* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Atrial fibrillation Patient Information Leaflet
Survey
Document related concepts
Saturated fat and cardiovascular disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Rheumatic fever wikipedia , lookup
Jatene procedure wikipedia , lookup
Heart failure wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Electrocardiography wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Transcript
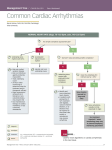
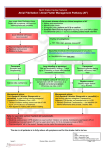
Atrial fibrillation Patient Information Leaflet Atrial fibrillation, often shortened to ‘AF’ is a very common heart rhythm abnormality. It affects 1 in 20 middle aged people and around 1 in 10 people over the age of 80. The right and left ‘atria’ are the two heart chambers which collect blood from the body and the lungs respectively. When working correctly, they push blood into the ‘ventricles’, the main pumping chambers, from which blood is then pumped to the lungs to be refreshed with oxygen or around the rest of the body to feed the brain, muscles, internal organs and the heart itself with nutrients and oxygen. Many patients are not aware that their heartbeat is no longer regular and in AF, and it is often only picked up on examination by a doctor and confirmed on an ECG (tracing of the electrical activity of the heart). AF may occur suddenly often due to an acute illness, may come and go intermittently (termed ‘episodic’ or ‘paroxysmal’) or be chronic and persistent. The healthy heart’s natural pacemaker and internal ‘wiring’ ensures that the timing of the contraction of the atria and ventricles is properly co-ordinated – this is called sinus rhythm. Atrial fibrillation, literally means ‘shaking or wobbling of the atria’. There is a loss of the normal contraction of the atria and the important co-ordination with the ventricles. The normal regular, steady heart beat becomes fast and chaotic leading to a reduction in the efficiency of heart function. Typical symptoms include: • Irregular pulse or sensation of fast, irregular heart beating in the chest – a form of palpitation • Shortness of breath and tiredness when walking or running • Chest tightness or pain • Feeling light-headed or dizzy There are a variety of conditions which can lead to AF. Common underlying causes include: • Undetected or uncontrolled high blood pressure • ‘Wear n’ tear’ of the heart’s internal electric wiring • Heart attacks due to coronary artery disease • Excessive chronic or binge alcohol drinking • Chronic lung damage due to smoking • Infections especially of the lung • Disorders of heart muscle cardiomyopathies • Thyroid gland disorders • Leaky or narrowed heart valve • Heart surgery The main long-term risks or complications to health related to AF are: • Blood clots developing within the atria causing a blockage in blood vessels supplying the arms, legs or internal organs called an embolus or part of the brain called an embolic stroke. • Enlargement and weakening of the heart resulting in heart failure. © Dr Winston Martin January 2007 - Information accurate at time of going to print. Darent Valley Hospital, Darenth Wood Road, Dartford, Kent , DA2 8DA - Telephone: 01322 428100 - www.dvh.nhs.uk 1 The main aims of treatment in AF are: • Rate control - Slowing the heart rate to ease symptoms and prevent heart enlargement. • Anticoagulation - Blood thinning to prevent blood clots. • Cardioversion - Restoration of normal heart rhythm if possible. • Maintaining sinus rhythm – Keeping the heart beat regular and co-ordinated. Rate control Maintaining SR Cardioversion Anticoagulation The exact treatment of a patient with AF can be complex and depends on a number of factors: • How long the heart has been in AF • The severity of any symptoms • The presence of any underlying heart disease • The presence of other underlying conditions or illnesses Rate control There are a number of different drugs termed anti-arrhythmic drugs which can reduce fast heart rate. Common drugs include: • Beta-blockers such as atenolol, bisoprolol and sotalol. Possible side-effects are tiredness, dizziness, breathlessness or wheezing . They are generally avoided in people with asthma. • Calcium channel blockers such as diltiazem and verapamil. Possible side-effects are flushing, ankle swelling and constipation. They are generally avoided in people with poor heart pump function or heart failure. • Digoxin alone used to be the most common treatment for AF. In injection form, it can help to slow the heart rate quickly. Nowadays it is most often used in combination with either beta-blockers or calcium channel blockers to improve heart rate control. Anticoagulation The risk of clot formation is high if AF occurs in association with an acute illness such as a heart attack or serious infection. In these circumstances, blood thinning heparin injections are given into the skin around the lower abdomen. If the heart has been in AF for longer than 2 days, warfarin in tablet form is started to prevent new clots developing and help any clots already present to dissolve while the heart rate is being slowed down. The drug blocks the action of vitamin K which is required by the liver for making clotting factors. Warfarin takes several days to become effective and this is measured by a standardised blood test called the ‘international normalised ratio’ or ‘INR’. The normal level in a well person not on warfarin is 1. The aim is to achieve an INR between 2 and 3. The correct dose varies from person to person, over time and can be affected by different foods and alcohol. Therefore regular blood checks are necessary and are generally performed in a special anticoagulation or warfarin clinic with the result and recommended daily dose recorded in a yellow booklet. If the INR is too low, the risk of clots and stroke remain high. If the INR is too high, then there is a much higher risk of internal bleeding. Warfarin is avoided if there is a high risk of bleeding due to stomach ulcers, chronic liver disease, unexplained anaemia or a high risk of falls or confusion. After a stroke, starting warfarin is best delayed for at least 2 weeks. Patients with AF who have had a previous stroke or mini-stroke, underlying heart disease (especially heart failure or valve disease), diabetes or over 65 years of