* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Peptic Ulcer Disease
Survey
Document related concepts
Ascending cholangitis wikipedia , lookup
Transmission (medicine) wikipedia , lookup
Kawasaki disease wikipedia , lookup
Behçet's disease wikipedia , lookup
Childhood immunizations in the United States wikipedia , lookup
Multiple sclerosis research wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Autoimmunity wikipedia , lookup
Schistosomiasis wikipedia , lookup
Ankylosing spondylitis wikipedia , lookup
Globalization and disease wikipedia , lookup
Germ theory of disease wikipedia , lookup
Rheumatoid arthritis wikipedia , lookup
Transcript
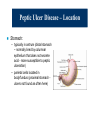
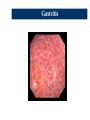
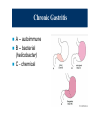
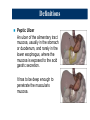
Upper Gastrointestinal Diseases Upper GI Diseases Esophagus Stomach Duodenum Esophageal Diseases Esophageal Diseases Esophageal Symptoms Esophageal Motility Disorders Gastroesophageal Reflux Esophageal Swallowing Disorders Esophageal Symptoms Dysphagia = difficulty swallowing – oropharyngeal dysphagia = difficulty initiating swallow or transferring food from mouth into esophagus. Can also experience nasopharyngeal regurgitation (comes out nose) or pulmonary aspiration. – esophageal dysphagia = food gets stuck in esophagus after swallowing Esophageal Motility Disorders Achalasia (failure to relax) Diffuse Esophageal Spasm (DES) Achalasia Most often results from post-ganglionic denervation of smooth muscle of esophagus absence of inhibitory neural input to LES ↑ LES pressure Functional esophageal obstruction can lead to esophageal dilatation Similar disorder in Chagas disease (Trypanosoma cruzi causes injury to myenteric plexuses of esophagus) Diffuse Esophageal Spasm (DES) periodic chest pain & dysphagia high amplitude, simultaneous, repetitive SM contractions – can be spontaneous or initiated by swallow barium swallow “corkscrew” appearance to esophagus pathogenesis unknown Gastroesophageal Reflux (GER) A little bit of GER is normal in all of us – Normally, thoraxic cavity has negative pressure during inspiration – GER would occur continuously without antireflux mechanisms – a portion of esophagus is below the diaphragm intra-abdominal pressure (+5 mm Hg) can reinforce LES pressure (antireflux effect) – Loss of subdiaphragmatic LES correlation between esophageal hernia and GERD Gastroesophageal Reflux (GER) Mechanisms Incompetent anti-reflux mechanisms Ineffective esophageal clearance Decreased gastric emptying Gastroesophageal Reflux (GER) Risk factors Obesity Pregnancy Smoking High-fat foods Theophylline Caffeine Coffee Chocolate High levels of estrogen/progesterone Gastroesophageal Reflux (GER) Pyrosis Dyspepsia Regurgitation Dysphagia Gastroesophageal Reflux (GER) Diagnosis of GER Best test: pH probe – checks for existence of acid reflux and association between esophageal acid and chest pain Other tests – Barium swallow – Esophagoscopy – Esophagial biopsy Gastroesophageal Reflux (GER) Complications of GERD – – – – – – – Erosive esophagitis Esophageal ulcer Bleeding Esophageal stricture Intestinal metaplasia (Barrett’s) Adencarcinoma from Barrett’s Lung diseases Gastritis and Ulcer Disease Peptic Ulcer Disease – Range of injury Ulcer: A lesion on an epithelial surface (skin or mucous membrane) caused by superficial loss of tissue. Erosion: A lesion on an epithelial surface (skin or mucous membrane) caused by superficial loss of tissue which is limited to the mucosa. Peptic Ulcer Disease – Location Stomach: – typically in antrum (distal stomach – normally lined by columnar epithelium that does not secrete acid - more susceptible to peptic ulceration) – parietal cells located in body/fundus (proximal stomach ulcers not found as often here) Peptic Ulcer Disease – Location Duodenum: – – – – within duodenal bulb can cause outlet obstruction usually single multiple/large/more distal ulcers (Zollinger-Ellison sdr.) Gastric Mucosa & Secretions The defensive forces – Bicarbonate – – – – The aggressive forces – – – – – – – Mucus layer Mucosal blood flow Prostaglandins Growth factors Helicobacter pylori HCl acid Pepsins NSAIDs Bile acids Ischemia and hypoxia Smoking and alcohol When the aggressive factors increase or the defensive factors decrease, mucosal damage will result, leading to erosions and ulcerations. Gastritis Causes of Acute Gastritis Alcohol NSAIDs Helicobacter Stress/ICU associated Mechanisms of Acute Gastritis Drugs (non-steroidal anti-inflammatory drugs NSAID), alcohol cause acute erosion (loss of mucosa superficial to muscularis mucosae).Can result in severe haemorrhage Acute Helicobacter infection has a prominent neutrophil infiltrate Chronic Gastritis A – autoimmune B – bacterial (helicobacter) C - chemical Chronic Gastritis Type A - Autoimmune (associated with vitamin B12 malabsorption (pernicious anaemia) Type B - Helicobacter pylori infection Type C - Chemical damage (bile reflux, drugs) Helicobacter Pylori Adapted to live in association with surface epithelium beneath mucus barrier Causes cell damage and inflammatory cell infiltration In most countries the majority of adults are infected Helicobacter Gastritis Acute inflammation mediated by complement and cytokines Polymorphisms infiltrate epithelium and may be partly responsible for its destruction An immune response is also initiated (antibodies may be detected in serum) Consequences of Gastritis Peptic ulcer disease (Helicobacter) Adenocarcinoma (all types) Definitions Peptic Ulcer An ulcer of the alimentary tract mucosa, usually in the stomach or duodenum, and rarely in the lower esophagus, where the mucosa is exposed to the acid gastric secretion. It has to be deep enough to penetrate the muscularis mucosa. Etiology The two most common causes of PUD are: – Helicobacter pylori infection – Non-steroidal anti-inflammatory drugs (NSAIDS) Other uncommon causes include: – – – – Gastrinoma (Gastrin secreting tumor) Stress ulceration (trauma, burns, critical illness) Viral infections Vascular insufficiency Etiology – Helicobacter pylori Helicobacter pylori PUD – Clinical Presentation Symptoms of PUD Pain – Epigastric pain – Hunger pain – Nocturnal pain Other symptoms – Waterbrash – Heartburn – Vomiting Asymptomatic – 1% - 3% adults endoscopy volunteers – 20% of complicated ulcers present without previous symptoms Peptic Ulcer Disease - Diagnosis Diagnosis of ulcer Diagnosis of H. pylori Diagnosis of H. pylori Tests for Helicobacter pylori Non-invasive C13 or C14 Urea Breath Test Stool antigen test H. pylori IgG titer (serology) Invasive Gastric mucosal biopsy Rapid Urease test PUD – Complications Complications of PUD Bleeding Perforation Gastric outlet or duodenal obstruction Chronic anemia