* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Blood and Immunity
Embryonic stem cell wikipedia , lookup
Homeostasis wikipedia , lookup
Cell culture wikipedia , lookup
Hematopoietic stem cell wikipedia , lookup
Human embryogenesis wikipedia , lookup
Artificial cell wikipedia , lookup
Microbial cooperation wikipedia , lookup
Neuronal lineage marker wikipedia , lookup
State switching wikipedia , lookup
Cell theory wikipedia , lookup
Human genetic resistance to malaria wikipedia , lookup
Organ-on-a-chip wikipedia , lookup
List of types of proteins wikipedia , lookup
Developmental biology wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
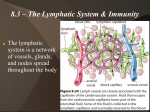
Blood Complex Transport Mixture • Connective Tissue (4-6 liters/person) • Maintains Homeostasis – Water / Electrolyte Balance – Ph Balance – Temperature Regulation • Transport Medium – Nutrients/ Wastes – Gases: Oxygen/Carbon dioxide – Hormones, Antibodies – Red Blood Cells, White Blood Cells – Clotting Factors and Platelets Figure 37-7 Blood Blood Section Components: Red Blood Cells, White Blood Cells 37-2 Platelets and Plasma Plasma Platelets White blood cells Red blood cells Whole Blood Sample Sample Placed in Centrifuge Spin to separate plasma from cellular components Blood Sample That Has Been Centrifuged Blood Composition Red Blood Cells / White Blood Cells Plasma: Liquid Portion Together= Blood Platelets: cell fragements Necessary for normal blood clotting Blood Components • Plasma (55%) Liquid portion – – – – – – – 90% Water Proteins Salts (Electrolytes) Nutrients (glucose, amino acids, fats, vitamins) Hormones Antibodies Cellular Wastes (Carbon dioxide, Urea) • Cellular Elements – Red Blood Cells (erythrocytes) • Contain Hemoglobin, carry oxygen – White Blood Cells (leukocytes) • – Defend body from infection/disease • Phagocytes (eat invaders) • Lymphocytes • (B ) Make antibodies and “Killer” Ts Platelets (cell fragments) • Blood Clotting Plasma: Liquid Portion • Straw-colored liquid (90% water) • 10% Dissolved substances – Salts – Nutrients: Sugars, dissolved fats, amino acids – Plasma proteins: clotting factors, transport proteins – Hormones (chemical messengers) – Antibodies (immune response) – Cellular Wastes Red Blood Cells (Erythrocytes) • Contain Hemoglobin (red pigment) that binds with Oxygen (250 million/RBC) • Delivers Oxygen to All body cells • Biconcave Disks • No nucleus • Most abundant of all blood cells • Made in Bone Marrow Platelets: Tiny cell Fragments • Formed in the Bone Marrow • Small pieces of Megakaryocytes break – off and enter the blood circulation • Platelets carried by blood to sites of injury • Release proteins and clotting factors • Forming Blood clots Figure 37-10 Blood Clotting Platelets go to site of injury, form a fibrin net/ ”plug” Clot Forms -- prevents blood loss from site Break in Capillary Wall Blood vessels injured. Clumping of Platelets Platelets clump at the site and release thromboplastin. Thromboplastin converts prothrombin into thrombin.. Clot Forms Thrombin converts fibrinogen into fibrin, which causes a clot. The clot prevents further loss of blood.. Platelets Form a Fibrin Net to form Clots “Fighting the Enemy Within” phagocytic leukocyte Immune System lymphocytes attacking cancer cell lymph system Why an immune system? • Attack from the outside & inside – lots of organisms want you for lunch! – we are a tasty vitamin-packed meal • cells are packages of proteins, carbohydrates & fats • no cell wall – animals must defend themselves against invaders • viruses – HIV, flu, cold, measles, chicken pox, SARS • bacteria – pneumonia, meningitis, tuberculosis • fungi – yeast • protists – amoeba, Lyme disease, malaria – cancer cells • abnormal body cells What’s for lunch?! Pathogens and Disease Section 40-1 Pathogen Types Viruses Bacteria Common cold Influenza Chicken pox Agent That Causes Disease Rhinovirus Two types (A, B), plus subtypes Varicella Measles Paramyxovirus Tuberculosis Meningitis Mycobacterium tuberculosis Neisseria meningitidis Vibrio cholerae Clostridium tetani Trypanosoma Disease Cholera Tetanus African sleeping Protists sickness Malaria Amoebic dysentery Worms Schistosomiasis Beef tapeworm Fungi Athlete’s foot Ringworm Plasmodium Entamoeba histolytica Schistosom a Taenia saginata Imperfect fungi Imperfect fungi Method of Transmission Airborne; direct contact with infected person Airborne; droplet infection; direct contact with infected person Airborne; direct contact with infected person Droplets in air; direct contact with secretions of infected person Droplets