* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Chapter 20 - Low pH Productions
Plasmodium falciparum wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Onchocerciasis wikipedia , lookup
Sarcocystis wikipedia , lookup
Orthohantavirus wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Ebola virus disease wikipedia , lookup
Chagas disease wikipedia , lookup
Herpes simplex virus wikipedia , lookup
Trichinosis wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Oesophagostomum wikipedia , lookup
West Nile fever wikipedia , lookup
Henipavirus wikipedia , lookup
Marburg virus disease wikipedia , lookup
Sexually transmitted infection wikipedia , lookup
Neonatal infection wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Leptospirosis wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Lymphocytic choriomeningitis wikipedia , lookup
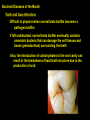
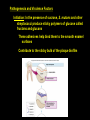
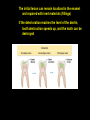
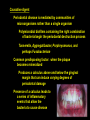
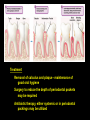
Chapter 20: Infectious Diseases Affecting the Gastrointestinal Tract Microbiology Fundamentals: A Clinical Approach. Marjorie Cowan, 1st ed. Part C Modified by JDB Bacterial Diseases of the Mouth Tooth and Gum Infections Difficult to pinpoint when normal biota biofilm becomes a pathogen biofilm If left undisturbed, normal biota biofilm eventually contains anaerobic bacteria that can damage the soft tissues and bones (periodontium) surrounding the teeth Also, the introduction of carbohydrates to the oral cavity can result in the breakdown of hard tooth structure due to the production of acid Bacteria live on the teeth as well as the soft structures of the mouth Numerous species live in large accretions known as dental plaque, a type of biofilm Bacteria held in the biofilm by specific recognition molecules Alpha-hemolytic streptococci are the first colonizers of the tooth surface after it has been cleaned Pellicle: mucinous glycoprotein covering on the tooth to which streptococci attach Other species attach specifically to proteins or sugars on the surface of streptococci Microscopic view of dental plaque, showing Gram-positive and Gramnegative bacteria. Dental Caries (Tooth Decay) (More) Most common infectious disease of human beings Involves the dissolution of solid tooth surface due to the metabolic action of bacteria Teeth are a hard surface and do not shed cells Allows for the accumulation of masses of microorganisms and their products – dental plaque (More) Oral bacteria convert sucrose and other carbohydrates into lactic acid that then erodes the tooth enamel Symptoms not noticeable, but range from: Minor disruption in the outer enamel surface of the tooth Complete destruction of enamel Destruction of deeper layers (Cavities) Deeper lesions can result in infection to the soft tissue inside the tooth called the pulp Infection leads to pain known as a “toothache” Causative agents: Over 700 species of bacteria have been isolated from the oral cavity Main cause - Streptococcus mutans S. mutans Oral, alpha-hemolytic streptococcus Likely caused by a mixed species consortium consisting of other Streptococcus species and some lactobacilli Early childhood caries may be caused by a newly discovered species Scardovia wiggsiae Pathogenesis and Virulence Factors Initiation: In the presence of sucrose, S. mutans and other streptococci produce sticky polymers of glucose called fructans and glucans These adhesives help bind them to the smooth enamel surfaces Contribute to the sticky bulk of the plaque biofilm Advanced decay: Lactobacillus spp are important in advancing the front of decay once it is established If plaque is not removed from sites that readily trap food, it can result in a carious lesion Streptococci, Lactobacillus and other bacteria produce acid as they ferment carbohydrates If acid is immediately flushed and the plaque is diluted in the mouth, it has little effect In denser regions of plaque, acid can accumulate in direct contact with enamel pH lowers to below 5 and calcium phosphate in the enamel can be dissolved The initial lesion can remain localized in the enamel and repaired with inert materials (fillings) If the deterioration reaches the level of the dentin, tooth destruction speeds up, and the tooth can be destroyed Transmission and Epidemiology Bacteria that cause dental caries are transmitted to babies and children by their close contacts Mother or closest caregiver Evidence for transfer