* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download this PDF file - Pacific Group of e
Remote ischemic conditioning wikipedia , lookup
Coronary artery disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Electrocardiography wikipedia , lookup
Pericardial heart valves wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Cardiothoracic surgery wikipedia , lookup
Artificial heart valve wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Atrial fibrillation wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
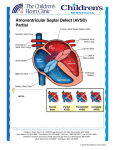
Original Article Observational Study of surgical closure of Ostium Primum Atrial Septal Defect in thirty paediatric patients Suraj Wasudeo Nagre1, Manisha Suraj Nagre2 1 2 Department of CVTS, Grant Medical College and J J Hospital, Mumbai, India Kasturba Hospital, Mumbai, India Keywords: Premum ASD, Atrioventricular Septal Defect, Partial AV Canal Abstract Primum atrial septal defect (ASD) is a common congenital cardiac anomaly that is typically repaired in the first years of life. Patients with isolated ostium primum atrial septal defects (ASDs) have benefited from important recent advances in the diagnosis, evaluation, and management of their conditions. Operative correction typically involves pericardial patch closure of the septal defect and closure of associated left atrioventricular valve cleft. This review will focus on thirty paediatric patients with sizeable ostium primum atrial septal defects who do not have other major associated cardiac defects. *Corresponding author: Dr Suraj Wasudeo Nagre, 31, Trimurti Building, J J Hospital Compound, Byculla, Mumbai, 400008, India Email [email protected]; Mobile +91-9967795303 This work is licensed under the Creative Commons Attribution 4.0 License. Published by Pacific Group of e-Journals (PaGe) Original Article A-2 INTRODUCTION Unlike a ostium secundum atrial septal defect (ASD), the ostium primum form of ASD is not amenable to device closure in the cardiac catheterization laboratory. The device is unable to be adequately seated secondary to an inadequate inferior rim of atrial septal tissue and the proximity of the defect to the atrioventricular (AV) valves. A left-to-right atrial shunt is considered significant when the Qp/Qs ratio is greater than 1.5/1.0, or if it causes dilation of the right heart chambers.1,2As a rule, an ASD must be at least 10 mm in diameter to carry a significant left-to-right shunt, although most ASDs are not circular, and maximum diameter may be difficult to measure accurately. Effort intolerance is the most common initial presenting symptom in children. Atrial fibrillation or flutter is an age-related reflection of atrial dilation and stretch that seldom occurs at <40 years of age3.In ECG the rhythm may be sinus, atrial fibrillation, or atrial flutter.First-degree heart block suggests a primum ASD 4 but may be seen in older patients with a secundum ASD.QRS axis is leftward or extremely to the right in ostium primum ASDs (OP ASDs). On chest X ray cardiomegaly may be present from right heart dilation and occasionally from left heart dilation if significant mitral regurgitation is present in the patient with an ostium primum ASD.5,6The central pulmonary arteries are characteristically enlarged, with pulmonary plethora indicating increased pulmonary flow. Transthoracic echocardiography documents the type(s) and size of the ASD(s), the direction(s) of the shunt, and, in experienced hands, the presence of anomalous pulmonary venous return.In a patient with a primum ASD, the left AV valve is trileaflet and almost always demonstrates some regurgitation. Patients with an isolated ostium primum ASD are typically referred for elective repair between the ages of 2 and 5 years. Some patients may reach adulthood without symptoms or ignoring the symptoms. In our study, children have tolerated surgery well as a whole. Pulmonary hypertension and elevated pulmonary vascular resistance do not appear to be contraindications and generally improve postoperatively. Long-term follow-up is requisite. atriotomy placed anteriorly, close to the atrioventricular junction gives excellent exposure of the atrial septum and both atrioventricular valves. The location of the coronary sinus as a landmark for the adjacent AV node, and the fossa ovalis with a potential secundum defect should be noted. Saline instillation into the left ventricle closes the mitral valve to allow an initial assessment of competency and the anatomy of the components of the anterior leaflet. The cleft closure is performed beginning at the base of the cleft, nearest the ventricular septum. I prefer a technique using horizontal mattress sutures of fine Prolene