* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Slide 1
Urinary tract infection wikipedia , lookup
Childhood immunizations in the United States wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Common cold wikipedia , lookup
Hepatitis C wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Psychoneuroimmunology wikipedia , lookup
Innate immune system wikipedia , lookup
Sjögren syndrome wikipedia , lookup
Schistosomiasis wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Hepatitis B wikipedia , lookup
Neonatal infection wikipedia , lookup
Infection control wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
X-linked severe combined immunodeficiency wikipedia , lookup
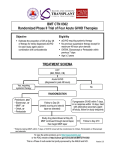
NCCS Web Conference 3/23/11 Angela Smith, MD, MS Outline the etiology and management of stem cell transplant (SCT) complications that may early post transplant setting. Brief History and Overview of SCT Potential Acute SCT Complications : Mucositis Veno-occlusive Disease (VOD) Pulmonary Hemorrhage Graft-versus-Host Disease (GVHD) Infection First successful related allogeneic bone marrow transplant was performed at the University of Minnesota in 1968. Since then, we have performed thousands of transplants and have pioneered many novel therapies: Umbilical cord blood transplants Transplant for metabolic disorders Delivery of high-dose chemotherapy +/radiation therapy to obliterate the bone marrow and suppress the recipient’s immune system. Replacement of the abnormally functioning bone marrow (or bone marrow derived) cells with healthy hematopoietic cells. Overall Goals: Eradicate any leukemic/cancer cells. Ablate the bone marrow and create space for donor cells. Suppress the recipients immune system to prevent rejection and GVHD. Augment the anti-tumor response. (graft-versusleukemia or graft-versus-tumor) Following transplant, the recipient immune and blood-forming cell systems are repopulated by normal donor-derived cells, all of which are thought to derive from a common primitive pluripotent stem cell. The stem cell is self-renewing and thus provides a sustained source of its own cell population. The recipient becomes a “chimera” (a mythical Greek beast that is part lion, part goat and part snake) – an individual whose blood cells are of foreign origin. Circulating RBC’s, platelets, leukocytes, lymphocytes, monocyte/macrophage derived cells (ex: osteoclasts, Kupffer cells, pulmonary alveolar macrophages) and perhaps some glial cell populations become donor in type. Neoplastic diseases – AML, ALL, CML, MDS, lymphoma, neuroblastoma, other solid tumors. Hematopoietic disorders – aplastic anemia, Dyskeratosis Congenita, Fanconi anemia, PNH, DBA, SDS, HLH, thalassemia, SCD. Immunodeficiency states – SCID and related disorders, Wiskott-Aldrich, CVID. Genetic diseases – In these cases, HCT provides a normally functioning cell and/or a cellular source for the deficient enzyme/protein. Mucopolysaccharidoses/Mucolipidoses (Hurler syndrome) Osteopetrosis Adrenoleukodystrophy Dystrophic Epidermolysis bullosa collagen type VII (major component of the basement membrane anchoring fibrils; made and secreted by keratinocytes and fibroblasts) Ultimate SCT outcome depends on many variables: Underlying disease and it’s remission status Health and age of the recipient Conditioning intensity Type of donor cells used Development of GVHD Despite advances in therapy and supportive care measures, transplant related complications remain a major cause of morbidity and mortality. Acute phase – first 100 days post SCT. 3 year male day +5 s/p matched sibling donor (MSD) transplant for ALL. Conditioning regimen: cytoxan, total body irradiation. GVHD prophylaxis: CSA, methotrexate. Mouth sores started on day +1 and have worsened. Increasing oxygen requirement for last 24 hours. Now with drooling, upper airway stridor, retractions, pCO2=75, sats 88% on 100% O2 via facemask. Inflammation and denudation of the mucous membranes. Caused by chemotherapy, radiation and neutropenia. Severity depends on many factors: Occurs throughout the GI tract mouth to anus. Patient age, type of conditioning, GVH prophylaxis, etc. Allows a portal of entry for bacteria. Symptomatic Cares – bowel rest, pain control with narcotics, platelet transfusion if bleeding. Mouth Cares – helps prevent infection. Airway management – may need intubation to protect the airway until swelling/sloughing resolve. Can be a difficult intubation as landmarks often hard to identify. More commonly presents with airway obstruction in small children. More severe in patients receiving methotrexate for GVHD prophy. Increased risk of infections with oral flora need anaerobic antibiotic coverage if febrile. Resolves with count recovery. 