* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Nutrition Therapy for Diabetes Mellitus (DM)
Malnutrition wikipedia , lookup
Calorie restriction wikipedia , lookup
Waist–hip ratio wikipedia , lookup
Body mass index wikipedia , lookup
Oral rehydration therapy wikipedia , lookup
Fat acceptance movement wikipedia , lookup
Low-carbohydrate diet wikipedia , lookup
Body fat percentage wikipedia , lookup
Adipose tissue wikipedia , lookup
Obesity and the environment wikipedia , lookup
Abdominal obesity wikipedia , lookup
Cigarette smoking for weight loss wikipedia , lookup
Saturated fat and cardiovascular disease wikipedia , lookup
Gastric bypass surgery wikipedia , lookup
Diet-induced obesity model wikipedia , lookup
Human nutrition wikipedia , lookup
Overeaters Anonymous wikipedia , lookup
Food choice wikipedia , lookup
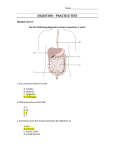
Nutrition Outline Exam 2 Lecture 3: Digestion, Absorption and Malabsorption • • • Gastrointestinal tract (GIT) is designed to – Digest carbohydrates, proteins, fats and beverages – Absorb fluids, micronutrients, and trace elements – Provide immunological barrier to microorganisms, foreign material and potential antigens consumed with food or formed during the digestive process One of the largest organs, has the greatest surface area, largest # of immune cells and is very metabolically active Cells lining the small intestines (45%) and colon (70%) are supplied by nutrients passing thru lumen and have a 3 to 5 day life span – Even after a few days of reduced/no food or beverage intake, the GIT atrophies (decrease in surface area, decrease in secretions, decrease in blood flow and synthetic functions decrease Secretions GIT secretions contribute 7 to 9 L of fluid in a day from 5 different organs: salivary glands, stomach, intestines, pancreas and liver (via gallbladder) -All but 100 to 150 mL of the fluid entering the lumen is reabsorbed Movement Peristalsis Inner circular muscles contract, tightening the tube, pushing the food forward in the intestines. When the circular muscles relax, the longitudinal muscles contract (opposing action). As these muscles contract and relax, the chyme moves ahead of the contraction. Segmentation Circular muscles contract creating segments within the intestines, As each set of circular muscles contract and relax, the chyme is broken up and mixed with digestive juices/enzymes. These contractions occur 12 to 16 times/minute. Mouth • Mastication of food grinds and crushed food into small particles and simultaneously moistened and lubricated by saliva • 3 pairs salivary glands produce ~ 1.5 L saliva/day • Salivary amylase (ptylin) begins digestion of starch (minimal) • Lingual lipase digests small amount of fat (predominant in infants) • Mucus helps particles stick together and lubricates the mass for swallowing • Food mass is passed back to the pharynx under voluntary control • Peristalsis moves food rapidly to the stomach under involuntary control Stomach • Extends from the lower esophageal sphincter to the pyloric sphincter • Volume at rest: ~50 mL (~2 oz); Expanded: 1.5 L (~37 – 52 oz) • Secretion 2 to 2.5 Liters of gastric juice daily – hydrochloric acid from the parietal cells – pepsinogen and gastric lipase from chief cells – Intrinsic factor a glycoprotein from parietal cells – mucus – Gastrin (hormone) • Holds food for 2-4 hours – dependent on concentration and type of macronutrients consumed • Results in the formation of chyme Small Intestine • Primary site for digestion and absorption, divided into: – Duodenum - ~0.5 Meters long – Jejunum - ~2 to 3 Meters long – Ileum -~ 3 to 4 Meters long • Acidic chyme enters duodenum from stomach is mixed with duodenal juices and the secretions from the pancreas and biliary tract resulting in an increase in pH and acidic chyme is neutralized • Release of several hormones that stimulate the secretion of enzymes and fluids and affect GI motility and satiety Small Intestine: Bile Metabolism • Bile which is composed mainly bile acids, cholesterol, phospholipids, bile pigments (bilirubin & biliverdin) dissolved in alkaline solution • Two main bile acids (referred to as the primary bile acids) are: – Chenodeoxycholic acid & cholic acid which can be conjugated (amide bonds) with either glycine or taurine – Most of the conjugated bile acids are present as bile salts with Na+ being the prominent biliary cation • Bile facilitates the digestion and absorption of lipids, cholesterol and fat-soluble vitamins via their surfactant properties • Conjugation improves ionization and ability to form micelles. Glycine (75%), Taurine (25%) • When the concentration of bile salts reached a certain level they form micelles (aggregates of monoglycerides, fatty acids, cholesterol, phospholipids, bile salts and other lipids) which are amphipatic molecules (polar ends of the molecules pointing into the lumen • The products of lipid digestion are solubilized in the central portion of the micelle and carried to the intestinal brush border • 95% of bile salts secreted by liver and gallbladder are reabsorbed in the distal ileum (enterohepatic circulation) and recycled by the liver Large Intestines • 1.5 m long: cecum, colon, and rectum • Nutrients formed here: vitamin K, vitamin B12, thiamin, riboflavin • Site of bacterial fermentation of any remaining carbohydrate and fiber to produce short-chain fatty acids (butyrate, proprionate, acetate and lactate) and gases (e.g. H2, CO2, CH4) • Short-chain fatty acids serve as fuel and stimulate proliferation of cells, reduce osmolality and enhance absorption of Na+ and water • Water reabsorption – ~ 1 to 1.5 Liters fluid enters the large intestines and ~ 100 mL remains to be excreted in feces – Feces generally consists of 75% solids and 25% water Absorption Carbohydrate Amino Acid • End products of protein digestion are absorbed as both amino acids and small peptides • Several transport molecules are required for different amino acids, some are sodium- or chloride- dependent, some are not Lipids • Normally, 95% to 97% of ingested fat is absorbed into lymph vessels • Small and medium-chained fatty acids (8-10 C) do not require bile for absorption and can go directly without esterification into the portal vein Vitamins and Minerals • Fat-soluble vitamins are absorbed via micelles, water-soluble forms of vitamins A, E, and K supplements