* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Autonomic Abnormality in Chronic Heart Failure
Survey
Document related concepts
Saturated fat and cardiovascular disease wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Rheumatic fever wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Electrocardiography wikipedia , lookup
Coronary artery disease wikipedia , lookup
Heart failure wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
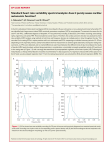
84 Heart Rate Variability 24 Autonomic Abnormality in Chronic H e a r t Failure evaluated by Heart Rate Variability Massimo Piepoli MD & Andrew JS Coats, DM,FRCP Department of Cardiac Medicine, Imperial College, National Heart & Lung Institute, Dovehouse Street, London. SW3 6LY. UK Chronic Heart Failure Prior work [I], utilizing pharmacological manipulation of blood pressure and analysis of resultant heart rate (HR) responses, suggested that withdrawal of parasympathetictone is a component of the autonomic dysfunction in chronic heart failure (CHF). Subsequently chronic activation of the adrenergic system together with impaired arterial baroreflex sensitivity have been also described as part of the syndrome [2]. Reduced baroreflex sensitivity and increased plasma noradrenaline levels have been shown to be independent predictors of increased mortality in CHF [3]. Heart Rate Variability The refinement of techniques for the assessment of heart rate variability (HRV), which provides a reliable estimate of the autonomic nervous system control of the cardiovascular system, has permitted an analysis of autonomic tone at rest without the need for provocative manoeuvres. Several studies have been published, but all of them confirmed the observation of a reduced HRV, with' increased sympathetic activation and depressed vagal tone in CHF patients The first works evaluated time domain indexes of HRV. In 1987, analysing 24 hour Holter tapes. Kleiger et al. [4] reported that, of all variables measured, a reduced HRV had the strongest univariate correlation with mortality, directly related to left ventricular ejection fraction and exercise capacity and inverse related to left ventricular failure during myocardial infarction. After this report, HRV was proposed as :I non invasive tool to investigate the autonomic abnormalities in CHF. Eriksson et al [5] in a review of the risk factors for heart failure in the general population, observed that reduced HRV, ;is well as other variables (such as hypertension, smoking. body weight o r heart volume) were independent risk ractors. In the patients awaiting for cardiac transplantation, a reduced HRV is superior to other prognostic indexes to assess the risk of death [6]. Caruana et a1 [7], evaluating 24 hour ambulatory intra-uteri:!! blood pressure recordings found that not only HRV was reduced but also blood pressure variability in CHF with respect to normals and that these indexes were correlated with the left ventricular ejection fraction and pulmonary wedge pressure. Reduction in HRV and increased HR in patients with CHF respect to controls was later confirmed during over 24 hours recording iS.91. In a following work, HRV although correlated with left ventricular ejection fraction. did not provide any significant help in identifying CHF patients at risk of sudden death [lo]. Coumel et al [ I I ] observed that a short lasting treatment with beta-blocker slowed non-uniformly the mean HR: -9.5% in normals and -19.1%in CHF. This confirmed a sympathetic predominance in CHF which was reflected by the Bblockade induced HR decrease that was twice as marked in patients as in controls. Also the indexes of vagal activity has been evaluated in this syndrome. From 24 hour Holter monitoring Nolan et al [ 121 measured the number of times each R-R interval exceeded the preceding R-R interval by more than 50 ms as an index of parasympathetic activity and found that this parameter was significantlycorrelated with [eft ventricular ejection fraction; thus the degree of vagal withdrawal seemed to correlate with the severity of heart failure. More recently the use of power spectral analysis approach to evaluate the variability of the cardiovascular signals allowed to further investigate the sympatho-vagal balance in this syndrome. Saul et al [ 131 observed that HRV was reduced at all frequencies examined (from O.OIHz to 1.0 Hz) in