* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Domestic Violence - Milton Keynes Council
Victor Skumin wikipedia , lookup
Psychiatric and mental health nursing wikipedia , lookup
History of psychiatric institutions wikipedia , lookup
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Mental disorder wikipedia , lookup
Pyotr Gannushkin wikipedia , lookup
Controversy surrounding psychiatry wikipedia , lookup
Mentally ill people in United States jails and prisons wikipedia , lookup
Classification of mental disorders wikipedia , lookup
Abnormal psychology wikipedia , lookup
Mental health professional wikipedia , lookup
Nazareth-Conferences wikipedia , lookup
Community mental health service wikipedia , lookup
Deinstitutionalisation wikipedia , lookup
Child psychopathology wikipedia , lookup
History of psychiatry wikipedia , lookup
Homelessness and mental health wikipedia , lookup
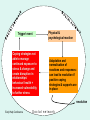
THE TOXIC TRIO: Assessing & Responding to the Impact on Children, Young People and their Families David Glover-Wright Early Help Conference • The term 'Toxic Trio' has been used to describe the issues of domestic abuse, mental ill-health and substance misuse which have been identified as common features of families where harm to children has occurred. They are viewed as indicators of increased risk of harm to children and young people. Early Help Conference Workshop to include: • The key aspects of contemporary practice when working with ‘the toxic trio’ • Assessing and evaluating the impact on children & young people • How to work with families where these problems exist, promoting ‘systemic’, child and family centred approaches • Safeguarding children through the application of holistic risk assessments, ongoing risk management and positive inter agency practice Early Help Conference Social learning/ peer group influences Psycho social factors, gender roles PARENTAL SUBSTANCE MISUSE cognitive/ behavioural impact PARENTAL DOMESTIC VIOLENCE child/ young person increased vulnerability, self medication, negative coping strategies ) Interdependency, emotional stress, trigger points established PARENTAL MENTAL ILL HEALTH Early Help Conference Personal values/ cultural influences/ factors/ / religion Happy families? Early Help Conference What are some of the key concerns? Take five minutes to talk with your neighbour and identify three key concerns in your working practice for families where there is domestic violence (historic/ present), alcohol/ drug dependency and mental health vulnerability. Early Help Conference The Family Model ( after Falkov 1998) Risks: environmental, social, economic, & family stressors = vulnerability Child emotional health & development Parenting & the parentchild relationship Adult mental/ physical health Protective factors and resources: family & social network, coping strategies, emotional resilience We have an ongoing responsibility to balance risk factors against protective factors when working with families. For this to be done effectively, there needs to be a family centred assessment process which focuses individually on the children and adults’ needs and then considers these in the ongoing parent/ child relationship. Early Help Conference Introduction to Mental Health Signs of Safety: • What’s working well? (strengths and positive coping strategies) • What are we worried about? (concerns impacting directly on the children’s wellbeing) • What needs to be done? • Drawing up a safety plan and working in partnership ‘The ecological model’ Early Help Conference • • • • • • • • • Information gathering and analysis is critical: The behaviours exhibited by children experiencing problems in their home environment are often similar, e.g. poor attachment to parents due to emotional unavailability or poor attendance at school or nursery. While mothers’ parenting appears to be adversely affected by domestic violence, there is evidence that their parenting can recover once they are no longer living with domestic violence (Stanley, p54) Cassell and Coleman (1995) suggest that, when assessing the risks of harm for children, professionals should consider the following factors: The warmth of the parent-child relationship The parent’s responsiveness to the child’s needs The content of any delusional thinking The parent’s history of anger management The availability of another responsible adult (Stanley et al p.334) Stanley N, Cleaver H, Hart D (2010) “The Impact of Domestic Violence, Parental Mental Health Problems, Substance Misuse and Learning Disability on Parenting Capacity” The Child’s World. 