can be absorbed in the absence of bile acids • Some water-soluble vitamins use passive and facilitative diffusion • B12-Intrinsic Factor complex requires intrinsic factor receptor in the distal ileum for absorption of B12 • Mineral absorption is more complex, particularly for the cation minerals which are usually chelated to a ligand, usually an acid, organic acid or amino acid so it is in a form that is absorbable by intestinal cells • Iron and zinc absorption depends on the needs of the host • Animal sources better absorbed than plant sources because of the interactions with the phytates and oxalates present in plant-based foods • Zinc absorption is impaired with increased amounts of calcium, magnesium and iron • Calcium absorption is regulated by vitamin D • Cobalt absorption is increased in people with iron deficiency but compete and inhibit one another’s absorption • Supplemental amounts of iron or zinc can decrease absorption of copper Major GI Hormones • Gastrin: released from G cells in the pyloric region of stomach in response to thoughts of food, food, distension of the antrum, peptides and amino acids, caffeine and vagus nerve – Stimulates release of HCl and pepsinogen • Secretin: released from proximal duodenum in response to acidic chyme – Stimulates release of water and bicarbonate from pancreas, • Cholecystokinin (CCK): released from proximal duodenum in response to HCl, peptides and amino acids. Stimulates secretion of pancreatic enzymes, contraction of the gallbladder • GIP (Glucose-dependent insulinotrophic polypeptide) and GLP-1 (Gucagon-like polypeptide) secreted by the intestinal mucosa are called incretin hormones because they help lower blood glucose levels – GIP stimulates insulin release – GLP-1 stimulates insulin release, inhibits glucagon release • Motilin released duodenal mucosa - Promotes gastric emptying and GI motility • Somatostatin released by D cells of the antrum and pylorus - Primary roles are inhibitory and antisecretory Malabsorption Syndromes • Malabsorption disorders are most detrimental to nutrition status – Nutrient deficiencies – multiple, Weight loss, Serious complications • Disorders associated with malabsorption – Genetic disorders e.g. Celiac disease, Crohn’s disease – Pancreatic disorders e.g. pancreatic insufficiency, Cystic Fibrosis – Intestinal disorders e.g. Ulcerative colitis – Intestinal infections e.g. Clostridium difficile – Liver disease (bile insufficiency) – Surgeries • Rarely involves single nutrient • Treatment of malabsorption disorders may also stress nutritional status Diarrhea • Exudative diarrhea always associated with mucosal damage – Mucus, fluid, blood, plasma proteins, electrolytes and water – Often seen in Crohn’s disease, ulcerative colitis and radiation enteritis • Osmotic diarrhea caused by poor absorbance of osmotically active solutes present in the intestinal tract. Dumping syndrome, Lactose intolerance. Resolves with fasting • Secretory diarrhea is the result of active intestinal secretion of electrolytes and water by intestinal epithelium – Bacterial exotoxins, viruses, increased intestinal hormone secretion – Does not resolve with fasting • • Malabsorptive diarrhea occurs when disease process impairs digestion and absorption with fat and other nutrients appear in the stool in increased amounts – Insufficient healthy absorptive area, decreased bile, decreased pancreatic enzymes or rapid transit Medication-induced diarrhea common in hospital and long-term care patients – Lactulose – used in management of treatment in hepatic encephalopathy – Sodium-polystyrene sulfonate with sorbitol – treat hyperkalemia – Antibiotic-associated diarrhea… Clostridium difficle most common Tx of Diarrhea • Because diarrhea is a symptom not a disease, first identify and treat underlying disorder • Manage fluid and electrolyte balance – sometimes a first priority – Oral rehydration solutions contain glucose, sodium, potassium – In retractable diarrhea, parenteral feeding may be required especially if patient is not expected to resume full oral intake within 5 to 7 days • Possible supplementation with probiotics – Lactobacillus, bifidobacteria and Saccharomyces boulardii (yogurt and kefir) • Soups, broths, vegetable juices, isotonic liquids – BRAT diet (bananas, rice, applesauce, toast) – nutrient poor Evaluating Malabsorption: Laboratory tests to determine malabsorption problems • D-xylose test: used to differentiate intestinal malabsorption from digestive pancreatic disorders • Hydrogen breath test: used to diagnose lactose intolerance & malabsorption of other carbohydrates • Schilling test: used to diagnose malabsorption of vitamin B12; further testing determines whether vitamin B12 malabsorption is caused by intrinsic factor deficiency or pancreatic enzyme insufficiency • Fecal fat test: detects excessive fat in the stool (steatorrhea = > 7g/day) Fat Malabsorption Causes • Illness that interferes with production or secretion of bile (severe liver disease) or pancreatic lipase (pancreatitis, cystic fibrosis) • Damage to intestinal mucosa (inflammatory disorders or radiation treatments) • Motility disorders causing rapid gastric emptying or intestinal transit Consequences: losses of food energy, essential fatty acids, fat-soluble vitamins, some minerals • Weight loss, Deficiencies of fat-soluble vitamins, Formation of soaps by some minerals & unabsorbed fatty acids, Bone loss from calcium deficiency, Increased risk of renal oxalate stones Dietary adjustments: fat-restricted diet – Relief of abdominal symptoms (diarrhea & flatulence) – Minimize loss of vitamins & minerals – Fats should not be restricted more than necessary – Alternative source of dietary fat: medium-chain triglycerides (MCT) • MCT do not require digestion by lipases or bile Celiac Disease • Celiac Disease AKA Gluten-Sensitive Enteropathy : Affects 1 in 133 people, any age, peak 40-60’s • Characterized by 4 factors: – Genetic susceptibility – Exposure to gluten: prolamines (glutenin and gliadin) found in wheat, rye, barley (oats) – Environmental “trigger” – stress, inflammation etc. – Autoimmune response – prolamines travel across intestinal epithelium into lamina propria and can trigger a response that atrophies and flattens the intestinal villi (clubbing) • Often affects the proximal and middle sections of small intestines • Children present with