* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Premenstrual syndrome (PMS) - The University of Western Australia
Diagnostic and Statistical Manual of Mental Disorders wikipedia , lookup
Glossary of psychiatry wikipedia , lookup
History of mental disorders wikipedia , lookup
Schizoaffective disorder wikipedia , lookup
Narcissistic personality disorder wikipedia , lookup
Classification of mental disorders wikipedia , lookup
Spectrum disorder wikipedia , lookup
Bipolar II disorder wikipedia , lookup
Dissociative identity disorder wikipedia , lookup
Child psychopathology wikipedia , lookup
Asperger syndrome wikipedia , lookup
Generalized anxiety disorder wikipedia , lookup
Postpartum depression wikipedia , lookup
Conversion disorder wikipedia , lookup
Major depressive disorder wikipedia , lookup
Depression in childhood and adolescence wikipedia , lookup
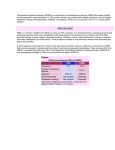
UNIVERSITY OF WESTERN AUSTRALIA SCHOOL OF ANATOMY AND HUMAN BIOLOGY Investigative Review: Premenstrual syndrome (PMS) Name: Nicole Mosseveld Student Number: 0220735 Unit Name: Human Reproduction 316 Unit co-ordinator: Neville Bruce Date Submitted: 5pm, 17-10-2005 Pages: 6 Premenstrual syndrome affects women of reproductive age to varying degrees, and the symptoms include physical, behavioural and emotional. Premenstrual dysphoric disorder (PMDD) is the more severe form of PMS, and like PMS, occurs during the last week of the luteal phase of the menstrual cycle. In order to diagnose women with PMS or PMDD certain criteria must be adhered to, in order to determine the prevalence of the disorder and most importantly, for the determining of effective treatment. PMDD can be treated using selective serotonin reuptake inhibitors (SSRIs) which act by blocking the receptors associated with neurotransmitters, and alleviating depression, which is associated with PMDD. The depression seen with PMDD patients may be caused by the fluctuating levels of gonadal hormones. It has been proposed that the cyclic changes in estrogen and progesterone during the menstrual cycle will have subsequent affects on the central nervous system (CNS) in regard to gamma-aminobutyric acid (GABA) and serotonergic systems in susceptible women. It is also suggested that the dysregulation of GABA due to PMDD may cause asymmetry in the amygdala resulting in mood changes. Therefore, there are many neuroendocrine changes that occur in women with PMDD that may result in depression. Premenstrual syndrome (PMS) is a generic term which includes a broad group of emotional, behavioural and physical symptoms, as seen in Table 1, which occur for several days to several weeks before menses and subside following the menstrual period4. What makes the symptoms distinct to this syndrome, is their cyclic nature. Table 1: Common Symptoms of PMS Physical Behavioural Swelling Breast tenderness Aches Headache Bloating/weight Sleep disturbances Appetite changes Poor concentration Decreased interest Social withdrawal Mood Irritability Mood swings Anxiety/tension Depression Feeling out of control 75% of women with regular menstrual cycles will experience some mild PMS symptoms such as breast tenderness and swelling during their reproductive years but do not perceive these symptoms as either distressing or debilitating1. Three to 15% will experience the more severe form known as Premenstrual Dysphoric Disorder (PMDD). PMDD is a disorder that occurs during the last week of the luteal phase of the menstrual cycle and is characterised by moderate to severe symptoms such as depressive mood, self depreciating thoughts, marked anxiety and tension affective lability, anger and irritability, difficulties in concentration, lack of interest in activities, lethargy, a sense of being overwhelmed, and suicidal ideation1. Women with PMDD experience marked disruptions in their relationships, and work and social activities that are similar to those with major depression1. Disorders such as PMDD are being treated increasingly by selective serotonin reuptake inhibitors (SSRIs) 8. SSRIs act by selectively blocking the reuptake of serotonin, resulting in and immediate increase in synaptic levels of serotonin6. Subsequent slow adaptive receptor changes in the brain lead to the alleviation of depression6. This occurs via the down-regulation of inhibitory presynaptic somatodendritic 5-HT1A receptors and inhibitory presynaptic terminal 5-HT1B which result in an increase of serotonin release6. The drugs ease of dosing and relatively safe side effects profile contributed to the SSRIs becoming the number one drug prescribed by psychiatrists8. However, in contrast to patients with major depression, PMDD patients respond better to lower doses of SSRIs and also to intermittent dosing2. Also response to treatment is seen within