* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download PowerPoint Presentation - Anticoagulants and Thrombolytics
Drug discovery wikipedia , lookup
Plateau principle wikipedia , lookup
Pharmacognosy wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Intravenous therapy wikipedia , lookup
Prescription costs wikipedia , lookup
Psychopharmacology wikipedia , lookup
Prescription drug prices in the United States wikipedia , lookup
Pharmacokinetics wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Neuropharmacology wikipedia , lookup
Drug interaction wikipedia , lookup
Discovery and development of direct Xa inhibitors wikipedia , lookup
Discovery and development of direct thrombin inhibitors wikipedia , lookup
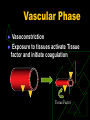
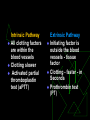
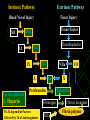
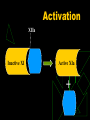
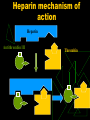
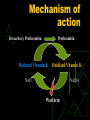
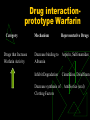
Anticoagulants and Thrombolytics S. Ramakrishnan Objectives To learn how Blood Clots are formed. How the blood clots are broken down ? What drugs can be used to regulate clotting ? How to rectify clotting deficiencies Blood clots - Thrombus Thrombus dislodge from arteries and veins and become an embolus. Venous emboli can block arterioles in the lung and pulmonary circulation Thromboembolism Classes of Drugs Prevent coagulation Dissolve clots Prevent bleeding and hemorrhage Hemostatic Overcome clotting deficiencies ( replacement therapies) Blood Clotting Vascular Phase Platelet Phase Coagulation Phase Fibrinolytic Phase Vascular Phase Vasoconstriction Exposure to tissues activate Tissue factor and initiate coagulation Tissue Factor Platelet phase Non-nucleated - arise from magakaryocytes blood vessel wall (endothelial cells) prevent platelet adhesion and aggregation platelets contain receptors for fibrinogen and von Willebrand factor after vessel injury Platelets adhere and aggregate. Release permeability increasing factors (e.g. vascular permeability factor, VPF) Loose their membrane and form a viscous plug Platelets and Thromboemolism Arteries : White Thrombus Platelets adhere Release ADP More adhesion/ aggregation Reduced blood flow (stasis) Fibrin clot Veins low pressure : Red thrombus is formed Especially in valve pockets Contains a long tail of fibrin Can detach and form emboli Coagulation Phase Two major pathways Intrinsic pathway Extrinsic pathway Both converge at a common point 13 soluble factors are involved in clotting Biosynthesis of these factors are dependent on Vitamin K1 and K2 Most of these factors are proteases Normally inactive and sequentially activated Hereditary lack of clotting factors lead to hemophilia -A Intrinsic Pathway All clotting factors are within the blood vessels Clotting slower Activated partial thromboplastin test (aPTT) Extrinsic Pathway Initiating factor is outside the blood vessels - tissue factor Clotting - faster - in Seconds Prothrombin test (PT) Prothrombin time (PT) Tissue Thromboplastin factor III Mix with phospholipid extract Add calcium and blood sample Determine clotting time Generally 12 - 14 seconds Used to detect defects in extrinsic pathway Activated partial thromboplastin time (APTT) Blood sample + EDTA or Citrate No clot ( recalcification will result in clot in about 2 - 4 min) Add calcium Mix with negatively charged phospholipid Kaoline (aluminum silicate) Determine clotting time Generally clotting occurs in 26 to 33 seconds Used to detect defects in the intrinsic pathway Diagnosis of coagulation defects Prolonged APTT No change in PT Defective Intrinsic Pathway No change in APTT Prolonged PT Defective Extrinsic Pathway Prolonged APTT Prolonged PT Defective in Common pathway Intrinsic Pathway Extrinsic Pathway Tissue Injury Blood Vessel Injury Tissue Factor XIIa XII Thromboplastin XIa XI IXa IX Xa X Factors affected By Heparin VIIa Prothrombin Vit. K dependent Factors Affected by Oral Anticoagulants Fibrinogen XIII VII X Thrombin Fribrin monomer Fibrin polymer Activation XIIa Inactive XI Active XIa + Thrombosis Arterial Thrombosis : Adherence of platelets to arterial walls - White in color - Often associated with MI, stroke and ischemia Venous Thrombosis : Develops in areas of stagnated blood flow (deep vein thrombosis), Red in color- Associated with Congestive Heart Failure, Cancer, Surgery. Anticoagulant