* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download What Is a Heart Attack Really Like? - Dartmouth
Remote ischemic conditioning wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Saturated fat and cardiovascular disease wikipedia , lookup
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Cardiac surgery wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Coronary artery disease wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
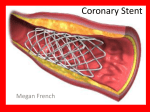
Advances in the Treatment of Coronary Artery Disease Craig A. Thompson, M.D., MMSc. Director, Cardiovascular Catheterization Laboratories Dartmouth Hitchcock Medical Center Dartmouth Medical School How Your Heart Functions • • • The heart pumps blood throughout the body. Blood carries oxygen and nutrients. Coronary arteries carry oxygenated blood to the heart muscle, much like garden hoses might water the lawn to maintain vitality Coronary anatomy • • • • • • 4 “Primary” Arteries run on surface of the heart These arteries have many “branches” that can reach all parts of the heart muscle Left Main (LM) • LAD • LCx Left anterior descending (LAD) • Diagonals • Septals Left circumflex (LCx) • Obtuse marginal (OM) • Left PDA? Right coronary artery (RCA) • PDA • PLV TERMINOLOGY Heart Attack Cardiac Arrest Heart Failure Sudden blockage of coronary artery Caused by ventricular arrhythmia Weakness of heart muscle or inability to pump blood to organs Atherosclerosis and the development of angina Advances in the Treatment of Coronary Artery Disease improvements in medical therapy • • • • • • Aspirin Beta Blockers “Statins” Plavix ACE inhibitors Others New Medicines improve symptoms, prolong life, reduce the likelihood of heart attack, stroke, and death!!! Different Presentations of Coronary Disease one size does not fit all No symptoms Stable angina Unstable Angina •Symptoms and exam NSTEMI STEMI Small “warning” heart Ongoing heart attack attack •EKG - electrocardiogram •Bloodwork (“cardiac enzymes”) How Does a Heart Attack Happen? Courtesy Possis Medical What People Expect a Heart Attack to be Like • Crushing chest pain • Sudden, intense, falls to the floor—like in the movies What Is a Heart Attack Really Like? • Heart attacks often begin with vague symptoms that slowly intensify. • Pain or discomfort can be relatively mild. • Symptoms may come and go. • Variety of symptoms may signal danger. Heart Attack Warning Signs • Chest discomfort—pressure, squeezing, fullness, or pain in center of chest • Discomfort in one or both arms, back, neck, jaw, or stomach • Shortness of breath, may come before or with chest discomfort • Breaking out in a cold sweat • Nausea • Light-headedness I have symptoms of Heart Attack what to do? • Chew an aspirin • Seek medical attention (911, emergency department, contact physician) • Medicines • Oxygen • Blood pressure • Heart rate/rhythm • Pain control • Blood thinners (heparin, low molecular weight heparin, glycoprotein 2b/3a blockers) • Thrombolytics (“clot buster”) • Cardiac catheterization and intervention Why People Delay • Think symptoms are due to something else • Afraid or unwilling to admit symptoms are serious • Embarrassed about: • “Causing a scene” • Having a false alarm • Do not understand need for getting to hospital fast Heart Attacks in Women • Women are as vulnerable as men. • Half of all heart attack deaths are in women. • Tend to delay longer than men in seeking help. Heart Attacks in Women • Like men, may feel pain or discomfort • Somewhat more likely to experience: • Shortness of breath • Nausea/vomiting • Back or jaw pain • Tend to delay telling others about symptoms to avoid causing bother or worry Non-DHMC Emergency Dept AMI diagnosed >30 min of CP and/or ECG with 1mmST elevation or LBBB Oxygen, ASA, low dose heparin, beta blocker, nitrates, Morphine, 2 IV lines, treat pain, CHF, shock, arrhythmias December 2001 Facilitated PCI Remote ER and Age < 75 Administer abciximab and ½ Dose Thrombolytic Acute Primary PCI ST elevationPrimary MI is Thrombolytic Therapy now on the DHMC “ALWAYS Alice Peck Day or TAKE” list VA Hospital Contraindication for Thrombolytic therapy/ abciximab Full Dose Thrombolytic Administer abciximab Transport to DHMC Cath Lab ASAP Transport to DHMC for potential salvage PCI ASAP DHMC Cardiovascular Catheterization Laboratories Interventional Gear the standard issue Guiding catheters Guidewires Deployed stent Stent on balloon Angioplasty balloon Rotoblator Removal of Blood Clot Courtesy Possis Medical Coronary Stents BxVelocity™ Stent Express2™ Stent Liberté™ Stent Express2™ Stent, Liberté™ Stent and BxVelocity™ Stent with equal amount of torque applied (0.576 N. mm). Stent size is 3.0 x 28 mm. Bench testing performed internally by Boston Scientific. Data on file. N=3. Bench test results not necessarily indicative of clinical performance. All images taken by Boston Scientific. Actual values may vary. Stent Placement Courtesy Possis Medical Drug eluting stents Courtesy Possis Medical Evolution of Angioplasty The Dominant Coronary Revascularization Therapy Over the last 30 years, percutaneous coronary intervention (PCI) has undergone progressive improvements in success, safety, and durability, as serial new technologies have been launched. While each innovation solved a serious prior problem, it has sometimes introduced rare new adverse events (e.g., 40 restenosis, stent thrombosis). in-stent Event Rate % 30 20 10 0 Failure Em CABG Restenosis Stent thrombosis VLST POBA early 1977 Dr. Don Baim, FDA Panel Meeting December 2006 Current results of DES-PCI are the BEST they have ever been. POBA late 1985 Stent early 1994 Innovations over time Stent late 1997 DES 2003-present Doctors Rethink Widespread Use Of Heart Stents By BARNABY J. FEDER Published: October 21, 2006 Doctors study risk of clots in new stents Incidence in drug-eluting models is extremely low but usually very serious By Stephen Heuser, Globe Staff | October 21, 2005 Benefit Risk Number of Revascularizations TAXUS® Stent BMS TAXUS® Stent BMS Identical long term risk for TAXUS® Stent and BMS = Large MI = Death Boston Scientific, Data on File. TAXUS Stent 4-year meta-analysis includes TAXUS II (4 yr), IV (4 yr), V (2 yr), VI (3 yr). With a >50% improved benefit through sustained reduction in need for revascularizations What Should Patients Really Be Concerned About? • If I have a TAXUS® Stent vs. a BMS… • What are my chances of death or having a large MI at the end of 4 years? • The chance of death are the same or lower with the TAXUS Stent vs. BMS • This annual death rate of 1.5% per year represents roughly the background rate seen in the “natural history” of patients with stable CAD • Should I be concerned about stent thrombosis? • • • • Given the identical or lower death and MI rate, why should I have a TAXUS Stent? • • • Late stent thrombosis is a low frequency event (0.5% over 4 years) It is just one small contributor to the risk of death or MI Looking at all causes, the chances of dying or having a large MI at the end of 4 years are still equivalent or less with the Taxus Stent versus a BMS Restenosis and repeat procedures can also cause major complications The TAXUS Stent prevents restenosis and reduces the need for a repeat procedure by half (from ~20%, to 10% percent or less) Is there anything else different if I get a TAXUS Stent? • • With a TAXUS Stent, you need to take Plavix® Medication for at least 6 months (or longer if recommended by your doctor) Prematurely stopping your Plavix Medication can increase your risk of stent thrombosis The safety and effectiveness of the TAXUS Express Stent have not been established in patients for longer than 12 months. Core Topics DHMC…the present and future Integrated imaging and telemedicine Conclusions • Heart attack is a major cause of death and disability in the US each year • Early recognition of symptoms and evaluation by medical personnel improves outcomes • Best therapy in 2005 includes medicines for heart rate/rhythm control, blood pressure management, and to thin blood to stabilize or dissolve clots • Best therapy in 2005 includes cardiac catheterization with coronary angiography, and if appropriate, intervention (angioplasty) or surgery • Risk factor modification is important both to prevent initial and recurrent coronary events