more GI symptoms (diarrhea, steatorrhea, bloating) poor weight gain • Frequently misdiagnosed as irritable bowel syndrome (IBS), lactase deficiency, gallbladder disease • Intestinal mucosa damage: Malabsorption of nutrients, anemia, osteoporosis, vitamin or mineral deficiencies, dermatitis hepetiformis (itchy skin rash) • Gluten intolerance: individuals who have symptoms and may or may not have CD – Nausea, abdominal cramps, diarrhea Diagnosis: • Combination of clinical, laboratory, and histological evaluations • Biopsy of small intestines – gold standard – if positive will show villus atrophy, increased intraepithelial lymphocytes and crypt cell hyperplasia • Serological tests identify presence of antibodies in the blood • Dietary changes can alter diagnostic results, the initial evaluation should be performed before the person has eliminated gluten-containing foods from their diet • Lifelong adherence to a gluten-free diet is the only treatment for CD • Patients should be assessed for nutrient deficiencies before supplementation is started Inflammatory Bowel Disease: Two major forms of IBD are Crohn’s disease and Ulcerative Colitis (UC) • Both are fairly rare and share some clinical characteristics – Diarrhea, fever, weight loss, anemia, malnutrition, growth failure, food intolerances and extra-intestinal manifestations (arthritic, dermatologic and hepatic) – Increased risk of malignancy within the intestines with duration of disease: Adenocarcinoma, T-cell lymphoma Ulcerative • Bloody diarrhea, Rectum always involved, moves continuously, Low inflammation, Deep ulcers, Few strictures, Abscesses in crypts, Surgical resection can result in short bowel syndrome Crohn’s • Abdominal pain (65%), Rectum may not be involved, Surgical removal of strictures • Can occur anywhere GIT: not continuous, “skip lesions”50% to 60% involve distal ileum and colon. More inflammation, Shallow ulcers • Abscesses, fistulas, localized strictures, obstruction of intestinal lumen Inflammatory Bowel Disease • Medical Management: Corticosteroids, Antibiotics, Immunosuppressants • Nutrition Management – Tube feeding / Parenteral Nutrition may be necessary – Foods as tolerated – Multivitamin and mineral supplement, especially folate, B12, and B6 – Omega-3 supplementation – Consider use of prebiotics and probiotics – Small frequent feedings are better tolerated than large meals – If steatorrhea present, MCT may be useful for adding calories Short Bowel Syndrome • Resection of the major parts of the small intestine (treatment for Crohn’s disease, small intestinal cancers etc.) can result in multiple nutrient deficiencies, fluid & electrolyte balance • Intestinal adaptation is the process of intestinal recovery leading to improved absorptive capacity. Ileum has greater adaptive capacity then jejunum. – Permanent effects on B12, nutrition and bile acid reabsorption if ileum removedworsens fat malabsorption and diarrhea – Removal of the ileocecal valve (sphincter) may result in infiltration of colonic bacteria into small intestine causing bacterial overgrowth Medical Nutrition Therapy • Immediately after surgery: fluid & electrolyte replacement (intravenous) • First weeks: rehydration of diarrheal fluid losses • PN (TPN) gradually reduced as oral feeding resumes • Introduction of oral feedings as soon as possible to promote intestinal adaptation – Sips of liquid formulas progressing to larger amounts, Solid foods as tolerated – Small, frequent feedings, Low-fat, high carbohydrate diet if steatorrhea present – Vitamin and mineral supplements, Low-oxalate diet to reduce risk of kidney stones Lactose Intolerance • Causes: genetic or secondary deficiency of lactase (hypolactasia) • Affects ~ 70% population worldwide, especially African Americans, Asians, South Americans • Inability to digest lactose into galactose and glucose • Undigested lactose enters into the colon where bacteria ferment it to short-chain fatty acids, carbon dioxide and hydrogen gas • Nutrition management requires dietary change to reduce/eliminate lactose-containing foods – Most people can tolerate small quantities of lactose; cheese and yogurt better tolerated 1. What is the diagnostic test for lactose intolerance? 2. Sight or smell of food produces vagal stimulation of the parietal cells of the gastric mucosa to produce ___________. 3. What is the function of secretin? 4. The most common cause of antibiotic-induced diarrhea is ______. 5. Why do renal oxalate stones form as a consequence of ileal resection? Lecture 2: Nutrition for Eating Disorders • • • • • ED are debilitating psychiatric illnesses characterized by a persistent disturbance of eating habits or weight control behaviors which significantly impair physical health and psychological functioning. American Psychiatric Association (APA) diagnostic criteria are published in the Diagnostic and Statistical Manual of Mental Disorders IV, TR (DSM-IV-TR). – Anorexia Nervosa (AN), Bulimia Nervosa (BN), Eating Disorder Not Otherwise Specified (EDNOS), Binge Eating Disorder (BED) Affect >10 million people – Females outnumber males 5:1 Typically develop during adolescence or young adulthood, Coexist with other psychological disorders, Recognition of disorder is critical to treatment Identical twins are more likely to share eating disorders. Fraternal twins are less likely Social and Cultural Factors: pressures that glorify thinness and place value on the perfect body Anorexia Nervosa • A disease characterized by:: Refusal to maintain a minimally normal body weight, Distorted body image, Amenorrhea in postmenarchal females • May be one of two subtypes: Restricting, Binge eating and purging • 0.3% to 3.7% of women; rate is about one-tenth in men • Initial presentation is usually during adolescence or young adulthood( as early as 7) • Genetic, environmental (social) and psychological factors, 5% to 25% of patients die • • • Usually Caucasian female, Middle-upper socioeconomic class “responsible, meticulous, and obedient”, Competitive and obsessive High family expectations, Expression of self control AN- Warning Signs • Abnormal, rigid eating habits, Eating very little food (< 1000 kcal/day) • Hiding and storing food, Exercising compulsively, Preparing meals for other, but not eating • Withdrawing from friends and family, Critical of self and others, • Sleep disturbances and depression, Amenorrhea, Vegetarian