* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Analysis of Heart Rate Variability and Clinical Implications
Saturated fat and cardiovascular disease wikipedia , lookup
Heart failure wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Electrocardiography wikipedia , lookup
Cardiac surgery wikipedia , lookup
Coronary artery disease wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
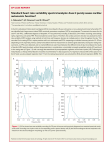
Analysis of Heart Rate Variability and Clinical Implications Analysis of Heart Rate Variability and Clinical Implications Meldijana Omerbegovic Clinic for Anesthesia and Reanimation, Clinical Center of University of Sarajevo, Bosnia and Herzegovina PROFESSIONAL PAPER Summary In the last decades analysis of heart rate variability has emerged as a new useful tool for assessing the changes in autonomic tone that influences cardiovascular function. High variability of oscillations and the integrated physiologic activities of heart and cardiovascular system is associated with physiologic functioning. Irregularity of the length of consecutive heart cycles, designated as heart rate variability, reflects the ability of cardiovascular system to adapt to different situations in everyday life. Reduction of these fluctuations of the heart periods has been shown to be associated with pathological conditions in many experimental and clinical trials. The extent and consistency of the reduction of heart rate variability in the patients after acute coronary events, were shown to be related to mortality and cardiovascular dysfunction. In patients with diabetes mellitus who develop autonomic neuropathy, reduced heart rate variability is quite common. Reduced heart rate variability was shown in endocrine disorders, neurological and psychiatric diseases, with use of different drugs and many other conditions. The most common ways of measuring heart rate variability are measuring in time domain analysis and frequency domain analysis. Parameters calculated from the measurements are related to the functions of sympathetic and parasympathetic nervous system. Measurements of changes in autonomic function is very important in the follow up in different diseases and for determination of the efficacy of the therapy. In the field of surgery and anaesthesia, besides preoperative risk stratification, there are many studies on the effects of different anaesthetics on heart rate variability. In this paper, some aspects of measurement of heart rate variability and changes of the values of parameters in different pathological conditions and clinical implications are reviewed. Key words : heart rate variability, noninvasive monitoring, autonomic nervous system, autonomic imbalance 1. INTRODUCTION Continuos electrocardiographic monitoring of heart rate in the perioperative period, in the setting of intensive care unit and during labour and some diagnostic procedures, is considered as a basic standard care. The scope of this paper is limited to description of the recently recognized parameters derived from analysis of different duration of the intervals between consecutive heart contractions, which is named heart rate variability (HRV) and clinical implications (1). Inherent automaticity of the depolarization of specialized cells in sino-atrial node determines heart rate, but it is the complex interplay of autonomic sympathetic and vagal parasympathetic activity that modulates frequency of the sinoatrial node depolarization . Vagal stimulation produce hyperpolarization of the cardiac pacemaker cells and reduced rate of depolarisation, on the contrary sympathetic stimulation causes increasing of rate of depolarization (2). With every beat of the heart, information about the state of the circulation, are sent to the neurons within the medulla oblongata and processed in the milieu of integrative modulating influences from hypothalamus and higher centers. Efferent signals are sent to output regions of 102 the central nervous system and ensure maintenance of the functioning of the cardiovascular system at the most appropriate level. Sympathetic preganglionic neurones give major contribution in the control of heart rate and blood pressure at the level of spinal cord. Figure 1 represents simplified scheme of the neural components that influence heart activity . Interactions between sympathetic and parasympathetic efferent projections involve different modulation of adenylate cyclase via G-protein-coupled receptor