* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download What is Cholesterol?......cont. - Home
Peptide synthesis wikipedia , lookup
Biochemistry wikipedia , lookup
Oligonucleotide synthesis wikipedia , lookup
Biosynthesis wikipedia , lookup
Artificial gene synthesis wikipedia , lookup
Fatty acid synthesis wikipedia , lookup
Amino acid synthesis wikipedia , lookup
Wilson's disease wikipedia , lookup
Glyceroneogenesis wikipedia , lookup
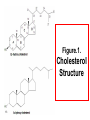
Gene expression profiling wikipedia , lookup
Human digestive system wikipedia , lookup
Cholesterol 1 Contents of The Lecture • • • • • • What is Cholesterol? Structure of Cholesterol Structure of Cholesteryl Ester Normal Cholestrol Level Sources of Cholesterol What Are The Exogenous Sources Of Cholesterol? • Absorption Of Exogenous Cholesterol 2 Contents of The Lecture • Endogenous Sources Of Cholesterol • The Main Role of the Liver in the Production of the Majority of the Body Cholesterol Pool • Cholesterol Synthesis • Regulation of Cholesterol Synthesis. • Cholesterol is Transprted from Intestine to Liver in Lipoproteins 3 Contents of The Lecture • • • • • How to Utilize Cholesterol ? Lipoprotein lipase The Fate of Unused LDL HDL (Good Cholesterol) What Happens if Cholesterol Gets High? How to Treat Hypercholestrolemia? • Biological Functions of Cholesterol • Cholesterol Catabolism 4 Contents of The Lecture • • • • • 5 Cholesterol Recycling And Excretion Principle of the Test Materials Method Results • What is Cholesterol? -Cholesterol is the most prominent member of steroid family of lipids -Cholesterol is present in tissues and in plasma either as free cholesterol or as a storage form, combined with a long chain fatty acid as cholesteryl ester. 6 What is Cholesterol?.....cont. -The term lipid applies to a class of compounds that are soluble in organic solvents and nearly insoluble in water. -Cholesterol is an amphipathic lipid, and , therefore, it becomes an essential structural component of membranes and of the outer layer of plasma membranes. 7 What is Cholesterol?.....cont. • Only a limited number of numerous different lipids are of clinical and analytical importance and cholesterol is one of these lipids that measuring its concentration is of a clinical and analytical importance since cholesterol is associated with cardiac vascular diseases. 8 What is Cholesterol?......cont. -Cholesterol is found principally in animals and humans, where it is also the main sterol. -Small quantities are sythesized in other eukaryotes, such as plants and fungi. -Virtually all human cells and body fluids contain some cholesterol. 9 •Structure of Cholesterol -Cholesterol is a sterol because it’s a steroid and alcohol at the same time. -Cholesterol is a solid alcohol of high molecular weight. -Cholesterol, like other steroids, is a derivative of the cyclic hydrocarbon Perhydrocyclopentanophenanthrene. 10 Perhydrocyclopentanophenanthrene 11 Structure of Cholesterol….cont. - Cholesterol consists of four rings. These rings are identified by the first four letters of the alphabet. - The carbons of cholesterol which are 27 are numbered in the sequence shown in figure 1 . 12 Figure.1. Cholesterol Structure 13 Structure of Cholesterol….cont. - In addition to the : 1. Basic ring structure 2. Cholesterol contains a hydroxyl group at C-3 3. An aliphatic chain of 8 carbons at C-17 of ring D. 4. Methyl groups at C-10 and C 13. 5. A 14 5 double bond. Structure of Cholesterol C A 15 B D Structure of Cholesteryl Ester Cholestryl esters: Much of the plasma cholesterol is in an esterified form (with a fatty acid attached at carbon 3) which makes the structure even more hydrophobic. 16 Cholestryl Ester Structure 17 Normal Cholestrol Level • Desirable total blood cholesterol level less than 200 mg/dL (5.13 mmol/l). About 50% of all adults fall into this cholesterol level. • Borderline high risk total blood cholesterol level 200-239 mg/dL (5.136.13 mmol/l). About 33% of adults fall into this cholesterol level. • High risk total blood cholesterol level 240 mg/dL (6.14 mmol/l) and over. You have twice the risk of coronary heart disease. About 17% of adults are in this cholesterol level. 