heard before steth on chest Murmurs Thrill: – a palpable murmur Bruits: – – – – – Vascular murmur sounds made by turbulent blood flow Heard over blood vessels with constricted lumens. Carotid and femoral are routinely assessed for bruits Sometimes found over the vertebral, subclavian and abdominal arteries