* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Cardiac Pathophysiology B
Saturated fat and cardiovascular disease wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Jatene procedure wikipedia , lookup
Rheumatic fever wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Electrocardiography wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Coronary artery disease wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Cardiac surgery wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Heart failure wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
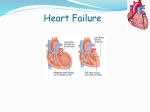
Cardiac Pathophysiology Part B 1 Heart Failure • The heart as a pump is insufficient to meet the metabolic requirements of tissues. • Can be due to: – dysfunction of the left ventricle – dysfunction of the right ventricle – or due to inadequate perfusion despite normal or elevated cardiac output 2 Classification of Heart Failure • Acute –develops quickly • Chronic – conditions gradually increase demands on the heart; when the heart and circulatory system can no longer adapt the result is heart failure – Can lead to acute failure with excessive cardiac demand 3 Four broad consequences of heart failure • • • • Congestion – blood backs up Activation of circulatory compensations Cardiac output declines Death 4 Types of Heart Failure • High output vs. Low output • High output – Anemia – Septicemia – Hyperthroidism (thyrotoxicosis) – Beriberi • Low output – Decreased pumping ability and cardiac output 5 • Right-sided vs. Left sided Heart Failure • Right-sided HF – Most common cause is left heart failure – Can occur independently in primary lung disease conditions • COPD, ARDS, cystic fibrosis • Cor pulmonale • Left-sided HF – Decreased output to body – Blood backs up 6 Systolic vs. Diastolic HF • Systolic – decreased contraction leads to decreased output and poor perfusion of tissues 7 Contractility is reduced by diseases that disrupt myocyte activity – Most common cause is myocardial infarction – Myocarditis – Myocardopathies • When contractility decreases, stroke volume decreases, and left ventricular end-diastolic volume (LVEDV) increases. • This causes dilation of the heart and increased preload 8 Preload can also increase with excess plasma volume – I.V. Fluid administration – Renal failure – Mitral valve disease • Increased LVEDV at first increases C.O., but over time can cause dysfunction of sarcomeres (stretched too far) and decreased contractility 9 Increased afterload is usually due to increased peripheral resistance – Hypertension • Left ventricle works harder to overcome resistance, and hypertrophies. • Hypertrophy causes changes in the myocytes. • Also see deposition of collagen between myocyctes which can disrupt contractility and make ventricle more likely to dilate and fail. 10 Leads to increased blood pressure and pulmonary congestion → – Dyspnea – Orthopnea – difficulty breathing in any position other than upright – Coughing up frothy sputum – Chest pain –due to hypoxia at heart – Fatigue/confusion – Skin is pale, cold, sweaty – Pulse and lung sounds abnormal – Decreased urine output – Edema 11 Treatment is aimed at breaking the cycle of decreasing contractility and increasing preload and afterload. • Oxygen, nitrates and morphine – improve myocardial oxygenation, help relieve coronary spasm while lowering preload through systemic vasodilation. • I.V. inotropic drugs such as dopamine or dobutamine – increase contractility of the heart and can raise B.P. in hypotensive individuals. 12 • Diuretics – reduce preload • ACE inhibitors – reduce preload and afterload by decreasing aldosterone levels and reducing peripheral venous resistance • Beta-blockers have been helpful in some people • Coronary by-pass • Salt restriction • Heart transplant 13 Diastolic Heart Failure • See symptoms and signs of heart failure, a preserved ejection fraction, and abnormal diastolic function • Accounts for 25 -40% of all cases of heart failure 14 Diastolic H.F. Results from: • Decreased compliance of left ventricle and abnormal diastolic relaxation- results in increased pressure in ventricle at the end of diastole • Pressure is reflected back into the atrium and pulmonary circulation 15 Major causes: • Hypertension – induced myocardial hypertrophy and myocardial ischemia with ventricular remodeling • Aortic valvular disease • Mitral valvular disease • Cardiomyopathies 16 Signs and symptoms are similar to systolic heart failure • Diagnosis made by echocardiography and heart cateterization 17 Management • Improve ventricular relaxation and prolong diastolic filling times to reduce diastolic pressure • Calcium channel blockers, beta-blockers, and ACE inhibitors have been used with success 18