* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Basic Pacing Concepts
Coronary artery disease wikipedia , lookup
Heart failure wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Cardiac surgery wikipedia , lookup
Myocardial infarction wikipedia , lookup
Atrial fibrillation wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
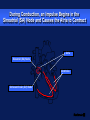
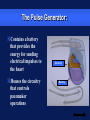
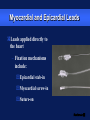
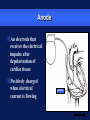
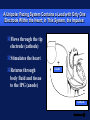
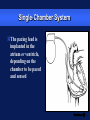
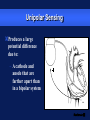
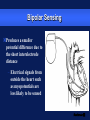
Basic Pacing Concepts The Heart Has an Intrinsic Pacemaker The heart generates electrical impulses that travel along a specialized conduction pathway This conduction process makes it possible for the heart to pump blood efficiently During Conduction, an Impulse Begins in the Sinoatrial (SA) Node and Causes the Atria to Contract Atria Sinoatrial (SA) Node Ventricles Atrioventricular (AV) Node Then, the Impulse Moves to the Atrioventricular (AV) Node and Down the Bundle Branches, Which Causes the Ventricles to Contract Atria SA node Ventricles AV node Bundle branches Diseased Heart Tissue May: Prevent impulse generation in the SA node SA node Inhibit impulse conduction AV node Implantable Pacemaker Systems Contain the Following Components: Lead wire(s) Implantable pulse generator (IPG) Pacemaker Components Combine with Body Tissue to Form a Complete Circuit Pulse generator: power source or battery Lead Leads or wires Cathode (negative electrode) Anode (positive electrode) Body tissue IPG Anode Cathode The Pulse Generator: Contains a battery that provides the energy for sending electrical impulses to the heart Houses the circuitry that controls pacemaker operations Circuitry Battery Leads Are Insulated Wires That: Deliver electrical impulses from the pulse generator to the heart Sense cardiac depolarization Lead Types of Leads Endocardial or transvenous leads Myocardial/Epicardial leads Transvenous Leads Have Different “Fixation” Mechanisms Passive fixation – The tines become lodged in the trabeculae (fibrous meshwork) of the heart Transvenous Leads Active Fixation – The helix (or screw) extends into the endocardial tissue – Allows for lead positioning anywhere in the heart’s chamber Myocardial and Epicardial Leads Leads applied directly to the heart – Fixation mechanisms include: Epicardial stab-in Myocardial screw-in Suture-on Cathode An electrode that is in contact with the heart tissue Negatively charged when electrical current is flowing Cathode Anode An electrode that receives the electrical impulse after depolarization of cardiac tissue Positively charged when electrical current is flowing Anode Conduction Pathways Body tissues and fluids are part of the conduction pathway between the anode and cathode Anode Tissue Cathode During Pacing, the Impulse: Begins in the pulse generator Flows through the lead and the cathode (–) Stimulates the heart Returns to the anode (+) Impulse onset * A Unipolar Pacing System Contains a Lead with Only One Electrode Within the Heart; In This System, the Impulse: Flows through the tip electrode (cathode) Stimulates the heart Returns through body fluid and tissue to the IPG (anode) + Anode Cathode A Bipolar Pacing System Contains a Lead with Two Electrodes Within the Heart. In This System, the Impulse: Flows through the tip electrode located at the end of the lead wire Stimulates the heart Returns to the ring electrode above the lead tip Anode Cathode Unipolar and Bipolar Leads Unipolar leads Unipolar leads may have a smaller diameter lead body than bipolar leads Unipolar leads usually exhibit larger pacing artifacts on the surface ECG Bipolar leads Bipolar leads are less susceptible to oversensing noncardiac signals (myopotentials and EMI) Coaxial Lead Design A Brief History of Pacemakers Single-Chamber and Dual-Chamber Pacing Systems Single-Chamber System The pacing lead is implanted in the atrium or ventricle, depending on the chamber to be paced and sensed Advantages and Disadvantages of Single-Chamber Pacing Systems Advantages Disadvantages Implantation of a single lead Single ventricular lead