2nd edition, London: Jessica Kingsley Publishers Cassell, D. and Coleman, R. (1995) Parents with psychiatric problems. In: Reder , R. and Lucey, C. (eds.) Assessment of parenting: psychiatric and psychological contributions. London: Routledge) Early Help Conference Reflective practice Early Help Conference Reflective practice • How can you ensure you are reflective in your practice? • What do you need in your working life to ensure this happens? To be reflective you need to develop your specialist knowledge and increase your practice experience. Early Help Conference KEY HEALTH CONCERNS & INDICATORS • How do we know if children are at risk with parents where there is evidence of the toxic trio? Early Help Conference HEALTH CONCERNS & INDICATORS: • Has the baby failed to thrive? Is the baby showing any of these symptoms irritation and high-pitched crying, often for long periods; rapid breathing and heart rate; disturbed sleep patterns; sweating and fever; vomiting and diarrhoea and feeding difficulties? • Babies of women whose use of opiates, cocaine or benzodiazepines during late pregnancy is heavy are likely to experience withdrawal symptoms. • Do children have accidental or non-accidental injuries? • Children are at increased risk of physical injury during an incident [of domestic violence], either by accident or because they attempt to intervene. • Poverty and a need to have easy access to drugs may lead families to live in unsafe communities where children are exposed to harmful anti-social behaviour and environmental dangers such as dirty needles in parks and other public places • Neglect involving denial of critical care and lack of supervision was most likely to be the sole form of maltreatment in those families with the most severe forms of domestic violence • When intoxicated, parents may fail to hear their child’s cries or notice he/she is unwell; they may accidentally smother them when unconscious due to drugs; they may leave the child unattended when seeking money or drugs Early Help Conference • • • • • HEALTH CONCERNS & INDICATORS contd Do young children present with stomach-aches and bed-wetting (psychosomatic symptomology)? Hester et al note that pre-school children are more likely to show physical symptoms such as stomach-aches and bed-wetting [as a result of living with domestic violence]. (Stanley et al, p.331) Are adolescents involved in problem alcohol or drug use or unsafe sex? Adolescents may become involved in drugs or early pregnancy [as a result of living with domestic violence] (Stanley et al, p.331) (Stanley N, Cleaver H, Hart D (2010) “The Impact of Domestic Violence, Parental Mental Health Problems, Substance Misuse and Learning Disability on Parenting Capacity” The Child’s World. 2nd edition, London: Jessica Kingsley Publishers) Early Help Conference Education concerns: • • • • • • • • • Are younger children meeting developmental milestones? Parents may not have the practical or emotional reserves to engage with their children in order to provide stimulation to support their development. (Stanley et al, p.337) Are appropriate toys available at home? Finding money for drugs may reduce what is available to meet basic needs Do children attend school or nursery regularly? If they attend do they arrive on time? Education can suffer when adolescents stay home to protect their parent or themselves from an abusive partner. For a variety of reasons including disorganisation and lack of self-esteem, drug misusing parents may fail to enable the child to attend pre-school facilities. Are children alert at school or nursery? Are children failing to achieve their educational and developmental potential? Research suggests that children’s education and performance in school may suffer because parental problems dominate the child’s thoughts and can affect concentration (young carers) Early Help Conference Emotional & behavioural development concerns: • • • • • • • • Is there poor attachment with parents? For babies and infants post natal depression may hamper the mother’s capacity to empathise with, and respond appropriately to, her baby’s needs. A consistent lack of warmth and negative responses increases the likelihood that the infant will become insecurely attached. Mood swings, a common feature in mental disorders, can result in inconsistent parenting, emotional unavailability and unexpected and unplanned for separations. The all consuming nature of significant substance misuse problems may mean it becomes the user’s primary attachment, distorting other relationships, including the ability to show children emotional warmth and make them feel valued. (Stanley et al, p.337) Are children expressing anxiety or stress? Primary age school children may present a wide range of behavioural and emotion problems [as a result of living with domestic violence] (Stanley et al, p.331) It is widely accepted that boys are more likely to act out their distress with anti social and aggressive behaviours while girls tend to respond by internalising their worries. Is there evidence of detachment and dissociation in the child/ young person’s behaviour? Witnessing domestic violence affects children’s emotions and behaviour and can lead to temper tantrums and aggression which are directed at family and peers, and cruelty towards animals Early Help Conference Child identity concerns: • What happens when there is lack of support for adolescents going through puberty? • Parental problem drug misuse may mean parents are unaware of children’s worries over their changing body/ personality and fail to provide support and advice • Is there an acceptance of domestic violence (and what happens as a consequence?) • Men participating in Stanley et al’s (2009) study of men’s views and experiences