* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download The Heart
Heart failure wikipedia , lookup
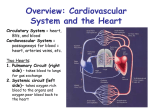
Management of acute coronary syndrome wikipedia , lookup
Electrocardiography wikipedia , lookup
Rheumatic fever wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Artificial heart valve wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Coronary artery disease wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Jatene procedure wikipedia , lookup
Congenital heart defect wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
9/25/13 Collin County Community College ! BIOL. 2402 Anatomy & Physiology ! WEEK 5 The Heart 1 (1578-1657) A groundbreaking work in the history of medicine, English physician William Harvey s Anatomical Essay on the Motion of the Heart and Blood in Animals named the heart as the organ responsible for pumping blood. He also was the first one to propose that CVS is a closed circuit. Although criticized when first published in 1628, Harvey s work was soon accepted by scientists and laid the groundwork for modern physiology. 2 1 9/25/13 The Heart and the CVS The heart is the pump that propels the blood through a closed circulatory system Blood cells never leave this circulation ! Red color indicates blood that isfully oxygenated. Blue color represents blood that is only partially oxygenated. 3 The Heart and the CVS The heart is actually a dual pump • Right side of the heart functions to propel blood through the pulmonary circulation • Left heart propels blood through the systemic circulation 4 2 9/25/13 5 The Heart and the CVS Main purpose of the heart is to generate blood flow and blood pressure One of the key functions is to provide the distant tissues with energy so that they can function . C6H12O6 + 6O2 6CO2 + 6H20 + 38 ATP Exchange of nutrients and gases occurs at the capillary level. • 5 % of total blood volume resides in the capillary beds. • Other 95 % of blood volume , with the heart and blood vessels, is involved in generating a pressure / flow system through the conduit. 6 3 9/25/13 Heart Anatomy Area between the two pleura is called the mediastinum 7 Heart Anatomy Parietal pericardium Epicardium 8 4 9/25/13 Heart Anatomy Visceral pericardium (epicardium) Parietal pericardium Pericarditis : Inflammation of the pericardium 9 Heart Anatomy Heart has two upper atria and two lower ventricles. (Expandable exterior portion of an atria is called the auricle) Right atrium connects to right ventricle and left atrium connects to left ventricle. There is no direct connection between left side and right side. Blood vessels leaving the heart are arteries/aorta Blood vessels arriving at the heart are veins 10 5 9/25/13 Heart Anatomy 11 Heart Anatomy and Blood flow 12 6 9/25/13 Major Blood Vessels at the Heart Major blood vessels of the heart include • Inferior and superior vena cavae • Pulmonary trunk (splits into pulmonary arteries) • Pulmonary veins • Aorta • Brachiocephalic • Left common carotid • Left subclavian 13 Blood flow and Heart valves The heart valves make sure that blood flows only in one direction They prevent backflow and also allow pressure to build up bt creating a closed system Atrio-Ventricular valves are located between the atria and ventricles • Left AV-valve or Bicuspid Valve (Mitral valve) • Right AV - valve or Tricuspid valve • Remember LAB-RAT Semi-lunar valves are located between ventricles and blood-vessel that guides blood out of the ventricle • Aortic semi-lunar valve between left ventricle and aorta • Pulmonary semi-lunar valve between right ventricle and pulmonary artery 14 7 9/25/13 Blood flow and Heart valves AV valves are connected to ventricular walls at the papillary muscles via the chordae tendineae ! They prevent the valves to flip open against the direction of the blood flow. 15 Blood flow and Heart valves 16 8 9/25/13 Blood flow and Heart valves 17 Blood flow and Heart valves 18 9 9/25/13 Blood flow and Heart valves 19 Blood flow and Heart valves 20 10 9/25/13 The Heart wall Components of the heart wall include • Epicardium = visceral pericardium • Myocardium = actual cardiac muscle mass • Endocardium = thin lining of endothelial cells that lines inside 21 The Heart wall 22 11 9/25/13 The Heart wall 23 Left and Right Ventricular Heart Wall 24 12 9/25/13 Microscopic Heart Cell Anatomy Cardiac cells have similar arrangement as striated skeletal cells, with some obvious differences • cells are connected via gap-junctions and desmosomes • have sarcomeres with A-I band arrangement of actin/myosin • 20-25 % of cell volume taken up by mitochondria (compare with 2% in skeletal muscle) • less T-tubules and SR 25 Microscopic Heart Cell Anatomy Cardiac muscle includes most of the structures seen in skeletal muscle, including the striated arrangement of actin and myosin. Adjacent myocarial cells are connected by intercalated disks, which have desmosomes for strength, and gap junctions for the coordination of contraction during pumping. 