systems. Catecholamines, released from sympathetic efferent projections or from circulation, influence myocardial tissue by binding to β1 and β2 adrenoreceptors,which are coupled to and stimulate adenylate cyclase via stimulatory guanine nucleotide-binding protein(Gs). Acetylcholine, released from parasympathetic efferent postganglionic neurons, binds to cardiomyocyte M2 muscarinic receptors, which inhibit adenylate cyclase via inhibitory guanine nucleotide-binding protein (Gi). Interactions between these two receptor-coupled systems at the adenylate cyclase level determine the formation of cAMP and influence the function of second messengers in myocyte and subsequently modulate the cell functions (2). Complex neuronal, reflex and local Med Arh 2009;63(2) • Stručni članci | Professional papers control of the frequency of heart rate is manifested in different length of cardiac cycle in physiological and it is quite changed in pathological conditions. Acceleration of heart rate is a result of increase in sympathetic activity or decrease in vagal activity with shortening of cardiac cycles and most effect on diastole duration , while bradycardia is a result of predominant parasympathetic activation. The clinical importance of HRV was recognized by Hon and Lee, who observed that fetal distress was associated with significant changes in HRV before any change in heart rate itself (3). An important observation was made by Wolf et al. in 1977 , who found that a reduced HRV was related to a higher risk of post-infarction mortality. About ten years later Kleiger et al. published a paper on the results of the Multi-Center Post-Infarction Project (MPIP) , what started a more serious interest in HRV among cardiologists (4). Since then a lot of studies have been performed on the issue of low measures of HRV which have been linked with different diseases and conditions . In 1996 Task force of the European Society of Cardiology and the North American Society of Pacing and Electrophysiology developed standards of measurements and physiological correlates of HRV and clinical applications. According to the guidelines measurement of heart rate variability (HRV) may provide quantitative information on the modulation of cardiac sympathetic and parasympathetic nerve activities. The two main applications that could be clinically useful are the risk stratification after myocardial infarction and the assessment of diabetic neuropathy (5). Impaired autonomic nervous activity has been recognized as an important symptom and is strongly associated with an increased risk of overall mortality in patients with heart disease. 2. MEASUREMENT OF HRV The most commonly used methods of HRV analysis can be categorised into four groups: time domain measures, frequency domain measures, rhythm analysis and non-linear methods (3). Two main methods that are used for evaluation of HRV in clinical practice are time domain methods and frequency domain methods. 2.1. Time Domain Method QRS detection is necessary for the Analysis of Heart Rate Variability and Clinical Implications HIGHER CENTERS ARTERIAL BARORECEPTORS NODOSE AFF. SOMA MEDULA DRG AFF.SOMA SPINAL CORD LCN Afferent soma S E soma CIRCULATING CATECHOLAMINS ANGIOTENSIN II EXTRACARDIAC INTRATHORACIC GANGLIA LCN SE soma neurit neurit PE soma M2 B1 Gs Gi Afferent soma INTRINSIC CARDIAC GANGLIONATED PLEXUS neurit HEART AC ATP cAMP Figure 1. Schematic representation of neural components that influence heart activity. Intrinsic cardiac ganglia comprisesympathetic (SE) and parasympathetic (PE) efferent neurons, local circuit neurons (LCN), and afferent neurons. Extracardiac intrathoracic ganglia include sympathetic efferent neurons, local circuit neurons, and afferent neurons. Aff.-afferent; DRG- dorsal root ganglia; Gs-stimulatory guanine nucleotide-binding protein; Gi-inhibitory guanine nucleotide-binding protein; AC-adenylate cyclase; B1- β1-adrenergic receptor; M2-muscarinic receptor.(Modified from Ardell J.L. Neurohumoral Control of Cardiac Function , ref.2 ) determination of the periods between adjacent QRS complexes which are named the N-N (normal-normal) intervals (9). The simplest calculated measures are: the mean interval length (meanNN) and the standard deviation (SDNN). SDANN is the standard deviation of intervals averaged over 5min sections. The parameter pNN50 is the proportion of interval differences of less than 50 ms. It is a marker for vagal activity. Geometrical measures are based on the density distribution of NN intervals. The shape of the histogram can be approximated by a geometrical shape, such as a triangle, and a measure of that shape can be used in further assessment (5). Different calculated variables of time domain measures are used for analysis of HRV and they are listed in the Table 1. 