* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Pacemaker Malfunction
Heart failure wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Jatene procedure wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Atrial fibrillation wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
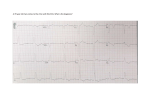
PACEMAKER PROBLEMS Jeff Ball and Hla Chaw The common complications after pacemaker insertion (temporary or permanent) are interpreted by the features on 12 lead ECG, monitoring, or CXR. 1 – COMPLICATIONS OF CENTRAL VENOUS CANNULATION (e.g.; pneumothorax, bleeding) 2 – PERFORATION OF HEART by the electrode tip leading to pericardial effusion, cardiac tamponade 3 – ELECTRODE DISPLACEMENT (microscopic or macroscopic) leading to: 4 - FAILURE TO CAPTURE CAUSES • Elevated Capture Threshold - After electrode implantation, oedema and inflammation around the tip result in a steady rise in the threshold over the first few weeks. The process is mild and self-limiting. - Electrolyte disturbance (e.g., hyperkalemia, acidemia), antiarrhythmic drugs (class 1c such as Flecainide) - Myocardial fibrosis (e.g., cardiomyopathy, myocardial infarction) can increase threshold. • • • Lead malfunction Lead fracture Lead dislodgement or perforation DIAGNOSIS - by 12 leads ECG shows the pacing spike with following QRS (fig .a –The fourth stimulus fails to capture the ventricle) TREATMENT – treat the underlying causes. 5 - FAILURE TO SENSE CAUSES • Lead dislodgement. Usually accompanied by failure to capture. • Lead insulation failure. • Inadequate endocardial signal. • Change in ECG. Transient changes in electrolyte or acid-base disturbance, permanent changes in myocardial infarction or cardiomyopathy. • Ectopic beats. • • Pulse generator failure. Functional under-sensing. If the intracardiac signal is of insufficient amplitude the pacing stimulus will not be suppressed, resulting in inappropriate pacemaker firing. DIAGNOSIS - 12 leads ECG. The atrial pacemaker has failed to sense the preceding atrial activity and therefore delivered the second stimulus. This has captured the atrium, with the P-wave in the ST segment, and subsequent conduction to the ventricle. (Fig b) - pacemaker check TREATMENT – Treat the causes. Fig.a – Failure to capture Fig.b – Failure to sense Fig.c - Oversensing 6 – INFECTION AROUND THE GENERATOR Once infection is established, or the skin is breached, it is almost never possible to eradicate infection with antibiotics: removal and replacement of the pacing system is required. 7 - INAPPROPRIATE INHIBITION (OVERSENSING) CAUSES • Local skeletal muscle stimulation • Damage to the conductor or insulation of the pacing electrode due to trauma at the site of ligation or compression between the clavicle and first rib. DIAGNOSIS – 12 lead ECG (fig c). The dual chamber pacemaker has sensed an electrical artefact throughout the ventricular lead and as a result has suppressed ventricular pacing, with the absence of ventricular activation following the third P-wave. TREATMENT – treat the causes. 8 – PACEMAKER SYNDROME Symptoms of fatigue, dizziness, or hypotension, which are associated with the presence of atrial cannon waves occurring as a result of simultaneous atrial and ventricular contraction. TREATMENT – If symptoms are troublesome, upgrade of the system to a dual-chamber unit is necessary. 9 – PACEMAKER MEDIATED TACHYCARDIA – A paced tachycardia that is sustained by the continued active participation of the pacemaker in the rhythm. DIAGNOSIS – pacemaker check TREATMENT - Reprogram 10 – PSEUDOMAL FUNCTION. Artefact with small spikes on the surface ECG. Pseudo malfunction when recording and digital artefacts are misinterpreted. DIAGNOSIS Obtain a 12-lead ECG and evaluate the following: Determine whether pacing stimulus artefacts are present and whether a. The appropriate chambers are captured. b. If no pacing stimulus can be seen, native depolarisation should be adequate. c. Evaluate whether native beats are appropriately sensed in relation to paced complexes. FOLLOW-UP Patients with permanent pacemakers require follow-up by a pacemaker clinic (CTC) To detect the complications To assess the status of the pulse generator battery To maximize the battery life Patients should be assessed at least annually by the clinic. Many patients who have long-standing heart block treated by permanent pacing have no underlying cardiac rhythm, and that failure of pacing system for whatever reason may be fatal. PACEMAKER CHECK, REPROGRAMME, CLINIC etc Temporary pacemaker may be checked by the ECG department Permanent pacemakers, refer to CTC.