18 Sources of Cholesterol - Cholesterol in the intestine comes from diet, bile, intestinal secretions. Therefore cholesterol has 2 major sources: -Exogenous -Endogenous 19 Major sources of liver cholesterol 1. Dietary cholesterol 3. Cholesterol synthesized in extrahepatic tissues 2. De novo synthesis in liver Chylomicron remnants HDL Liver Cholesterol Pool Secretion of HDL and VLDL 20 Conversion to bile acids/salts Free cholesterol secreted in bile Major routes by which cholesterol leaves liver What Are The Exogenous Sources Of Cholesterol? -As a typical product of animal metabolism, cholesterol occurs in foods of animal origin such as egg yolk, meat, liver, seafood, whole fat dairy products and brain. -These animal products provide the bulk of dietary cholesterol. 21 What Are The Exogenous Sources Of Cholesterol?........cont. • However the fat found in food is composed mainly of triglycerides of about 98 – 99% and only the remaining 1% to 2% of the lipids include cholesterol and other lipids. 22 Absorption Of Exogenous Cholesterol • Practically cholesterol in the intestine is present in the unesterified (free) form, since esterified cholesterol is rapidly hydrolyzed in the intestine by cholesterol esterases which exisit in pancreatic and small intestinal secretions. 23 Absorption Of Exogenous Cholesterol ….cont. • The liver and gut are connected by a cystic duct which empties bile from the gallbladder into the gut. • The bile is formed in the liver, and stored in the gall bladder until a meal with fat enters the upper small intestine. Bile solubilize cholesterol (and other lipids) make them readily absorbed by intestinal cells. 24 Absorption Of Exogenous Cholesterol……cont • In order to be absorbed, cholesterol is soluibilized by formation of mixed micelles containing : (1) unesterified cholesterol, (2) fatty acids, (3) monoglycerides (monoacylglycerols), (4) phospholipids (lysolecithin) and (5) conjugated bile acids. These micelles also facilitate cholesterol transport across the luminal cell surfaces. 25 Absorption Of Exogenous Cholesterol….cont. • In the absence of bile acids, digestion and absorption of both cholesterol and triglycerides are severely impaired. On the average 30-60% of dietary and intestinal cholesterol is absorbed daily, to a maximum of ~1 g/d when the oral intake reaches 3 g/d 26 -Endogenous Sources Of Cholesterol • Cholesterol is synthesized by virtually all tissues in humans. •Liver is the major site of cholesterol synthesis. •Intestine is also a main site of cholesterol synthesis after the liver 27 -Endogenous Sources Of Cholesterol …..cont. •Adrenal cortex and reproductive tissues including ovaries, testes and placenta make the largest contributions to the body’s cholesterol pool after the liver and intestine. 28 Endogenous Sources Of Cholesterol ……cont. -In adults the liver and intestinal wall (gut) propably supply over 90% of the plasma cholesterol of endogenous origin. -Almost all animal tissues synthesize cholesterol from acetyl Co.A. 29 The Main Role of the Liver in the Production of the Majority of the Body Cholesterol Pool • Of endogenous cholesterol, up to 75% of cholesterol in the body is produced by the liver. 30 The Main Role of the Liver in the Production of the Majority of the Body Cholesterol Pool ……cont. • In other words, the liver synthesizes cholesterol even in the total absence of cholesterol in the diet. • With an increased intake of cholesterol in the diet, there is a somewhat reduced synthesis of cholesterol in the liver, keeping the total cholesterol pool roughly constant. .31 Cholesterol Synthesis • Similar to ketogenic pathway • Occurs in cytosol • Requires NADPH and ATP • Highly regulated • 80 % in liver, ~10% intestine, ~5% skin 32 •De Novo Synthesis Of Cholesterol -Mevalonate Synthesis: 1- The sequence of cholesterol biosynthesis begins with a condensation in the cytosol of two molecules of acetyl Co.A. A reaction catalyzed by thiolase. 33 De Novo Synthesis Of Cholesterol • Mevalonate Synthesis….cont. 2- The next step requires the enzyme βhydroxy-β - methylgularyl-Co.A (HMG-CoA) synthase. This enzyme catalyzes the condensation of a third acetyl-CoA with βketobutyryl-CoA to yield HMG –CoA. 3- HMG-CoA is then reduced to mevalonate by HMG-CoA reductase. The activity of this “reductase’ is primarily responsible for control of the rate of cholesterol biosynthesis. 34 De Novo Synthesis of Cholesterol HMG.Co.A Sythase 35 HMG.Co.A Reductase Biosynthesis of Cholesterol …..cont. • After the Formation of Mevalonate. The biosynthesis of cholesterol (from mevalonate) may be divided into 4 setps. 