* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Page 1
Psychopharmacology wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Orphan drug wikipedia , lookup
Polysubstance dependence wikipedia , lookup
Plateau principle wikipedia , lookup
Compounding wikipedia , lookup
Neuropharmacology wikipedia , lookup
Pharmacognosy wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Prescription costs wikipedia , lookup
Drug design wikipedia , lookup
Drug discovery wikipedia , lookup
Theralizumab wikipedia , lookup
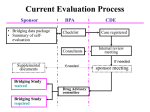
Pharmacokinetics and Pharmacodynamics Pharmacokinetic Phase Overview Pharmacokinetics Absorption Distribution Metabolism Excretion Dose Carrie K. K Jones Department of Pharmacology Vanderbilt Program in Drug Discovery Pharmacodynamic Phase Blood Receptor interaction Concentration & Receptor response Preclinical or Clinical ec Effect Pharmacokinetics: study of drug disposition-all processes by which the body handles foreign chemicals including drugs (i.e. ADME) “what body does to the drug” Resources: 1. Gibson and Skett (2001) Introduction to Drug Metabolism, Nelson Thornes Publishers 2. Donald J. Burkett, (2002) Pharmacokinetics Made Easy McGraw-Hill Austarlia Pty Ltd 3. Slides adapted from DMPK lectures given Joseph Awad, MD Pharmacodynamics: relationship between unbound (‘free’) drug concentration at the receptor and the drug response (i.e. therapeutic effect) “what drug does to the body” Bioavailability Overview of Drug Disposition A – Absorption: Passage of drug from site of administration to circulation D – Distribution: Distribution of drug from plasma to organs, tissues, etc…biophase M – Metabolism: Conversion of xenobiotics into water soluble derivatives; liver E – Excretion: Elimination of drugs & metabolites with adequate kinetics • Slow elimination leads to drug/metabolite accumulation and toxicity • Rapid elimination requires repeated dosing • Routes: renal, rectal, pulmonary, oral, cutaneous y Mutagenic, g , tetragenic g and ggeneral toxicity y of drug g and metabolites. ***T – Toxicity: Bioavailability is a measurement of the rate and extent of a therapeutically active drug that reaches the systemic circulation and is available at the site of action. Absolute bioavailability: comparison of bioavailability (estimated as the area under the curve, or AUC) of the active drug in systemic circulation following non-intravenous administration (i.e., after oral, rectal, transdermal, subcutaneous, sublingual administration), with bioavailability of the same drug following intravenous administration. I order In d tto determine d t i absolute b l t bi bioavailability il bilit off a d drug, a pharmacokinetic h ki ti study t d mustt be b done d tto obtain bt i a plasma drug concentration vs time plot for the drug after both intravenous (IV) and non-intravenous administration. The absolute bioavailability is the dose-corrected area under curve (AUC) non-intravenous divided by AUC intravenous. For example, the formula for calculating F for a drug administered by the oral route (po) is given below. ****Therefore, a drug given by the intravenous route will have an absolute bioavailability of 1 (F=1) while drugs given by other routes usually have an absolute bioavailability of less than one. Relative bioavailability: measures the bioavailability (estimated as area under the curve, or AUC) of a certain drug when compared with another formulation of the same drug, usually an established standard, or through administration via a different route. When the standard consists of intravenously administered drug, this is known as relative bioavailability. Page 1 1 Routes of Administration / Bioavailability Bioavailability • Factors affecting bioavailability > Route of administration • • Parenteral > > > > Intravenous (iv) Intramuscular (im) Subcutaneous (sc, sq) Intraperitoneal (ip) Alimentary > Oral (po) > Sublingual (sl) > per rectum (pr) Miscellaneous > Topical (skin or eye) > Inhalation > Spinal (it) Bioavailability Factors affecting bioavailability > Route of administration > Chemical properties of the drug » Rapid, accurate, ?toxic …control, but requires access …perfusion, depot …slower and longer …rare for clinical applications » Convenient, safer, cheaper …variable absorption …bypass liver …useful, but inconvenient » Special Uses …irritation, bypass liver …rapid, limitations …technically challenging Chemical Properties / Bioavailability • Most drugs must cross mucosal barriers. • Dependent on chemical properties of drug. • Passive processes: > filtration > diffusion diff i > carrier-facilitated transport (amino/nucleic acid-like drugs) • Active processes: > > > > > up a gradient, energy requiring protein transporter substrate specificity, susceptible to competition saturable neural membranes, choroid plexus, liver and kidney cells Page 2 2 Passive Diffusion • • • Lipid:Water Partition Accounts for most drug absorption Fick’s Law: dQ/dt = -D • A dC/dx > > > > • Lipid Solubility / Bioavailability Coefficient (log P) > e.g. Octanol:Water > Site of action discussion!!! dQ/dt - Quantity moving in time D - constant depending on Temp and MW A - surface area dC/dx - dependent on lipid solubility of drug • Ionization I i ti Eff Effects t > Ionized compounds have low lipid:water partition coefficient > Ionization status variable dependent on pH • Weak acids not ionized at low pH • Weak bases not ionized at high pH Absorption dependent on drug: > Molecular Weight (size) > Lipid Solubility • Absorption dependent on host: > Surface area [1000 HA - A Plasma pH=7.4 Gastric Juice pH=1.4 ] +H+ HA 7.0-7.5 4.3-4.7 3.4-4.2 • Aqueous Solubility 1001 Total [HA]+[A-] > Confounds effect of pH > Weak acids (+ other hydrophobic drugs) may not be well dissolved in stomach > Weak acids require special formulation Lipid Mucosal Barrier [1] Blood Mouth Stomach Duodenum Jejunum and Ileum Colon Sweat Vagina Nl pH Range 7.2-7.6 6.2-7.2 1.0-3.0 4.8-8.2 7.5-8.0 Chemical Properties / Bioavailability Example of Weak Acid Partition [1] Compartment • Chemical Stability [0.001 A - ] +H+ Weak acid with pKa of 4.4 > Survival of drug in acidic gastric environment > Intrinsic stability > Protected by formulation > Suppression of acid 1.001 [A-]/[HA]=10(pH-pKa) Page 3 3 Drug Formulation (Pharmaceutics) Bioavailability Factors affecting bioavailability • Disintegration of drug delivery system must be > Route of administration > Chemical properties of the drug > Formulation of the drug (Pharmaceutics) reliable. • Enteric coating - protection from gastric acidity • Controlled Controlled-release release preparations > reduce need for frequent dosing > complexity = greater interpatient variability > dose dumping > target drug to particular area • Bioequivalent • Pharmaceutical Equivalent Formulation for Preclinical Studies Bioavailability For systemic administration: ***must pH solution ~ 6.5-7.5 Sterile water Artificial CSF (cerebrospinal fluid) Saline (0.9% NaCl) 1N NaOH and water 8.5% lactic acid and water 10-20% BCD 10% solutol 10% Tween 80 10% Tween 20 *** no EtOH !!! Factors affecting bioavailability 10%-100% PEG 400 10% DMSO 0.5-1% methylcellulose 0.5% acacia > Route of administration > Chemical properties of the drug > Formulation of the drug (Pharmaceutics) > Metabolism-presystemic M b li i > Site of administration relative to site of metabolism ICV, IC, IT, or Direct Site administration: ***must pH solution ~ 6.5-7.5 Sterile water Artificial CSF (cerebrospinal fluid) Buffer saline (0.9% NaCl) 10-20% BCD Page 4 4 Metabolism / Bioavailability Pre-Systemic Clearance Systemic Circulation • Drug must enter circulation faster than • Hepatic Veins metabolized Sites of metabolism Hepatic Drug Transport and Metabolism > Liver > Intestine > Lung > Kidney ((bile)) Drug • Presystemic Clearance (“first pass” Portal Vein Metabolite metabolism) Intestinal Drug Transport and Metabolism CYP3A4 P-glycoprotein p.o. > PO dose >> IV > Interindividual variability greater Bioavailability <100% • Bioactivation - Prodrugs Biotransformation and Elimination Metabolism Basics • Drug Metabolism Phase I (Degradative) • Oxidation • Reduction • Hydrolysis* >Phase I >Phase II • Enterohepatic Circulation / Hepatic Elimination Phase II (Conjugative) Glucuronidation* Sulfation Acetylation/Methylation* Amino Acids • • • • > Glutathione > Glycine • Renal Excretion • Pulmonary Excretion/Metabolism • Placental Transfer • Breast Milk Exposes chemical groups appropriate for Phase II metabolism Mostly ER Energy requiring Mostly Cytosol Page 5 5 Focus on Metabolism-Phase I • Cytochrome (CY) P450~75% of total Focus on Oxidation • Cytochrome P450 metabolism > Inducibility • CYP 2E1: ethanol, acetone, isoniazid • CYP 3A4: anticonvulsants, rifampin, steroids • CYP 1A: hydrocarbons > Inhibition > Genetic polymorphism > Hepatic Dysfunction > Superfamily of enzymes (12 human) > Phase I oxidation and some reduction > Oxidation • CYP hemoprotein and CYP 450 reductase • Oxygen and NADPH > CYP 1, 2 & 3 responsible for most drug biotransformations > ****drugs may increase or decrease activity • Non Endoplasmic Reticulum > Alcohol dehydrogenase - cytosol > Xanthine oxidase, monoamine oxidase – Phenytoin induces CYP1A2, CYP2C9, CYP2C19, CYP3A4 – Problem if other drugs are substrates for activate CYP (i.e . Carbamazepine) Focus on GlucuronidationPhase II Focus on Glutathione (GSH)-Phase II • Yields highly polar conjugates • Conjugates generally inactive • Actively excreted bile and urine • Potential for enterohepatic circulation • Enzyme Quantity: birth, induction, liver • • • • • disease Glucose-1-PO4 + UTP + 2 NAD +H2O>>> UDPGA + 2 NADPH + 2H UDPGA + Drug ---------> Glucuronyl-Drug UDP-glucuronosyl transferase Tripeptide substrate for GSH-transferases Detoxifies electrophilic intermediates Conjugates further metabolized mM quantities in liver Acetaminophen overdose-use N -acetylcysteine (NAC), precursor of glutathione. SH NH 2 CH 2 α | H H γ | H O=C-C-C-C-C--N-C-C--N-C-C=0 | H H H H H H H OH OH Glutamate Cystiene Glycine Page 6 6 Hepatic Elimination Renal Elimination Excretion versus Metabolism • Metabolite Disposition • >Enter circulation Glomerular Filtration > perfusion • Glucuronide metabolites largely excreted by y kidney > size, lipid solubility and protein binding • Tubular Secretion - active > less dependent on protein binding >Excreted in bile > probenicid • • Enterohepatic Circulation Tubular Resorption - passive > weak acids - alkalinize urine > weak bases - acidify urine > helpful in treating some poisonings Bioavailability Assorted Topics • Pulmonary Elimination Factors affecting bioavailability > Route of administration > Chemical properties of the drug > Formulation of the drug (Pharmaceutics) > Metabolism-presystemic M b li i > Site of administration relative to site of metabolism > Site of drug action > Pharmacodynamic parameters > Host factors (“Patient" factors) >Exhalation of volatile lipid soluble drugs • Alcohol, anesthetic gases Some biotransformation >Some • Placental Transfer >Not a barrier to most drugs • Breast Milk >Lipid soluble drugs pass well >Acidic compared to plasma Page 7 7 Patient Factors / Bioavailability Pharmokinetics and Dosing • Metabolic Differences • Discuss factors which affect initial > Genetic > Age > Gender > Medical Conditions > Concurrent Drug Use concentration of drug after administration. • Discuss two common time courses of drug elimination. elimination • Gastrointestinal (GI) Tract > 1st order - linear > Zero order - non-linear > Achlorhydria (no acid) > Gastric stasis > Gastric surgery > Small bowel problems > Colonic resection *** How does age and health of preclinical species affect • Discuss factors affecting drug dosing. > Repeated dosing > Changing dosing > Loading doses bioavailability? Experimental Determination of Vd Drug 500 F Drug Con ncentration Vd = Dose / C0 Elimination 7 100 % 400 300 F 50% 200 F 100 12.5% F 6.25% F F 0 Plasma Vascular organs 25% 0 1 2 3 4 5 Time after Administration LN Drug Concentration