* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download MCB 32, FALL 2000
Heart failure wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Electrocardiography wikipedia , lookup
Coronary artery disease wikipedia , lookup
Artificial heart valve wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Cardiac surgery wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Jatene procedure wikipedia , lookup
Myocardial infarction wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
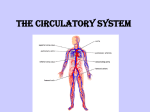
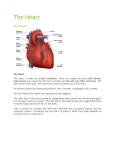
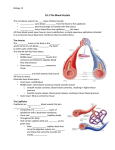
MCB 32, FALL 2000 CARDIOVASCUAR SYSTEM ANATOMY AND PHYSIOLOGY Reading: Chapters 8 and Chapter 9 I. Diffusion and bulk flow Diffusion delivers substances over short distances (10-200 µm). If distances are longer than this, then diffusion is a very slow process. Bulk flow required for rapid delivery of substances over long distances like those in the cardiovascular system, e.g., delivery of nutrients from the gastrointestinal tract to the tissues of the body and delivery of wastes from the tissues to the kidneys. II. Blood composition Blood is composed of cells (approx 50%) and plasma (approx 50%). Red blood cells are produced in bone marrow and are basically bags of hemoglobin, which is responsible for binding oxygen in the lungs, delivering and then releasing it to the tissues. This function will be discussed later in the Respiration portion of the course. White cells are involved in specific and non-specific defenses of the body. This will be discussed during Immunology. Plasma contains all the nutrients and waste products circulating in the blood stream, and also plasma proteins (many of these are antibodies that are available to fight infectious agents. Plasma composition of salts and water are largely the same as those in the tissues, i.e., high [Na] and [Cl] low [K]. III. General anatomy of the circulatory system: Fig. 8.1 Systemic (L heart, aorta, arteries, capillaries, veins, vena cava) and pulmonary (R heart, pulmonary artery, arterioles, lung capillaries, veins, pulmonary vein) circulations. Series and parallel arrangements of blood vessels: blood flows in series through systemic and pulmonary circulations, while it flows in parallel to the muscles and the kidneys and gastroinestinal tract. The body must be able to control the distribution of the blood so that the metabolism of each tissue can be provided with proper blood supply. IV. Heart anatomy: Fig. 8.6 Left and right hearts in chest cavity, bounded by diaphragm Pericardium connective tissue covering Left atrium (blood collection from pulmonary circulation) and ventricle (propulsion; thick wall due to large pressures involved). Right atrium (blood collection from vena cava and systemic circulation) and ventricle (propulsion; thinner wall due to lower pressures in pulmonary circulation) Coronary blood flow refers to blood that flows in arteries, capillaries and veins that go directly to the heart itself. Little of the heart’s nutrients come from the blood inside the heart. Coronary supply is critical to operation of heart, since interruption of blood supply leads to inadequate supply of oxygen. If coronary vessel become blocked, this leads to death of some portion of the heart tissue and a heart attack. Valves: connective tissue with attached chordae tendinae to prevent eversion. Valves move only passively in response to pressures on each side. One-way operation to assure correct diretional movement of blood during pulsatile contraction and relaxation of heart. Make sounds as they close. Sometimes close incompletely, leading to murmur (turbulent blood flow is noisy, in contrast to laminar flow) Note that the left and right hearts perform quite different functions. Left heart pumps blood to many different organs and does so by generating high pressures. Right heart pumps blood only to the lungs and does so by generating only low pressures. Left heart is therefore thicker than right heart. V. SA node is the cardiac pacemaker; conduction system assures orderly electrical excitation: Fig. 8.6 Coordinated activity of heart is necessary. If electrical activity occurred randomly, contraction would similarly be random, and there would be no possibility for efficient contraction of atria followed by the ventricles. Electrical activity begins in sino-atial node, which has the capability to generate its own action potentials, at rate of heart beat. AP gap junctions electrical excitation followed by contraction throughout the atria. AP AV node and Purkinje fibers, specialized set of fibers with less contractile ability but good transmission capability. Purkinje fibers ventricular musculature VI. Frequency of action potentials from SA node can be modulated by autonomic nervous system: Fig. 8.7 Sympathetic nerves release norepinehrine onto the cells of the heart (including those in the SA node – see below), which speeds rate at which action potentials are generated in the cells, increasing the rate of contraction. Parasympathetic nerves (primarily