days compared to 2-4 weeks with depressive patients2. This suggests that PMDD and major depression are distinct clinical entities and thus should be diagnosed accordingly. Diagnostic criteria are important for aspects such as, distinguishing between PMS and PMDD, determining the prevalence of the disorder and most importantly, for the determining of effective treatment4. The criterion for the diagnosis of PMDD requires; five PMDD symptoms to be experiences at a severe level premenstrually, and must be low or absent postmenstrually4. The symptoms should appear to interfere markedly with relationships with others, in regard to work or school or other social activities4. The symptoms are found not to be exasperated by another physical or mental disorder, and the criteria must be confirmed by prospective daily ratings (for example via a questionnaire) for at least two consecutive menstrual cycles4. As depression is a major symptom seen in women with PMDD during the luteal phase of the menstrual cycle the criteria from the diagnostic and statistical manual of mental disorders forth edition (DSM-IV) is also used for diagnosis6. Depression is the leading cause of disease-related disability in women9. Studies have shown that the lifetime prevalence of a major depressive disorder in women is almost twice that of men9. The sex difference in prevalence first appears around the age of 10 years and persists until midlife, suggesting that women have the greatest risk for a first episode of depression or developing depressive disorders during their reproductive years9. These gender-based rates of depression include neuroendocrine factors specific to women5. Gonadal hormones are stable and low in prepubertal children; however, with the onset of menarche at puberty, the female brain is exposed to monthly surges of estrogen and progesterone, which continues until menopause5. This suggests that in susceptible women hormone fluctuation may contribute to mood change. Estrogen and progesterone are found in different brain regions and exert a wide range of actions on different neurons, including serotonergic (5-HT), noradrenergic (NE), gamma-aminobutyric acid (GABA), dopaminergic (DA) and anticholinergic neurons. Estrogen and progesterone receptors have also been identified in multiple brain regions, including the amygdala, hippocampus, and the midbrain raphe nuclei5. The mechanism by which estrogen and other steroidal hormones modulate serotonin and other neuronal systems is increasingly understood. By binding to intracellular receptors estrogen mediates a broad range of cellular effects; these include the transcription of genes that encode enzymes which regulate numerous pathways involved in the synthesis and metabolism of neurotransmitters, their receptors, and neurotransmitter transporters5. The serotonergic system is complex and involves numerous serotonin postsynaptic receptors, and dysregulation of postsynaptic serotonergic function has been implicated in depression5, as a function of serotonin, is to control of mood and emotion6. Clinical studies suggest that serotonin exerts an inhibitory influence on symptoms such as irritability, affect lability and depressive mood, suggesting that serotonin deficiency may lead to depressive symptoms. Estrogen and progesterone have also been shown to exert their effect on the central nervous system (CNS) serotonin reuptake transporter10. In humans serotonin is a neurotransmitter found in platelets and cells of the digestive tract. The reuptake of serotonin in platelets and the uptake of serotonin in brain transmitter terminals are similar active transport processes10. As for the serotonin transporter, the 5-HT2A receptors in platelets are similar to that of the human brain, thus making research into this area easier10. In studies in has been found that the number of platelet serotonin transporters (Bmax) is significantly lower in PMDD patients compared to normal subjects7,10. Bmax was at its lowest during the mid-luteal phase, when progesterone concentrations reach their peak10. On the other hand Bmax reached its maximum during the late follicular phase during the pre-ovulatory estrogen peak10. This suggests that the high and fluctuating endogenous concentrations of steroid hormones in reproductive women affect these serotonergic measures. The fluctuating concentration of estrogen and progesterone may also have an affect on the amygdala brain region. In women without PMDD the neurotransmitters GABA and serotonin peak premenstrually, during the luteal phase, and decline during the follicular phase of the cycle1. In contrast the normal premenstrual peak serum levels of these neurotransmitters are absent during the late luteal phase of the cycle for women with PMDD1. Thus clarifying (as above) that