CHF with respect to normals and virtually absent at frequencies greater than 0.04 Hz. In fact the very low frequency (LF) (defined as 0.OIHz to 0.04 Hz) less cffcctively difl'erentiated CHF from controls, due to discrete (about 65 seconds, 0.015 Hz) oscillation in HR. which was associated with ii similar pattern in respiratory activity in many of the patients with CHF. These findings demonstrated a marked derangement of autonomic control of the heart in CHF patients. The frequency characteristics of HRV (absence of HRV above 0.04 Hz and relative preserved very low frequency component) in these patients are consistent with abnormal barorellex responsiveness to physiological stimuli, and suggest that there is diminished vagal, but relatively preserved sympathetic, modulation of HR. In a subsequent study, it was confirmed the abnormal pattern of HRV spectrum in CHF patients (affected by idiopathic dilated cardiomyopathy) who presented absence of high frequency component (HF) (defined as >O.lHz) and a predominant sympathetically mediated LF area (defined as 0.02-0.1Hz) [14]. By pharmacological interventions, which decreased vagal tone and enhanced sympathetic activation, it was possible to induce in normal subjects the same autonomic alterations typical of the CHF patients: administration of atropine reduced the HF area (within the range noted in patients with CHF); the administration of isoproterenol augmented the LF area without changing the HF m a [l4]. These findings suggest that augmented sympathetic drive itself does not mimic the HRV spectrum of CHF and emphasizes that parasympathetic withdrawal is a necessary component of the autonomic profile. Experimental studies in a paced canine model with the induction of congestive heart failure resulted in alterations in the autonomic profile that resembled those seen in humans with ventricular failure: the prominent HF component of the spectrum at baseline, indicating a predominance of parasympathetic tone, was absent after the evolution of CHF with marked augmentation of the LF of the spectrum. The power spectral analysis of HRV is able to detect the autonomic profile characteristics of CHF, with increased sympathetic tone and parasympathetic withdrawal. HRV seems also to provide a noninvasive information regarding the neurohumoral abnormality in CHF. In fact both time domain (standard deviation of R-R interval) and frequency domain (LF and HF components) parameters of HRV were correlated with indicators of sympathoexcitation, muscle sympathetic nerve activity and plasma noradrennlinc in CHF [IS]. Not uniform data have heen published regarding the correlation between severity of CHF and indexes of HRV. While Nolan et a1 [ 121 reported a direct correlation between reduction in vagal activity index and the severity of heart failure, Saul et al [I31 found no significant correlation between spectral data and age or survival; a weak correlation was present between LF component and several Iineinodynomic varieblcs, such as pulmonary capillary wedge pressure (r=-0.545). cardiac index ( ~ 0 . 4 6 6 )Kienzle . et a1 [IS] reported that frequency domain parameters of HRV correlated weekly but significantly with cardiac output (r = 0.49 and ~ 0 . 4 2 respectively), but all the other parameters of HRV (both in time and frequency domain) did not correlate with index of severity of CHF (left ventricular ejection fraction, cardiac output or functional classification). Instead Stefanelli et a1 [I61 reported that in CHF the overall 24-h HRV and nighvday HR ratio was reduced. depending on the NYHA functional class. The typical morphology of R-R interval histograms was a sensitive marker of the clinical state at baseline: the higher the NYHA class, the smaller the R-R interval variability and standard deviation of R-R intervals. They also observed that the clinical deterioration after 6 months was accompanied by a tendency to further shortening of the mean total HRV. In patients with clinical improvement no significant change in HRV was observed. They concluded that while severe clinical disease progression may be. associated with further reductions in the HRV, improvement in the clinical state of CHF is not necessarily associated with changes in HR behaviour. More recently other authors [I71observed that the more advanced state of severity in CHF were associated with different patterns of HRV: while NYHA class I1 showed predominance of LF components (a marker of increased sympathetic activation) and a blunted response to tilting, class III patients showed an unresponsiveness to tilting, and class IV patients an even more depressed HRV indexes and an almost absence of the LF components. Correlations between HRV indexes and seventy in CHF have been also recently reported by Casolo et al [IS] who observed that while time domains parameters correlated well with.the degree of CHF severity, spectral components of HRV did not show a progressive impairments: LF and HF decreased severely from NYHA class I to class 11, with less reduction in the more advanced classes. Instead Takase et a1 [ 191 reported that while clinical deterioration and autonomic neuropathy were associated with more severe depression of HRV (as assessed by standard deviation), also after clinical improvement improvement in spectral analysis index was observed with higher standard deviation. The different methods and indexes used for assessing autonomic controls during the evolution of the syndrome may at least partially explain the discordant findings reported. We observed in fact 120) that the different methods t~ assess sympathovagal balance (time domain and frequency domain indexes) did not correlate, with the exception of Heart Rate Variability day and night-time HR and the expected inverse correlation between LF and HF (r = -0.92). However. no method correlated significantly with peak oxygen uptake. exercise tolerance or ejection fraction. Thus in CHF the individual parameters of autonomic control seemed to reflect different aspects of the circulatory control, hence a comprehensive description of the autonomic tone may require multiple methods. The therapeutic approaches to this syndrome, have been also' evaluated in relation to their capability to partially reverse the autonomic abnormalities, assessed by HRV. Flapan 1211 investigating the effect of with angiotensinconverting enzyme inhibitors (captopril) therapy, reported an increase in HRV. The authors concluded that the results may be relevant to the improved prognosis of this group of patients when treated with angiotensin-converting enzyme inhibitors. Similar beneficial effects on HRV by an other ACE-inhibitor drug (zofenopril) [22] and by low dose scopolamine [23]. We have looked at the effects on the autonomic balance of physical conditioning in CHF [20,24]. In a controlled cross-over trial after 8 ,weeks of physical training at home, both time and frequency domains indexes showed improvement in autonomic balance. The circadian pattern of HRV in CHF patients and the relative effect of physical training were also recently evaluated in the 24-hour recordings[25]. We found that the training improved all HRV indexes, during different time intervals, suggesting that the improvement was an inherent phenomenon rather than due to increased physical activity. The preservation of a circadian variation of the LF and the HF components of HRV in patients after both training and detraining suggested that the syndrome of CHF is characterised by a resetting of autonomic balance rather than autonomic neuropathy (figure 1). The effect of short duration pulsed inotrope therapy was assessed in C H F it induced a pharmacological conditioning, similar to that induced by physical conditioning, with up-regulation of the B-adrenoceptors and enhancement of the chronotropic responsiveness 1261. Figure 1. Circadian patterns of the LF and HF components of HRV in controls (closed squares) and in CHFpatients after training (open circles) and after de-training (closed circles). Note the higher powers during the sleeping status in all groups and the higher powers in normals compared to patients also after training and detraining and the higher powers after training compared to after detraining (reproduced from [25]). 