does not provide AV synchrony Single atrial lead does not provide ventricular backup if A-to-V conduction is lost Dual-Chamber Systems Have Two Leads: One implanted in both the atrium and the ventricle Most Pacemakers Perform Four Functions: Stimulate cardiac depolarization Sense intrinsic cardiac function Respond to increased metabolic demand by providing rate responsive pacing Provide diagnostic information stored by the pacemaker Every Electrical Pacing Circuit Has the Following Characteristics: Voltage Current Impedance Impedance Changes Affect Pacemaker Function and Battery Longevity High impedance reading reduces battery current drain and increases longevity Low impedance reading increases battery current drain and decreases longevity Impedance reading values range from 300 to 1,000 W – High impedance leads will show impedance reading values greater than 1,000 ohms Lead Impedance Values Will Change Due to: Insulation breaks Wire fractures An Insulation Break Around the Lead Wire Can Cause Impedance Values to Fall Insulation breaks expose the wire to body fluids which have a low resistance and cause impedance values to fall Current drains through the insulation break into the body which depletes the battery An insulation break can cause impedance values to fall below 300 W Insulation break Decreased resistance A Wire Fracture Within the Insulating Sheath May Cause Impedance Values to Rise Impedance values across a break in the wire will increase Current flow may be too low to be effective Impedance values may exceed 3,000 W Lead wire fracture Increased resistance Stimulation Stimulation Threshold The minimum electrical stimulus needed to consistently capture the heart outside of the heart’s refractory period Capture VVI / 60 Non-Capture Two Settings Are Used to Ensure Capture: Amplitude Pulse width Amplitude is the Amount of Voltage Delivered to the Heart By the Pacemaker Amplitude reflects the strength or height of the impulse: – The amplitude of the impulse must be large enough to cause depolarization ( i.e., to “capture” the heart) – The amplitude of the impulse must be sufficient to provide an appropriate pacing safety margin Pulse Width Is the Time (Duration) of the Pacing Pulse Pulse width is expressed in milliseconds (ms) The pulse width must be long enough for depolarization to disperse to the surrounding tissue 5V 0.5 ms 0.25 ms 1.0 ms The strength-duration curve illustrates the relationship of amplitude and pulse width – Values on or above the curve will result in capture Stimulation Threshold (Volts) The Strength-Duration Curve 2.0 1.5 1.0 Capture .50 .25 0.5 1.0 Duration Pulse Width (ms) 1.5 Adequate safety margins must be achieved due to: – Acute or chronic pacing system – Daily fluctuations in threshold Stimulation Threshold (Volts) Clinical Usefulness of the Strength-Duration Curve 2.0 1.5 1.0 Capture .50 .25 0.5 1.0 Duration Pulse Width (ms) 1.5 Electrode Design May Also Impact Stimulation Thresholds Lead maturation process Lead Maturation Process Fibrotic “capsule” develops around the electrode following lead implantation Sensing Sensing Sensing is the ability of the pacemaker to “see” when a natural (intrinsic) depolarization is occurring – Pacemakers sense cardiac depolarization by measuring changes in electrical potential of myocardial cells between the anode and cathode A Pacemaker Must Be Able to Sense and Respond to Cardiac Rhythms Accurate sensing enables the pacemaker to determine whether or not the heart has created a beat on its own The pacemaker is usually programmed to respond with a pacing impulse only when the heart fails to produce an intrinsic beat Accurate Sensing... Ensures that undersensing will not occur – the pacemaker will not miss P or R waves that should have been sensed Ensures that oversensing will not occur – the pacemaker will not mistake extra-cardiac activity for intrinsic cardiac events Provides for proper timing of the pacing pulse – an appropriately sensed event resets the timing sequence of the pacemaker Accurate Sensing is Dependent on . . . The electrophysiological properties of the myocardium The characteristics of the electrode and its placement within the heart The sensing amplifiers of the pacemaker Unipolar Sensing