Clinical Characteristics and Acomplications of AN • Cachectic, “skin and bones” appearance, Lanugo; dry and brittle hair • Cold intolerance, cyanosis of the extremities • Protein-energy malnutrition and cardiovascular complications • Lower basal metabolism, decreased heart rate • Nutrient deficiencies, Gastrointestinal complications, constipation • Osteopenia, osteoporosis, Effects growth and development in children and adolescence Female Athlete Triad of Eating Disorders • Affects athletes in appearance-based sports: 15% swimmers; 62% gymnasts; 32% other sports • Disordered eating, Irregular menses or amenorrhea • Osteoporosis and loss of estrogen: Bone density = 50- 60 y/o/ Bone loss is largely irreversible AN DSM4 Criteria • Refusal to maintain body weight at or above a minimally normal weight for age and height (body weight < 85% of that expected) • Intense fear of gaining weight or becoming fat • Amenorrhea in postmenarchal female: Absence of 3 consecutive menstrual cycles • Restricting type: not regularly engaging in binge eating or purging behavior • Binge-eating purging type: Regularly engaging in binge eating and purging behavior Bulimia Nervosa • Characterized by repeated episodes of binge eating followed by inappropriate compensatory behaviors to prevent weight gain – Self-induced vomiting, laxative and or diuretic misuse, compulsive exercise, or fasting • Affects 1% to 3% adult women • Unusually large amount of food in a discrete period (usually 2-hours) and usually range between 1000 and 2000 kcals per binge – 33% to 75% absorbed after vomiting – 90% absorbed when laxatives are consumed (no vomiting) • Psychiatric comorbidities Bulimia Profile • Young adults (commonly female college students) • Predisposed to becoming overweight: At or slightly above normal weight • Tried several weight reduction diets as a teen • Impulsive behavior, Usually from disengaged families Bulimia Warning Signs • Wrapper/containers indicating consumption of large amounts of food – Hidden binge-and-purge habits, Convenient, high-fat, high-calorie foods • Frequent trips to the bathroom after meals • Signs of vomiting (stains on teeth, calluses on hands) • Excessive and rigid exercise routine (“debting”) • Withdrawal from usual friends and relatives Complications of BN • Related to vomiting: Signs of self-induced vomiting (Russell’s sign) – Erosion of dental enamel, increased dental caries, Esophagitis, sore throat, Dehydration • Laxative use : Dehydration, abdominal cramps, rectal bleeding • Cardiac arrhythmias can occur secondary to electrolyte and acid-base imbalance caused by vomiting, laxative and diuretic use Bulimia DSm4 Criteria • Recurrent episodes of binge eating within any 2 hour period – Large amounts of food, Sense of lack of control over eating during the episode • Recurrent compensatory behavior: Vom, laxatives, diuretics, enemas, fasting, excessing exercise • Binge eating and compensatory behaviors both occurring at least 2 times a week for 3 months Binge Eating Disorder • Characterized by binge-eating episodes at least twice a week for a 6-month period • No inappropriate compensatory behaviors after a binge • Emotional distress and feeling of powerless • Most individuals are overweight: 15% to 50% of individuals are in weight control programs • Night eating syndrome: Eating 1/3 of total calories after evening meal Eating Disorder Not Otherwise Specified • A diagnostic category for eating disorders that meet most, but not all, criteria for either anorexia nervosa or bulimia nervosa – E.g., criteria for AN met but individual has regular menses – E.g., criteria for BN met but compensatory mechanisms occur less than twice a week for less than 3 months – E.g., individual repeatedly chews and spits out, does not swallow, large amounts of food EDNOS: DSM 4 Criteria • Females: all criteria for AN are met except individual has regular menses • All criteria of AN are met except that, despite significant weight loss, individual’s current weight is in normal range • All criteria for BN are met except that binge eating and compensatory behaviors occur at frequency of less than twice a week for less than 3 months • An individual regularly chews and spits out (does not swallow) large amounts of food Eating Disorder Treatment • Multidisciplinary: psychiatric or psychological, medical nutritional • Treatment includes inpatient hospitalization, residential treatment, day hospitalization, intensive outpatient treatment, and outpatient treatment Psychotherapy Treatment • Goals – Help patient understand and cooperate with nutritional and physical rehabilitation – Help patients understand and change behaviors and dysfunctional attitudes towards their EDs – Address psychopathology and psychological conflicts • Behavioral reinforce: Rewards/privilege for attainment of target weight or improved Bx • Treatment usually last a year or more Nutritional Assesment • Anthropometric assessment – Height, weight, skin folds, bioelectrical impedance, Long-term monitoring • Biochemical assessment – Visceral protein stores usually normal , Vitamin and mineral deficiencies – Fluid and electrolyte balance, Accurate lipid profile can only be obtained after a period of dietary stabilization Diet History • Over- and underreporting of food intake • Difficult in estimating calories retained from binges • Chaotic eating difficult to estimate intake • Assessments of eating habits e.g., binge trigger foods, food aversions Anorexia: Medical Nutrition Therapy: Correct the biological and psychological sequelae of malnutrition • Restore body weight – Supervised weight gain in specialized hospital or residential ED program – Three phases: weight stabilization, prevention of further weight loss, weight gain and weight maintenance – 2 to 3 lb/week for hospitalized patient – 0.5 to 1.0 lb/week for outpatient • • • • • • • • • • • Initial caloric prescription may be in the range of 1000 to 1600 kcals/day (30 to 40 kcal/kg of body weight per day) Progressive increases in energy will be needed to promote a consistent and targeted rate of weight gain. To accomplish this the calories are often increased in 100 to 200 calories increments every 2 to 3 days. Aggressive refeeding of the severely malnourished AN patient (<70% standard body weight) may precipitate refeeding syndrome during the fist week of refeeding. AN