that keep the edges of the leaflets rolled under, causing less distortion of the valve. The distance between the points where the AV valve tissue meets the AV annulus superiorly and inferiorly is measured [FIGURE 1 ]. It is important to make the portion of the patch that attaches between these points slightly smaller than this distance. This will create a slight annuloplasty effect as well as prevent lateral tension on the cleft closure. After cleft closure the competence of the valve should be tested and annuloplasty stitches may be added adjacent to one or both commissures, if needed. Attachment of the autologous, gluterladehyde-fixed pericardial patch for closure of the septal defect is begun at the mid-point of the valve, adjacent to the base of the closed cleft. Tying down the first stitch allows superior or inferior traction on this suture which facilitates identification of the right-left leaflet junction for attaching the remainder of the base of the patch to the ventricular septal crest. Inferiorly, as the patch is attached within the atrium moving away from the valve, care must be taken to avoid injury to the AV node and His bundle [FIGURE 2 ]. MATERIALS AND METHODS Thirty patients (20 males, 10 females; mean age 32.4+/-11.1 years; range: 2 to 5 years) who had surgical repair of OP-ASD between 2010 and 2015 were followed. All patients were examined physically and underwent chest radiography, ECG and echocardiography (cross-sectional and Doppler) before and after surgery. Cardiopulmonary support utilizing bicaval cannulation and mild hypothermia is employed. A longitudinal right Figure 1: Ostium Primum Atrial Septal Defect with normal Tricuspid and Mitral Valve [No Anterior Mitral Valve Leaflet Cleft ] An additional PFO or small secundum ASD is usually closed separately using a primary suture technique, or may be incorporated into the lateral attachment of the pericardial patch. http://www.pacificejournals.com/awch A-3 AWCH; 1(1): 2015 DISCUSSION During fetal development, the rudimentary atrium is divided by the septum primum, except for an anterior and inferior space that is the ostium primum. The ostium primum is sealed by fusion of the superior and inferior endocardial cushions around 5 weeks' gestation. Failure to do so results in an ostium primum ASD. The endocardial cushions also contribute to the complete formation of 2 separate AV valves and the inlet interventricular septum. For this reason, ostium primum ASDs commonly are associated with malformations of these structures. Figure 2: Closed ostium primum atrial septal defect with pericardial patch, associated patent foramen ovale also seen Intraoperative transesophageal echocardiography is routinely used following weaning from bypass to assess the repair. In our practice we plan for extubation in the operating room, observation overnight in the cardiac ICU, and a typical inpatient stay of 3 to 4 days.Patients often require inotropic support and/or afterload reduction in the early postoperative period. Atrial pacing restores AV synchrony and may be beneficial to reduce AV valve insufficiency and increase cardiac output. RESULT Autologous pericardium was used to close the defect in all patients. Mitral valvuloplasty (repair of the cleft) was performed in 16patients, and De Vega annuloplasty in five .The abnormal AV junction results in an “unwedged” aorta and leads to a displacement of the AV conduction tissue, which in turn produces the characteristic left-axis deviation and predisposes these patients to heart block.The most common associated anomalies are a secundum ASD and a persistent left SVC draining into the coronary sinus. The occurrence of surgical complete heart block in these patients has practically disappeared in the modern era.11 There were no hospital deaths. In one case a pacemaker was implanted five days after surgery because of complete heart block. Preoperatively, eighteen patients (60%) were in NYHA classes III and IV; at the end of follow up, 28 (93.3%) were in classes I and II. The preoperative mean cardiac volume index of 660 +/- 208 ml/m(2) was reduced significantly after repair to 512 +/102 ml/m(2) (p < 0.05). Before surgery, mitral regurgitation was observed (severe in five cases, moderate in fifteen, mild in ten). Postoperatively, a residual intracardiac shunt was identified in one case. Postoperative mitral regurgitation was noted in six patients (moderate in two, mild in four). The right ventricular dimension was decreased significantly, from 5.2 +/- 1.4 mm before surgery to 3.4 +/- 0.4 mm after repair (p < 0.001). Ostium primum ASDs are most commonly seen with a cleft in the anterior leaflet of the mitral valve, but they may occur in