of domestic violence undertaken in northern England described how their perpetration of domestic violence was interwoven with other forms of community violence encountered in childhood and with traditional and persistent conceptions of masculinity (football!) • Does the child or young person have low self-esteem? • Studies undertaken from the perspectives of children and young people also draw attention to the effects of the secrecy and stigma surrounding domestic violence on young people’s self-confidence, self-esteem and consequent capacity for making Early Help Conference Family and social relationships concerns: • Does the child have irregular meal and bed times? • Difficulty in organising day to day living [as a result of parental substance misuse] means that important events such as birthdays or holidays are disrupted and family rituals and routines such as meal or bed times, which cement family relationships, are difficult to sustain. • Adolescents with few friends: • Many adolescents cope with the stress of domestic violence by distancing themselves from their family or friends. • Studies undertaken from the perspectives of children and young people also draw attention to the effects of the secrecy and stigma surrounding domestic violence on young people’s self-confidence, self-esteem and consequent capacity for making relationship with peers. (Stanley, p.31) Early Help Conference Social presentation concerns: • Are children unwashed and wearing dirty clothes? • Difficulty in organising day to day living [as a result of parental substance misuse] means that important events such as birthdays or holidays are disrupted and family rituals and routines such as meal or bed times, which cement family relationships, are difficult to sustain. Early Help Conference Level of self care skills • Are the older siblings caring for their younger siblings? • Education may also be interrupted while parental mental health problems become severe and young people stay home in order to look after their parent or younger siblings. • Do adolescents present as “older than their years?”: • When parents are unable to look after adolescent children adequately [as a result of substance misuse], the normal pace of emotional maturity can be accelerated and for some the relationship between parent and child is reversed. Early Help Conference Good multi agency practice – the key to keeping children safe Partnership working • Research findings (Ward et al 2010) indicate that social workers rarely consult or collaborate with services for substance misuse and domestic violence in carrying out assessments or planning • Collaboration should be given greater priority because practitioners in domestic violence units, alcohol and drug services will have a better understanding of how these issues impact on adult family members and family functioning. • The expertise of practitioners in these specialist services should be used to inform the social work assessments, judgements and planning. How can we promote more effective multi agency practice? (Ward H, Brown R, Westlake D, Munro ER (2010) Infants suffering, or likely to suffer, significant harm: A prospective longitudinal study, London: Department for Education) Early Help Conference Parental mental health • Mental health vulnerabilities are going to be present if there are abusive/ violent parental relationships and if there is substance misuse/ alcohol dependency. Early Help Conference Diagnostic and Statistical Manual of Mental Disorders (DSM-IV) • Organic, including symptomatic, mental disorders (dementias) • Mental and behavioural disorders due to use of psychoactive substances (substance misuse) • Schizophrenia, schizotypal and delusional disorders • Mood [affective] disorders (bipolar, depression) • Neurotic, stress-related and somatoform disorders (anxiety/ agoraphobia) • Behavioural syndromes associated with physiological disturbances and physical factors (eating disorders, nightmares) • Disorders of personality and behaviour in adult persons (BDP, pyromania, transsexualism, paedophilia) • Mental retardation (mild, moderate, severe) • Disorders of psychological development (dyslexia, language disorders) • Behavioural and emotional disorders with onset usually occurring in childhood and adolescence (ADHD) • Unspecified mental disorders (nobody knows…) Early Help Conference Diagnostic labels……… • • • • • • • • Acute psychotic depression Schizoaffective disorder Schizophrenia Long term depression with psychological problems Primary depressive disorder Recurrent psychotic depression Bi-polar disorder Personality disorder (s) Early Help Conference 24 ‘Would you go behind the blinds, take off your personality and put this label on …?’ Illustration by Fran Orford Early Help Conference 25 Impact of Parental Mental Health Problems on Children • Children of mentally ill parents are an ‘at risk group’ • Higher prevalence of emotional and behavioural difficulties in children with a parent with a psychiatric disorder- about a third of these children have a persistent disorder and a further third have transient psychiatric difficulties compared to 10% of a community sample. (Rutter & Quinton,1984, ONS data, 1999, Research in Practice, 2009) Early Help Conference Impact of Parental Mental Health Problems on Children • Increased rates of disorder in children results more from greater psychosocial disadvantage experienced in families affected by parental mental health problems than from the illness per se. • Children’s problems appear to be exacerbated by factors such as marital discord, family disruption and the quality of parent-child interaction. • Recent studies show a more complex relationship between specific disorders in parents and disorders in children. Early Help Conference Early Years • Children develop quickly in their early years and the impact of parental mental health problems can be significant if key developmental stages are affected or impaired Early Help Conference Impact of The Toxic Trio on Children - Feelings • • • • • Distress Anger Worries – fear for themselves Fear for parents Confusion about the situation & the parent’s difficulties. Not understanding the nature of the parent’s illness. • Guilt & Blame – blaming themselves or being blamed • Experiencing hostility and scape-goating for parents’ problems Early Help Conference Impact of The Toxic Trio on Children • • • • • Missing school Missing leisure opportunities eg outings, having friends home Young carers ‘Loss of childhood’ Early Help Conference • But…..How many parents in the UK actually have mental health problems? Early Help Conference • Approximately one in 10 mothers and one in 20 fathers are thought to have mental health problems impacting on their children • At least one in four adults in contact with mental health services is a parent. • As many as 25% of children between the ages of five and 16 have a mother who is at risk of a common mental health problem such as depression or anxiety. • In an average primary school class six or seven children will be living with a mother with a mental health problem; many of these will be lone mothers who are statistically more at risk . Early Help Conference How many parents in the UK have mental health problems? • Overall more women than men have mental health problems. • More younger women and more lone parents than those in couples have mental health problems. • Lone parenthood, particularly among women, seems to be a risk factor for mental health problems. • This is often associated with socio-economic disadvantage and the interaction of other risk factors. Early Help Conference Working together? • Once identified, it is clear that in many cases parents with mental health problems fall through the net and their needs are not met. Services often fail to work holistically with families (despite the ‘Think Family’ approach); poor collaboration and service coordination, together with confusion over professional roles and responsibilities, make the difficulties worse. Early Help Conference Introduction to Mental Health Case scenario 1 • Putting the pieces together Early Help Conference • Children's Social Care received a referral from Weavers School due to concerns for a mother's emotional wellbeing and her problems in getting one of her children to school on time. This seems due to current mental health concerns centring on her anxiety and depression. The family have recently moved to MK from Luton. • Gina has become emotionally distressed due to her partner (and children’s father) Joe leaving the family home a few weeks earlier. School have assisted Gina in seeking medical support from the GP. Joe has since returned to the family home but continually comes and goes leaving for a few weeks at a time. Gina is not willing to accept support from the local CFP but has a good relationship with her GP. • Gina is struggling to sort out her relationship with Joe and has suffered violence and aggression from him in the past. Both Gina and Joe have had difficult childhoods. Gina suffered physical and sexual abuse whilst Joe had a very unhappy childhood with his father dying from alcohol poisoning when he was 11 years. There was also a significant level of domestic violence in his family home. Early Help Conference Introduction to Mental Health Case scenario 1 contd • Joe and Gina confirm relationship problems exist between them. Gina's anxieties and depression impacts on family life and makes it difficult for her to prioritise her 3 young children’s needs. • Joe finds it difficult to cope with ‘family life’ and struggles particularly to have any feelings for Justin (6years). He often shouts at him when things are going wrong in the family. He sometimes loses his temper and will physically damage things by punching and hitting etc. Gina feels her depression is not out of control and doesn’t think its affecting her children in any negative way. She admits she sometimes struggles to get Justin to school as she often feels low and wants to remain in the safety of her home. • The family are isolated and have few contacts in their new area of MK. The other two children (Joshua, 3ys and Jaidon, 1yr) seem to remain in the family home for long periods of time and they seem to seldom leave the family home. 1. What are the key issues and priorities in this case? 2. How can we work with