* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Digestive System
Survey
Document related concepts
Transcript
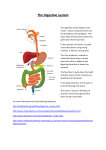
Chapter 24 The Digestive System BIO 211 Lab Instructor Dr. Gollwitzer 1 • Today in class we will: – Discuss the gastrointestinal tract and identify its components – Identify the accessory organs associated with the digestive tract – The layers that make up the digestive tract wall and each layer’s characteristics • • • • Mucosa Submucosa Muscularis externa Serosa – Begin our discussion of the gastrointestinal tract components in more detail • Oral cavity • Pharynx • Esophagus 2 Digestive System • Gastrointestinal (GI) tract = continuous, muscular tube from mouth to anus – Oral cavity (mouth) – Pharynx – Esophagus – Stomach – Small intestine – Large intestine – Anus 3 Digestive System • Accessory digestive organs = any digestive organ attached to the GI tract – Teeth – Tongue – Glandular organs • Salivary glands • Pancreas • Liver – Gall Bladder 4 Figure 24-1 5 Histological Organization • 4 Major layers to wall – Mucosa – Submucosa – Muscularis externa – Serosa 6 Figure 24-3 7 Mucosa • Inner lining of digestive tract • A mucous membrane • Consists of – Epithelium - moistened by glandular secretions – Lamina propria = areolar CT “filler” 8 Mucosa: Digestive Epithelia • Depend on location, function, stresses • Simple or stratified • Columnar or squamous 9 Mucosa: Digestive Epithelia • Nonkeratinized stratified squamous epithelium – Where mechanical stress most severe – In oral cavity, pharynx, esophagus, rectum – Life span = 2-3 days • Simple columnar epithelium – Where absorption and secretion occur (with villi and goblet cells) – Stomach, small intestine, most of large intestine – Life span = 6 days 10 Mucosa: Lamina Propria • Layer of areolar (loose connective) tissue • Contains – Blood vessels, sensory nerve endings, lymphatic vessels, lymphoid tissue – Mucosal glands and glandular secretions – Muscularis mucosae/interna • Band of smooth muscle and elastic fibers • Smooth muscle arranged in 2 concentric layers – Inner, circular layer (around lumen) – Outer, longitudinal layer • Contractions alter shape of lumen and move epithelial folds 11 Mucosa: Glandular Structures • Have secretory function • Associated with simple columnar cells and/or mucous-secreting cells • Goblet cells (exocrine) mucus • Enteroendocrine cells – hormones (e.g., G cells gastrin) – Coordinate activities of digestive tract and accessory glands • e.g., chief cells, G cells, parietal cells 12 Submucosa • Layer of dense, irregular connective tissue • Around muscularis mucosae • Contains – Large blood vessels and lymphatic vessels – Exocrine glands buffers and enzymes into lumen – Submucosal plexus contains nerve fibers and neurons 13 Muscularis Externa • Dominated by smooth muscle cells – Inner, circular layer – Outer, longitudinal layer • Important role in mechanical processing and movement of materials along tract • Also contains – Lymphoid nodules (Peyer’s patches) • Masses of lymphoid tissue; have lymphocytes that protect small intestine from bacteria that are normal inhabitants of large intestine – Myenteric plexus/plexus of Auerbach • Network of neurons located between circular and longitudinal muscle layers • Movements coordinated by enteric nervous system (part of ANS) 14 Serosa • A serous membrane = lines sealed, internal subdivisions of ventral body cavity • Covers muscularis externa of most of digestive tract – except oral cavity, pharynx, esophagus, and rectum, which have adventitia (a dense collagen fibrous sheath) 15 Figure 24-3 16 Figure 24-3 17 Oral (Buccal) Cavity • Space within mouth • Lined by oral mucosa (nonkeratinized stratified squamous epithelium) • Vestibule = space between cheeks or lips and teeth – Labial frenulum = fold of mucosa; connects lip to gum • Cheeks = lateral walls of oral cavity – Mucosae supported by fat pads and buccinator muscles • Labia (lips) • Gingivae (gums) – Ridges that surround base of each tooth – On alveolar processes of maxillary bones and mandible 18 Oral (Buccal) Cavity • Palates – Hard palate – formed by maxillary bones (anterior) and palatine bones (posterior) – Soft palate – fleshy part posterior to hard palate • Formed from skeletal muscle • Posterior margin supports uvula = dangling process that helps prevent food from entering pharynx prematurely • Tongue – Muscular organ attached to floor of oral cavity – Dorsum (superior) surface covered with lingual papillae (location of taste buds) – Lingual frenulum – thin fold of mucous membrane that attaches tongue to floor of oral cavity 19 Figure 24-6 20 Pharynx • Throat area posterior to nasal and oral cavities – Shared by respiratory and digestive systems • Extends between internal nares and entrances to larynx and esophagus – Nasopharynx • Posterior portion or nasal cavity • Separated from oral cavity by soft palate • Contains – Pharyngeal tonsils and opening to auditory (eustachian) tube – Oropharynx • Posterior portion of oral cavity • Between soft palate and base of tongue • Fauces = opening between oral cavity and oropharynx – Laryngopharynx • Inferior part • Between hyoid bone and entrances to esophagus and larynx 21 Esophagus • Hollow, muscular tube • From posterior laryngopharynx to stomach • Descends through thoracic cavity posterior to trachea • Enters abdominopelvic cavity through esophageal hiatus in diaphragm 22 Esophageal Histology • Muscularis externa transitions from – Skeletal muscle fibers (superior third) to – Smooth muscle fibers (inferior third) • Adventitia – CT outside muscularis externa (no serosa) – Anchors esophagus against dorsal body wall 23 Esophageal Sphincters • Circular smooth muscles that control entrance/exit to esophagus • Upper esophageal sphincter – In superior 1 in. – Prevents air from entering • Lower esophageal sphincter – At inferior end – Prevents backflow from stomach 24 • Today in class we will: – Complete our more detailed discussion of the gastrointestinal tract components • • • • Stomach Small intestine Large intestine Anus – Begin our discussion of the 4 accessory digestive organs • Teeth • Tongue • Glandular organs – Salivary glands 25 Stomach • Muscular tube with extra layers of smooth muscle cells – Strengthen stomach wall – Assist in mixing/churning activities required to form chyme – Muscularis mucosae/interna – has extra outer, circular layer – Muscularis externa – has oblique layer 26 Figure 24-13 27 Stomach • Has expanded J shape – Lesser curvature = shorter, inner, medial surface – Greater curvature = longer, outer, lateral surface 28 Figure 24-12b 29 Stomach • Has 4 regions – Cardia • Smallest region where esophagus enters (at gastroesophageal/cardiac sphincter) – Fundus • Superior hump to left of cardia that contacts the diaphragm – Body (corpus) • Main (middle) region of the stomach between fundus and curve – Pylorus • Last part of stomach that enters the duodenum through pyloric sphincter 30 Stomach • Rugae – Folds of gastric mucosa – Temporary features – Let gastric lumen expand (almost disappear when stomach full) 31 Stomach • Gastric pits – Depressions that open onto gastric surface – Each communicates with several gastric glands – Mucous cells line neck • Gastric glands – In fundus and body of stomach – 2 types of secretory cells • Parietal cells • Chief cells 32 Figure 24-13b 33 Small Intestine • 3 Regions – Duodenum (10 in.) • First part; connects to pylorus • “Mixing bowl” – Receives chyme from stomach and secretions from pancreas and liver • Curves in a C that encloses head of the pancreas – Jejunum (8 feet) • Middle part • Site for most of chemical digestion and nutrient absorption – Ileum (12 feet) • Last part • Connects to large intestine via ileocecal valve 34 Small Intestine • Plicae circulares – inner folds in intestinal lining – Permanent feature -- do not disappear when small intestine fills • Wall – Mucosa • Intestinal epithelium – Simple columnar epithelium; covers villi (pl; singular = villus) • • • • Villus capillaries/villus capillary network Lacteals Intestinal glands (goblet cells, enteroendocrine cells) Muscularis mucosae/interna – Submucosa, muscularis externa, and serosa as described previously 35 Figure 24-16 36 Figure 24-17 37 Large Intestine (Bowel) • 3 Main sections – Cecum – Colon (4.5 ft) – Rectum (6 in.) 38 Large Intestine (Bowel) • Cecum – Pouch-like structure that connects to ileum (at ileocecal valve) – Vermiform appendix = small, worm-like appendage of lymphoid tissue attached to cecum 39 Large Intestine (Bowel) • Colon – Ascending colon – along right side; takes right turn at superior end = right colic/hepatic flexure – Transverse colon – crosses from R to L; takes right turn downward at left end = left colic/splenic flexure – Descending colon – along left side; curves medially at sigmoid flexure – Sigmoid colon – S-shaped; empties into rectum • Haustra – Pouches caused by longitudinal bands of muscularis externa (taeniae coli) – Permit expansion and elongation of colon 40 Large Intestine (Bowel) • Rectum – Anal canal = last portion – Contain small longitudinal folds (anal columns) – Anus/anal orifice = exit of anal canal – Contains 2 sphincters • Internal anal sphincter – smooth muscle, involuntary control • External anal sphincter – skeletal muscle, voluntary control 41 Figure 24-24a 42 Teeth • Located in alveoli (bony sockets) on alveolar