* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download lead I
Coronary artery disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Jatene procedure wikipedia , lookup
Myocardial infarction wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Atrial fibrillation wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Essentials of
Electrocardiography
Majid Haghjoo, MD
Professor, Cardiac Electrophysiologist
Department of Cardiac Pacing and Electrophysiology
Rajaie Cardiovascular Medical and Research Center
Introduction
• The electrocardiogram (ECG or EKG) is a
graphic recording of electric potentials
generated by the heart. The signals are detected
by means of metal electrodes attached to the
extremities and chest wall and are then amplified
and recorded by the electrocardiograph.
• ECG leads actually display the instantaneous
differences in potential between these electrodes.
Introduction
• The clinical utility of the ECG derives from its
immediate availability as a noninvasive,
inexpensive, and highly versatile test.
• In addition to its use in detecting arrhythmias,
conduction disturbances, and myocardial ischemia,
electrocardiography may reveal other findings
related to life-threatening metabolic disturbances
(e.g., hyperkalemia) or increased susceptibility to
sudden cardiac death (e.g., QT prolongation
syndromes).
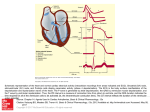
Electrophysiology
• Depolarization of the heart is the initiating event for
cardiac contraction. The electric currents that spread
through the heart are produced by three components:
– Cardiac pacemaker cells
– Specialized conduction tissue
– Heart muscle itself
• The ECG, however, records only the depolarization and
repolarization potentials generated by the atrial and
ventricular myocardium.
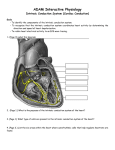
Schematic of the cardiac conduction system
ECG waveforms and intervals
Standard ECG features
• The electrocardiogram is recorded on special graph paper (1-mm2).
• Since the ECG paper speed is generally 25 mm/s, the smallest (1
mm) horizontal divisions correspond to 0.04 s (40 ms), with heavier
lines at intervals of 0.20 s (200 ms).
• Vertically, the ECG graph measures the amplitude of a given wave or
deflection (1 mV = 10 mm with standard calibration).
Heart Rate Measurement
• Each small square represents 0.04 seconds and each
large square represents 0.20 seconds, therefore:
- 1500 small squares in 1 minute (60 s)
- 300 large squares in 1 minute (60 s)
• The heart rate can be readily computed from the
interbeat (R-R) interval according to following formula:
– Rate = 300 ÷ number of the large squares in between two
consecutive QRS complexes
– Rate = 1500 ÷ number of the small squares in between two
consecutive QRS complexes
Quick Tips
•
•
•
•
•
300 ÷ 1 large square = 300
300 ÷ 2 large squares = 150
300 ÷ 3 large squares = 100 bpm
300 ÷ 4 large squares = 75 bpm
…
9
ECG intervals
• The PR interval measures the time (normally 120-200
ms) between atrial and ventricular depolarization.
• The QRS interval (normally 60-100 ms) reflects the
duration of ventricular depolarization.
• The QT interval includes both ventricular
depolarization and repolarization times and varies
inversely with the heart rate. A rate-related
("corrected") QT interval, QTc, can be calculated as
QT/√R-R and normally is ≤ 440 ms.
ECG waveforms
• The QRS complex is subdivided into specific
deflections or waves:
–
–
–
–
First negative deflection is termed a Q wave;
First positive deflection is termed an R wave.
A negative deflection after an R wave is an S wave.
Subsequent positive or negative waves are labeled
R' and S' waves, respectively.
– An uppercase capital letter (QRS) describes a
sizable wave (≥ 5 mm); a lowercase letter (qrs)
describes a tiny wave (< 5 mm).
– An entirely negative QRS complex is termed a QS
wave.
QRS morphologies
ECG recording tools
ECG Electrodes
ECG Leads
• ECG leads are divided into two groups: six limb
(extremity) leads and six chest (precordial) leads.
• The limb leads record potentials transmitted onto
the frontal plane, and the chest leads record
potentials transmitted onto the horizontal plane.
ECG Leads: six limb leads
• Each bipolar lead measures the difference in
potential between electrodes at two extremities:
– lead I = left arm (+) - right arm (-)
– lead II = left leg (+) - right arm (-)
– lead III = left leg (+) - left arm (-)
• The unipolar leads measure the voltage (V) at
one locus relative to an electrode (called the
central terminal or indifferent electrode):
– aVR = right arm (+)
– aVL = left arm (+)
– aVF = left foot (+)
ECG Leads: six chest or precordial leads
• The six chest leads are unipolar recordings
obtained by electrodes in the following positions:
– lead V1, fourth intercostal space just to the right of
the sternum
– lead V2, fourth intercostal space just to the left of the
sternum
– lead V3, midway between V2 and V4
– lead V4, midclavicular line fifth intercostal space
– lead V5, anterior axillary line same level as V4
– lead V6, midaxillary line, same level as V4 and V5.