2.2. Frequency Domain Method In the spectral analysis of the tachogram, ECG signal is differentiated into the frequencies using a mathematical algorithm (fast Fourier transformation) ,that can be represented on a graph, and area under the curve is designated as a spectral power (5). The frequency domain is divided into bands, which isolate typical peaks, as shown in Figure 2. For short-term recordings, the high band (HF) is in range between 0.15 Hz and 0.4 Hz, the low band (LF) from 0.04 Hz to 0.15 Hz and the very low band (VLF) of frequencies below 0.04 Hz. The measurement of VLF, LF and HF power components is mostly in absolute values of power (milliseconds squared–msec2 ). Frequency domain methods are appropriate for analysis of short-term recordings and time domain methods are ideal for the analysis of long-term recordings. Several frequency domain measures are listed in the Table 2. 3. PHYSIOLOGICAL CHANGES OF HRV PARAMETERS In the complex interaction of parasympathic and sympathetic influences, under resting conditions parasympathetic tone exceeds sympathetic effects in healthy subjects. The efferent vagal activity is a major contributor to the HF component. Sympathetic activation is related to spectral power in the LF band, but it can also be influenced by vagal activation (5). The sympatho-vagal balance is expressed in the relation of LF/HF. Spectral analysis of 24-h recordings shows in normal subjects a circadian pattern with higher values of LF in the daytime and higher HF at night. An increase in LF is observed during 90◦ tilt, standing, mental stress, and moderate exercise in healthy subjects (6). Increased LF power and decreased HF power, reflect the normal response to upright tilt movement (5). Increase in HF components is induced by controlled respiration, cold stimulation of the face and rotational stimuli (7). 4. CHANGES OF HRV PARAMETERS IN DISEASE variations of RR intervals and LF and HF components are also present (8). In the days after the infarction there is a depression in the time and frequency domain parameters of HRV with predominance of sympathetic components. In the later period, after weeks and months, the HRV could be partially recovered (5). The aim of risk stratification is to identify the patients with a high risk of post-infarct mortality.These patients could have benefit from further treatment, as it was shown in a clinical trial by Moss and coworkers (9). On the contrary to their findings, the investigators of DINAMIT trial did not show beneficial effects of implantable cardiac defibrillator in patients with high risk after acute myocardial infarction (10). The HRV is independent from other predictors, like depressed left ventricular ejection fraction, increased ventricular ectopic activity. There is a general consensus that HRV should be measured a week after myocardial infarction, as a high proportion of complications may occur in that period (5). Some recent studies did not show strong predictive power of HRV in risk stratification after myocardial infarction, what could be explained with the use of thrombolysis, early revascularisation and medications like beta blockers and inhibitors of angiotensinconverting enzyme (11). It was also shown that HRV could be an independent prognostic factor in patients with stable angina (12). Data from meta-analyses indicated that within the initial two years after myocardial infarction, patients with lower HRV demonstrated great increase in major arrhythmic events like ventricular fibrillation, ventricular tachycardia or sudden cardiac death (13). There have been many clinical multicenter trials on the possible beneficial effects of risk stratification , after myo- 4.1. Cardiovascular diseases Numerous experimental and clinical studies have shown significant relationship between the autonomic nervous system disorders and cardiovascular diseases. In the first hours after the myocardial infarction there is a significant reduction of SDNN. The Variable Units Description vagal stimulation STATISTICAL MEASURES is decreased and SDNN ms Standard deviation of all NN intervals sympathetic in- SDANN Standard deviation of the averages