drugs to treat thromboembolism Drug Class Anticoagulant Parenteral Prototype Heparin Action Inactivation of clotting Factors Effect Prevent venous Thrombosis Anticoagulant Warfarin Decrease synthesis of Oral Clotting factors Prevent venous Thrombosis Antiplatelet drugs Aspirin Prevent arterial Thrombosis Thrombolytic Drugs Streptokinase Fibinolysis Decrease platelet aggregation Breakdown of thrombi Heparin Sulphated carbohydrate Purified from bovine lungs Different size Active in vitro and in vivo Administration - parenteral- Do not inject IM only IV or deep s.c. Half-life 1 - 5 hrs - monitor aPTT Adverse effect - hemorrhage - antidote protamine sulphate Heparin mechanism of action Heparin Antithrombin III Thrombin Oral anticoagulants : warfarin, dicumarol Coumarins - warfarin, dicumarol Isolated from clover leaves Structurally related to vitamin K Inhibits production of active clotting factors Absorption rapid - binds to albumin Clearance is slow - 36 hrs Delayed onset 8 - 12 hrs Overdose - reversed by vitamin K infusion Can cross placenta - do not use during late pregnancies Mechanism of action Descarboxy Prothrombin Prothrombin Reduced Vitamin K Oxidized Vitamin K NAD NADH Warfarin Antiplatelet drugs Aspirin Prevents platelet aggregation /adhesion Clinical use - prevents arterial thrombus Myocardial infarction (MI), stroke, heart valve replacement and shunts Other antiplatelet drugs are - Dipyridamole, sulfinpyrazone and Ticlopidine Mechanism of action Aspirin inhibits cyclooxygenase (COX) COX is a key enzyme involved in the synthesis of thromboxane 2 (prostaglandins) Inhibits platelet aggregation Prophylactic use of Aspirin Low dose daily ( 180 mg/day) Prevents ischemic attack (ministroke) and MI 335 mg/day reduced the risk of heart attack in patients over 50 More than 1000 mg/day NO EFFECT High dose inhibits prostacyclin synthesis in cells surrounding vessels. PS normally prevents platelet aggregation. Therefore, inhibition of PS leads to abrogation of the prophylactic benefit of Aspirin Contraindication - DO NOT give to patients with glucose 6-PO4 dehydrogenase deficiency Drug interactionprototype Warfarin Category Drugs that Increase Warfarin Activity Mechanism Representative Drugs Decrease binding to Albumin Aspirin, Sulfonamides Inhibit Degradation Cimetidine, Disulfiram Decrease synthesis of Clotting Factors Antibiotics (oral) Drug interactionprototype Warfarin Drugs that promote bleeding Drugs that decrease Warfarin activity Inhibition of platelets Aspirin Inhibition of clotting Factors heparin antimetabolites Induction of metabolizing Enzymes Barbiturates Phenytoin Promote clotting factor Synthesis Reduced absorption Vitamin K OC cholestyramine colestipol Fibrinolysis Enhance degradation of clots Activation of endogenous protease Plasminogen (inactive form) is converted to Plasmin (active form) Plasmin breaks down fibrin clots Fibrinolysis Exogenously administered drugs Streptokinase - bacterial product - continuous use - immune reaction Urokinase - human tissue derived - no immune response Tissue plasminogen activator (tPA) - genetically cloned - no immune reaction - EXPENSIVE Inhibitors of fibrinolysis - aminocaproic acid Lysine analog- inhibits proteases Drug preparations : To reduce clotting Heparin Parenteral - 1000 - 40,000 U/ml Warfarin (generic , Coumadin) (generic, Liquaemin sodium) Oral : 2 - 20 mg tablets Dipyridamole (Persantine) Oral : 25,50,75 mg tablets Drug preparations : to lyse clots Alteplase recombinant (tPA, Activase) streptokinase (Kabikinase, streptase) 20, 50 mg Lyophilized powder - reconstitute for iv Parenteral : 250000 - 1.5 million units per vial . Lyophilized powder. Reconstitute for iv Urokinase ( Abbokinase) Parenteral : 250000 units per vial. Powder to reconstitute to 5000 u/ml for injection Drug preparations : clotting deficiencies Vitamin K ( Phytonadione (K1), Mephyton Plasma fractions - for hemophilia Antihemophilic factor ( VIII, AHF) Parenteral Factor IX complex (konyne HT, proplex T) Oral : 5 mg tablets Parenteral : in vials Due to HIV risks in blood products recombinant proteins of the factors are made. E.g. transgenic goats secreting factors into milk Drug preparations : to stop bleeding Systemic use : aminocaproic acid (Amicar); Tranexamic acid (cyclokapron),Vitamin K Local adsorbable drugs Gelatin sponge (Gelfoam) Gelatin film Oxidized cellulose ( Oxycel) Microfibrillar collagen (Avitene) Thrombin