serotonin deficiency may lead to depressive symptoms. Both serotonin and GABA mediate inhibitory input to the amygdala, a structure known to connect to the frontal cortical areas of the brain 1. Recent studies have shown that asymmetry in the activity of neurons in frontal cortical areas is a correlate of affect1. Meaning that the affect is mediated by a combined action of a positive emotion/approach system in the left frontal cortex, and a negative emotion/avoidance system in the right frontal cortex1. Thus if right frontal activity exceeds left frontal activity, a depressive affect results. It was found that with PMDD, which is associated with profound affective psychopathology and characterised clinically by extreme negative effect, there were changes in the prefrontal cortex during the luteal phase, in the direction of greater right that left cortical activation. One of the specific effects of PMDD is a profound reduction of the GABA neurotransmitter during the luteal phase of the menstrual cycle. GABA is known to function as an inhibitory transmitter throughout the nervous system, exerting a tonic inhibitory effect on many neurons including those in the dorsal and ventral regions of the amygdala1,3. The amygdala is known to play an important role in the elaboration of negative emotion, and shows asymmetrical responses to different kinds of emotionrelevant input3. Normal subjects display more actively in the right amygdala in response to negative stimuli, compared to women with PMDD where the amygdala showed increased activity in both the left and right amygdala1. This suggests that if the inhibitory ability of GABA to keep mildly aversive stimuli from overexciting the amygdala is compromised, as with PMDD, the normally regulated negative emotions and non-dangerous stimuli may generate an unnecessary amount of fear and anxiety1. In conclusion, premenstrual syndrome (PMS) and premenstrual dysphoric disorder (PMDD) are common, but relatively hard to diagnose, as timing, type and severity of symptoms as well as the prevalence of other mental disorders, can interfere with its diagnosis. The symptoms occur in a cyclic fashion and the fluctuations in estrogen and progesterone have a profound effect. Hormonal fluctuations affect the serotonergic system in susceptible women, such as those with PMDD as serotonin deficiency and a decreased Bmax lead to depressive symptoms. PMDD can be treated with SSRIs which selectively block the reuptake of serotonin, resulting in and immediate increase in synaptic levels of serotonin and alleviating depression. The decrease in GABA also leads to increased amounts of fear and anxiety in women with PMDD, and also as a result of decreased GABA the left and right amygdala activity increases. Therefore, PMDD in particular is considered an important disorder that involves numerous neuroendocrine factors. Further study may include other women’s illnesses such as postpartum depression and perimenopausal depression, and perhaps their linkage to PMDD via common genes. References 1. Baehr E, Rosenfeld P, Miller L, Baehr R, (2004) Premenstrual dysphoric disorder and changes in frontal alpha asymmetry. Psychophysiology 52, 159-167. 2. Cohen L, Soares C, Otto M, Sweeney B, Liberman R, Harlow B, (2002) Prevalence and predictors of premenstrual dysphoric disorder (PMDD) in older premenopausal women The Harvard Study of Moods and Cycles. Affective Disorders 70, 125-132. 3. De Ronchi D, Manjola U, Boaron F, Muro A, Piselli M, Quartesan R, (2005) Symptoms of depression in late luteal phase dysphoric disorder: a variant of mood disorder? Affective Disorders 86, 169-174. 4. Freeman E, (2003) Premenstrual syndrome and premenstrual dysphoric disorder: definitions and diagnosis. Psychoneuroendocrinology 28, 25-37. 5. Joffe H, Cohen L, (1998) Estrogen, serotonin, and mood disturbance: where is the therapeutic bridge? Elsevier Science Inc 6. Lulich KM, (2003) CNS Pharmacology: Antidepressants. Lecture 6. Department of Medicine and Pharmacology, The University of Western Australia. 7. Melke J, Westburg L, Landen M, Sundblad C, Eriksson O, Baghei F, Rosmond R, Eriksson E, Ekman A, (2003) Serotonin transporter gene polymorphisms and platelet [3H]paroxetine binding in premenstrual dysphoria. Psychoneuroendocrinology 28, 446-458. 8. Metzi J, Angel J (2003) Assessing the impact of SSRI antidepressants in the popular notions of women’s depressive illness. Department of Psychiatry and Women’s Studies Program, University of Michigan 9. Noble R, (2005) Depression in women. Metabolism Clinical and Experimental 54, 49-52. 10. Wihlback A, Sundtrom Poromaa I, Bixo M, Allard P Mjorndal T, Spigset O, (2004) Influence of menstrual cycle on platelet serotonin uptake site and serotonin2A receptor binding. Psychoneuroendocrinology 29, 757-766.