of oral bacteria between children at day care centers Culture and Diagnosis Dental professionals diagnose caries based on the tooth condition Culture of the lesion is not routinely performed Prevention and Treatment The best way to prevent dental caries is through dietary restriction of sucrose and refined carbohydrates Regular brushing and flossing to remove plaque are also important Trace amounts of fluoride added to drinking water can incorporate into tooth structure and strengthen enamel Fluoride also encourages the remineralization of teeth that have begun the demineralization process Fluoride is also added to toothpastes and mouth rinses Treatment of a carious lesion Removal of the affected part of the tooth or whole tooth in advanced caries Restoration of the tooth structure with an artificial material Dental Caries Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Disease Table 20.4 Dental Caries Causative Organism(s) Streptococcus mutans, Scardovia wiggsiae, others Most Common Modes of Transmission Direct contact Virulence Factors Adhesion, acid production Culture/Diagnosis – Prevention Oral hygiene, fluoride supplementation Treatment Removal of diseased tooth material Periodontal Disease (More) 97% - 100% of the population has some manifestation by age 45 Most are due to bacterial colonization and varying degrees of inflammation Periodontitis (More) Initial stage is called gingivitis - swelling, loss of normal contour, patches of redness, and increased bleeding of the gingivae (gums), pockets or spaces develop between the tooth and gum If this condition persists, periodontitis develops: The natural extension of gingivitis into the periodontal membrane and cementum results in damage by an inflammatory response This increases the size of pockets between the tooth and the gingival and can cause bone resorption enough to loosen and possible lose the tooth Many different bacteria including members of Porphyromonas are found in these infections Causative Agent Periodontal disease is mediated by communities of microorganisms rather than a single organism Polymicrobial biofilms containing the right combination of bacteria begin the periodontal destruction process Tannerella, Aggregatibacter, Porphryomonas, and perhaps Fusobacterium Common predisposing factor: when the plaque becomes mineralized Produces a calculus above and below the gingival margin that can induce varying degrees of periodontal damage Presence of a calculus leads to a series of inflammatory events that allow the bacteria to cause disease Treatment Removal of calculus and plaque - maintenance of good oral hygiene Surgery to reduce the depth of periodontal pockets may be required Antibiotic therapy, either systemic or in periodontal packings may be utilized Acute Necrotizing Ulcerative Gingivitis (More) The most destructive periodontal diseases These diseases are synergistic infections involving Prevotella intermedia, Treponema vincentii, and Fusobacterium species Together they produce several invasive factors that cause rapid advancement into the periodontal tissues The condition is associated with severe pain, bleeding, pseudomembrane formation, and necrosis Periodontitis Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Disease Table 20.5 Periodontitis Disease Periodontitis Causative Organism(s) Polymicrobial community including some or all of Tannerella forsythia, Aggregatibacter actinomycetemcomitans, Porphyromonas gingivalis, others Most Common Modes of Transmission – Virulence Factors Induction of inflammation, enzymatic destruction of tissues Culture/ Diagnosis – Prevention Oral hygiene Treatment Removal of plaque and calculus, gum reconstruction, tetracycline, possibly anti-inflammatory treatments Mumps (More) – Paramyxovirus - Paramyxovirvividae A self-limited mildly epidemic illness associated with painful swelling at the angle of the jaw Incubation period of 2 to 3 weeks Signs and Symptoms Initial symptoms: fever, nasal discharge, muscle pain, and malaise May be followed by inflammation of the salivary glands, producing gopher-like swelling of the cheeks (parotitis) Multiplication in the salivary glands followed by invasion of other organs, especially testes, ovaries, thyroid gland, pancreas, meninges, heart, and kidneys Symptoms: cramping, nausea, vomiting, and diarrhea Toxin triggers brain vomiting reflex center Rapid recovery- usually within 24 hours Parotitis - Swelling of the parotid salivary gland Can cause considerable discomfort Viral multiplication