36 Biosynthesis of Cholesterol……cont. • After the Formation of Mevalonate ……cont. 1. Formation of isoprenoid (isoprene units) ,isopentenyl pyrophosphate (5C) from mevalonate by loss of CO2. 37 2. Condensation of six isoprenoid units form squalene (30C). Cholesterol Synthesis 38 Biosynthesis of Cholesterol…cont. • After the Formation of Mevalonate …….cont. 3. Cyclization of squalene give rise to the parents steroid, lanosterol by cyclase. 4. Formation of cholesterol from lanosterol (30C) by removal of 3 methyl groups. 39 De Novo Synthesis of Cholesterol HMG.Co.A Sythase 40 HMG.Co.A Reductase Cholesterol Synthesis 41 Biosynthesis of Cholesterol …..cont. The Rate-Limitting Step • Cholesterol synthesis is controlled by regulation of the rate of mevalonate. Synthesis, i.e., the synthesis is controlled by regulation of HMG-CoA reductase. 42 HMG.Co.A Reductase 43 The RateLimitting Step in De Novo Synthesis of Cholesterol Biosynthesis of Cholesterol…..cont. The Rate-Limitting Step ……cont. •Therefore HMG-CoA is an important intermediate for the biosynthesis of cholesterol. -The biosynthesis of cholesterol is catalyzed by enzymes in the cytosol and enzymes including HMG – Co.A reductase, bound to the endoplasmic reticulum. 44 Regulation of Cholesterol Synthesis. 1. Dietary Factors: Reduced synthesis of cholesterol during starvation is accompained by a decrease in the activity of the enzyme. Therefore, we can say that hepatic HMGCoA reductase is regulated by some dietary factors. 45 Regulation of Cholesterol Synthesis…..cont. . 2. Feedback Inhibition: HMG-CoA reductase in liver is inhibited by mevalonate, the immediate product of the pathway, and by cholesterol, the main product. • However, it is only hepatic synthesis that is inhibited by dietary cholesterol. • Feedback control of hepatic cholesterogenesis is also mediated, directly or indirectly by bile 46 acids. Regulation of Cholesterol Synthesis By Feed-Back Inhibition of these Substances ( Intermediates) 47 Regulation of Cholesterol Synthesis …..cont. 3. Hormonal Regulation: Both Glucagon and glucocorticoids decrease HMG-CoA reductase activity. 48 Regulation of Cholesterol Synthesis …..cont. 4. Sterol- Mediated regulation of transcription: The synthesis of cholesterol is also regulated by the amount of cholesterol taken up by the cells during lipoprotein metabolism. 49 Regulation of Cholesterol Synthesis……cont. 4. Sterol- Mediated regulation of transcription ……cont. 1) Chylomicron remnants internalized by liver cells, and 2) low density lipoproteins (LDL) internalized by cells of the liver and peripheral tissues, to provide cholesterol, which causes a decrease in transcription of the HMG-CoA reductase gene, leading to a decrease in the de novo synthesis of cholesterol. 50 Regulation of Cholesterol Synthesis….cont. 5. Inhibition by Drugs (statins): Lovastatin and mevastatin are reversible, competitive inhibitors of HMG-CoA reductase, They are used to decrease plasma cholesterol levels in patients with hypercholestrolemia. 51 Cholesterol is Transprted from Intestine to Liver in Lipoproteins • The liver and the gut (intestine) are the two major organs of lipoprotein synthesis and transport. 52 Cholesterol is Transprted from Intestine to Liver in Chylomicrons • Bile salts in the bile help in emulsifying the fats so they can be more easily digested and absorbed in the gut. • Within the epithelial cells of the gut wall, a combination of triglycerides, and cholesterol, and fatty acids are coated with protein to form large lipoproteins known as 53 chylomicrons . Structure of Lipoproteins 54 Structure of Chylomicrons 55 Cholesterol is Transprted from Intestine to Liver in Chylomicrons……cont. Chylomicrons • Chylomicrons are absorbed into the lymphatic system, which eventually drains into the circulation. • Chylomicrons then goes to the liver where they are broken down to contribute to the triglyceride and the cholesterol pool within 56the liver. Cholesterol is Transprted from Liver to Other Body Tissues by VLDL Lipoproteins • The use of cholesterol by the liver is to supply cholesterol for the rest of the body’s needs. • In order to do this, cholesterol from the liver’s pool is combined with triglycerides and coated with a special protein that makes it soluble in our blood. • These rather large molecular weight structures are called very low density lipoproteins (VLDL=Cholestrol+ Cholestryl ester + TG + additional lipids), • VLDL is released from the liver into the circulation 57 to supply the body’s needs for triglycerides and cholesterol. Structure of Lipoproteins: VLDL,IDL,LDL,and HDL 58 How to Utilize Cholesterol ? • The liver’s cholesterol pool, regardless of the source, is used in two major ways. 1. It’s used to form bile salts. 