in air; contaminated milk and dairy products Direct contact with a carrier Contaminated drinking water Contaminated wound; usually puncture wound Spread by tsetse fly Spread by Anopheles mosquitoes Contaminated drinking water Freshwater streams and rice paddies Contaminated meat Contact with infected person Exchange of hats, combs, or athletic head gear with infected person How are invaders recognized? • Antigens – chemical name tags on the surface of every cell • “self” vs. “invader” one of your own cells disease-causing virus disease-causing bacteria antigens say: “I belong here” antigens say: “I am an invader” antigens say: “I am an invader” The Immune System: Lines of Defense Against Disease Nonspecific Defenses 1. 2. 3. First Line of Defense Second Line of Defense Interferon Specific Defenses 1. 2. 3. C. D. B- cells T-Cells Permanent Immunity Active Immunity Passive Immunity Nonspecific Defenses: Include 1st and 2nd Lines • First Line: BARRIERS: Prevent Pathogens from entering body – Skin (largest organ)- Physical barrier; oil & sweat glands create acidic environment – killing many pathogens – Mucus in Nose and Throat – traps bacteria and viruses and using cilia push away from entering lungs – Acids and Digestive enzymes in stomach destroy many pathogens – Tears, Saliva, sweat contain Lysozymes 37-9 Our Types Body’s of White Blood Cells White BloodFigure Cells: Defenders When pathogens get past barriers, Section 37-2 WBCs “Get Involoved” Function Cell Type Neutrophils Eosinophils Basophils Monocytes Lymphocytes Engulf and destroy small bacteria and foreign substances Attack parasites; limit inflammation associated with allergic reactions Release histamines that cause inflammation; release anticoagulants, which prevent blood clots Give rise to leukocytes that engulf and destroy large bacteria and substances Some destroy foreign cells by causing their membranes to rupture; some develop into cells that produce antibodies, which target specific foreign substances Neutrophil Monocyte Basophil Lymphocyte Eosinophil Phagocytes macrophage bacteria white blood cells that eat macrophage yeast The Inflammatory Response: Second Line of Defense Section 40-2 Nonspecific Response to Tissue Damage Skin Wound Phagocytes move into the area and engulf the bacteria and cell debris Bacteria enter the wound Capillary Injured cells signal capillaries to expand, become “leaky”, allowing more Phagocytic WBCs to arrive along with Platelets to Patch injury 3rd Line/Specific Defenses: “Immune Response” • If pathogens get past the 2nd level of defense, and enter cells or blood, then the 3rd line of defense is alerted! • Antigens are protein “markers” on cell surfaces. “Foreign” antigens are considered a threat • Note: Antigens are found on all cells and viruses; our Lymphocytes attack antigens that are seen as “non-self” Types of Lymphocytes • B Lymphs (B-cells) • Make ANTIBODIES – “custom made” , Yshaped Proteins that bind to and help destroy foreign antigens (pathogens) – Mature B-cells reside and multiply in our lymph nodes – Memory B-cells always remember the pathogen • T Lymphs (T-cells) • Helper T; – Activate B-cells to produce antibodies – Activate Killer-T cells (recognize pathogen and divide) • Killer T; – Tears open cells infected with pathogens; destroying the cell and pathogens inside Structure of an Antibody Section 40-2 Antigenbinding sites Note: An Antibody “fits” only one specific Antigen; all antibodies are “custom made” Antigen Antibody Antibodies • Proteins made by B cells that tag invaders in the blood so macrophages can eat them – tag says “this is an invader” gotcha! • biological “handcuffs” – antibody attaches to antigen on invader B cells releasing antibodies Y Y Y Y Y Y Y invading germs tagged with antibodies Y Y Y Y Y Y macrophage eating tagged invaders The Lymphatic System: Network of thin-walled vessels that collect and filter the fluid seeping out of our Blood vessels. Lymph nodes, swellings in lymphatic vessels, contain lymphocytes Superior vena cava Thymus Heart Thoracic duct Spleen Lymph nodes Lymph vessels B- Lymphs: Immune Response Section 40-2 Bacteria With Antigens on Surface Bacterial antigens also stimulate B cells A large phagocyte called a macrophage engulfs a bacterium T cell Macrophage Antigens are displayed on surface of macrofage after digestion of bacterium B cell T cell binds to activated macrophage Helper T cell assists the activated B cell to develop into an antibodyproducing plasma cell T cell, activated by macrophage, becomes a helper T cell Active B cells proliferate to