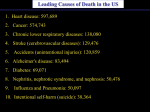
* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Heart disease regulations: implications for work and play
Survey
Document related concepts
History of invasive and interventional cardiology wikipedia , lookup
Electrocardiography wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Heart failure wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Saturated fat and cardiovascular disease wikipedia , lookup
Cardiac surgery wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Transcript
Mills and Boon Heart disease part 2_Layout 1 17/09/2014 11:24 Page 1 CARDIOVASCULAR MEDICINE 31 Heart disease regulations: implications for work and play – part 2 NICHOLAS L. MILLS AND NICHOLAS A. BOON Authorities may impose restrictions on the activities of patients with heart disease in order to protect the individual, society or the interests of their institution. In the second article of this two-part series, the authors look at the scientific basis underpinning current advice on driving, flying and a range of sporting activities. n part 1 of this series, we outlined the concept of acceptable risk and discussed the implications for patients with coronary artery disease and implanted devices.1 Here, we look at the implications of heart disease for drivers, air passengers, divers (Figure 1), climbers and professional athletes. I HEART DISEASE AND DRIVING In the UK, 1 per cent of the 130 000 road traffic accidents per annum occur as a result of an underlying medical condition.2 The Road Traffic Act 1988 sets out the legal basis through which the Driver and Vehicle Licensing Agency (DVLA) has responsibility to ensure that all licence holders are fit to drive. The DVLA publishes national guidelines that outline restrictions for all categories of licence holders for all relevant medical conditions, and these guidelines are updated twice a year.3 TRENDS IN UROLOGY & MEN’S HEALTH Figure 1. Diving poses special risks to patients with heart disease ( ”Photostock Israel/Science Photo Library) The medical standards for drivers of heavygoods and passenger-carrying vehicles (group 2) are higher than those for drivers of cars or motorcycles (group 1), because of the size and weight of the vehicle, and the length of time the driver spends at the wheel (Table 1). Indeed, the case fatality rates for accidents involving these vehicles are three- to fourfold greater than those involving ordinary private cars. Thus, following an acute coronary syndrome, group 1 licence holders are allowed to return to driving after one week if they have undergone percutaneous revascularisation or four weeks if they have not been revascularised, and do not need to inform the DVLA. In contrast, group 2 SEPTEMBER/OCTOBER 2014 Nicholas L. Mills, PhD, MRCP, Consultant Cardiologist; Nicholas A. Boon, MD, FRCP, Consultant Cardiologist, Royal Infirmary of Edinburgh www.trendsinurology.com Mills and Boon Heart disease part 2_Layout 1 17/09/2014 11:25 Page 2 CARDIOVASCULAR MEDICINE 32 Condition Group 1 Group 2* Angina pectoris Driving must cease when symptoms occur at rest, with emotion or at the wheel Refusal or revocation with continuing symptoms (treated and/or untreated) (r1) Acute coronary syndrome If successfully treated by coronary angioplasty, driving may recommence after 1 week provided no urgent revascularisation planned and LVEF >40% All acute coronary syndromes disqualify the licence holder from driving for at least 6 weeks (r1) If not successfully treated by coronary angioplasty, driving may recommence after 4 weeks Elective PCI Driving must cease for at least 1 week Disqualifies from driving for at least 6 weeks (r1) Elective CABG Driving must cease for at least 4 weeks Disqualifies from driving for at least 3 months (r2) Heart failure Driving may continue if no symptoms that may distract driver’s attention Disqualifies from driving if symptomatic (r3) Pacemaker implant Driving must cease for at least 1 week Disqualifies from driving for 6 weeks (r4) ICD implant – Ventricular arrhythmia with incapacity Should not drive for 6 months after implant or after any device therapy (shock or anti-tachycardia pacing)* Permanent bar Should not drive for 2 years if device therapy accompanied by incapacity* – Sustained ventricular arrhythmia, no incapacity Should not drive for 1 month after ICD implant providing LVEF >35%, no fast VT (RR <250ms), induced VT can be pace-terminated by the ICD and as above for device therapy* Permanent bar – Prophylaxis Should not drive for 1 month after ICD implant and as above for device therapy* Permanent bar *Notifiable to the DVLA: all categories for group 2 and selected group 1 licence holders. r, Relicensing may be permitted provided the following requirements can be met: r1, free from angina for 6 weeks and exercise or other functional test requirements can be met; r2, free from angina for 3 months with no evidence of significant impairment of left ventricular function (LVEF ≥40%) and exercise or other functional test requirements can be met; r3, asymptomatic, LVEF ≥40% and no