* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download W12-1600-Dunn-ClinicalImpact
Survey
Document related concepts
Meningococcal disease wikipedia , lookup
West Nile fever wikipedia , lookup
Gastroenteritis wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Anaerobic infection wikipedia , lookup
Carbapenem-resistant enterobacteriaceae wikipedia , lookup
Surround optical-fiber immunoassay wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Marburg virus disease wikipedia , lookup
Leptospirosis wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Oesophagostomum wikipedia , lookup
Neonatal infection wikipedia , lookup
Neisseria meningitidis wikipedia , lookup
Transcript
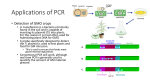
The Clinical Impact of Real-Time Molecular Infectious Disease Diagnostics Jim Dunn, Ph.D., D(ABMM) Cook Children’s Medical Center Ft. Worth, TX Molecular Microbiology Fastest growing area in clinical laboratory medicine Integral and necessary component of many diagnostic laboratories Traditional methods being rapidly displaced by molecular testing 2 Clinical Value Qualitative (pos/neg) nucleic acid tests are especially valuable for the detection of infectious agents that are: Unculturable Present in extremely low quantities Fastidious or slow-growing Dangerous to amplify in culture 3 Clinical Value Quantitative (viral load) methods are important for monitoring certain chronic infections. These tests allow us to: monitor therapy detect the development of drug resistance predict disease progression 4 Real-Time PCR Introduced in mid-1990’s Rapidly evolving field with numerous technological advances Continuous fluorescence monitoring of nucleic acid amplification within a closed system. One tube amplification and detection 5 Fluorescence Monitoring Plateau: Qualitative end-point read Exponential: Quantitative real-time read 6 Real-Time PCR Rapid assay development Simplified primer and probe design Simple and versatile to perform Pre-optimized universal master mixes Universal conditions for amplification Multiple chemistries available Choice of instrumentation 7 What’s the impact on patient management and outcomes? Case #1 4 y.o. boy presents with 2-day history of fever and headache Day of presentation began to complain of neck pain Temp = 102.7oF Mild photophobia No rashes Intact neurologic exam 9 Case #1 Complete Blood Count - 9,300 cells/mm3 - 45% PMN, 40% lymph, 15 mono Cerebrospinal Fluid (CSF) - WBC = 75 cells/mm3 - 72% PMN, 8% lymph, 20% mono - protein = 22 mg/dl - glucose = 60 mg/dl 10 Case #1 CSF gram stain mod WBC, no organisms I.V. ceftriaxone started Blood, CSF, urine bacterial cultures obtained Enterovirus RT-PCR on CSF ordered 11 Case #1 ANSWER Blood, CSF, urine bacterial cultures = neg Enterovirus RT-PCR = POSITIVE DIAGNOSIS: Viral Meningitis 12 Aseptic Meningitis Clinical and lab evidence of meningeal inflammation not due to bacteria 75,000 cases/year in US 80 to 90% due to Enteroviruses Occur mainly in summer and fall Difficult to distinguish from bacterial meningitis based on clinical features alone Enteroviral meningitis has good prognosis 13 Enteroviruses aseptic meningitis, myocarditis, flaccid paralysis, neonatal sepsis-like disease, encephalitis, febrile rash disease now probably >100 serotypes based on capsid sequence analysis molecular diagnosis has replaced traditional cell culture 14 Enteroviruses Comparison of RT-PCR vs. Viral Culture 59 inpatient CSF samples tested Result RT-PCR Culture Pos 37 22 Neg 22 37 Sensitivity of CSF viral culture = 60% Culture time to detection = 3 – 5 days RT-PCR time to detection = 3 – 4 hours 15 Enteroviruses Rapid diagnosis of enteroviral meningitis by real time PCR impacts clinical management: Earlier hospital discharge Fewer additional diagnostic tests Decreased antibiotic usage Decreased overall health care costs 16 17 Hospital-Acquired Infections (HAIs) On an annual basis account for: ~2 million infections ~100,000 deaths $4-6 billion in health care costs 50–60% of the HAIs occurring in the USA each year are caused by antibiotic-resistant bacteria High rate of antibiotic resistance increases morbidity, mortality & costs associated with HAIs Jones. Chest 2001;119:397S–404S Weinstein. Emerg Infect Dis 1998;4:416–420 Vancomycin-Resistant Enterococci (VRE) Since 1989, a rapid increase in the incidence of infection and colonization with VRE has been reported by U.S. hospitals This poses important problems, including: Lack of available antimicrobial therapy for VRE infections because most VRE are also resistant to drugs previously used to treat such infections Possibility that vancomycin-resistance genes present in VRE can be transferred to other gram-positive bacteria (e.g. Staphylococcus aureus ) 19 Vancomycin-Resistant Enterococci (VRE) E. faecium and E. faecalis that have acquired genes vanA and/or vanB Most important reservoir for VRE is the colonized gastrointestinal