produce clones of memory cells Plasma cell produces large amounts of antibody proteins, released into the bloodstream Circulating antibodies bind to bacterial antigens, helping other immune cells to identify and destroy bacteria Humoral Immunity Section 40-2 Macrophage T-Cell Immune Response T cell binds to activated macrophage Helper T cell activates killer T cells and B cells Helper T Cell Killer T Cell T Cell Antigens are displayed on surface of macrophage T cell, activated by macrophage, becomes a helper T cell Cell-Mediated Immunity Infected Cell Killer T cells bind to infected cells, disrupting their cell membranes and destroying them Antibody Concentration Section 40-2 Primary and Secondary Immune Responses Interval between exposures First exposure Second exposure Provides Permanent Immunity to pathogen Time Memory B-cells respond quickly if re-exposed to a pathogen by Producing large numbers of antibodies (protecting us from disease) How Can We Avoid Diseases? •In the United States, babies and small children are usually given a series of vaccines, which protect them from many infectious diseases. • A vaccine is an injection of a weakened or mild form of a pathogen. People may also receive vaccines against certain diseases later in their lives. Vaccination results in Active Immunity without the Risk • Receiving dead, weakened or parts of a pathogen stimulates our immune system • B lymphocytes ACTIVELY produce antibodies and MEMORY CELLS • When ever WE make our own antibodies and memory cells (for future protection), it’s called ACTIVE IMMUNITY Vaccinations • Exposure to harmless version of germ (pathogen) – stimulates immune system to produce antibodies to invader – rapid response if future exposure • Most successful against viral diseases Passive Immunity: Antibodies Given to Us Don’t Last Long • Mothers provide passive immunity to their babies • Antibodies made by mom are passed to babies in breast milk • The baby will only be protected while receiving milk (short-term) • Injected antibodies made by others will provide only short term protection • Borrowed antibodies are destroyed within weeks • Considered passive because our immune system did not make them Immune System Disorders • Allergies: Exaggerated response to – non pathogenic Antigens (pollen, food, etc) Histamines cause • • • running nose, eyes Itching and swelling Anaphylactic Shock B. Autoimmune Disease: Immune system mistakenly attacks own body cells – – – – MS (Multiple Sclerosis)-destruction of myelin sheathing of nerves Myasthenia gravis – antibodies attack nerve receptors of the muscles Juvenile-onset diabetes- antibodies attack insulin-producing cells of pancreas Rheumatoid Arthritis Immune system malfunctions • Allergies – over-reaction to harmless compounds • allergens – proteins on pollen – proteins from dust mites – proteins in animal saliva • body mistakenly thinks they are attackers Immune system malfunctions • Auto-immune diseases – immune system attacks own cells • lupus – antibodies attack many different body cells • rheumatoid arthritis – antibodies causing damage to cartilage & bone • diabetes – beta-islet cells of pancreas attacked & destroyed • multiple sclerosis – T cells attack myelin sheath of brain & spinal cord nerves Autoimmune Disease • Rheumatoid Arthritis Immunodeficiency Diseases • People lack one or more parts of the immune system or it is defective • Rendering them susceptible to infections that ordinarily cause no problems – SCID (Severe Combined Immunodeficiency)deficit in both B and T cells – AIDS (Acquired immunodeficiency Syndrome) caused by HIV, a virus that occupies and suppresses Helper T-cell function • Death results from the inability to fight other infections Stages of HIV Infection As T-cell concentration goes down, HIV concentration goes up Infection; Immune system eliminates most of HIV Symptoms, such as swollen lymph nodes, are few Loss of immune function more Almost apparent; appearance total loss of characteristic of cellular diseases such as immunity; yeast infections AIDS Relative HIV concentration T cell concentration Years HIV interferes with normal Helper-T function (does not recognize HIV as an Invader) In turn, does not activate B-cells and Killer T-cells Blood Transfusions Section 37-2 Blood Transfusion: Applying Our knowledge of Antigen-Antibody interaction to Medicine Blood Type of Donor Antigens on Cells Blood Type of Recipient Antigens on Recipient’s cells A B AB O A B AB O Unsuccessful transfusion Successful transfusion Recall: We will make antibodies AGAINST Non-Self Antigens