processes of maxillary bones and mandible • Number – Primary (deciduous) • 5/side/jaw = 20 – Secondary • +3 molars/side/jaw = 32 • Replace primary teeth 43 Figure 24-9a, b 44 Tooth Type No./ Jaw Location Shape Function No. Roots Incisors 4 Center front Blade Clip/cut 1 Cuspids/ Canines 2 Lateral to incisors Conical w/sharp ridge, pointed tip Tear/ slash/ shear 1 Bicuspids/ Premolars 4 Posterior to Flattened cuspids crown, prominent ridges Crush/ mash/ grind 1 or 2 Molars (wisdom teeth) 6 Posterior to Large, bicuspids flattened crown, prominent ridges Crush/ grind 3 or more 45 Teeth • Parts – Crown – above gum line – Neck – boundary between crown and root – Root – below gum line; sits in alveolus 46 Teeth • Layers/Regions – Outer • Enamel – Thin, white layer that covers crown – Hardest biologically manufactured substance • Cementum – Thin layer that covers root; protects and helps anchor tooth – Inner • Dentin – Makes up bulk of tooth – Mineralized matrix (CaPO4 crystals) similar to bone, except acellular • Pulp cavity – Central region – Receives blood vessels and nerves from root canal • Root canal – Narrow tunnel at root/base of tooth – Blood vessels and nerves enter through apical foramen 47 Figure 24-8a, b 48 Salivary Glands • Outside oral cavity, but secrete into oral cavity • 3 pairs – Parotid glands • Extend from mastoid process of temporal bone across outer surface of masseter muscle • Parotid (Stenson’s) duct – from parotid through buccinator to oral cavity – Sublingual glands • Under the floor of the mouth • Many small sublingual (Rivinus’) ducts open along side of lingual frenulum – Submandibular glands • Along inner surfaces of mandible • Submandibular (Wharton’s) ducts – open into mouth on either side of lingual frenulum immediately posterior to teeth 49 Figure 24-7a, b 50 • Today in class we will: – Complete our discussion of the 4 accessory digestive organs • Glandular organs – Pancreas – Liver » Histology » Bile duct system • Gall bladder – Trace the path of food through the digestive system 51 Pancreas • Lies posterior to stomach, extends laterally from duodenum toward spleen • Covered by thin, CT capsule • 3 regions – Head – burrowed in loop of duodenum – Tail – tapered end against spleen – Body – slender middle region • Ducts – deliver digestive enzymes and buffers to duodenum – Main pancreatic duct (of Wirsung) – large, main duct major duodenal papilla with common bile duct duodenal ampulla (chamber) – Accessory pancreatic duct (of Santorini) – may branch from pancreatic duct minor duodenal papilla duodenal ampulla 52 Fig. 24-18, p. 888 53 Gallbladder • Hollow, pear-shaped, muscular sac • Located in recess on posterior surface of liver’s right lobe • 3 regions – Fundus – bottom of pouch – Body – main region – Neck – narrow end where cystic duct exits 54 Figure 24-19 55 Liver • Largest visceral organ • Covered by tough, fibrous capsule • Divided into 4 lobes – Right lobe – largest, in right hypochondriac region – Left lobe – narrow part extending into left hypochondriac region – Caudate lobe – on inferior side; superior, near IVC – Quadrate lobe – inferior to caudate, near gallbladder • Falciform ligament – on anterior surface between R and L lobes 56 Liver Histology • Hepatocytes = liver cells; simple cuboidal cells • Each liver lobe divided into lobules • Liver lobule = basic functional unit of liver – Has hexagonal shape (6 corners) – Hepatic triad at each corner contains • Branch of hepatic portal vein • Branch of hepatic artery • Branch of bile duct – Separated by interlobular septa – Each has a central vein – Hepatocytes • Form 1-cell wide plates arranged like spokes around a wheel around central vein – Plates are separated by sinusoids = modified blood vessels for large solutes can pass out of/into blood stream 57 Liver Histology • Branches of hepatic portal vein (from intestine to liver) and hepatic artery (to liver from systemic circulation) sinusoids – Hepatocytes absorb solutes and secrete materials (plasma proteins) into sinusoids – Blood leaves sinusoids and enters central vein of lobule – Central veins hepatic veins IVC heart • Kupffer cells – Phagocytic cells (lymphatic cells) – Functions • Engulf pathogens, cell debris and damaged blood vessels • Store iron, lipids, heavy metals absorbed by digestive tract 58 Figure 24-20 59 Bile Duct System • Hepatocytes bile bile canaliculi bile ductules R and L hepatic ducts common hepatic duct • Common hepatic duct + cystic duct (to/from gallbladder) common bile duct • Common bile duct meets pancreatic duct at duodenal ampulla duodenal papilla • Hepatopancreatic sphincter - encircles – Common bile duct, pancreatic duct, and duodenal papilla 60 Figure 24-21a, b 61