patients may need 3000 to 4000 kcals per day to achieve goal weight. Patients who require significantly more calories should be questioned or observed for discarding of food, excessive exercising After the goal weight is reached the caloric prescription can be slowly decreased to promote weight maintenance Extreme avoidance of fat is common and avoidance will make it very difficult to provide a concentrated source of energy for weight restoration. Between meal snacks important to reach intake goal for calories Fat intake 30% of total calories recommended Protein intake 15% to 20% of total calories recommended – Vegetarian diets should be discouraged during weight restoration Carbohydrate intake 50% to 55% of calories is well tolerated – Fiber intake important to relieve constipation Calcium and vitamin D rich foods are encourage to help increase bone mineral density Bulimia Medical Nutrition Therapy • BN patients are infrequently hospitalized, counseling will be on out-patient basis • Goals are to develop a plan of controlled eating; interrupt the binge-and-purge cycle, restore normal eating behavior, and stabilize body weight; improved body image and self acceptance • Assess energy needs; reduce calories to ~ 1600 if there is evidence of hypometabolic rate • Body weight should be monitored until weight is stable • BN patients require encouragement to follow weight-maintenance vs. weight-loss diets • Fat intake 25 to 30% of total calories recommended • Protein intake 15% to 20% of total calories recommended • Carbohydrate intake 50% to 55% of calories is well tolerated • Fiber intake important to relieve constipation • BN patients are usually more receptive to counseling than AN patients 1. For individuals with anorexia nervosa, what percentages of protein, carbohydrate and fat are recommended? 2. The definition of amenorrhea is the absence of _______ consecutive menstrual cycles in postmenarchal women. 3. In which eating disorder might a person binge but not try to compensate for this behavior? Lecture 5: Nutrition for Weight Management • • • • • Body weight is often described in terms of its composition and is a total of bones, muscle, organs, adipose tissue and body fluids A two-compartment model divides the body into: – Fat mass (FM): fat from all body sources – Fat-free mass (FFM): includes water, protein and mineral components Lean body mass (LBM) which is only muscle: higher in men, Increases with resistance exercise, Decreases with age Body fat – Essential fat: Essential for normal physiologic functioning, stored in muscle, heart, lung, liver, bone marrow, spleen and nervous system • ~ 3% men, 12% in women – Storage fat: Energy reserve primarily as triglycerides in adipose tissue Total body fat as % of body weight should be: 10% to 25% in men, 18% to 30% in women Adipose Tissue • White: Repository for triglycerides, energy source, insulator and cushion to protect internal organs • Brown: Rapid source of energy and heat production primarily for infants • During normal growth, the greatest % of body fat (25%) is set by 6 months of age, in lean children, fat cell size then decreases; this does not occur in obese children • At age 6 in lean children, adiposity rebound occurs, especially in girls, with an increase in body fat • Fatty acid (FA) composition of adipose tissue mirrors the FA content of the diet • Semivolatile organic compounds (SVOCs) accumulate in adipose tissue from exposure to toxins, chemicals and pesticides. • Weight loss mobilizes the SVOCs and could cause potential harm to the fetus of an obese pregnant female who is undergoing weight loss • Lipoprotein lipase (LPL) moves lipid, from the various lipoproteins in the blood, into the adipose tissue by hydrolyzing the fatty acids from the glycerol backbone of the triglyceride. • Hormones affect LPL activity in different adipose tissue regions – Estrogens stimulate LPL activity in the gluteofemoral adipocytes, needed during pregnancy and lactation • Android (apple) shaped: Body fat stored mainly around upper body • Gynoid (pear) shaped:Body fat stored mainly in gluteofemoral areas Components of Energy Expenditure • Basal Metabolic Rate (BMR) : Minimum amount of energy required to maintain life while physically and mentally at rest in a thermoneutral environment • Resting Metabolic Rate (RMR) – Energy expended in activities necessary to sustain normal body functions (e.g., respiration and circulation) – BMR is rarely measured, RMR is used in its place – Accounts for 60% to 70% of total energy expenditure – RMR declines with age or with restriction of energy intake • Thermic Effect of Food – Energy associated with the consumption, digestion and absorption of food – ~10% total energy expenditure Activity thermogenesis – Most variable component of energy expenditure – Under normal circumstances accounts for 15% to 30% of total energy expenditure • Body Weight Regulation • Short-term regulation – Satiety is associated with the postprandial state when excess food is being stored – Hunger is associated with the postabsorptive state when those stores are being mobilized (dominant control) • Long-term regulation – Involves a feedback mechanism when “normal” body composition is disturbed – Adipocytokines (e.g., leptin, adiponectin, ghrelin, ) released by the adipose cell that act as signaling molecules Estimating Energy Intake • Traditionally, recommendations for energy requirements were based on self-recorded estimates – 24-hour recalls, diet records etc. • Self-reported data problematic: 10% to 45% of people underreport food intake • Online programs allow persons to enter data that will estimate the nutrient content of foods consumed Overweight/Obesity in US (want to reduce or improve by 10%) • 66% of adults are overweight • 32% of adults are obese: Higher in black and Hispanic populations • 33% of children and adolescents are overweight Overweight/Obesity Causes • Genetics: Many hormonal and neural factors involved in weight regulation are determined genetically. Genes determine 50% to 70% of the predisposition to obesity • Ob gene, Adiponectin gene, B3-adrenoreceptor gene, FTO gene • Caloric overconsumption, Inadequate physical activity • • • Sleep deprivation alters endocrine regulation of hunger and appetite promoting excessive energy intake Stress stimulates release of cortisol which stimulates release of