85 Controversies Several studies have been published during the last few years. and probably even more will be presented in the near future. However. some important debates are still open. First it is the physiological meaning of the HRV findings. In fact it is well known that the sympathovagal balance to the heart is tonically and phasically modulated by the interaction of several factors: central neural integration, peripheral receptor activation with inhibitory and excitatory reflex mechanisms. However it still unclear what part of the autonomic nervous system is specifically investigated by the HRV technique. We recently evaluated whether HRV can differentiate between sympathetic stimulation induced by endogenous sympathetic stimulation (i.e. physical exercise) and exogenous sympathetic stimulation (by inotrope infusion): exercise and inotrope infusion produced similar changes in HRV (figure 2); however plasma noradrenaline was elevated by exercise but unchanged by dobutamine [27]. Therefore HRV could not differentiate between the two sympathetic stimulations. indicating that the degree of receptor stimulations rather than the level of sympathetic drive would appear to determine the changes in HRV. An other important point is how reproducible is this methodology in a condition of profound autonomic imbalance such as CHF. A considerable day-to day variation in 24 hour Holter monitoring was reported in normals and also in CHF [28,29]; however stability from short lasting recordings is not been established. An abnormal HRV patter is evident in more advances stages of CHF the original observation of Saul et al [13] was later confirmed [ 17,301. i.e. the pattern of HRV in CHF patients is characterized by depressed HRV with predominant very low frequency fluctuations. whose exact origins are still under debate. In fact these fluctuations niay be influenced by various physiological factors, like reninangiotensin system, thermal regulation [3 1,321. A possible origin from abnormal respiratory pattern with Cheyne-Stokes respiration was hypothcsised [33], which may induces an abnormal activity of chemoreceptors: further investigation are needed to confirm this hypothesis. Figure 2. Changes in LF (upper) and HF (lower graph) of HRV (means It standard error) during dobutamine infusions (open symbols, continuous lines) and supine exercise tests (filled symbols, dotted lines): *=p<O.OS vs. pre-dobutamine rest, #=p<O.OS vs. preexercise rest (reproduced from [27]) 2 In-msec .. '"1 5.61 A I rl\ K a a e7 t- 5. 2 In-meec 7007 i\ L a : P Ipm 7pm lam Tam h.. \+.:. ., 86 Heart Rate Variability References I . Eckberg DL. Drabinsky M. Braunwald E. Defective cardiac parasympathetic control in patients with heart disease. N Engl J Med 1971; 285877-83. 2. Hasking GJ, Esler MD, Jennings GL, Burton D, Johns JA, Korner PI. Norepinephrine spillover to plasma in congestive heart failure: Evidence of increased cardiorenal and total sympathetic nerve activity. Circulation 1986;73615-21. 3. Leimbach WN Jr, Wallin BG, Victor RG. Aylward PE, Sundolf G. Mark AL. Direct evidence from intraneural recordings for increased central sympathetic outflow in patients with heart failure. Circulation 1986;73:913-9 4. Kleiger RE,Miller JP, Bigger JT, Moss AJ and the Multicenter Post-Infarction Research Group. Decreased heart rate variability and its association with increased mortality after acute mycocardial infarction. Am J Cardiol 1987;59;256-62 5 . Eriksson H, Svardsud? K. Larsson B, et al. Risk factors for heart failure in the general population: the study of men born in 1913. Eur Heart J 1989;lO: 647-56 6. Binder T. Frey B, Porenta G, Heinz G, et al. Prognostic value of heart rate variabilitv in Datients awaiting cardiac transplantation. PACE 1992;lS: 2i15-20. 7 . Caruana MP, Lahiri A, Cashman PM. Altman DG, Raftery EB. Effects of chronic congestive heart failure secondary to coronary artery disease on the circadian rhythm of blood pressure and heart rate. Am J Cardio1.1988;62:755-9 8. Hermida IS, de Jode P, Jarry G, et al. Sinus rhythm and standard deviation in cardiac cycles. Influence of myocardial status and beta-blocker treatment. Arch Ma1 Coeur Vaiss 1989;82:1993-2000 9 . Casolo G. Balli E, Taddei T. Amuhasi J. Gori C. Decreased spontaneous heart rate viiriability in congestive heart failure. Am J Ciirdiol 1989;64:1 162-7 10. Fei L, Keeling PJ, Gill JS. et al. Heart rate variability and its relation to ventricular arrhythmia in congestive heart failure. Br Heart J 1994;71:322-8 I I . Coumel P, Herniida JS. Wennerblom B. et al. Heart rate variability in left ventricular hypertrophy and heart failure, and the effects of beta-blockade. A non-spectral analysis of heart rate variability in the frequency domain and in the time domain. Eur Heart J 1991;12:412-22 12. N o h J. Flapan AD, Capewell S.MacDonald TM, Neilson JM, Ewing DJ. Decreased cardiac parasympathetic activity in chronic heart failure and its relation to left ventricular function.Br Heart J 1992;67:482-5 13. Saul JP, Arai Y, Berger RD. Lilly LS, Colucci WS, Cohen RJ. Assessment of autonomic regulation in chronic congestive heart failure by heart rate spectral analysis. Am-J Cardiol 1988;61:1292-9. 