in the salivary glands is followed by invasion of other organs Testes, ovaries, thyroid gland, pancreas, meninges, heart, and kidney Despite invasion of multiple organs, prognosis of most infections is complete, uncomplicated recovery with permanent immunity Complications in Mumps In 20 – 30% of young adult males, mumps infection localizes in the epididymis and testes, usually on one side only Orchitis and epididymitis can be painful No permanent damage usually occurs Transmission and Epidemiology of Mumps Virus Humans are exclusive natural hosts Communicated primarily through salivary and respiratory secretions Most cases occur in children under the age of 15, and most are subclinical Lasting immunity follows any form of mumps infection No long-term carrier reservoir exists in the population Prevention and Treatment Symptomatic treatment to relieve fever, dehydration, and pain Vaccine recommendations MMR at 12 and 15 months, booster at 4 – 6 years Healthcare workers and college students who haven’t had both doses are advised to do so Mumps Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Disease Table 20.6 Mumps Causative Organism(s) Mumps virus (genus Paramyxovirus) Most Common Modes of Transmission Droplet contact Virulence FactorsS Spike-induced syncytium formation Culture/Diagnosis Clinical, fluorescent Ag tests, ELISA for Ab Prevention MMR live attenuated vaccine Treatment Supportive Gastritis and Gastric Ulcers (More) - Helicobacter pylori Helicobacter pylori thrives in the acidic environment of the stomach and has been linked to a variety of gastrointestinal ailments Long-term infection with H. pylori might be a contributing factor to stomach cancer Gastritis: sharp or burning pain emanating from the abdomen Gastric ulcers (AKA peptic ulcer) are actual lesions in the mucosa of the stomach Duodenal ulcer: lesion in uppermost portion of the small intestine Signs and Symptoms Severe ulcers can be accompanied by bloody stools, vomiting Symptoms are often worse at night, after eating, or under conditions of psychological stress Benign Gastric Ulcer Causative Agent Helicobacter pylori - Gram-negative, microaerophilic, curved rods Closely related to Campylobacter Pathogenesis and Virulence Factors H. pylori bores through the outermost mucus layer that lines the stomach epithelium to avoid low pH of stomach Attaches to specific binding sites on the cells and entrenches itself Produces large amounts of urease – converts urea to ammonia – creates local high pH in the area of growth Dozens of the curved bacteria fill the lumen of a gastric foveola (pit). Ammonia and other products (proteases) are toxic to the epithelial cells Before the bacterium was discovered, spicy food, high-sugar diets, and psychological stress were considered to be the causes of gastritis age These factors merely aggravate the underlying infection Transmission and Epidemiology a Mode of transmission remains a mystery Studies have revealed that the pathogen is present in a large portion of the population Occurs in the stomachs of 25% of healthy, middle-aged adults and 60% of adults over 60 years of age H. pylori is probably transmitted from person to person by the oral-oral or fecal-oral route Seems to be acquired early in life and carried asymptomatically until its activities begin to damage the digestive mucosa Other animals are susceptible to H. pylori and develop gastric ulcers It has been proposed that it is a zoonosis transmitted from an animal reservoir Bacterium also found in water sources Prevention and Treatment The only preventative approaches currently are those that diminish some of the aggravating factors Over-the counter remedies offer symptom relief Most of them neutralize stomach acid Best treatment is a course of antibiotics augmented by acid suppressors Gastritis and Gastric Ulcers Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Disease Table 20.7 Gastritis and Gastric Ulcers Causative Organism(s) Helicobacter pylori Most Common Modes of Transmission ? Virulence Factors Adhesins, urease Culture/Diagnosis Endoscopy, urea breath test, stool antigen test Prevention None Treatment Antibiotics plus acid suppressors (clarithromycin or metronidazole plus omeprazole or bismuth subsalicylate) Hepatitis (More) Inflammatory disease marked by necrosis of hepatocytes and a mononuclear response that swells and disrupts the liver architecture Pathologic changes interfere with the liver’s excretion of bile pigments such as bilirubin into the intestine May result