insulin to maintain blood glucose levels for a “fight or flight” response….this increases appetite Obesogens “endocrine disruptors” – E.g. bisphenol A and phthalates found in many plastics used in food packaging Assessment of Body Weight • Body Mass Index (BMI) :W/H2 (W= wt in kg, H = ht in meters) • NIH classifications of BMI:: – Normal 18.5 to 24.9 – Overweight 25 to 29.9 – Obese >30 • Class I BMI 30 to 34.9 • Class II BMI 35 to 39.9 • Class III BMI 40 or greater: AKA morbid obesity • Waist Circumference: Men > 40 in; Women > 35 in • Waist to hip ratio: Men: 1; Women: 0.8 • Deurenberg equation: Uses BMI, age and gender Health Risks and Longevity • Heart disease, hypertension, stroke, gallbladder disease, infertility, sleep apnea, hormonal cancers, osteoarthritis, degenerative joint disease, nonalcoholic fatty liver disease • Increased adiposity and reduced physical activity are strong independent risk factors for death in women • Metabolic syndrome, Type 2 diabetes Management of Obesity in Adults • Goal of obesity treatment should focus on weight management, attaining the best weight possible in the context of overall health • Achieving an “ideal” body weight or percentage of body fat may not be realistic • Maintaining present body weight or moderate weight loss is beneficial and may be more achievable • Rate and extent of weight loss: Weight loss involves the loss of both protein and fat • Severe reduction in calories resulting in high rates of weight loss can stimulate the starvation response • Use of glycogen stores, ~ 12% of energy expenditure is from protein and the balance from fat for the first 1 to 2 weeks; then 97% from stored triglycerides • Men reduce weight faster than women of similar size because of their higher LBM and RMR • Mobilizing fat spares LBM, avoids the sharp decline in RMR • Moderate intensity exercise (60% VO Max) for fat oxidation • • • Energy deficits that result in a loss of: – 0.5 to 1 lb per week for a person with BMI 27 to 35 – 1 to 2 lbs per week for a person with BMI > 35 ( 3500 kcal deficit = 1 lb weight loss) This should continue for 6 months for a reduction of ~10% of body weight The focus after 6 months should then be weight maintenance – then further weight loss can be considered • Weight goals should be individualized and realistic with a reduction in body fat as the focus – The gynoid-types and the morbidly obese will not be able to maintain a large weight loss. BMIs of 25 are unreasonable goals for many dieters • Best combination when looking to energy stores is to increase the amount of physical activity and to reduce caloric intake A reduction of 3500 kcals/week = 1 lb body weight = 500 kcals/day decrease caloric intake 250 kcals and increase activity 250 kcals/ day = 500 kcals per day • • • • • • • • • Lifestyle modification (behavior modification) is the key.. Stimulus control (puts us in control) involves modification of: – settings/events that precede eating – Foods consumed when eating does occur – Consequences of eating Problem solving and cognitive restructuring – defining the intake problem and generating possible solutions; implementing a new balance; correct negative thoughts that undermine their efforts Self-monitoring can reveal patterns – records of intake, place/time and physical activity Weight loss programs with success integrate dietary changes with exercise, behavior modification, nutrition education and psychological and social support Several weight-loss programs that have these components – E.g., Weight Watchers® ( eat/prepare foods from supermarket), eDiets Some programs have the many of the same components as Weight Watchers® but they require you to purchase their foods and snacks – E.g., Jenny Craig®, Nutrisystem® Dietary Modification Recommendations: Any calorie-reducing diet should emphasize a balanced approach emphasizing • 50% to 55% of total calories from carbohydrates • 15% to 25% of from protein, 30% or less from fat Vitamin and mineral supplements should be considered when caloric levels of < 1200 for women and <1800 for men are being consumed Meal Replacement Programs – Ready-to-use, portion controlled meal replacements – Goal is to replace other higher calorie foods – Usually contain 10 to 14 g of protein, 0 to 5 g fiber, 0 to 10 g fat, and various amounts of carbohydrates • Substituting one or two daily meals or snacks with meal replacements is a successful weight loss/maintenance strategy. E.g., Medifast®, Optifast®, Slim fast® • Good for individuals who have difficulty with portion control Very-Low-Calorie Diets (200 - 800 kcals/day) – Hypocaloric but have increased protein levels (0.8 -1.5 g/kg/IBW/ per day) – Usually given for a period of 12 to 16 weeks to people who have a BMI > 30 who have not been successful with other diet programs – Occasionally recommended for people with BMI of 27 to 30 with additional comorbidities or other risk factors • Greater weight losses in the short-term, no difference in long-term losses • Increased risk of gallstones, increase of urinary ketones and gout Pharmaceutical Management • Can augment diet, physical activity, and behavior therapy as treatment for people with BMI > 30 or BMI > 27 with significant risk factors or disease Bariatric Surgery • Acceptable form of treatment for people with BMI > 40 or a BMI > 35 with comorbidities • Diet progression after surgery: liquid diet for 2 days, pureed diet day 3 to 3 weeks, soft foods 3 to 6 weeks, regular small meals beyond 6 weeks Physical Activity – important for weight loss and later weight maintenance • 2010 Dietary Guidelines recommends increasing physical activity and reducing time spent in sedentary behaviors • USDA recommends 60 to 90 minutes of moderate-intensity exercise most days of week – Pedometer is a good tool to monitor activity as steps • Aerobic and Resistance Training – Aerobic exercise is important for cardiovascular health through elevated RMR, calorie expenditure, energy deficit and loss of fat – Resistance training increases LBM which in turn increases RMR and increases bonemineral density which is important for women – Bonus: displaces sedentary behaviors, improved sense of well being, better sleep – High-intensity exercise is not required Common Problem in Obesity Treatment • Maintaining Reduced Weight: Energy requirements for weight maintenance after weight loss are ~ 25% less than