the vagus) release acetylcholine onto the cells of the heart (including the SA node – see below), which slows rate of action potentials, slowing rate of contraction of heart. VII. Coordinated activity of the heart: Fig. 8.10 SA node action potential atria contract Atrial systole Action potential --> AV node and conducting system ventricles contract Pressure in ventricle rises atrio-ventricular valves shut (first heart sound), with no change in volume (isometric or isovolumetric contraction) Pressure in ventricle > aortic pressure, valve opens, blood ejected (isotonic contraction), arterial pressure rises to systolic level. Ejection phase. Ventricular systole End of action potential, ventricular musculature relaxes (ventricular diasotle) aortic valve closes (second heart sound) Blood begins to fill atria and ventricles VIII. Control of heart rate by autonomic nerves: Fig. 8.8 Control center: medulla oblongata. This region of the brain stem receives information from the peripheral blood pressure monitors, including the pressure receptors in the aorta and large arteries and also in the heart itself. Sympathetic nerves increase rate of depolarization increase frequency of AP in SA node. This response occurs during “fight or flight” situations, or during exercise. Parasympathetic nerves decrease rate of depolarization reduce frequency of AP in SA node. This response occurs during times when cardiovascular system needs to reduce blood pressure and maintain vegetative state. IX. Control of cardiac output CO (liters/min) = stroke volume (ml/beat) x heart rate (beats/min) Normal human CO = 5 l/min = 72 ml/beat x 70 beats/min Control by changing heart rate (sympathetic increase, parasympathetic decrease) and stroke volume. Stroke volume can be changed by altering contractility of heart muscle, usually increased by sympathetic nerves. This increases amount of force generated by the myosin and actin, often through changes in cell [Ca]. Stroke vol also changed by alterations of size of heart (length tension diagram of muscle). This in turn controlled by venous return. X. Structure and functions of blood vessels: Figs 9.3 – 9.9 All are lined with endothelium, thin layer of cells connected by tight junctions, function: provide smooth surface for blood flow. Amount and types of connective tissue and smooth muscle vary with type of vessel. Arteries Large diameter compared to other vessels, lots of connective tissue to support high pressures present inside One artery per organ Store P energy of heart, for smooth distribution of blood during diastole. This is shown well in Fig. 9.2. Arterioles Smaller, great deal of muscle compared to size of vessels Sites of controlled resistance, regulated by nerves, hormones and, most importantly, by paracrine factors produced by the tissues themselves. Thus, there can be localized regulation of blood flow. Arterioles are the vessels that are most important for controlling pressures and flows in CV system. Three mechanisms for regulating blood flow through arterioles: 1. Myogenic autoregulation: mechanism for maintenance of constancy 2. Metabolic control by paracrines: lactic acid or other metabolites are produced during periods of intense metabolic activity. Accumulation of these products causes smooth muscle to relax, leading to increased blood flow to the affected tissue. No nerves required for this response. 3. Sympathetic control: increase constriction to increase pressure Veins Veins are low resistance (easy to force blood through them) reservoirs (have large volume of blood in them). Veins are larger in diameter than arterioles and also have less connective tissue and smooth muscle because pressures are low. Valves (Fig. 9.5) assure one-way movement of blood back to the heart. Muscle and respiratory pumps refer to the increased blood flow through the veins that occur during exercise: rhythmic changes in contraction and relaxation of the skeletal muscles, and also the increased depth and rate of breathing, which reduces pressure surrounding veins near the heart and thereby increases blood flow back to the heart. Capillaries: Fig. 9.4 Small diameter, low rate of flow, very large number (nearly one per cell of body) Delivery of nutrients to tissues and elimination of wastes (CO2, lactic acid etc) occurs by diffusion. Water exchange across capillaries. Fluid exchange across the capillaries is by filtration (pressure due to heart’s pumping forces fluid out of capillaries into tissue spaces) and by osmosis (large plasma proteins pull water into the capillaries). Figs 9.15 and 9.16 Imbalance of forces often leads to edema (collection of excess tissue fluid), e.g., in heart patients. Lymph vessels collect excess tissue fluid and proteins These are blind-ended capillary-like structures that are very permeable to proteins and fluids. They collect the excess tissue fluid, which then circulates through larger and larger vessels, ultimately back into the venous system. The flow of fluid though the lymph vessels appears to occur like that through the veins, with valves and muscle pumps.