other disqualifying condition with exercise or other functional testing possibly required depending on the likely cause for the heart failure; r4, 6 weeks if no other disqualifying condition. LVEF, left ventricular ejection fraction; PCI, percutaneous coronary intervention; CABG, coronary artery bypass grafting; ICD, implantable cardioverter defibrillator; VT, ventricular tachycardia. Table 1. Driver and Vehicle Licensing Agency (DVLA) driving restrictions for group 1 and 2 licence holders with selected cardiovascular conditions3 www.trendsinurology.com TRENDS IN UROLOGY & MEN’S HEALTH SEPTEMBER/OCTOBER 2014 Mills and Boon Heart disease part 2_Layout 1 17/09/2014 11:25 Page 3 CARDIOVASCULAR MEDICINE 33 licence holders must inform the DVLA and are disqualified from driving for at least six weeks, with relicensing permitted only following an exercise test or equivalent functional assessment. It is the duty of the licence holder to notify DVLA of any medical condition that may affect safe driving. AIR TRAVEL A combination of factors encountered during air travel, including forced immobility, low humidity, cosmic rays and hypobaric hypoxia, may have adverse effects on health.4 Most aircraft have limited facilities for healthcare and anyone who becomes ill in this environment may have a worse outcome. Nevertheless, a working party of the British Cardiovascular Society has concluded that there are very few cardiovascular conditions that warrant denial of the right to fly as a passenger (Table 2).5 Commercial airlines typically fly at altitudes of 7000–12 000 metres, and in spite of the use of pressurised cabins, air travel induces hypobaric hypoxaemia. International regulations specify that commercial aircraft are required to be pressurised to the equivalent pressure encountered at an altitude of 2438 metres. At this pressure-altitude the cabin oxygen partial pressure is 15.7kPa and therefore oxygen saturations in healthy individuals are between 90 and 93 per cent. Experimental studies suggest that these blood oxygen saturations have few adverse effects and are unlikely to trigger myocardial ischaemia, myocardial infarction, left ventricular failure or arrhythmia in patients with stable ischaemic heart disease.4 Patients with severe cardiopulmonary disease (eg Eisenmenger’s syndrome) may deteriorate as a result of additional hypoxia during flight. All commercial airlines provide access to oxygen for medical use if required. Patients who have undergone thoracic surgery should not fly for at least 10 days because they may have air in the chest, which could expand at altitude, resulting in pneumothorax or surgical emphysema. TRENDS IN UROLOGY & MEN’S HEALTH Condition Functional status Restriction or guidance Angina CCS I-II CCS III CCS IV Post-myocardial Low risk infarction* Medium risk High risk Elective PCI – Elective CABG – Acute heart failure – Chronic heart failure or NYHA I and II valvular heart disease NYHA III NYHA IV Cyanotic congenital heart disease NYHA I and II NYHA III Pacemaker implant ICD implant NYHA IV – – Arrhythmia Ablation therapy – – No restriction Airport assistance Defer travel, medical escort, oxygen Fly after 3 days Fly after 10 days Defer travel until stable Fly after 2 days Fly after 10 days if no complications Fly after 6 weeks if stabilised No restrictions May require in-flight oxygen Defer travel or in-flight oxygen and assistance May require in-flight oxygen May require in-flight oxygen, airport assistance In-flight oxygen and airport assistance Fly after 2 days Defer for 1 month post-implant or device therapy (shock) No restriction Fly after 2 days CCS, Canadian Classification Score; NYHA, New York Heart Association; PCI, percutaneous coronary intervention; CABG, coronary artery bypass grafting; ICD, implantable cardioverter defibrillator. *Low risk: age <65, first event, successful reperfusion, ejection fraction (EF) >45%, no complications, no planned investigations or interventions; medium risk: EF >40%, no symptoms of heart failure, no evidence of inducible ischaemia or arrhythmia, no planned investigations or interventions; high risk: EF <40% with signs and symptoms of heart failure, or those pending planned investigation, revascularisation or device therapy. Table 2. Restrictions for commercial air flight in patients with cardiovascular disease, adapted from a recent British Cardiovascular Society working party report5 PARTICIPATION IN SPORTS Clinicians are often asked to advise men with heart disease if they are fit to participate in sporting activities. Any recommendations should take into account the type and intensity of exercise performed, the risk of a sudden debilitating event, and the impact that such an event might have on other participants. By way of illustration, we discuss the implications of heart disease for divers, climbers and professional athletes. In the UK, professional divers are subject to detailed regular medical examinations under the auspices of the Health and Safety Executive; the discovery of organic heart disease will be considered a bar to