Drug Distribution 6 F F 5 F F 4 lnCt = lnC -k(t) 3 F 0 F 2 1 0 0 1 2 3 4 5 Time after Administration Measure plasma drug concentrations after dose and back-extrapolate to time 0. Vd = Dose / C0 Fat (reservoir) Volume of Distrubution of compound: concentration of drug in plasma to total amount of drug in the body Page 8 8 Can Vd be > Volume Patient? • • Implications • Changes in concentration with dose Yes: Vd is a Virtual Volume > Small Vd, small dose to increase concentration and vice versa Drugs with high Vd are being sucked into fat and reservoir sites. • It may take a long time to fill f the tank when the volume of distribution is quite large. > Example: drugs which accumulate in fat. • It may take a long time to empty the tank, to get rid of a drug. Protein Binding of Drugs PK Assumptions / Givens Free drug is generally active form (word about plasma; 92% water, 8% blood plasma proteins) • Drug effects are related to [Drug] • [Drug] in the circulation or biophase is related > Albumin, alpha1-acid glycoproteins, lipoproteins ***remember unbound or free fraction drug only exerts biological effects, metabolized and excreted • to dose • [Drug] changes with time • Drug therapy is enhanced by knowledge of Binding affects distribution of drugs > generally passive process > dependent on free drug concentration > *** If the amount of plasma protein is decreased (such as in catabolism, malnutrition, liver disease, renal disease), there would also be a higher fraction unbound • the relationship of [Drug] to drug dose and the expected changes with time, thus Drugs can compete for or saturate binding sites > avoiding ineffective therapy > avoiding drug toxicity > can affect free drug concentration > can affect elimination > Example: drug A % free fraction double= effects doubled Page 9 9 Scenario 1: Data • blood pressure (BP) • Assume instantaneous mixing and • drug distribution • Measure plasma drug concentration • over time 500 × 100% Constant proportion of g disappears pp with drug each time period Exponential (firstorder) decay • 300 Ū × 200 25% Ū × 12.5% Ū × 6.25% Ū × Ū Ū × 100 0 Mean Arterial BP • × 1 0 0 5 1 2 3 4 5 Time 6 5 4 3 2 × Ū × Ū × Ū × Ū × Ū × Ū 1 0 Cls = kel • Vd or kel = Cls / Vd 0 1 2 3 4 5 Time > Clearance (Clsystemic) the virtual volume completely cleared of drug / unit time 75 • 70 0 Allows calculation of kelimination (kel) > units = time-1 > proportion of drug eliminated • -1 4 2 7 lnCt = lnC0 - k • t 85 80 3 4 3 Time Log plot of data is linear Ū × 90 2 5 Starting the Number Crunch to T1/2 × Ū Ū Ū × Ū × Ū × 95 1 LN Drug Concentration • Blood pressure 50% × Ū × Ū × Ū × Ū × Ū × Ū 6 lnCt = lnC0 - k • t Scenario 1: Data (cont.) 100 Ū × 7 400 0 • Measure BP response over time • Repeat with half the dose response is proportional to: >dose and > Ct C0 is proportional to dose LN Drug Con ncentration • Administer medicine IV which lowers Drug Conce entration Empiric Approach: Scenario 1 1 2 3 4 Allows prediction of the effect of changes of Vd on drug half-life (T1/2) 5 Time Page 10 10 Half-life • Solving for T1/2 A convenient way to think of how long drug sticks around kel • t = ln (C0 /Ct) > Comparisons, dosing, etc. t = ln (C0 /Ct) / kel [5] l Ct = ln ln l C0 - kel • t [1] kel • t = ln C0 - ln Ct [2] kel • t = ln (C0 /Ct) [3] At T1/2, C0 /Ct = 2 Relating T1/2 to Vd T1/2 = 0.693 / kel kel = Cls / Vd [3] [6] T1/2 = ln (2) / kel [7] T1/2 = 0.693 / kel [8] Critical Factors Clearance of compound: efficiency of irreversible elimination of drug from system [8] Elimination rate (mg/hr)= clearance (Cl) (L/hour) * plasma drug concentration (C) (mg/L) [[10]] Maintenance dose rate (DR) (mg/hr)= clearance (CL)( L/hr)* steady state drug concentration (Css) (mg/L) T1/2 = 0.693 • Vd / Cls [11] Clearance (L/hr) = dose (mg)/ AUC (mg*hr/L) Page 11 11 What does it mean? Summary: Single Compartment-1st Order T1/2 = 0.693 / kel or T1/2 = 0.693 • Vd / Cls • Simplistic model that describes PK of most drugs • Assumes • T1/2 not intrinsic to a drug > Drug in faster than drug out > Equilibration E ilib ti relatively l ti l quick i k > Can sum all elimination routes in single equation >not same for every person >not same for an individual at all times • T1/2 dependent on: Drug In >Individual’s elimination capacity (clearance) >Individual’s Vd Circulation kel Drug out (or rapidly equilibrated Vd) Summary: Single Compartment-1st Order Drug In Circulation Half life Related to Vd and Cls • T1/2 = 0.693 • Vd / kel Drug out Cls (or rapidly equilibrated Vd) T1/2 = 0.693 • Vd / Cls * Shows us that T1/2 dependent on Vd and Cls * Predicts effect of organ impairment on T1/2 * Clearance is sum of all contributions to clearance * Constant proportion (not amount) is eliminated per unit time * Regardless of initial amount, >95% gone in 4-5 half-lives Page 12 12 Scenario 2: Zero-order Elimination Scenario 2: Alcohol Elimination • Students celebrate time, not proportion • Limited capacity for metabolism or other • elimination mechanism • • Elimination is saturable • Part or whole dose-concentration range • Example: ethanol zero-order throughout • concentration range • 2 × 1.6 12 1.2 × Ū × Ū × Ū 0.8 × Ū × × Ū 0.4 Ū × 0 0 1 2 3 4 5 6 7 Time (hours) Scenario 3: Repeated Dosing, 1st Order • • • • The usual situation in treating disease • Repeated administration before total elimination (>4-5 half-lives) leads to drug accumulation. accumulation • Dose given every half-life Peak with first dose = 500 The median [SS] is 1.5 times the initial [peak] After 3 half-lives half lives 87.5% 87 5% of SS has been achieved After 5 half-lives >95% if SS has been achieved CSS = 1.5 • (T 1/2/τ) • C0 • Zero order not the same • • If a constant schedule is followed, a steady • state concentration of drug will result. • At steady state (SS): Drug in = Drug out • If the drug is given in boluses, the blood 1200 Drug Concen ntration Repeated Dosing: First-order Kinetics end summer course Student 1: 6 oz. Jack Daniels Student 2: 4.5 oz. Jack Daniels T1/2 does not apply with zero order kinetics Time per drink Blood EtOH H (g/L) • Constant amount of drug removed / 1000 × 800 × × × × × × × × × × × 600 × 400 200 × × × 0 × 0 1 2 3 4 5 6 7 8 9 Multiple of Half-lives [Drug] will vary around a SS concentration Page 13 13 Therapeutic Window on Intervals Determining Drug Dose and Interval • Dose (quantity) must give non-toxic peak level • Frequency q y must not allow trough g level to be sub-therapeutic, or drug effect must last longer than the drug • • Dosing interval must be conducive to • patient compliance First-Order Dose Changing Narrow Swings: same dose more frequently (divided in smaller intervals) If wider swings can be tolerated, give more drug over wider interval Zero-order Difficulties • Concentration directly proportional to dose • New dose= [desired]/[current] x old dose • Lack of Predictability > Transition from first to zero order unpredictable > Drug level can rise precipitously > Ethanol, ASA, Theophyline, and Phenytoin (Dilantin®) • Steady State Equation (in = out) > Css x Cls = F x Dose /τ > Css = (F x Dose /τ ) / Cls > Cls = (F x Dose /τ ) / Css Page 14 14 Loading Dose Loading dose: initial higher dose administered at beginning of a course of treatment before dropping down to a lower dose (when you need to get there sooner.) > C0 = F x Dose / Vd > i.e. digoxin, phenytoin Example: Hypothetical drug X,X long half-life w/ only 10% cleared from blood/day by kidney and liver; drug optimal efficacy when total dose in body = 1 gram; maintenance dose= 100 mg per day No loading dose: start with 100 mg of drug X per day…take many days to reach optimal drug levels Day 1: 100 mg; clear 10 mg = total 90 mg Day 2: 100 mg; 100+ 90= 190 mg; clear 19 mg = total 171 mg Day 3: 100 mg; 100+ 171= 271 mg; clear 27 mg = total 244 mg Loading dose: start with 1000 mg Day 1: 1000 mg; clear 100mg = total 900 mg Day 2: 100 mg; 100+ 900= 1000 mg; clear 100 mg = total 900 mg Day 3: 100 mg; 100+ 900= 1000 mg; clear 100 mg = total 900 mg, etc. Page 15 15