14. Binklev PF. Nunziata E. Haas GJ. Nelson SD. Codv RJ. Parasimpathetic withdrawal is an. integral component of autonomic imbalance in congestive heart failure: demonstration in human subjects and verification in a paced canine model of ventricular failure. J Am Coll Cardiol 1991;18:464-72 15. Kienzle MG, Ferguson DW, Birkett CL, Myers GA. Berg WJ, Mariano DJ. Clinical, hemodynamic and sympathetic neural correlates of heart rate variability in congestive heart failure. Am J Cardiol 1992;69:761-7 16. Stefenelli T. Bergler Klein J, Globits S. Pacher R, Glogar D. Heart rate behaviour at different stages of,congestive heart faihre. Eur Heart J 199213:902-7. 17. Guzzetti S, Cogliati C, Turiel M, Crema C, Lombardi F, Malliani A. Sympathetic predominance fo:lowed by functional Y denervation in the progression of chronic heart failure. Eur Heart J 1995; 16: 1100-7 18. Casolo G. Stroder P. Sulla A. Chelucci A. Freni A. Zerauschek M. Heart’rate variability and functional &verity of congestive heart failure secondary to coronary artery disease. Eur Heart J 1995;16:360-7 19. Takase B, Kurita A, Noritake M, et al.. Heart rate variability in patients with diabetes mellitus, ischemic heart disease, and congestive heart fiiiluw. J Electrocardiol 1992;25:79-88 20. Adamopoulos S,Piepoli M, McCance A. et al. Comparison of different mcthods for assessing sympathovagal balance in chronic congestive heart failure secondary to coronary artery disease. Am J Cardiol 1992;70: 1576-82. 2 I . Flapan AD, Nolan J, Neilson JM, Ewing DJ. Effect of captopril on cardiac parasympathetic activity in chronic cardiac failure secondary to coronary artery disease. Am J Cardiol 1992; 69~532-5 22. Binkley PF. Haas GJ. Starling RC, et al. Sustained augmentation of parasympathetic tone with angiotensinconverting enzyme inhibition in patients with congestive heart failure. J Am Coll Cardiol 1993: 21:655-61 23. La Rovere MT. Mortara A. Pantaleo P. Maestri R, Cobelli F, T a v a u i L. Scopolamine improves autonomic balance in advanced congestive heart failure. Circulation 1994; W838-43 24. Coats AJS, Adamopoulos S. Radaelli A, et al. Controlled trial of physical training in chronic heart failure: Exercise performance, hemodynamics, ventilation and autonomic function. Circulation 1992;85:2119-31. 25. Adamopoulos S,Ponikowski P, Cerquetani E. et al. Circadian Pattern of Heart Rate Variability in Chronic Heart Failure Patients: Effects of Physical Training. Eur Heart J 1995 (in press) 26. Adamopoulos S, Piepoli M, Qiang F. et al. Short duration pulsed inotrope therapy induces pharmacologicalconditioning in congestive heart failure; up-regulates R-adrenoceptors and enhances chronotropic responsiveness. Lancet 1995; 345344-9 27. Piepoli M. Adamopoulos S. Bemardi L, Sleight, P, Coats AJS, Autonomic Cardiovascular Control in Heart Failure: power spectal analysis of heart rate variability shows similarity between exogenous and endogenous R-receptor stimulation. C1 Sci 1995; 89:155-164 28. Van-Hoogenhuyze D. Weinstein N. Martin GJ, et al. Reproducibility and relation to mean heart rate of heart rate variability in normal subjects and in patients with congestive heart failure secondarv to coronarv . arterv , .disease Am J Cardiol 1991;68:1668-76 29. Stein PK. Rich MW, Rottman JN, Kleiger RE. Stability of index of heart rate variability in patients with congestive heart failure. Am J Cardiol 1995;129:975-81 30. Mortara A, La Rovere MT, Signorini MG, et al. Can power spectal analysis of heart rate Variability identify a high risk subgroup of congestive heart failure patients with excessive sympathetic activation? A pilot study before and after heart transplantation. Br Heart J 1994; 71: 422-430. 3 I . Akselrod S. Gordon D, Ubel FA, Shannon DC. Barger AC. Cohen RJ. Power spectral analysis of heart rate fluctuations: a quantitative probe of beat-to-beat cardiovascular control. Science 198 1:213:22&223. 32. Sayers B Mck. Analysis of heart rate variability. Ergonomics 1973;16:17-32. 33. Ichmaru Y, Yanaga T. 24-hr ambulatory electrocardiographic monitoring. Comput Biomed Res 1989;22225-33