2 year old male day +7 s/p UCBT for HLH Conditioning regimen: busulfan, cytoxan, ATG GVHD Prophy: CSA, MMF Progressive fluid retention – gained 2 kg. Abdominal distention/pain with increasing hepatomegaly and RUQ pain. Creatinine has tripled in the last 2 days, UOP slowing despite diuretics. New O2 requirement. Abdominal U/S – hepatomegaly, gallbladder sludge, moderate ascites. Increased resistive indices in the portal vessels, but flow is anterograde. AKA Sinusoidal Obstruction Syndrome (SOS) Blockage of small intrahepatic veins by loose connective tissue, fibrinogen and F VIII resulting on post-sinusoidal obstruction and intrahepatic portal hypertension. Cause is unknown – likely sinusoidal endothelial injury from chemo/radiation local hypercoaguable state progressive occlusion of the hepatic venous outflow clinical manifestations. Typically occurs within 3 weeks of SCT. Diagnosis CLINICAL Abdominal U/S with doppler sometimes helpful. Liver biopsy rarely indicated. Severity Spectrum: mild severe (progressive) Mild = very common, easily treatable, mortality 3%. Severe = life-threatening, difficult to treat, mortality up to 98%! Death typically from renal and/or cardiopulmonary failure. Aggressive Fluid Management – diuretics +/colloid. Ursodiol – to prevent cholestasis, more for prophy. ATIII – only if deficient. NO systemic heparin – still used in some centers, but carries a very real risk of lifethreatening bleeding. Defibrotide – **not currently FDA approved, clinical trial is open** Large, single-stranded polydeoxyribonucleotide Anti-thrombotic, anti-ischemic, anti-inflammatory and thrombolytic effects without significant systemic anticoagulant effects. Complex mechanism of action. Well-tolerated with few SE’s (1-9%) Flushing, nausea, abdominal discomfort. Hypotension Bleeding (rare) Identifying and treating VOD early is KEY!! Life-threatening if severe. Can cause progressive renal and respiratory failure. May require intubation secondary to abdominal distention and/or pulmonary edema. May lead to renal failure requiring hemodialysis. If using defibrotide to treat, remember that there is a risk of bleeding and hypotension with the drug. If either is significant and/or life-threatening, defibrotide must be held. Keep platelets >30K and INR <1.5 16 year old male day +10 s/p matched unrelated donor (MURD) BMT for Dyskeratosis Congenita. Conditioning Regimen: campath, cytoxan, fludarabine, TBI GVHD Prophy: CSA, MMF Progressive O2 requirement and respiratory distress. CXR with new bilateral patchy infiltrates. CXR -- Extensive bilateral diffuse pulmonary consolidation with sparing of the periphery of the lungs. BAL – Frank blood in the airway that doesn’t clear with lavage. Diagnosis: Respiratory distress/failure, CXR findings, bloody BAL fluid. Etiology: Multifactorial Thrombocytopenia/Coagulopathy Endothelial injury Vasculitis ?GVHD Neutrophil influx into the lung Infection Risk Factors: Intensive chemotherapy Thoracic radiation and/or TBI Pulmonary infection Underlying disease – Hurler’s, dyskeratosis congenita Incidence 1-21%, Mortality >60%. Maintain Airway – usually requires intubation and frequent suctioning. Control Bleeding: Keep platelets ≥ 50-100K activated Factor VII (90mcg/kg x 1-2 doses) Methylprednisone (0.5-2g/day) – careful is infection is suspected. +/- DDAVP (0.3mcg/kg/day x 3 doses) Certain patients are more likely to have hemorrhage: Hurler’s, Dyskeratosis Congenita, h/o fungal/viral lung infection. Treat EARLY and aggressively! 10 year female day +33 s/p 1 antigen mismatched (i.e. 7/8) URD transplant for AML. Conditioning Regimen: cytoxan, TBI GVHD Prophy: CSA, MMF No major complications. Engrafted on day +20, transitioning to oral CSA, but some difficulty tolerating the pills. New red, maculopapular rash covering 75% of her body and involving the palms/soles. No desquamation. Also with 1 liter dark, watery stool output in the last 24 hours. No blood. Immune competent donor T cells attack recipient epithelial tissues. Common targets: skin, gut, liver 3 stages 1) Injury to the host environment results in release proinflammatory cytokines. 