isolation. This is sometimes termed a partial AV canal defect or a partial AV septal defect. In this case, a 5-leaflet AV valve is arranged so that separate right and left components (a tricuspid valve and a mitral valve) are present. The leaflets connect to each other and then adhere to the crest of the interventricular septum. This results in shunting at the atrial level with no ventricular level shunting. Generally, a commissure is observed between the left superior and inferior bridging leaflets because of abnormal fusion of the left tubercle of the superior and inferior cushions, which results in a cleft in the anterior leaflet of the mitral valve. Pathophysiology: Shunting is predominantly left-to-right in the absence of pulmonary vascular disease or significant right ventricular outflow tract obstruction. This results in volume overload of the right atrium and ventricle and pulmonary overcirculation. If the mitral valve cleft causes significant mitral regurgitation, the left side of the heart also becomes volume overloaded. A left ventricle to right atrium shunt can be present, which further overloads both the right and left heart. Etiology: The most common cause of an ostium primum ASD is genetic, associated with trisomy 21. Well-described associations have been reported with Holt-Oram syndrome, Noonan syndrome, and Ellis-van Creveld syndrome, among others. In children with normal chromosomes, however, the cause remains unknown. Research into the molecular genetic basis for AV canal and AV septal defects is ongoing. The male-to-female ratio is 1:1. Patients with smaller defects and little or no mitral regurgitation may present at any age with a murmur and/or an abnormal ECG. Those with more severe mitral regurgitation typically present with CHF in the first 1-2 years of life. Prognosis: Pediatric patients with small left-to-right shunts and no significant mitral regurgitation who have not undergone surgery are at relatively low risk for Annals of Woman and Child Health, Vol. 1; Issue 1: 2015 Original Article A-4 complications. In these patients, adult survival is expected, but complications can develop as age advances. Untreated patients with large shunts and/or significant mitral regurgitation are at significant risk of morbidity and mortality. Death, arrhythmia, heart block, refractory heart failure, and advanced pulmonary vascular disease are the most common complications and tend to increase with advancing age. Pulmonary vascular obstructive disease may develop in a subset of patients, with patients with Down syndrome at highest risk. Prognosis is guarded, and morbidity and mortality are high regardless of therapy. Surgical repair generally improves life expectancy and alters the natural course of the disease. Age and preoperative moderate-to-severe left AV valve regurgitation were predictors of reoperation. None declared. REFERENCES 1. 2. 3. CONCLUSION Patients aged between 2 to 5 years with OP ASD will benefit from surgical repair of the defect. Sizeable OP ASDs with right heart dilation are associated with important age-related morbidity and mortality. Advanced diagnostic modalities, earlier closure, and the advent of catheter intervention (for OP ASDs) are all likely to improve long-term prospects for these patients. Current evidence would suggest that all types of OPASDs with right heart dilation should be considered for timely closure once the diagnosis is established, irrespective of age. ACKNOWLEDGEMENTS None. 4. 5. 6. Gatzoulis MA, Hechter S, Webb GD, Williams WG. Surgery for partial atrioventricularseptal defect in the adult. Ann Thorac Surg. 1999; 67: 504–510 Therrien J, Warnes C, Daliento L, Hess J, Hoffmann A, Marelli A, Thilen U, Presbitero P, Perloff J, Somerville J, Webb GD. Canadian Cardiovascular Society Consensus Conference 2001 update: recommendations for the management of adults with congenital heart disease part III. Can J Cardiol. 2001; 17: 1135–1158. Gatzoulis MA, Freeman MA, Siu SC, Webb GD, Harris L. Atrial arrhythmia after surgical closure of atrial septal defects in adults. N Engl J Med. 1999; 340: 839–846. Fournier A, Young ML, Garcia OL, Tamer DF, Wolff GS. Electrophysiologic cardiac function before and after surgery in children with atrioventricular canal. Am J Cardiol. 1986; 57: 1137–1141. Egeblad H, Berning J, Efsen F, Wennevold A. Non-invasive diagnosis in clinically suspected atrial septal defect of secundum or sinus venosus type: value of combining chest x-ray, phonocardiography, and M-mode echocardiography. Br Heart J. 1980; 44: 317–321. Reading M. Chest x-ray quiz: an atrial septal defect. AustCrit Care. 2000; 13: 96–119. FUNDING None. COMPETING INTERESTS http://www.pacificejournals.com/awch