occupational diving unless it is deemed by a cardiologist to be haemodynamically unimportant. Diving Diving is perceived by many to be a hazardous activity; fatal accidents are The UK Sport Diving Medical Committee provides amateur divers with an assessment of fitness to dive against a set of uniform medical SEPTEMBER/OCTOBER 2014 certainly more common among professional divers than in many other high-risk occupations such as construction. www.trendsinurology.com Mills and Boon Heart disease part 2_Layout 1 17/09/2014 11:25 Page 4 CARDIOVASCULAR MEDICINE 34 standards through a network of physicians with accredited diving medicine expertise. Restrictions are imposed on divers with conditions that may cause sudden or unexpected incapacity that could be hazardous to the individual or his or her diving partner; for example, limits are imposed for both depth and dive times in patients with arrhythmias so that, in the event of symptoms, they can return to the surface safely without prolonged decompression stops. usually advised to undergo percutaneous closure. Screening for a PFO is not considered necessary for recreational divers. Nevertheless, contrast echocardiography should be advised in any diver who has suffered a neurological, cutaneous or cardiorespiratory decompression illness; this is particularly important if the individual has a history of migraine with aura (a condition that is associated with PFO) or there was nothing untoward in the dive profile. During decompression at the end of a dive, bubbles of nitrogen gas are liberated from solution and can be detected in venous blood; paradoxical gas embolism may occur if the diver has a structural defect capable of intra-cardiac shunting, such as an atrial septal defect, and this is recognised as an important cause of neurological decompression illness.6,7 Effect of altitude Every year millions of tourists and mountaineers visit high-altitude locations, where inadequate acclimatisation can result in a spectrum of illnesses. Acute mountain sickness is defined as a syndrome of nonspecific symptoms including headache, gastrointestinal disturbance, insomnia and fatigue occurring in an unacclimatised person who has recently arrived at an altitude above 2500 metres.8 High-altitude pulmonary oedema and high-altitude cerebral oedema represent the end-stage of acute mountain sickness and can be fatal if not identified and treated promptly. Patent foramen ovale (PFO) is found in approximately 20 per cent of the general population and may predispose to paradoxical embolism in some circumstances. In the UK, most professional divers are screened for a PFO by contrast echocardiography, and those who are found to have a significant defect are The partial pressure of oxygen is reduced by 20 per cent at 2500 metres and by up to 60 per cent at 8000 metres, resulting in acute changes in cardiopulmonary physiology that include pulmonary and systemic arterial vasoconstriction, augmentation of the sympathetic nervous system, with increases in heart rate and myocardial contractility.9 These physiological effects could in theory trigger an acute coronary syndrome or cause acute decompensation in patients with congestive cardiac failure or pulmonary hypertension. Patients with class 3 or 4 heart failure or unstable angina and those with severe pulmonary hypertension should therefore be advised to avoid ascending to altitudes above 1500 metres. A recent review of the literature suggests that patients with stable coronary artery disease (Canadian Cardiovascular Society functional class I or II) can travel to altitudes of 3000–5000 metres with minimal risk;9 nevertheless, it is recommended that such patients ascend slowly and minimise physical activity for the first three to four days at altitude. Professional athletes While the incidence of sudden death among athletes is very low (Figure 2), many have argued for cardiovascular screening of professional athletes and elite sports men and women.10 Most screening programmes involve documentation of any personal and family history of cardiovascular disease, physical examination and ECG recordings. Recent evidence from a large prospective screening programme in Italy that included a 12-lead ECG suggested that this method of identifying and disqualifying athletes with hypertrophic cardiomyopathy may have prevented some deaths.11 On the other hand, the yield of most screening programmes is very low; in the Italian project, for example, screening 33 735 athletes identified only 22 new cases of hypertrophic cardiomyopathy. Figure 2. Cardiac arrest among elite athletes is very rare, but high-profile events, such as the collapse of Fabrice Muamba during a football match, have triggered intense interest in the value of pre-participation screening (”Getty Images) www.trendsinurology.com Moreover, screening tends to unearth many equivocal or borderline abnormalities that TRENDS IN UROLOGY & MEN’S HEALTH SEPTEMBER/OCTOBER 2014 Mills and Boon Heart disease part 2_Layout 1 17/09/2014 11:25 Page 5 CARDIOVASCULAR MEDICINE 35 require careful investigation