* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download How are the respiratory and circulatory system connected?
Survey
Document related concepts
Transcript
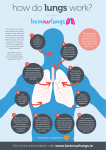
How are the respiratory and circulatory system connected? Organs of the respiratory system • Nose-internal hairs and mucus pick up unwanted materials – FYI-remember anthrax? Those particles are small enough to get past these hairs – This bacteria releases toxins that cause death • Sinuses-reduce weight of skull and effect voice quality • Pharynx-throat (food travels from mouth to esophagus) produces sounds of speech • Larynx-conducts air in and out of trachea and prevents foreign objects from entering the trachea; houses vocal cords (made of muscle and elastic fibers) • Trachea-windpipe; split into the left and right bronchi • Bronchial tree-tubes leading into the air sacs – Bronchi – Bronchioles – Alveolar sacs (made of alveoli) • Lungs-contain air passages and alveoli – Right is bigger than the left. Inspiration vs. Expiration Inspiration • Pressure is low in lungs and alveoli • Atmospheric pressure pushes outside air INTO airways • Diaphragm contracts and moves down • Lungs expand to fill with air Expiration • Increase in lung and alveoli pressure • Atmospheric pressure pushes air OUT of the airways • Diaphragm relaxes and pushes back to position (moves up) • Air moves out of lungs • Returning to original shape Respiratory Air Volume and Capacities • Respiratory cycle-1 inspiration and 1 expiration • 4 distinct air volumes – Tidal volume-air that moves in (or out) during a single respiratory cycle (500 mL) – Inspiratory reserve volume-extra volume that enters during forced inspiration (3000 mL) – Expiratory reserve volume-extra volume that is forced out (1100 mL) – Residual volume-left over volume after maximal expiration • Vital capacity-maximum amount of air a person can exhale after taking the deepest breath possible – IRV + TV + ERV • Inspiratory capacity-maximum volume of air a person can inhale following exhalation of the tidal volume – TV + IRV • Functional residual capacity-volume of air that remains in the lungs after a person exhales the tidal volume • Total Lung Capacity-Vital capacity + residual volume What controls breathing? • Pons and medulla oblongata -The inspiratory area determines the basic rhythm and is also responsible for the contraction of the diaphragm. -The expiratory center is usually inactive during normal respiration, however during forceful expiration e.g. during exercise, it is activated by nerve impulses from the inspiratory area. muscles, resulting in a forced expiration. • Pneumotaxic area regulates breathing rate. – Part of the pons – Helps to facilitate expiration. Factors that control breathing • Chemoreceptors – Stimulate these and increase breathing – Stimulated by blood concentration of carbon dioxide and hydrogen ions • Chemoreceptors in arterial walls – Sense low oxygen concentration • Overstretching of lungs triggers an inflation reflex. – Prevent overinflation of lungs Gas Exchange in the Lungs Alveolar Gas Exchange • Respiratory membrane-two layers of epithelial cells and a basement membrane that separates the blood from the alveolar gases • Gases move due to partial pressure • Oxygen and carbon dioxide move from high pressure to a low pressure-diffusion – Many factors effect this: surface area and solubility of gases (emphysema reduce the surface area so oxygen isn’t exchanged as well) Gas Transport-Oxygen • Oxygen that blood transports is attached to hemoglobin (iron containing protein)-forms oxyhemoglobin – They do not form a strong bond so hemoglobin releases oxygen easily so it can diffuse into the cells • RELEASES IN AREAS WHERE PRESSURE OF OXYGEN IS LOW (diffusion) – How much oxygen will oxyhemoglobin release? • Carbon dioxide levels increases • Blood temperature increases • pH of blood decrease (acid) • Hypoxia-deficiency of blood in the tissues – Decreased arterial pressure (hypoxemia), inadequate blood flow (ischemic hypoxia), lack ability to transport blood (anemic hypoxia), or a defect at the cell Gas Transport-Carbon Dioxide • Transported back to the lungs as: dissolved in plasma (7%), binds to hemoglobin, form of bicarbonate ion • Bind with hemoglobin called carbaminohemoglobin (23%) • Most common form-bicarbonate ion (70%) – Carbon dioxide reacts with water to form carbonic acid (carbonic anhydrase speeds this up) – This will dissociate to form H+ and bicarbonate ions • At the lungs, dissolved carbon dioxide enters the alveoli; bicarbonate ion and hydrogen recombine to form carbonic acid but quickly breaks down into carbon dioxide and water What do we breathe out? BREATHE OUT • 4-5% is Carbon dioxide • 17-18% is oxygen • 74.9% is inert nitrogen gas • 6.2% is water • • • • • BREATHE IN 21% oxygen 0.04% carbon dioxide 78% nitrogen 0.5% water How does smoking effect this? • The normal percent of hemoglobin that bind to CO (carbon monoxide) is 2% • Smokers may exceed 20% • Increased levels prevent oxygen from binding, starving tissues of oxygen, and causing chest pains, shortness of breath, fatigue, confusion, and abnormal heart rhythm Common disorders • Asthma-destruction of airwayss • Emphysema• Bronchitisalveolar walls lose inflammation of the elasticity and bronchi remained filled • Pneumoniawith air during infection or exhale (lungs inflammation of become alveoli/fill up with permanently fluid and dead wbc inflated) Common disorder • Tuberculosis-caused by bacteria (mycobacterium tuberculosis); destroys lung tissue and is replaced by tough fibrous tissue • Lung cancer-bronchogenic carcinoma – Starts in bronchial walls – Goblet cells get bigger and secrete more mucus – Other cells divide and take up more space