* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Anatomy and physiology of the cardiovascular system
Survey
Document related concepts
Cardiac contractility modulation wikipedia , lookup
Electrocardiography wikipedia , lookup
Heart failure wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Cardiac surgery wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Jatene procedure wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
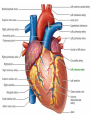
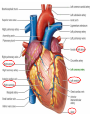
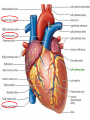
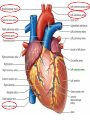
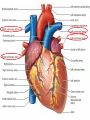
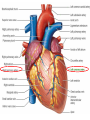
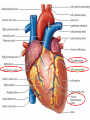
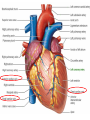
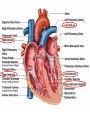
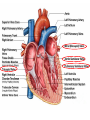
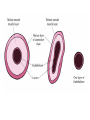
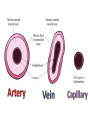
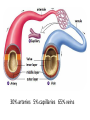
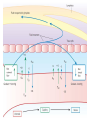
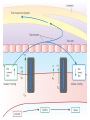
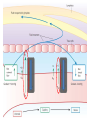
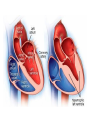
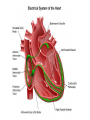
Anatomy and physiology of the cardiovascular system Dr Cath Spoors Consultant, Anaesthesia and Burns Intensive Care Broomfield Hospital, Chelmsford Cardiovascular system • Giant circular shuttle system • Transport – Oxygen, nutrients, cells – CO2, waste products • Distribution – The right stuff to the right place at the right time What price failure? What price failure? What price failure? What price failure? What price failure? 30% arteries 5% capillaries 65% veins Large arteries • Elastic arteries – large and proximal. Vessel wall distension in the presence of a competent aortic valve acts as a secondary pump • Muscular arteries – high-pressure conduits. Pressure waves within them are palpable as peripheral pulses. Arterioles • Control of local blood flow • Major determinant of systemic vascular resistance (SVR) and therefore blood pressure • Independent in any given organ bed (control distribution of cardiac output around the body) • Influence capillary hydrostatic pressure Control of blood flow • Myogenic – stretch causes vasoconstriction, slackening causes vasodilation. Important in brain and kidney Control of blood flow • Metabolic – substances produced by active tissues cause vasodilatation to “attract” more blood to the area (bradykinin, CO2). Hypoxia also causes vasodilatation • Sympathetic – basal arteriolar tone. α1 receptors – vasoconstriction (most beds esp skin, gut, kidneys). Β2 receptors – vasodilatation (skeletal muscle). Brain and heart less affected by neurogenic control • Hormonal – adrenaline on adrenoceptors Capillaries • Continuous – muscle, brain, connective tissue. Cells joined by tight junctions. Water, oxygen, carbon dioxide and small water-soluble molecules can pass relatively easily. Larger molecules must be transported across • Fenestrated – intestine, kidneys. Contain pores which allow rapid exchange of water and small molecules • Sinusoidal – liver, bone marrow – whole blood can pass out into the interstitium Capillaries • Gradients Capillaries • Gradients Capillaries • Gradients Veins and the venous reservoir • Low-pressure system for conducting blood back to heart • Valves to prevent stasis • Distend – can accommodate large volumes with little pressure change. “Buffer” for blood volume • Venous reservoirs in lungs, liver, gut and skin – under sympathetic control • Skeletal muscle augments return of venous blood to heart • Respiratory pump increases intrathoracic and right ventricular volume by sucking in blood from veins Cardiac output • The volume of blood pumped out of the left ventricle per unit time • Approx 3.5-7.5L/min in adults Cardiac output • The volume of blood pumped out of the left ventricle per unit time • Approx 3.5-7.5L/min in adults Cardiac output • The volume of blood pumped out of the left ventricle per unit time • Approx 3.5-7.5L/min in adults Venous return • The volume of blood returned to the right atrium per unit time Cardiac output • The volume of blood pumped out of the left ventricle per unit time • Approx 3.5-7.5L/min in adults Venous return • The volume of blood returned to the right atrium per unit time Determinants of stroke volume • Preload • Afterload • Contractility Determinants of heart rate • Autonomic function • Dysrhythmias • Pacemakers Preload • Myocardial muscle cells obey Starling’s law (force-length relationship) Preload • Myocardial muscle cells obey Starling’s law (force-length relationship) Preload • Myocardial muscle cells obey Starling’s law (force-length relationship) Determinants of preload • Volume status – Hypovolaemia reduces pre-load and cardiac efficiency – Hypervolaemia over-distends the right heart and reduces efficiency • PEEP – High PEEP (recruitment manoeuvres) can reduce venous return by increasing thoracic pressure which impedes flow into the heart • Arrhythmias – The chambers need time to fill; if the duration of diastole is reduced this will impede ventricular filling • Regurgitant cardiac valves • Cardiac tamponade Afterload • The force opposing shortening of muscle fibres during contraction • Increases in afterload will reduce the stroke volume • Increases with increased pressure in the chamber cavity • Increases with diameter of the chamber cavity • Decreases with wall thickness Afterload • Most afterload is provided by systemic vascular resistance • Arterial dilatation will reduce afterload but this may compromise coronary perfusion Afterload • Most afterload is provided by systemic vascular resistance • Arterial dilatation will reduce afterload but this may compromise coronary perfusion Contractility • This is the contractile energy of the heart not related to preload or afterload • Increased contractility will give an increased stroke volume • Increased by – Sympathetic stimulation (catecholamines) – Extracellular calcium levels – Increased heart rate (Bowditch effect) • Decreased by – – – – Ischaemia Drugs Sepsis Toxins Contractility • This is the contractile energy of the heart not related to preload or afterload • Increased contractility will give an increased stroke volume • Increased by – Sympathetic stimulation (catecholamines) – Extracellular calcium levels – Increased heart rate (Bowditch effect) • Decreased by – – – – Ischaemia Drugs Sepsis Toxins Determinants of heart rate • In sinus rhythm, the SA node determines the heart rate • Control is by reciprocal action of sympathetic and parasympathetic nerves • Circulating catecholamines also increase heart rate • β1 adrenoceptors in the SA node speed up; muscarinic (parasympathetic) slow down • Optimisation is the key to heart rate manipulations – trade off between cardiac work (oxygen demand), output, and venous return (filling)