2) Donor T-cell activation, proliferation, and differentiation. 3) Cellular and inflammatory attack on host tissues. Incidence: 30 - 50% MSD recipients 50 - 70% URD recipients 30% single UCBT recipients 60% double UCBT (increase grade II) Donor source HLA disparity Sex mismatch Parity Older age CMV status compared to recipient Source – PBSC > BM, double UCB > single UCB Cell dose, T cell depletion Recipient factors Older age CMV positive serostatus Previous SCT Use of TBI Most commonly involved organ. Maculopapular rash, +/- pruritic/painful. May have epidermal necrosis and/or bullae. DDx: drug allergy, viral exanthem, SJS, chemoradiotherapy effect. Dx: Biopsy Diffuse erythroderma with desquamation Blister Formation Patients with stage IV skin GVHD are best treated like a burn patient. Pay meticulous attention to skin and wound care, nutrition, and infection control. Lower GI disease: profuse, watery diarrhea; crampy abdominal pain. Grade IV = intestinal bleeding, ileus. Upper GI disease: anorexia, intractable nausea/vomiting. DDx: chemoradiotherapy effects, mucositis, infection (c.diff, CMV, adeno) Dx: Biopsy Potential Issues: Fluid Management Fluid and protein losses often hard to keep up with. Need accurate recording of stool output. Replace stool output. Bleeding Keep platelets 50-100K. Correct coagulopathy. Concomitant Infection CMV common. Least common, hardly ever seen in the absence of skin/gut involvement. SSx: cholestatic jaundice. DDx: hepatic VOD, infection, drug toxicity (CSA, etc) Supportive cares as previously outlined Immune Suppression depends on grade of aGVHD ALL patients receive prophylaxis. CSA weekly levels, goal 200-400. MTX or MMF or steroids Prophylaxis MTX/MMF/MP + CSA Mild GVHD Moderate Severe CSA CSA CSA Topical Steroids Topical Steroids Topical Steroids Prednisone High Dose MP ATG Steroid Taper Skin > Gut >>> Liver Commonly occurs between days 30-60 post SCT. Extreme susceptibility to INFECTION!! Infection is the major cause of death in patients with GVHD. Treated with increased immune suppression. 16 year old male day +22 s/p UCBT for relapsed AML. Conditioning regimen: cytoxan, fludarabine, TBI GVHD prophy: CSA, MMF Persistent fevers with acute onset of hypotension, respiratory distress and coagulopathy. Not yet engrafted (WBC < 0.1). Presentation of infections in the post SCT setting are unique. Quick onset Severe and often prolonged course Serious infections often occur with “common, benign” organisms. Line Infections – CONS, alpha-hemolytic strep. Pneumonia Sepsis/DIC – gram negative rods **Especially common in those receiving ATG or Campath** CMV – pneumonitis, colitis, retinitis EBV – PTLD, mono-like illness Adeno – diarrhea, pneumonitis, colitis, liver failure HHV-6 – rash, marrow suppression, graft failure, pneumonitis, encephalitis HSV – stomatitis VZV – zoster, pneumonitis Influenza/RSV – pneumonia Candida spp Aspergillus spp Other – Rhizopus, Mucor, Histoplasma, Blastomycoses. Frequent monitoring – culture with fevers, follow viral DNA PCR’s. Aggressive antibiotics/antivirals/antifungals. Supportive care – mechanical ventilation, pressors, fluids, IVIG. If documented fungal infection prior to engraftment, consider granulocyte infusions. **Regardless of whether or not an infection documented, if fever is present, antimicrobials will be continued until engraftment and resolution of fever** Antifungals (until day +100) Fluconazole – Routine risk patients Voriconazole – High risk patients SAA, FA, AML/MDS Levaquin – Streptococcus HEPA filtered air systems/laminar airflow rooms, isolation rooms Hand washing, oral hygiene Onset, severity and duration of infections in immune compromised patients are unique. Patients receiving ATG or Campath are at very high risk for viral infections (early and late). Heavily pre-treated patients (AML) and those who had prolonged neutropenia prior to SCT (FA, SAA, MDS) are at very high risk for fungal infections. Prophylaxis, pre-emptive therapy and early treatment are key!