this family? Early Help Conference A Family-Centred Approach • Talk to children & help parents talk to children, promoting good communication & attachment. • Use child-centred language. Always consider the age • and developmental stage of the child(ren) • Drawing, toys and play can help children communicate (signs of safety) • Check out the child’s understanding of parent’s illness. • Provide a child centred explanation of parent’s illness sufficient to help child (ren) make sense of the situation but not so much that it Earlyoverwhelms. Help Conference A Family- Centred Approach Services should plan & work proactively with the family: • Children may want to know about prognosis • Children’s understanding of their parent’s needs can help to pick up on ‘relapse indicators’ • Contingency plans need to be in place for when parent is unwell • There needs to be a positive response to young carer issues • Interventions should promote normal opportunities for children • Supportive relationships need to be engendered in the family’s wider networks (FGCs). Early Help Conference • Working in partnership with the family (systemic approaches) – how can we address the needs of parents and their children using safe and child centred approaches? Early Help Conference Introduction to Mental Health Think Family Approach Early Help Conference Introduction to Mental Health •And not…………. Early Help Conference Circled by Agencies! Early Help Conference Introduction to Mental Health The ecological model • Where are the strengths and where are the weaknesses? • How do we determine what is ‘safe’ and what is risk laden? Early Help Conference APPLYING SYSTEMIC THEORY TO SOCIAL CARE SITUATIONS Social and cultural constraints GP Carol friends Roger Alice Mental Health Social pressures Grandad friends Early Help Conference Introduction to Mental Health Liam Craig school Case Study 3 Craig 14ys, Alice 12ys and Liam 11ys live together with their mother (Carol) and father (Roger) in a small mid-terraced house in Bletchley. Roger and Carol have had a stormy relationship for some years. Roger has begun to spend an increasing amount of time away from the family home staying late at his job as a mechanic in the local garage. When he’s not working he is usually down the local pub and often comes home in a drunken state, which usually sparks off arguments and noisy exchanges. Roger’s behaviour towards his wife has deteriorated and he has begun punching and shoving her when they argue. Carol has become increasingly stressed by the situation and has begun to experience incessant headaches and feelings of panic. She has found it difficult to go to the shops after recently experiencing a panic attack whilst she was waiting in the check out queue. Roger has got in to a dispute with a neighbour and there are regular angry exchanges after complaints were made about the noisy late night rows. The two boys have started to target local families and there are regular incidents of vandalism and criminal damage. The community safety team are already involved with the family as a consequence. The local Age Concern day centre are concerned about Roger’s father and he has been attending with bruising evident to his arms and legs. Carol seems to be her father-in-law’s main carer and she has put this down to his ‘bruising easily’. Craig is persistently truanting from school. He has been hanging out in the city centre and has a pending court case for assault and criminal damage. Both boys are heavy smokers and Carol has found evidence of ‘drugs paraphenalia’ in their bedroom. Liam has been suspended from school for swearing at a teacher and Carol finds it increasingly difficult to discipline the two boys. Early Help Conference Introduction to Mental Health Case Study 3 contd. Carol recently went to her GP and was prescribed tranquillising medication which makes her feel much worse. Alice attends school on a regular basis and has made good progress in her new secondary school. She seems to want to stay on late at school and seldom talks about life at home. Teachers describe her as a very serious intense child who finds it hard making friends. One evening after a particularly violent row with Roger, Carol took a serious over dose necessitating her admission to a medical ward for a few days. Roger attempts to keep the family together as best he can but has frequent angry exchanges with Craig who accuses him of trying to kill their mother. Things reach crisis point later in the week when Craig has a major row with his dad and leaves the house. Carol returns home from hospital to find her husband distraught and upset, Liam has gone out after his brother and Alice is alone in her bedroom. Roger’s father appears to be oblivious to it all and is sitting in his chair from which he seldom moves. 1) What plan of action can you put together which encompasses the needs of this family? 