original weight – Common modifications that have been successful • Eating a relatively low-fat breakfast (24%) of diet, Eating breakfast most days • Weighing regularly, 60 to 90 minutes of physical activity per day • Plateau Effect • Weight Cycling (yo-yo) effect Weight Management in Children • Primary goal is to achieve healthy eating and activity NOT an ideal body weight • For children < 7 years of age – Prolonged weight maintentance without weight gain – let them grow into their weight if no secondary complications are present – If secondary complication(s) is(are) present, then children may benefit from weight loss if their BMI is at the 95th percentile or higher • For children > 7 years – Prolonged weight maintenance if their BMI is between the 85th and 95th percentile and no secondary complications are present – If secondary complication(s) is(are) present or if BMI is at the 95th percentile or above, weight loss (1 lb month is appropriate) • Balanced macronutrient intake for children: – 45% to 60% of kcals from carbohydrates – 25% to 40% fat – 10% to 35% protein • • • • Physical activity is important to displace the sedentary behaviors/hobbies Family modification of diet and behaviors is important Behaviors/habits developed in childhood carryover into adulthood. Adolescent weight is a good predictor of adult weight Physical inactivity may be the result of obesity in children (new theory) 1. What methods of weight reduction have the highest rates of success? 2. _______ may develop during fasting or ager following a very-low-caloric diet. 3. What is the recommended amount and type of exercise for weight maintenance? Nutrition Therapy for Diabetes Mellitus (DM) Reading: Krause’s Food and the Nutrition Care Process 13th ed., Chapter 31, pp. 676-710. Mahan, EscottStump and Raymond. Objectives 1. Understand the basic findings from the Diabetes Control and Complications Trial (DCCT) and the United Kingdom Prospective Diabetes Study (UKPDS). 2. Recommend a nutrition prescription based on given parameters. 3. Identify causes and possible solutions for hypoglycemic and hyperglycemic reactions. 4. Be able to recommend pre- and postexercise nutrition recommendations. Screening and Diagnostic Criteria for Type 2 Diabetes in Asymptomatic Individuals Adults Consider testing for DM in all individuals at age 45 years or above Increase priority if BMI > 25; if normal repeat every 3 years Consider testing in younger individuals who have BMI .25 and have additional risk factors Children and Adolescents Consider testing for DM in individuals who are overweight (BMI >85th percentile) and have two of the following risk factors: First- or second-degree relative with type 2 DM Belongs to a high-risk population group e.g., African American, Native American, Latino, Asian American Begin at age 10 or onset of puberty; if normal repeat every 2 years Major Risk Factors for Type 2 DM (see Chp. 31, page 681 in text) 3 Main Goals for Nutrition Therapy for Individuals with DM 1. To attain and maintain optimal metabolic outcomes: The patient’s blood glucose level should be in the normal range or as close to normal as possible. The lipid and lipoprotein profile should reduce the individual’s risk for macrovascular disease. Blood pressure should be in a range to reduce vascular disease. 2. To prevent, slow the rate of and treat the chronic complications of DM. Modify nutrient intake and lifestyle for the prevention and treatment of obesity, dyslipidemia, cardiovascular disease, hypertension, retinopathy, neuropathy and nephropathy. 3. To improve health through healthy food choices and physical activity. Individualize for each person considering their personal and cultural preferences, lifestyle, and willingness to change. Major nutrition goal for children and adolescents with Type 1 DM is maintenance of normal growth and development. The nutrition prescription is based upon the nutrition assessment. The initial meal plan must provide adequate calories to restore and maintain normal body weight. Many of the newly diagnosed children present with weight loss and hunger. Management of DM is to control blood glucose levels and prevent, delay the onset or progression of retinopathy, nephropathy, neuropathy and long-term cardiovascular problems. Carbohydrate Recommendations Specific to Type 1 and Type 2 DM Type 1 Individuals receiving intensive insulin therapy should adjust their premeal insulin dosages based on the carbohydrate content of meals. Individuals receiving fixed daily insulin dosages should try to be consistent in their daily intake of carbohydrates. Percentage of carbohydrate should be based on an individual nutritional assessment. Fiber intakes should at least meet the minimum 25 grams per day. Type 2 Carbohydrate and monounsaturated fat together should provide 60% to 70% of energy intake. This will need to be individualized according to their metabolic profile and need for weight loss. Fiber intakes should at least meet the minimum of 25 grams per day and larger amounts (up to 50 grams/day) may be beneficial. Protein Recommendations for both Type 1 and Type 2 DM In individuals with controlled Type 2 DM, ingested protein does not increase plasma glucose concentrations. For individuals who have problems with optimal glycemic control, protein requirements may be higher than the RDA of 0.8 grams/kg/body weight. Do not increase protein intake to > 20% of total daily energy. Diets high in protein and low in carbohydrates may produce short-term weight loss and improve plasma glucose levels but long-term effect on LDL-cholesterol a concern. Fat Recommendations for both Type 1 and Type 2 DM Polyunsaturated fat intake should be approximately 10% of total energy intake. Saturated fat intake should be < 10% of total energy intake in individual people with LDLcholesterol < 100 mg/dL. If LDL-cholesterol levels are > 100 mg/dL, decrease saturated fat to < 7% of total energy. Dietary cholesterol should be < 300 mg/day. In individuals with LDL-cholesterol > 100 mg/dL, lower dietary cholesterol intake to < 200 mg/day. Avoid trans fatty acids. Incorporate 2 to 3 servings (~ 2 grams) of plant stanol or sterol foods per day. Substitute this food for similar food. There are good food sources in the bread spreads, salad dressings, mayonnaise-type products on the market. The plant sterol/stanols will lower total and