59 Sources of Cholesterol Diet De novo synthesis Cholesterol synthesized in extrahepatic tissues Liver cholesterol pool Secretion of HDL and VLDL 60 Free cholesterol In bile Conversion to bile salts/acids How to Utilize Cholesterol ? • The liver’s cholesterol pool, regardless of the source, is used in two major ways……cont. 2. Exporting cholesterol to extra-hepatic tissues in VLDL lipoproteins. 61 Lipoprotein Lipase • Lipoprotein lipase is an enzyme found throughout the body, with high amounts in the arterial walls. • Lipoprotein lipase helps to strip off triglycerides from the VLDL. • Those triglycerides can be used in various tissues throughout the body. 62 Lipoprotein lipase ……cont. • As triglycerides are removed from the VLDL, the VLDL gets smaller and becomes enriched with a higher percentage of its composition as cholesterol. In this stage the lipoproteins are referred to as intermediate density lipoproteins,(IDL = VLDL- some of TG). • Further removal of triglycerides from IDL enriches the percentage of cholesterol even more, and results in an even more compact molecule called low density lipoprotein (LDL=IDL – all of the TG) 63 The Fate of Unused LDL • The regulated receptors on the liver will help return some of the cholesterol to the liver from unused LDL. . • LDL is the so-called “bad cholesterol” and genetic differences in these regulated receptors can result in the accumulation or large amounts of LDL in the circulation (familial hyper-cholesterolemia). 64 The Fate of Unused LDL 65 HDL Good Cholesterol • Another lipoprotein formed by the liver is called high density lipoprotein (HDL), sometimes referred to as the “good cholesterol.” • High density lipoprotein is formed with very small amounts of cholesterol, small amounts of triglyceride and a special protein coat within the liver that makes it distinct from the VLDL, also formed in the liver. 66 HDL Good Cholesterol…..cont. • The HDL in the circulation acts like a sponge in picking up excess cholesterol from tissues that normally metabolize cholesterol but are receiving more than they can possibly use. • An enzyme important in this process of reverse cholesterol transport is called lecithin-cholesterol acyl transferase. LCAT stimulates reverse cholesterol transport from tissues that have excessive amounts of cholesterol into the HDL molecules 67 Classification of Lipoproteins “Bad” “Good” (non-HDL( 68 Good Vs. Bad Lipoprotein • 69 plasma lipoproteins , there are good and bad forms of lipoproteins in terms of their effect in the formation of atherosclerotic plaque. Hypercholesterolemia Causes Atherosclerosis 70 Maturing HDL • As HDL absorbs cholesterol from many tissues it becomes mature and it returns to the liver. The lipoprotein coat of HDL helps the liver to recognize it, and direct the cholesterol to the liver pool. 71 Cholesterol is Transported by Different Lipoproteins 72 What Happens if Cholesterol Gets High? • Increases the risk of vascular disease…..mainly IHD…. • What are the risk factors of IHD? -Hyperlipidemia ( hypercholesterolemia) -Hypertension. -Diabetes mellitis. -Smoking. - Obesity - +ve family history. 73 HOW TO TREAT HYPERCHOLESTEROLEMIA 74 HOW TO TREAT HYPERCHOLESTEROLEMIA 1) INCREASE YOUR "GOOD" CHOLESTEROL LEVELS: High-density lipoproteins (HDL) or "good" cholesterol, carries bad cholesterol away from the arteries and heart and back to the liver where it can be used by the body. Replacing saturated fats with mono- or poly- unsaturated fats found in nuts and vegetable oils will help raise HDL levels. 75 HOW TO TREAT HYPERCHLESTLEMIA ….Cont. 2) MAINTAIN A HEALTHY BODY WEIGHT: Individuals who are overweight should aim to decrease their weight with regular physical activity and a balanced, healthy diet. Weight management and cholesterol control go hand in hand. 76 HOW TO TREAT HYPERCHOLESTEROLEMIA ….Cont. 3) EAT A DIET HIGH IN FIBER: Fiber binds to excess cholesterol in the intestine and removes it from the body. Soluble fiber found in oatmeal and whole grains can help to control cholesterol levels. 