age are at increased risk of clots and strokes. Warfarin is often continued lifelong in these patients even if normal regular sinus rhythm is restored because there is a high likelihood of AF occurring again without warning (see cardioversion below). Aspirin is another drug which blocks the action of platelets in the blood. It can be used to reduce the development of clots but is much less effective than warfarin, especially in high clot and stroke risk patients. Whereas warfarin © Dr Winston Martin January 2007 - Information accurate at time of going to print. Darent Valley Hospital, Darenth Wood Road, Dartford, Kent , DA2 8DA - Telephone: 01322 428100 - www.dvh.nhs.uk 2 reduces the yearly risk of stroke by 2/3rds, aspirin reduces the risk by less than 1/3rd. Aspirin is suitable for patients aged 60-65 years without high risk features. It is often given with a stomach protecting agent e.g. omeprazole or lansoprazole to reduce the risk of stomach ulcers. Clopidogrel, is another antiplatelet agent. Studies however have shown that it is not an effective alternative used on its own or in combination with aspirin and is associated with an increased risk of internal bleeding. The decision regarding the choice of blood thinning medication requires careful assessment of the clot and stroke risk and discussion between the patient and specialist doctor regarding the risks and benefits of treatment. Any decision may also need to be reviewed from time to time if circumstances change and as the patient gets older. Cardioversion If the AF is of sudden onset, then normal heart rhythm may return by itself within several hours especially if any underlying acute illness is treated. Where this does not occur spontaneously, restoration of normal sinus rhythm by other means is desirable, if possible. This is normally achieved by the use of drugs, electric shock treatment or a combination of both of these. Helpful drugs include beta-blockers, flecainide, propafenone and amiodarone. In AF of sudden onset, these drugs may be given by injection or by mouth to restore sinus rhythm quickly. cardioversion Electrical cardioversion performed under a shortacting general anaesthetic is used in two circumstances: • As an emergency treatment where the patient has very low blood pressure as a result of AF • As a planned daycase procedure where normal sinus rhythm has not been restored by drugs. If treatment with blood thinning injections is started within 48 hours of AF onset, then cardioversion can be performed before leaving hospital. Otherwise, it is best delayed for at least 4 weeks to ensure that any possible clots in the heart have dissolved. Although cardioversion is generally effective, it does not work in some patients, especially those who have been in AF a long time, are very overweight, have underlying heart disease or the very elderly. Unfortunately even in those that do convert initially, there is a fairly high risk of AF occurring again – 40-50% in the first year. It is for this reason that warfarin is often continued for at least a few months after a successful cardioversion. Where cardioversion is not successful, a repeat attempt with prior loading with amiodarone or sotalol is sometimes tried if restoring sinus rhythm is very desirable as in severe heart failure. There is however no benefit in many repeated attempts; treatment should then focus on achieving good rate control. Maintenance of sinus rhythm For patients who suffer with episodic or paroxysmal AF or in patients after a successful cardioversion, it is often helpful to use drugs to improve the chances of the heart staying in sinus rhythm. Agents such as beta-blockers, calcium channel blockers, flecainide, propafenone and amiodarone are used alone or sometimes in careful combination. Amiodarone is the most effective drug for maintaining sinus rhythm but can cause a number of side-effects in the long term especially if used at high dose. These sideeffects include: thyroid function abnormalities, liver inflammation, numbness or ‘pins & needles’, lung scarring, glaring of vision in bright light and increased skin sensitivity to sunlight. Use of high factor sunscreen lotion, sunglasses and hat are recommended especially during the summer months. Regular yearly blood checks on thyroid and liver function are recommended. Importantly, amiodarone affects the action of warfarin and digoxin and the doses of these often need to be reduced to prevent side-effects. Drug therapy unfortunately rarely provides a complete ‘cure’ and at best reduces the frequency, severity and duration of palpitations helping the patient to continue or return to normal activities as quickly as possible. © Dr Winston Martin January 2007 - Information accurate at time of going to print. Darent Valley Hospital, Darenth Wood Road, Dartford, Kent , DA2 8DA - Telephone: 01322 428100 - www.dvh.nhs.uk 3 Invasive therapies Over recent years, newer more invasive techniques termed ablation have been developed which offer the prospect of ‘curing’ AF palpitations. These involve introducing long electrodes via the veins at the top of the legs into the heart and cauterising or burning specific spots or foci of abnormal electrical activity or creating tracks to isolate or block them. Because of the risk of heart injury with ablation treatments, they are generally only considered if drug therapy has failed to control symptoms effectively, and are better suited to treating episodic or paroxysmal AF rather than persistent or permanent AF. Anti-arrhythmic drugs can hopefully be stopped after a successful procedure, however aspirin or warfarin are generally continued longterm as the risk of clots and stroke still persists. Summary AF is common and can present with a variety of symptoms or be identified on medical examination or on an ECG. There are various types and causes of AF. Most patients with AF are treated successfully with a combination of drugs which are used to reduce symptoms and reduce the risks of clot formation, stroke and heart failure. Newer minimally invasive ablation techniques are being used increasingly to prevent symptomatic palpitations. © Dr Winston Martin January 2007 - Information accurate at time of going to print. Darent Valley Hospital, Darenth Wood Road, Dartford, Kent , DA2 8DA - Telephone: 01322 428100 - www.dvh.nhs.uk 4