2) What are the key issues you need to address with the family? Early Introduction Help Conference to Mental David Glover-Wright Health The container theory • Rubbish bin or safe container? Early Help Conference The container-contained relationship (Bion 1962) • “Mother is receptive to the baby’s feelings - feeling the baby’s feelings in herself,.Through this the baby’s state of mind and feelings can be tolerated and known by the mother and some sense can be made of them (meaningful attachment). Therefore feelings that were too powerful for the infant to hold within himself can be thus made tolerable…and can be contained by the mother who acts as a container” . • The mother is open to emotional communication- has space for uncertainty and ambiguity in communication, and to think about meaning. Workers should develop this capacity through focused work with parents. • Developing reflective practice and countering the ‘fight or flight’ mechanism. • “Having a sense of being kept in mind provides an opportunity to reflect on emotional experiences” – taking the young person’s thoughts and predicament seriously encourages communication of inner states to take place (Briggs 2002) • The absence of containment leads to children experiencing reduced hope or faith in the possibility of communicating to others about their state of mind; ultimately withdrawal and an emotional shut down will occur • The experiences of being contained in childhood influences the adolescent’s capacity to make sense of and contain the anxiety, ambiguity and uncertainty of adolescence. Having a containing relationship helps one to understand and develop one’s individuality. • Achieving a secure identity can only take place through and within a relationship with others. Early Help Conference 49 Developing a containing relationship with a child/ young person This will involve: • accepting and respecting the child/ young person’s circumstances • striving to be reliable, attentive, empathic, sympathetically responsive and encouraging the child/ young person to talk about their thoughts and feelings • recognising the importance of emotional communications • providing psychological space and keeping him/her in mind • having a ‘psychological space’ to reflect & think Because: • Containing relationships has a transformational impact on adolescent turbulence. Being kept in mind enables the adolescent to develop and bear the emotional impact of his/her thoughts and feelings. • Developing their capacity to make intimate emotional bonds with others, enables effective personal functioning and stable mental health Early Help Conference 50 Developing emotional resilience in families • Understanding the cycle of crisis Early Help Conference 51 • Families where there are multiple problems and poor coping strategies will often ‘cycle’ in and out of crisis. This can have a serious impact on children and young people’s emotional wellbeing and their later life experiences. Early Help Conference Crisis Theory • Caplan’s theory of crisis and crisis intervention: • 4 stages of crisis: • 1) situation is challenged by trigger events (change/ loss/ threat to status quo). People cope using their resources; there is awareness of strained relationships and changing roles but people ‘make do and mend’ • 2) situation becomes ‘normalised’; people adapt to the crisis sustaining routines and behaviour but emotional and psychological pressures being to grow • 3) situation begins to become ‘externalised’ there are confrontations, angry exchanges and ‘flash points’ which are patched up but tensions are breaking through and behaviours/ roles are changing; young people are labelled and formalised in a crisis role • 4) situation breaks down; coping strategies are no longer working and strengths and resources have been exhausted. Caplan called this stage the ‘disequilibrium of crisis’ and he saw this as the time when the most positive work could be undertaken. Early Help Conference Trigger/ event Coping strategies not able to manage continued exposure to stress & change and create disruption in relationships/ behaviour/ health = increased vulnerability to further stress Physical & psychological reaction Adaptation and normalisation of reactions and responses: can lead to resolution if positive coping strategies & supports are in place resolution Early Help Conference SocIal network Stress/ Performance Curve Performance Optimal Stress/ Performance curve Optimal level of output; mental/ physical exertion lead to exhaustion Stress increases but performance doesn’t Crisis point Early Help Conference Stress Children's messages Early Help Conference • • • • • Introduce yourself – tell us what your job is Give us as much information as you can Tell us what is wrong with our parents Tell us what is going to happen next Talk to us and listen to us. Remember it’s not hard to speak to us; we are not aliens • Ask us what we know and what we think. We live with our parents; we know how they have been behaving Early Help Conference • Tell us it’s not our fault. We can feel guilty if our mum or dad is ill. We need to know we are not to blame • Please don’t ignore us. Remember we are part of the family and we live there too. • Keep on talking to us and keep us informed. We need to know what is happening • Tell us if there is anyone we can talk to. MAYBE IT COULD BE YOU. Early Help Conference Risk management and safeguarding in families where there is evidence of the toxic trio Working