tracts of patients Transmission can occur: Contaminated hands of healthcare workers Contamination of environment 20 Vancomycin-Resistant Enterococci The Problem? Major nosocomial pathogen Up to 6.3% of nosocomial enterococcal bloodstream infections in pediatric hospitals 28.5% of nosocomial enterococcal infections in ICU patients (NNIS-2003) Wisplinghoff, et al. Pediatr Infect Dis J 22:686, 2003. NNIS. Am J Infect Control 32:470, 2004. Vancomycin-Resistant Enterococci What Should Be Done? Active Surveillance (SHEA & CDC) High Risk Patients/Locations: Admission & Periodic (e.g. weekly) VRE culture often requires ≥ 72 hrs. High Rate of False Negatives with Culture Muto, et al. Infect Control Hosp Epi 24:362, 2003. CDC. MMWR 44:1, 1995. Vancomycin-Resistant Enterococci Lab-Developed Taqman Real Time Multiplex vanA/vanB PCR Assay Sens = 100%, Spec = 98% PPV = 91%, NPV = 100% Screening & Surveillance in Admitted Oncology and Bone Marrow Transplant Pre-emptive isolation until VRE result known 23 VRE by Real Time PCR Greater sensitivity & More rapid results Rapid Detection → Infection Control Measures Reduce Duration of Contact Isolation Excess costs associated with nosocomial infections justify screening and preventive infection control measures 24 Cost-Effectiveness of VRE Surveillance Attributable cost of surveillance vs. cost of nosocomial infections $1,000,000 $761,320 $800,000 $600,000 2-year period Hosp #1 $253,099 $400,000 $200,000 Hosp #2 $0 Hosp #1 No surveillance Surveillance Hosp #2 Muto, et al. Infect Control Hosp Epidemiol 23:429-435, 2002. Cost-Effectiveness of VRE Surveillance by Real Time PCR University of Iowa Hospital Real Time PCR for VRE Average TAT = 1.3 days (3.4 days for culture) ↓ length of stay by ~2 days for patients discharged to long-term care facilities $205,000 annual savings 26 Cost-Effectiveness of VRE Surveillance by Real Time PCR Rapid determination of VRE colonization status prevented 2,348 isolation days/year when compared to culture Annual savings = $87,600 $187,200 $200,000 $150,000 $99,600 $100,000 $50,000 $0 27 MPCR Culture Bordetella pertussis 28 Bordetella pertussis Endemic disease, occurs year-round, epidemic cycles every 3 or 4 years Transmitted by large droplets Attack rates among close contacts as high as 80 to 100% Waning immunity leads to susceptible adolescents and adults Family members often source for infected infants 29 Bordetella pertussis 30 Bordetella pertussis 31 Diagnosis Specimens NP swab or aspirate Throat & anterior nares swabs Lower rates of recovery Ciliated respiratory epithelium not found in pharynx 32 Diagnosis Find highest concentration of organism during catarrhal stage and beginning of paroxysmal stage Concentration of organism negatively correlates with increasing age conc. in infants conc. adolescents/adults 33 Diagnosis Culture: still “gold standard” DFA: low sens and variable spec Sens actually 15-60% compared to PCR Special media/transport, long incubation Always back-up with cx or PCR Serology: not part of case definition Not standardized Epidemiology/vaccine efficacy 34 Real-Time PCR Very sensitive (~1 cfu/rxn) Don’t need viable organism Good for mild, atypical cases, older patients Results within hours Not standardized between labs Some labs multiplex with B. parapertussis 35 Hospital-Acquired Pertussis Among Newborns 36 Cook Children’s 6 infants admitted with pertussis w/in a few days of each other Confirmed by real-time PCR w/in 24 hrs admit 4 infants in PICU Investigation reveals all born at same local hospital One HCW in newborn nursery with cough, post-tussive emesis, dyspnea PCR pos for B. pertussis MMWR 57:600-603, 2008. Timeline of Infants with Pertussis from a General Hospital Newborn Nursery Nursery Worker: Prodrome? § ** 07/10/2004 Infant # 1 *† Infant # 2 *† Infant # 3 *† Infant # 4 Infant #6 * § PICU §§ PICU §§ PICU §§ ¶ § PICU §§ ¶ §§ ¶ § *† Infant # 8 §§ ¶ § † ¶ § *† Infant # 7 ¶ §§ § *† Infant # 9 Infant # 10 § *† Infant # 5 ¶ § ††7/17/2004 PICU ¶ § *† *† ¶ 2 4 6 8 10 12 14 16 18 20 22 24 26 28 30 2 4 6 8 10 12 14 16 18 20 22 24 26 28 30 2 June July Aug * Date born † Exposure in nursery § Symptoms started ¶ Admission/Diagnosis Date **Outbreak noted †† HCW PCR +/Furlough §§ Discharge Date ¶ 8/28 Out pt § unk ¶ 10/4 *† Infant # 11 §§ 8/7 § unk Out pt Summary HCW furloughed/treated Families of 110 infants born at local hospital evaluated for cough illness 18 with cough: PCR neg 2 additional PCR pos Total of 11 infants with confirmed pertussis Attack rate ~10% MMWR 57:600-603, 2008. Cook Children’s Molecular Lab 40 What’s So Cool About Real-Time PCR? Decreased Turnaround Times/High Throughput Closed system No additions made after specimen is added Contamination control – No false positives More Standardized Simultaneous amplification, detection, & data analysis Pre-optimized master mixes, reproducible Less expensive that traditional PCR Increased Sensitivity 41 Thanks