from autoimmune disease, drug, alcohol, or chemical toxicity, EB virus, CMV, or the hepatitis viruses A - E Causes jaundice when bilirubin accumulates in the blood and tissues Hepatitis A (HAV) and Hepatitis E Virus (HEV) (More) Viruses are considered together because: In general, far milder and self-limiting hepatitis than the other forms Single-stranded, nonenveloped ssRNA viruses Transmitted through the fecal-oral route HAV – Picornaviridae - Picornavirus HEV infects pregnant women - disease is more often severe and is associated with a clinical syndrome called fulminant hepatic failure – 15 - 25% mortality HEV - Hepeviridae Hepevirus Signs and Symptoms Subclinical or accompanied by vague, flulike symptoms malaise, anorexia, abdominal pain, arthralgia, and fever Overt cases Jaundice Swollen liver Darkened urine often seen Viruses are not oncogenic In most everyone besides pregnant women, complete, uncomplicated recovery results Transmission and Epidemiology Associated with deficient personal hygiene and lack of public health measures In countries with inadequate sewage control, outbreaks are associated with fecally contaminated water and food Most infections result from Unhygienic food handling Eating shellfish Sexual transmission Travel to other countries Hepatitis A can occasionally be spread by blood or blood products Exception rather than the rule In developing countries, children are the most common victims because exposure occurs early in life The virus is not carried chronically Principal reservoirs are asymptomatic, short-term carriers (often children) or people with clinical disease Prevention and Treatment Prevention of hepatitis A is based primarily on immunization Inactivated viral vaccine (Havrix) has been in use since the 1990s Administration after exposure can prevent symptoms Short-term protection can be conferred by passive immune globulin Useful for people who have come into contact with HAV-infected people Also used when people have eaten at a restaurant that was the source of a recent outbreak Combined hepatitis A/hepatitis B vaccine (Twinrix) Recommended for people with chronic liver dysfunction, intravenous drug users, anyone engaging in anal-oral intercourse Travelers to areas with high rates of both diseases should obtain vaccine coverage No specific medicine is available for hepatitis A or hepatitis E Drinking lots of fluids and avoiding liver irritants such as aspirin or alcohol will speed recovery Hepatitis B Virus (HBV) (More) - Hepadnaviridae Enveloped DNA virus - genome is partly double-stranded and partly single-stranded Intact viruses are called Dane particles Surface (S) antigen is an antigen of clinical and immunologic significance Signs and Symptoms Direct damage to liver cells Fever, chills, malaise, anorexia, abdominal discomfort, diarrhea, and nausea Rashes may appear and arthritis may occur HBV infection can be serious, even life-threatening A small number of patients develop glomerulonephritis and arterial inflammation Complete liver regeneration and restored function occur in most patients A small number of patients develop chronic liver disease in the form of cirrhosis or necrosis In some cases, chronic HBV infection can lead to liver cancer Patients who become infected as children have significantly higher risks of long-term infection and disease 90% of neonates infected at birth develop chronic infection 30% of children infected between ages 1 and 5 also develop chronic infection Only 6% of persons infected after age 5 develop chronic infection This finding is one of the justifications of routine vaccination of children Pathogenesis and Virulence Factors Hepatitis B virus enters the body through a break in the skin, mucous membrane, or by injection into the bloodstream Eventually reaches liver cells (hepatocytes) where it multiplies and releases viruses into the blood Incubation period 4 – 24 weeks (7 weeks average) The majority of those infected exhibit few overt symptoms and eventually develop an immunity to HBV Multiplies exclusively in the liver and continuously seeds the blood with viruses Electron microscopy studies have shown up to 107 virions per milliliter of infected blood Even a minute amount of blood can transmit infection Simple practices such as sharing a toothbrush or a razor can transmit the infection HBV has been detected in semen and vaginal secretions, and can be transmitted by these Cirrhosis Virus is spread by close contact in families or institutions Vertical transmission is