Produces a large potential difference due to: – A cathode and anode that are farther apart than in a bipolar system _ Bipolar Sensing Produces a smaller potential difference due to the short interelectrode distance – Electrical signals from outside the heart such as myopotentials are less likely to be sensed Electromagnetic Interference Electromagnetic Interference (EMI) Interference is caused by electromagnetic energy with a source that is outside the body Electromagnetic fields that may affect pacemakers are radio-frequency waves – 50-60 Hz are most frequently associated with pacemaker interference Few sources of EMI are found in the home or office but several exist in hospitals EMI May Result in the Following Problems: Oversensing Transient mode change (noise reversion) Reprogramming (Power on Reset or “POR”) Oversensing May Occur When EMI Signals Are Incorrectly Interpreted as P Waves or R Waves Pacing rates will vary as a result of EMI: – Rates will accelerate if sensed as P waves in dual-chamber systems (P waves are “tracked”) – Rates will be low or inhibited if sensed in single-chamber systems, or on ventricular lead in dual-chamber systems New technologies will continue to create new, unanticipated sources of EMI: Cellular phones (digital) Sources of EMI Are Found Most Commonly in Hospital Environments Sources of EMI that interfere with pacemaker operation include surgical/therapeutic equipment such as: – Electrocautery – Transthoracic defibrillation – Extracorporeal shock-wave lithotripsy – Therapeutic radiation – RF ablation – TENS units – MRI Sources of EMI Are Found More Rarely in: Home, office, and shopping environments Industrial environments with very high electrical outputs Transportation systems with high electrical energy exposure or with high-powered radar and radio transmission – Engines or subway braking systems – Airport radar – Airplane engines TV and radio transmission sites Rate Responsive Pacing Rate Responsive Pacing When the need for oxygenated blood increases, the pacemaker ensures that the heart rate increases to provide additional cardiac output Adjusting Heart Rate to Activity Normal Heart Rate Rate Responsive Pacing Fixed-Rate Pacing Daily Activities Rate Response Rate responsive (also called rate modulated) pacemakers provide patients with the ability to vary heart rate when the sinus node cannot provide the appropriate rate Rate responsive pacing is indicated for: – Patients who are chronotropically incompetent (heart rate cannot reach appropriate levels during exercise or to meet other metabolic demands) – Patients in chronic atrial fibrillation with slow ventricular response Rate Responsive Pacing Cardiac output (CO) is determined by the combination of stroke volume (SV) and heart rate (HR) SV X HR = CO Changes in cardiac output depend on the ability of the HR and SV to respond to metabolic requirements Rate Responsive Pacing SV reserves can account for increases in cardiac output of up to 50% HR reserves can nearly triple total cardiac output in response to metabolic demands A Variety of Rate Response Sensors Exist Those most accepted in the market place are: – Activity sensors that detect physical movement and increase the rate according to the level of activity – Minute ventilation sensors that measure the change in respiration rate and tidal volume via transthoracic impedance readings Rate Responsive Pacing Activity sensors employ a piezoelectric crystal that detects mechanical signals produced by movement The crystal translates the mechanical signals into electrical signals that in turn increase the rate of the pacemaker Piezoelectric crystal Rate Responsive Pacing Minute Ventilation (MV) is the volume of air introduced into the lungs per unit of time MV has two components: – Tidal volume–the volume of air introduced into the lungs in a single respiration cycle – Respiration rate–the number of respiration cycles per minute Rate Responsive Pacing Minute ventilation can be measured by measuring the changes in electrical impedance across the chest cavity to calculate changes in lung volume over time Rate Responsive Pacing Adjusting Heart Rate to Activity Normal Heart Rate Rate Responsive Pacing Fixed-Rate Pacing Daily Activities PACING FUTURE !!??