and may generate a lot of potentially unnecessary expense and anxiety; indeed, it is notoriously difficult to distinguish mild hypertrophic cardiomyopathy from physiological left ventricular hypertrophy or ‘athlete’s heart’. This remains a controversial issue; thus, many sporting bodies and organisations now recommend or require active participants to undergo cardiovascular screening, while most health authorities continue to advise against universal pre-participation screening of athletes and other sportsmen (Box 1).12 BOX 1. Sport and heart disease l Sudden death in young athletes is a rare tragedy that is often caused by unrecognised cardiovascular disease, particularly hypertrophic cardiomyopathy l Pre-participation screening is recommended by many authorities, although it is often difficult to distinguish hypertrophic cardiomyopathy from physiological left ventricular hypertrophy caused by athletic training l The optimum mode of screening remains controversial, but should include a minimum of medical history, family history and physical examination. Additional tests such as 12-lead ECG and echocardiography may be helpful, but have been shown to generate many false-positive results l Patients with poor left ventricular function, exercise-induced arrhythmias, ischaemia and syncope, and those with significant valvular heart disease (particularly aortic stenosis) should be advised to avoid high-intensity sports activity SPECIAL OCCUPATIONS Employees with heart disease may experience discrimination because of the potential risk of sudden incapacity. The risk can usually be quantified and, if deemed unacceptable, the employee may qualify for critical illness benefits. The level of risk that is acceptable will depend on the underlying medical condition and the nature of the occupation. For example, drivers of mainline trains and tankers are not permitted to work following an acute myocardial infarction, because of the potential for incapacity to harm large numbers of innocent people. Separate specific regulations are available for pilots, firemen, seamen, the armed forces, police, offshore workers, scaffolders, arc welders, and many others. Dedicated occupational health services are usually available to help and advise affected employees and may request reports or specific investigations from the treating clinician. Declaration of interests: none declared. KEY POINTS • The medical standards for airplane pilots, professional divers and the drivers of heavy-goods and passenger-carrying vehicles are exacting and usually require specialist assessment and investigation • There are very few cardiovascular conditions that warrant denial of the right to fly as a passenger; however, people who are potentially vulnerable to a fall in oxygen saturations may require supplementary oxygen during flight • Patients with very poor left ventricular function, severe hypertrophic obstructive cardiomyopathy, critical valvular heart disease and unstable coronary disease should be advised to avoid high-intensity sports because extreme exertion can sometimes trigger myocardial infarction and/or malignant arrhythmias 4. 5. REFERENCES 1. 2. 3. Mills NL, Boon NA. Heart disease regulations: implications for work and play – part 1. Trends Urol Mens Health 2014;5(4):9–11. Department of Transport. Reported road casualties Great Britain 2012. www.gov.uk/government/publications/ reported-road-casualties-great-britainannual-report-2012 Driver and Vehicle Licensing Agency. At a glance guide to the current TRENDS IN UROLOGY & MEN’S HEALTH 6. 7. SEPTEMBER/OCTOBER 2014 medical standards of fitness to drive. Swansea: Drivers Medical Group, 2013. www.gov.uk/ government/publications/ at-a-glance Silverman D, Gendreau M. Medical issues associated with commercial flights. Lancet 2009;373:2067–77. Smith D, Toff W, Joy M, et al. Fitness to fly for passengers with cardiovascular disease. British Cardiovascular Society Working Group. Heart 2010;96:1–16. www.bcs.com/documents/BCS_FITNESS_ TO_FLY_REPORT.pdf Wilmshurst PT, Byrne JC, Webb-Peploe MM. Relation between interatrial shunts and decompression sickness in divers. Lancet 1989;2:1302–6. Moon RE, Camporesi EM, Kisslo JA. Patent foramen ovale and decompression sickness in divers. Lancet 1989;1:513–14. 8. 9. 10. 11. 12. Hackett PH, Roach RC. High-altitude illness. N Engl J Med 2001;345:107–14. Bartsch P, Gibbs JS. Effect of altitude on the heart and the lungs. Circulation 2007;116:2191–202. Crawford MH. Screening athletes for heart disease. Heart 2007;93:875. Corrado D, Basso C, Schiavon M, Thiene G. Screening for hypertrophic cardiomyopathy in young athletes. N Engl J Med 1998; 339:364–9. Maron BJ, Thompson PD, Ackerman MJ, et al. Recommendations and considerations related to preparticipation screening for cardiovascular abnormalities in competitive athletes: 2007 update: a scientific statement from the American Heart Association Council on Nutrition, Physical Activity, and Metabolism: endorsed by the American College of Cardiology Foundation. Circulation 2007;115:1643–55. www.trendsinurology.com