possible Predisposes the child to development of the carrier state and increased risk of liver cancer Also known as serum hepatitis One of the major infectious concerns for healthcare workers Needlesticks can easily transmit the virus Healthcare workers are required to have the full HBV vaccination series HBV remains infective for days in dried blood, for months when stored in serum at room temperature, and for decades when frozen HVB Not inactivated after 4 hours of exposure to 60°C Boiling for the same time period can destroy it Disinfectants containing chlorine, iodine, and glutaraldehyde show potent anti-hepatitis B activity Prevention and Treatment Primary prevention for HBV is vaccination Vaccination is a must for medical and dental workers and students, patients receiving multiple transfusions, immunodeficient patients, and cancer patients Vaccine now strongly recommended for newborns as part of a routine immunization schedule Passive immunization with hepatitis B immune globulin (HBIG) Gives significant immediate protection to people who have been exposed to the virus through needle puncture, broken blood containers, or skin or mucosal contact with blood Also recommended for neonates born to infected mothers Mild cases of HBV are managed with symptomatic treatment and supportive care care Chronic HBV infection can be controlled with recombinant human interferon and other drugs All of these can help stop virus multiplication in many but not all patients None of the drugs are considered curative Hepatitis D Virus (HDV) (More) - Deltavirus Hepatitis D virus considered to be a subviral satellite because it can propagate only in the presence of HBV (cannot produce infection on it’s own) Transmission of HDV can occur either via simultaneous infection with HBV (coinfection) or via infection of an individual previously infected with HBV (superinfection)) Results in more severe complications compared to infection with HBV alone A greater likelihood of experiencing liver failure in acute infections and a rapid progression to liver cirrhosis Increased chance of developing liver cancer in chronic infections 20% mortality rate (highest of the Hepatitis viruses) Transmission: Parenteral (intravenous drug use) Hepatitis C Virus (HCV) (More) - Flaviviridae ssRNA virus “silent epidemic” – one of the most common reasons for liver transplants 4 million Americans are infected with the virus Takes many years to cause noticeable symptoms Signs and Symptoms People have widely varying experiences with this infection Shares many characteristics with HBV More likely to become chronic Of those infected, 75 – 80% will remain infected indefinitely Possible to have severe infections without permanent liver damage More common to have chronic liver disease even without overt symptoms Cancer may result from chronic HCV infection Worldwide, HBV infection is the most common cause of liver cancer In the U.S., liver cancer is more likely caused by HCV Metastatic Hepatic Carcinoma Transmission and Epidemiology Virus is acquired in ways similar to HBV More commonly transmitted through blood contact Blood transfusions Injecting drug users Vertical transfer is also possible Frequently transmitted through blood transfusions before a blood test was available Frequently transmitted through blood transfusions before a blood test was available Hemophiliacs who were treated with clotting factor before 1985 were infected with HCV at a high rate Once blood began to be tested for HIV and screened for “non-A, non-B” hepatitis, the risk of contracting HCV was reduced Prevention and Treatment Currently no vaccine for hepatitis C Current treatment regimens are not curative, but prevent or lessen damage to the liver Hepatitis Copyright © The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Disease Table 20.8 Hepatitis Causative Organism(s) Hepatitis A or E virus Hepatitis B virus Hepatitis C virus Most Common Modes of Transmission Fecal-oral, vehicle Parenteral (blood contact), direct contact (especially sexual), vertical Parenteral (blood contact), vertical Virulence Factors – Latency Core protein suppresses immune function Culture/Diagnosis IgM serology Serology (ELISA, radioimmunoassay) Serology Prevention Hepatitis A vaccine or combined HAV/HBV vaccine HBV recombinant vaccine – Treatment Hep A: hepatitis A vaccine or immune globulin; hep E: immune globulin Interferon, nucleoside analogs (Pegylated) interferon, with or without ribavirin Incubation Period 2–7 weeks 1–6 months 2–8 weeks