of NN intervals in all 5-minute segments of ms the recording fluences predomSDSD ms Standard deviation of differences between adjacent NN intervals inate. The shift Percent of difference between adjacent NN intervals that are greater than 50 % in sympatho-va- pNN50 ms gal balance is ex- GEOMETRIC MEASURES Total number of all NN intervals divided by the height of the histogram of all NN pressed in a pre- HRV triangular index intervals measured on a discrete scale dominant LF and a Baseline width of the minimum square difference triangular interpolation of the ms highest peak of the histogram of all NN intervals reduced HF , with TINN high LF/HF ratio. Table 1. Selected Time Domain Measures of HRV (5) Reduced circadian Med Arh 2009;63(2) • Stručni članci | Professional papers 103 Analysis of Heart Rate Variability and Clinical Implications tricular ejection fraction of more than 40% and depressed HRV could benefit from prophylactic antiarrhythmic treatment with amiodarone, but the need for further studies in an independent data set before further recommendations was emphasized (17). The population of patients with chronic heart failure is growing and there is evidence that autonomic nervous imbalance plays important role in the progression of the disease. In the Figure 2. Power spectral density of the healthy subject during rest (5) initial stages of disease increases of LF and a decrease of HF are detected. In the cardial infarction. Bigger et al. analysed advanced stages of heart failure both LF HRV spectral parameters from ECG re- and HF bands are decreased (18). cordings in 715 participants in the Mul4.2. Respiratory Diseases ticenter Post Infarction Program (MPIP) Obstructive sleep apnea syndrome is during the period of four years and found characterized by repetitive episodes of strong association between mortality upper airway collapse during sleep. The and total, ULF, and VLF power. They obstruction of the airway produces vigorous efforts to breathe, leading Variable Units Description Frequency range to transient arousal and restoraTotal power ms² Variance of all NN intervals =< 0,4 Hz tion of the pattency of the upULF ms² Power in ULF range < 0,003 Hz per airway. Many data support VLF ms² Power in VLF range 0,003-0,04 Hz the hypothesis that long-term LF ms² Power in LF range 0,04 -.0,15 Hz exposure to episodic apnea and HF ms² Power in HF range 0,15 – 0,4 Hz arousal constitutes an indepenTable 2. Selected Frequency Domain Measures of HRV (5) dent risk factor for systemic hypertension, heart failure, myofound that adding measures of heart pecardial infarction, and stroke (19). Sevriod variability to previously known preeral studies have shown the usefulness dictors of risk after myocardial infarcof measuring HRV as a powerful tool for tion could identify small subgroups with obstructive sleep apnea syndrome diagtwo and a half year mortality risk of apnosis and follow up of therapeutic proceproximately 50% (14). dures (19). In patients with mild chronic In the prospective study Autonomic obstructive pulmonary disease, cardiac Tone and Reflexes After Myocardial Indisorders are the leading causes of hosfarction (ATRAMI), in which 55% of pitalization, accounting for 42 to 48% of deaths were sudden, it was shown that all hospitalizations. Monitoring of HRV within the group of patients after myochanges in the patients with COPD have cardial infarction who had a depressed been shown as a possible marker of carleft ventricular ejection fraction, an indiac comorbidities (20). creased risk of death was associated with 4.3. Endocrine diseases the presence of autonomic imbalance Cardiovascular autonomic neurop(15). In the trial named AzimiLide Postathy is one of the most common and Infarct SurVival Evaluation (ALIVE) a most investigated complications in panovel class III antiarrhythmic drug, aztients with diabetes mellitus. The earliimilide, was investigated for its effects est sign , that can be detected in asympon mortality in patients after myocartomatic patients is a depression of heart dial infarction, and results showed that rate variability. Primary damage is of azimilide did not improve or worsen the branches of vagus nerve, with resulthe mortality of patients after myocartant resting tachycardia. After latency dial infarction, while low HRV indepenof some years, damage of sympathetic dently identified a subpopulation at high nerve fibers changes the sympathovarisk of mortality, what is presented in the