LDL cholesterol levels. Monounsaturated fat and carbohydrate together should provide ~ 60% to 70% of total energy intake. Two or more servings of fatty fish per week will provide n-3 polyunsaturated fat (omega-3 FA). Consider recommending a good omega-3 fish oil supplement if needed. Use of low-fat food and fat substitutes may reduce total fat and energy intake and help to facilitate weight loss. Micronutrient Recommendations for both Type 1 and Type 2 DM There is no clear evidence of benefit from vitamin or mineral supplements in this population unless the individual has underlying deficiencies. Patients should be screened for a vitamin D deficiency and supplementation be initiated in deficient. Emphasis of colorful fruits and vegetables for their phytochemical and antioxidant properties should be emphasized vs. supplements due to uncertainty as to their long-term efficacy and safety. Alcohol Precautions for a diabetic population are the same as the general population. If alcohol is consumed, intake should be limited to one drink per adult woman and two drinks for adult men. One drink is defined as 12-oz beer, 5-oz glass wine, or 1.5-oz glass of distilled spirits. The alcohol should be consumed with food to reduce the risk of hypoglycemia. Physical Activity Previously sedentary individuals can attain significant health benefits by incorporating more lifestyle activities into their daily routines. By accumulating at least 30 minutes per day of moderate activities such as walking, yard work, household chores can make improvements in their overall fitness. Start by incorporating short, frequent intervals throughout the day to reach 30 minutes per session. Exercise Guidelines Blood glucose level must be monitored before and after exercise or periodically during prolonged or unusually intense exercise. This will allow the individual to anticipate the onset of hypo- or hyperglycemia and to take early corrective action. Dosages of insulin or insulin secretagogues should be adjusted as needed for exercise. A 30% to 50% reduction in the dosage of insulin acting during the time of exercise is generally accepted as a safe guideline. Greater reductions may be needed for prolonged, vigorous activity such as long-distance running. Moderate exercise for less than 30 minutes usually does not require any additional carbohydrate or insulin adjustment. If pre-exercise glucose levels are < 100 mg/dL, added carbohydrates should be ingested. Additional carbohydrate foods can be consumed as a pre-exercise meal or snack 1 to 3 hours before the start of exercise. An intake of 1 to 4.5 grams carbohydrate per kg/body weight will optimize liver and muscle glycogen stores. Consume 15 grams of carbohydrate every 30 to 60 minutes of activity if exercise is prolonged (> 45-60 minutes) or intense exercise (>80% maximal heart rate). Post-exercise, as a part of planned meals and snacks. Intake of 1.5 grams carbohydrate per kg/body weight within 30 minutes of an extended exercise session (lasting > 90 minutes) and intake of additional 1.5 grams carbohydrate per kg 2 hours later will support glycogen repletion and reduce the risk of post-exercise hypoglycemia. Hypoglycemia The cause of hypoglycemia is insulin-more is available than is needed relative to food intake and physical activity. The lower the blood glucose targets, the more likely hypoglycemia will occur. Stress, variability in the absorption of diabetes medications and the action on other nondiabetic drugs can also contribute to inconsistent blood glucose level and risk of hypoglycemia. Symptoms are individualized but may include weakness, trouble concentrating, anxiety, blurred vision, tingling in the extremities, headache, shakiness, perspiration, hunger and a rapid heart beat. Mild symptoms can be self-treated. (Rule of 15s) If glucose level is 51-70 mg/dL, consume 15 grams of carbohydrate (1/2 cup juice or regular soft drink, tablespoon of honey or syrup, 3-4 glucose tabs, or 3-8 hard candies). If glucose level is <50 mg/dL, consume 20-30 grams carbohydrate. Check blood glucose level after 15 minutes and repeat if blood glucose does not return to normal range. If it is more than one hour until the next meal, test again after treating as additional carbohydrate may be needed. Hyperglycemia Hyperglycemia refers to any preprandial blood glucose level higher than 130 mg/dL or postprandial blood glucose level higher than 180 mg/dL for men and non-pregnant women. Primary causes of hyperglycemia are related to the balance of food intake, physical activity, therapy for insulin deficiency/insulin resistance, and the level of psychological stress. Inappropriate timing of food and medications is a common contributor. Illness, surgery, hormonal changes, intense emotions are some of the physiologic stressors that can elevate a blood glucose level. Common symptoms are polyuria, polydipsia, polyphagia, blurred vision, weight loss when insulin deficiency is present long enough. Treatment options for short-term hyperglycemia are usually limited to injecting a correcting dose of rapid acting insulin or increasing oral diabetic medications; modifying food intake; and/or increasing activity level. When blood glucose level is chronically elevated, medications and the food plan need to be evaluated and adjusted as needed. Meal-Planning Methods Once the diet prescription has been completed and the goals of nutrition therapy have been established, the intervention process to enable patient self-care can begin. Again, the macronutrient distribution is individualized to the patient based upon their metabolic profile. E.g. Nutrition Prescription: 1900-2000 kcals 50% Carbohydrate (230 grams) 20% Protein (90 grams) 30% Fat (65 grams) There are several ways to plan meals around this prescription. One is to use the “Exchange Lists” for carbohydrates, fruits, vegetables, milk, meats, fats, and sweets/desserts/other carbohydrates. See example in Table 31-9, page 700 text. Another approach is to count carbohydrates which gives more variety and flexibility than the exchange list approach. 15 grams of carbohydrate is = to 1 point (1 carbohydrate choice) or equal to one fruit or starch exchange. 1 milk (8oz) is also equal to 1 point or carbohydrate choice. Protein and fat intake are not counted and this can be problematic if the patient increases their intake of protein and/or fat.