77 Cholesterol Metabolism - Biological functions: • Because of the well established positive association between plasma cholesterol concentration and coronary heat disease (CHD), it may be thought that of cholesterol as a harmful substance. 78 Biological Functions of Cholesterol …..cont. - Cholesterol is essential for normal functioning of the organism because it is: 1. An essential structural component of the membranes of all animal cells and sub -cellular particles. 79 Biological Functions of Cholesterol …..cont. I- Cholesterol increases the fluidity of plasma membranes. II. It is required to establish proper membrane permeability, it reduces the permeability of plasma membrane to H+ and Na+ 80 Biological Functions of Cholesterol …...cont. 2. An obligatory precursor of bile acids. • In the liver, cholesterol is converted to bile. Bile contain bile salts which solubilize fats in the digestive tract and aid in the intestinal absorption of fat molecules as well as fat soluble vitamins: Vitamin A, Vitamin D, Vitamin E and Vitamin K. 81 Biological Functions of Cholesterol …...cont. 3. A precursor of all steroid hormones : I) Sex hormones: progesterone, estrogens, and testosterone and their derivatives. II) Adrenal gland hormones : cortisol and aldesteron. 82 Sex Hormones Derived from Cholesterol 83 Adrenal Gland Hormones 84 Cholesterol Catabolism - The ring structure of cholesterol cannot be metabolized to CO2 and H2O in humans. 85 Cholesterol Catabolism • After cholesterol enters the cell, the esters are hydrolyzed by the action of specific lysosomal esterases. The lack or malfunction of these lysosomal enzymes results in intracellular accumulation of cholesteryl esters and produces a clinical disorder known as cholesteryl ester storage disease. 86 Cholesterol Recycling And Excretion • Cholesterol is oxidized by the liver into a variety of bile acids (about 30 / d). The bile acid synthesis rate average 200-400mg /d. • These in turn are conjugated with glycine, taurine, glucuronic acid, or sulfate. A mixture of conjugated and non-conjugated bile acids along with cholesterol itself is excreted from the liver into the bile. Approximately 95% of the bile acids are reabsorbed from the intestines and the remainder lost in the feces.[ 87 Cholesterol Recycling And Excretion • The excretion and reabsorption of bile acids forms the basis of the enterohepatic circulation which is essential for the digestion and absorption of dietary fats. • Under certain circumstances, when more cholesterol is concentrated, as in the gallbladder, cholesterol crystallises and is the major constitute of most gallstones. 88 Principle of the Test. -In this experiment cholesterol is estimated by a chemical method rather than an enzymatic method. -This method is qualitative and quantitative one. 89 Principle of the Test …..cont. - In this method: Cholesterol reacts as a typical alcohol with strong, concentrated acid. The products are green-colored substances, mainly cholestapolyenes and cholestapolyene carbonium ions (Liebermann – Burchard reaction) 90 Principle of the Test ….cont. -In this procedure cholesterol reacts with : 1. Acetic acid and acetic anhydride which act as solvents and dehydrating agents. 2. Sulfuric acid that used as a dehydrating and oxidizing reagent. - The absorbance of the green compound is then measured at 610nm. 91 Materials 1. Cholesterol reagent (Acetic anhydride + acetic acid) 2. Sulphuric acid 95-97% 3. Standard cholesterol (300 mg/dl) 4. Samples 5. Test Tubes 6. Pipettes 7. Cuvettes 8. Spectrophotometer 9. Water bath 92 Method 1- Label 7 test tubes for test 1(A,B)test 2 (C,D) standard (E,F) and blank (O) pipette the following Sample 1 (A,B) 0.1 ml Sample 2 (C,D) 93 (B) 0.1 ml Standard Cholesterol Distilled Water Cholesterol 4 ml reagent (E,F) 0.1 ml 0.1 ml 4 ml 4 ml 4ml Method ……cont. 2- Stand for 20 minutes 3- Pipette 1.0 ml of sulphuric acid into each tube running the acid cautiously down the side of the tube. 4- Place the tube in a water bath at room temperature. 5- After around 5 minutes remove from the water bath and shake vigorously to remove any adhered proteins to the walls of the tubes, 6- Stand for 10 minutes then measure the absorbance of the samples against the blank at 610nm. 94 Results Absorbance of samples X 300 = ----------- mg/dl Absorbance of standard 95 Results Sample 1 A= B= mg/dl mg/dl Sample 2 C= D= mg/dl mg/dl Standard cholesterol E= F= 96 mg / dl mg/dl