gal balance, but tachycardia remains. Fig. 3 (16). In the European Myocardial Later symptoms such as exercise intolInfarct Amiodarone Trial (EMIAT) it erance, orthostatic hypotension and furwas investigated if the patients with dether decrease of HRV are the manifespressed heart rate variability could have tations of progressive damage to the aubenefit from amiodarone treatment. Retonomic balance (21). Investigations of sults showed that patients with left venHRV in patients with hyperthyroidism 104 Med Arh 2009;63(2) • Stručni članci | Professional papers have suggested that thyroid hormone excess may reduce parasympathetic activity (22). Patients with clinical hypothyroidism have a sympatho-vagal imbalance, and the changes of repolarization times may predispose to the potentially life-threatening arrhythmias. The assessment of HRV in patients with clinical hypothyroidism may be a useful tool in monitoring of the cardiovascular complications (23). 4.4. Renal diseases Autonomic nervous system dysfunction is a prominent characteristic of the uremic state and analysis of HRV has demonstrated striking changes of cardiac autonomic nervous system in patients with chronic renal failure. It has also been associated with sudden death in patients undergoing hemodialysis, especially in those with coronary stenosis and nocturnal myocardial ischemia (24). 4.5. Psychiatric diseases Depression has significant adverse effects on the course and outcome of coronary heart disease and it has been suggested to be associated with about a three fold increase in cardiac mortality (25). Physiological studies have demonstrated compromised modulation of the sympathetic and parasympathetic nervous system in psychosis. The fact that many antipsychotics could have potentially dangerous cardiac side effects led to investigations with atypical antipsyhotics, which have been demonstrated to have beneficial side effects profile (26). Power spectrum analysis demonstrated significant reduction of HRV, vagal tone activity and augmented sympathetic activity in the patients with posttraumatic stress disorder (PTSD) who had no medications in comparison to healthy subjects. Significant autonomic dysregulation of patients with PTSD at rest, could be corrected with administration of selective serotonin reuptake inhibitors (27). 5. CHANGES OF HRV PARAMETERS UNDER MEDICATION Heart rate variability could be significantly changed by different groups of drugs, and it could also be used as a parameter to quantify the effects of the drugs in some diseases. Beta-blockers, calcium channel blockers and different antiarrhythmics have been studied in the patients with CVS diseases (16,17). Beta- adrenergic blockers prevent Analysis of Heart Rate Variability and Clinical Implications toring of sympatho-vagal balance during induction and maintaining of anesthesia are in focus of many current trials of HRV in perioperative period (33). 7. CONCLUSION Heart rate variability reflects the response of the heart to a variety of influences. Substantial reFigure 3. Kaplan-Meier curve of all-cause mortality in placebo patients in ductions of HRV are seen in the high risk group (HRV< 20U) and low risk group (HRV>20U). (From Camm AJ et al. Mortality in Patients After a Recent Myocardial Infarction, ref.16 ) setting after acute cardiac events, like acute myocardial infarction, the rise in the LF component observed and it was shown as an indepenin the morning hours. Carvedilol ther- dent predictive factor of mortality in apy in patients with chronic heart fail- the patients after acute coronary event. ure significantly increased HRV with Reduced HRV is an early finding in pabeneficial effects on hemodynamics (28). tients with cardiac diabetic autonomic The trials with antihypertensive agents neuropathy before development of clinihave shown better effects of angiotensin cal symptoms. In many other endocrine II receptors antagonists in regard to an- disorders, neurological and psychiatric gitensin converting enzyme inhibitors diseases, monitoring of changes in HRV (29). Among other medications, antiep- enables following of the effects of therileptics are known to impair cardiac au- apy and the state of the disease. Perioperative period is another imtonomic function, and it is known that carbamazepine increases sympathetic portant issue, as monitoring of preopand parasympathetic tone, which could erative HRV could be of great imporbe very important in the overall mor- tance