Precordial electrode placement
ECG leads
• The conventional 12-lead ECG can be supplemented
with additional leads under special circumstances:
– right precordial leads V3R, V4R, etc., are useful in detecting evidence of
acute right ventricular ischemia.
– Bedside monitors and ambulatory ECG recordings usually
employ only one or two modified leads (MCL1, MCL6).
Right precordial leads
MCL1
MCL6
P Wave
• The normal atrial depolarization vector is oriented
downward and toward the subject's left. Since this vector
points toward the positive pole of lead II and toward the
negative pole of lead aVR, the normal P wave will be positive
in lead II and negative in lead aVR.
• By contrast, activation of the atria from an ectopic
pacemaker in the lower part of either atrium or in the
AV junction region may produce retrograde P waves
(negative in lead II, positive in lead aVR).
• The normal P wave in lead V1 may be biphasic with a positive
component reflecting right atrial depolarization, followed by a
small (<1 mm2) negative component reflecting left atrial
depolarization.
P-wave vector
Normal p-wave
Ectopic p-wave
QRS Complex
• Normal ventricular depolarization can be illustrated
by two major vector:
• Depolarization of the interventricular septum from the
left to the right and anteriorly (vector 1).
• Simultaneous depolarization of the right and left
ventricles; it is normally dominated by the more massive
left ventricle (vector 2).
• The precordial lead where the
R = S waves is referred to as
the transition zone (usually V3 or V4).
QRS complex axis
• The QRS pattern in the extremity leads may
vary considerably from one normal subject to
another depending on the electrical axis of the
QRS, which describes the mean orientation of
the QRS vector with reference to the six frontal
plane leads. Normally, the QRS axis ranges
from -30° to +100°.
• An axis more negative than -30° is referred to as
left axis deviation, while an axis more positive
than +100° is referred to as right axis deviation.
QRS complex axis
QRS Complex
• Left axis deviation may occur as a normal variant
but is more commonly associated with left
ventricular hypertrophy, a left anterior fascicular
hemiblock, or inferior myocardial infarction.
• Right axis deviation may also occur as a normal
variant (particularly in children and young
adults); as a spurious finding due to reversal of
the left and right arm electrodes; or in conditions
such as right ventricular overload (acute or
chronic), infarction of the lateral wall of the left
ventricle, dextrocardia, left pneumothorax, or left
posterior fascicular block.
T wave
• Normally, the mean T-wave vector is oriented
roughly concordant with the mean QRS vector.
• Since depolarization and repolarization are
electrically opposite processes, this normal
QRS-T wave vector concordance indicates that
repolarization must normally proceed in the
reverse direction from depolarization (i.e., from
ventricular epicardium to endocardium).
U wave
• The normal U wave is a small, rounded deflection (1
mm) that follows the T wave and usually has the same
polarity as the T wave.
• An abnormal increase in U-wave amplitude is most
commonly due to drugs (e.g., dofetilide, amiodarone,
sotalol, quinidine, procainamide, disopyramide) or to
hypokalemia.
• Very prominent U waves are a marker of increased
susceptibility to the torsades de pointe type of ventricular
tachycardia. Inversion of the U wave in the precordial
leads is abnormal and may be a subtle sign of ischemia.
Normal electrocardiogram
P-wave abnormalities
• Right atrial overload (acute or chronic)
may lead to an increase in P-wave
amplitude (≥ 2.5 mm) (right atrial
abnormality).
• Left atrial overload typically produces a
biphasic P wave in V1 with a broad
negative component or a broad (≥ 120
ms), often notched P wave in one or
more limb leads. This pattern may also
occur with left atrial conduction delays in
the absence of actual atrial enlargement,
leading to the more general designation
of left atrial abnormality.
Right Ventricular Hypertrophy
• Right ventricular hypertrophy (RVH) due to a
pressure load is characterized by a relatively tall R
wave in lead V1 (R≥S wave), usually with right axis
deviation; alternatively, there may be a qR pattern in
V1 or V3R. ST depression and T-wave inversion in
the right to midprecordial leads are also often
present (right ventricular strain). Prominent S waves
may occur in the left lateral precordial leads.