in partnership with families Early Help Conference Competent risk management practice with children and families should: • 1 – Adopt a holistic, family centred approach • 2 – Employ identified risk criteria thresholds within a framework of assessment and related intervention seeking advice and support from senior staff – assessment needs to be side-byside with intervention Early Help Conference • 3 – Involve parents and children in ongoing practice, validating their perceptions and opinions • 4 – Avoid gender bias; this is particularly pertinent in a female dominated work force where the role and opinion of fathers can be neglected • 5 – Utilize multi disciplinary processes of assessment and decision making, validating other profession’s perspectives and knowledge base • 6 – Be explicitly shared in supervision and case discussions and then recorded in ongoing case notes and decision making processes • 7 – Compile detailed and family centred risk assessment and management documentation Early Help Conference • RISK ASSESSMENT FOR FAMILIES WHERE THERE ARE MENTAL HEALTH PROBLEMS: • Identified Risk Areas: • Score out of 5: 5 = current; 4= historic/ recent (last 6 months); 3 = historic/ past (over 6 months); 2 = background predictors (family history); 1 = background predictors (current circumstances) 0 = no risk factors present Early Help Conference 7 most frequently encountered risk factors for children in families where there are MH problems Parenting problems Environment Early Help Conference Neglect Substance misuse Family/ Third party Domestic violence Child’s behaviour/ health Define behaviours which generate scores noted above: • Parenting: (Poor attachment/ inconsistent approaches) • Environment: (Unhygienic living conditions/ hazardous environment) • Neglect: (Children left alone unsupervised/ health appointments missed/ educational problems) • Substance Misuse: (Alcohol consumption/ substance misuse leading to intoxication ) • Family/ Third Party: (Ongoing unknown adult visitors to home) • Domestic Violence: (Current/ previous partner violent & abusive) • Child’s Behaviour/ Health: (Child destructive and unable to settle/ poor routines) Early Help Conference Risk assessment contd. • Outline risk areas which may interact in a dangerous manner, provide evidence for this in current family situation and information source (eg domestic violence and alcohol consumption/ poor parenting and leaving child alone/ previous evidence of risks occurring) Early Help Conference Risk assessment contd. • Outline family strengths and resources which can be consolidated & developed to address risk factors outlined above: • 1) • 2) • 3) • 4) Early Help Conference Define key interventions & resources needed to address risks outlined above: • • • • • • • Parenting: Environment: Neglect: Substance Misuse: Family/ Third Party: Domestic Violence: Child’s Behaviour/ Health: Early Help Conference Risk Factor Parenting Environment Neglect Substance misuse Family/ third party Domestic violence Child’s behaviour/ health needs Early Help Conference Hoped for outcomes Risk assessment contd. • Share the risk plan with the family and encourage their participation and ownership • Review the risk plan and evaluate with the family providing positive reinforcement as progress is made Early Help Conference Safeguarding children in families with a parent with mental health problems • The responsibility for safeguarding children does not only lie with children’s services. It is a requirement of safeguarding children that adult services, including mental health services, know whether their service users have children or are in contact with children. • It is therefore important to be able to recognise and understand what contribution adult mental health problems make to an assessment of overall risk of harm to children. Early Help Conference Introduction to Mental Health Signs of Safety Model Signs of safety Assessment & Planning Form SAFETY DANGER/ RISK List all aspects that demonstrate likelihood of maltreatment (past, present & future) What are we worried about? Safety & Context Scale: List all aspects that demonstrate safety (resources, goals, willingness to change) What is working well? Safety scale: Rate the situation 0-10 where 0 means recurrence of similar or worse abuse/ neglect is certain and 10 means there is sufficient safety for the child. Context scale: rate this case on a scale of 0-10, where 10 means no action is taken and 0 means this is the worse case of child abuse/ neglect the agency has observed Agency goals: What will the agency need to see occur to be willing to close the case? Family goals: What does the family want generally and regarding safety? Immediate progress: What would indicate to the agency that some small progress has been made? Early Help Conference What needs to happen? Early Help Conference Signs of Safety Model • Turnell, A. and Edwards, S. (1999). Signs of Safety: A safety and solution oriented approach to child protection casework, New York: WW Norton. Early Help Conference • Thank you and any feedback would be welcome! • David Glover-Wright ([email protected]) Independent Trainer Early Help Conference