for the risk stratification of the bidity and mortality (30,31). Most anti- patients with cardiovascular diseases psychotic drugs have cardiac effects as and predicting possible complications. a consequence of their pharmacological Large prospective and standardized triactions, and it was shown that HRV was als could give more information on relereduced. Studies with olanzapine and vance of this noninvasive monitoring of amilsupride also showed that amilsu- autonomic nervous system function in pride had a more vagotonic effect, sug- the perioperative period. Development gesting greater cardiovascular safety in of the technique of monitoring, analycomparison to olanzapine (32). sis and standardization of procedures of measurement of the heart rate variability 6. HRV CHANGES IN (HRV) could give a useful tool in evalPERIOPERATIVE PERIOD uating of autonomic changes and autoGeneral anaesthesia and surgery pro- nomic imbalances in the specific disease duce significant changes in autonomic states and perioperative period. nervous system function. Most studies that investigated the effects of different References 1. Omerbegovic M. Heart Rate Variability - Noninvasive Moanaesthetics were performed during innitoring of Autonomic Nervous System Function. AIM, 2009; vol 17(1): 53-8. duction of anaesthesia, with findings 2. Ardell J.L. Neurohumoral Control of Cardiac Function.In Sperelakis N, Kurachi Y,Terzic A,Cohen M.eds.: Heart Physiothat all most common used induction logy and Pathophysiology. Fourth Edition.New York. Academic Press. 2001; pp 45-59. agents reduce total HRV, with different 3. Barbieri R, Matten F.C, Alabi A.R, Brown E.N. A point-proeffects on sympathetic and parasympacess model of human heartbeat intervals: new definitions of heart rate and heart rate variability. Am J Physiol Heart Circ thetic related components.Clinical triPhysiol .2005; 288: H424–H435, 2005. RE, Miller JP, Bigger JT , Moss AJ. Decreased Heals with inhalational agents have shown 4. Kleiger art Rate Variability and its association with increased mortality after acute myocardial infarction. Am J Carreductions in total power of HRV. Most diol.1987;59:256-62. trials revealed that all anaesthetic agents 5. Task Force of The European Society of Cardiolgy and the North American Society of Pacing and Electrophysiology. produced significant changes of heart Heart rate variability: standards of measurement, physiogical interpretation and clinical use. Circulation.1996; 93: 1043-65. rate variability, but further large studies 6. Lucini D, Norbiato G, Clerici M, Pagani M. Hemodynamic and autonomic adjustments to real life stress conditions in are required for getting more informahumans. Hypertension.2002; 39: 184–188. tion and evidence on the effects of differ- 7. Ducla-Soares J.L, M. Santos-Bento M, Laranjo S, Andrade A .Wavelet analysis of autonomic outflow of normal subjects on ent anaesthetic agents in perioperative head-up tilt, cold pressor test, Valsalva manoeuvre and deep breathing.Exp Physiol,2007; 92(4):677- 686. period and in different patients popula- 8. Balanescu S, Corlan AD, Dorobantu M, Gherasim L. Prognostic value of heart rate variability after acute myocardial intions (1). Very important issues of risk farction. Med Sci Monit, 2004; 10: 307–315. stratification before surgery and moni- 9. Moss AJ, Zareba W, Hall WJ, Klein H, Wilber DJ, Cannom DS 10. 11. 12. 13. 14. 15. 16. 17. 18. 19. 20. 21. 22. 23. 24. 25. 26. 27. 28. 29. 30. 31. 32. 33. et al. Prophylactic implantation of a defibrillator in patients with a myocardial infarctionand reduced ejection fraction. N Engl J Med.2002;346:877-83. Hohnloser SH, Kuck KH, Dorian P, Roberts RS. DINAMIT Investigators. Prophylactic use of an implantable cardioverter-defibrillator after acute myocardial infarction. N Engl J Med. 2004 ;351(24):2481-8. Huikuri HV,Tapanainen JM,Lindgren K,Raatikainen P, Makikallio TH, Airaksinen KEJ, et al. Prediction of sudden cardiac death after myocardial infarctionin the beta-blocking era. J Am Coll Cardiol .2003;42 :652-8. Lanza GA, Cianflone D, Rebuzzi AG, Angeloni G, Sestito A, Ciriello G, et al. Prognostic value of ventricular arrhythmias and heart rate variability in patients with unstable angina. Heart. 2006 Aug; 92(8):1055-63. Bailey JJ, Berson AS, Handelsman H, Hodges M. Utility of current risk stratification tests for predicting major arrhythmic events after myocardial infarction. J Am Coll Cardiol 2001;38:1902-1911. Bigger JT, Fleiss JL, Rolnitzky LM,Steinman RC. The ability of several short-term measures of RR variability to predict mortality after myocardial infarction .Circulation. 