• RVH due to ostium secundum-type atrial septal
defects, with the accompanying right ventricular
volume overload, is commonly associated with an
incomplete or complete right bundle branch block
pattern with a rightward QRS axis.
Left Ventricular Hypertrophy
• A number of different voltage criteria for left ventricular
hypertrophy (LVH) have been proposed on the basis of
the presence of tall left precordial R waves and deep
right precordial S waves [e.g., SV1+ (RV5 or RV6) > 35
mm]. Repolarization abnormalities (ST depression with
T-wave inversions (left ventricular strain) may also
appear in leads with prominent R waves.
• LVH may increase limb lead voltage with or without
increased precordial voltage (e.g., RaVL+ SV3 > 20
mm in women and > 28 mm in men). The presence of
LA abnormality increases the likelihood of underlying
LVH in cases with borderline voltage criteria. LVH
often progresses to incomplete or complete left bundle
branch block.
Ventricular Hypertrophy
Bundle Branch Blocks
• Impairment of conduction in either the right or left bundle
system leads to widening of the QRS interval (complete
bundle branch blocks, ≥120 ms; incomplete 100 and 120
ms).
• The QRS vector is usually oriented in the direction of the
myocardial region where depolarization is delayed. Thus,
with right bundle branch block (RBBB), the terminal QRS
vector is oriented to the right and anteriorly (rSR' in V1 and
qRS in V6). Left bundle branch block (LBBB) alters both
early and later phases of ventricular depolarization. The
major QRS vector is directed to the left and posteriorly. In
addition, the normal early left-to-right pattern of septal
activation is disrupted such that septal depolarization
proceeds from right to left as well. As a result, LBBB
generates wide, predominantly negative (QS) complexes in
lead V1 and entirely positive (R) complexes in lead V6.
Typical QRS-T patterns in RBBB vs. LBBB
Bundle Branch Blocks
• Bundle branch block may occur in a variety of
conditions. In subjects without structural heart disease,
RBBB is seen more commonly than LBBB. RBBB also
occurs with heart disease, both congenital (e.g., atrial
septal defect) and acquired (e.g., valvular, ischemic).
• LBBB is often a marker of one of four underlying
conditions associated with increased risk of
cardiovascular morbidity and mortality: coronary heart
disease, hypertensive heart disease, aortic valve disease,
and cardiomyopathy. Bundle branch blocks may be
chronic or intermittent. A bundle branch block may be
rate-related; for example, it often occurs when the
heart rate exceeds some critical value.
Bundle Branch Blocks
• Partial blocks (fascicular or "hemiblocks") in the left
bundle system (left anterior or posterior fascicular
blocks) generally do not prolong the QRS duration
substantially but instead are associated with shifts in
the frontal plane QRS axis (leftward or rightward,
respectively).
• More complex combinations of fascicular and bundle
branch blocks may occur involving the left and right
bundle system. Examples of bifascicular block include
right bundle branch block and left posterior fascicular
block, right bundle branch block with left anterior
fascicular block, and complete left bundle branch
block.
Wolff-Parkinson-White
• Prolongation of QRS duration does not necessarily
indicate a conduction delay but may be due to
preexcitation of the ventricles via a bypass tract, as in
Wolff-Parkinson-White (WPW) patterns and related
variants.
• The diagnostic triad of WPW consists of a wide QRS
complex associated with a relatively short PR interval
and slurring of the initial part of the QRS (delta wave),
the latter effect due to aberrant activation of ventricular
myocardium.
Myocardial Ischemia and
Infarction
• When the acute ischemia is transmural, the ST vector is usually
shifted in the direction of the outer (epicardial) layers, producing
ST elevations and sometimes, in the earliest stages of ischemia,
tall, positive so-called hyperacute T waves over the ischemic
zone.
• With ischemia confined primarily to the subendocardium, the ST
vector typically shifts toward the subendocardium and ventricular
cavity, so that overlying leads show ST-segment depression.
Clinical Interpretation of the ECG
• Many mistakes in ECG interpretation are errors
of omission. Therefore, a systematic approach is
essential. The following 14 points should be
analyzed carefully in every ECG:
(1) standardization (calibration) and technical features (including
lead placement and artifacts); (2) rhythm; (3) heart rate; (4) PR
interval/AV conduction; (5) QRS interval; (6) QT/QTc
interval; (7) mean QRS electrical axis; (8) P waves; (9) QRS
voltages; (10) precordial R-wave progression; (11) abnormal Q
waves; (12) ST segments; (13) T waves; (14) U waves.