1993;88:927-934 La Rovere MT, Bigger JT Jr, Marcus FI, et al, for the ATRAMI (Autonomic) Camm AJ,Pratt CM ,Schwartz PJ, Al-Khalidi HR, Spyt MJ, Holroyde MJ, Karam R. Mortality in Patients After a Recent Myocardial Infarction- A Randomized, Placebo-Controlled Trial of Azimilide Using Heart Rate Variability for Risk Stratification. Circulation, 2004;109:990-996. Malik M, Camm AJ, Janse MJ, MD, Julian DG, Frangin GA, Schwartz PJ. Depressed Heart Rate Variability Identifies Postinfarction Patients Who Might Benefit From Prophylactic Treatment With Amiodarone .J Am Coll Cardiol, 2000;35:1263–75. Van de Borne P, Montno N, Pagani M, Oren R, Somers VK. Absence of low-frequency variability of sympathetic nerve activity in severe heart failure. Circulation, 1997; 95 :1449-54. Jo JA, Blasi A, Valladares E, Juarez R, Baydur A, Khoo MC. Determinants of heart rate variability in obstructive sleep apnea syndrome during wakefulness and sleep. Am J Physiol Heart Circ Physiol, 2005 Mar;288(3):H1103-12. Tükek T, Yildiz P, Atilgan D, Tuzcu V, Eren M, Erk O, Demirel S, Akkaya V, Dilmener M, Korkut F. Effect of diurnal variability of heart rate on development of arrhythmia in patients with chronic obstructive pulmonary disease. Int J Cardiol, 2003 Apr;88 (2-3):199-206. Urbancic-Rovan V, Meglic B, Stefanovska A, Bernjak A, Azman-Juvan K, Kocijancic A. Incipient cardiovascular autonomic imbalance revealed by wavelet analysis of heart rate variability in Type 2 diabetic patients.Diabet Med, 2007 Jan;24(1):18-26. Chen JL, Chiu HW, Tseng YJ, Chu WC. Hyperthyroidism is characterized by both increased symphatetic and decreased vagal modulation of heart rate: evidence from spectral analysis of heart rate variability. Clinical Endocrinology. 2006;64(6):611-6. Galetta F, Franzoni F, Fallahi P, Tocchini L, Braccini L, Santoro G et al. Changes in heart rate variability and QT dispersion in patients with overt hypothyroidism. Europ J Endocrinol, 2008; 158 : 85–90. Cashion AK, Holmes SL, Acchiardo SR, Hathaway DK, Arheart KL. Heart rate variability and mortality in patients with end stage renal disease. Nephrology Nursing Journal. 2005;32(2)173-84. Grace SL, Abbey SE, Kapral MK, Fang J, Nolan RP, Stewart DE. Effect of depression on five-year mortality after an acute coronary syndrome. Am J Cardiol, 2005;96(9):1179-1185. Agelink MW, Majewski T,Wurthmann C,Lukas K,Ullrich H ,Linka T,Klieser E.Effects of newer atypical antipsychotics on autonomic neurocardiac function: A comparison between am ilsupride,olanzapine,sertindole and clozapine.J Clin Psyhopharmacol, 2001;21:8-13. Cohen H, Kotler M, Matar M, Kaplan Z. Normalization of heart rate variability in post-traumatic stress disorder patients following fluoxetine treatment: preliminary results. Isr Med Assoc J, 2000 Apr; 2(4):296-301. Chiu KM, Chan HL, Chu SH, Lin TY. Carvedilol can restore the multifractal properties of heart beat dynamics in patients with advanced congestive heart failure. Autonomic Neuroscience: Basic & Clinical. 2007:132(1/2):76-80. Lewandowski J, Abramczyk P, Dobosiewicz A, Bidiuk J, Sinski M, Gaciong Z. The effect of enalapril and telmisartan on clinical and biochemical indices of sympathetic activity in hypertensive patients. Clinical & Experimental Hypertension. 2008;30(5):423-32. Lossius MI, Erikssen JE, Mowinckel P, Gulbrandsen P, Gjerstad L. Changes in autonomic cardiac control in patients with epilepsy after discontinuation of antiepileptic drugs: a randomized controlled withdrawal study. European Journal of Neurology. 2007;14(9):1022-8. Halliglou O, Okuyaz C, Mert E, Makharoblidze K. Effects of antiepileptic drug therapy on heart rate variability in children with epilepsy. Epilepsy Res. 2008 ;79(1):49-4. Wang YC, Yang CC, Bai YM, Kuo TB. Heart rate variability in schizophrenic patients switched from typical antipsychotic agents to amilsupride and olanzapine. Neuropsyhobiology. 2008;57(4):200-5. Knuettgen D, Trojan S, Weber M, Wolf M, Wappler F. Preoperative measurement of heart rate variability in diabetics: a method to estimate blood pressure stability during anaesthesia induction. Anasthesists. 2005;54:442-9. Corresponding author: Meldijana Omerbegović, MD. Klinika za anesteziju i reanimaciju, Klinički Centar Univerziteta u Sarajevu. Email: [email protected] Med Arh 2009;63(2) • Stručni članci | Professional papers 105