26 13 9/25/13 Microscopic Heart Cell Anatomy 27 Blood Supply to the Heart Cardiac muscle requires its own blood supply to provide the oxygen and necessary nutrients. This is done by the coronary blood vessels. • Arteries include • the right and left coronary arteries, • anterior and posterior interventricular arteries, • and the circumflex artery • Veins include • the great cardiac vein, • anterior and posterior cardiac veins, • the middle cardiac vein, and the small cardiac vein 28 14 9/25/13 Blood Supply to the Heart Coronary arteries originate at the base of the aorta. Posterior Coronary veins drain into the coronary sinus, which empties into the right atrium. 29 Blood Supply to the Heart CAD = coronary artery disease Ischemia = reduced circulatory supply 30 15 9/25/13 Blood Supply to the Heart Angina pectoris = temporary ischemia develops during increased workload on the heart ( such as exercise) Medication : • sympathetic blockers (propranolol) • Vasodilators ( nitroglycerin) • Calcium blockers 31 Autorhythmic Activity of the Heart The Heart has the property of being able to contract without impulses from the nervous system. This auto-rhythmic property is due to the presence of specialized cell that fire action potentials at a certain rhythm. • Main pacemaker center is called the Sino Atrial (SA) node, located in the upper part of the right atria • Electrical impulses are picked up by the AtrioVentricular Node and conducted via the Bundle of His down the intraventricular septum and the left and right bundle branches. • Finally, electrical impulses are conducted up the walls of the ventricles via the Purkinje fibers. 32 16 9/25/13 Autorhythmic Activity of the Heart The heart s pacemaker and conducting system are shown in bright yellow. 33 Autorhythmic Activity of the Heart The sinoatrial node is the heart s pacemaker because it initiates each wave of excitation with atrial contraction. The Bundle of His and other parts of the conducting system deliver the excitation to the apex of the heart so that ventricular contraction occurs in an upward sweep. 34 17 9/25/13 Autorhythmic Activity of the Heart This electrical discharge by the autorhythmic cells provides a neat coordinated process with the contractile activity of the cardiomyocytes, which in turn provides the heart beat, blood flow and blood pressure. This sweep of electrical activity across the heart is at the basis of the electrocardiogram (ECG or EKG). 35 The Heart Beat Two types of cells are involved in a normal heart beat. • the autorhythmic cells (depolarize with a certain rhythm) • the cardiomyocytes 36 18 9/25/13 The Heart Beat and action potentials What ionic events occur during a normal action potential in a nerve or skeletal muscle cell ? 37 The Heart Beat: AP s in the pacemaker cells The action potential of an autorhythmic cardiac cell. The rhythmic aspect is due to an unstable resting membrane potential called the pacemaker potential or pre-potential. When it reaches threshold it result in an action potential. What causes this prepotential to drift ? 38 19 9/25/13 The Heart Beat: AP s in the pacemaker cells Unstable prepotential is due to closure of K+ channels and brief opening of funny channels that slowly let more Na+ in. Funny channels close and T-calcium briefly open and close. At threshold, L-type Calcium open, resulting in depolarization. L-type Calcium channels close and K+ channels open, resulting in re39 polarization. The Heart Beat: the conducting cells ParaSympathetic activity : • ACh increases K+ permeability during the prepotential drift. • Prolongs the time to reach threshold ; HR slows down Sympathetic activity : • NE binds to beta-1 receptors and opens Ca-channels • This increases the rate of depolarization during the prepotential phase; HR increases ! 40 20 9/25/13 The Heart Beat: the conducting cells • Heart is stimulated by the sympathetic cardioacceleratory center • Heart is inhibited by the parasympathetic cardioinhibitory center 41 The Heart Beat: AP s in the contracting cells The action potential of a myocardial pumping cell. The top graph shows the action potential. The lower graph shows what happens to the ion permeability of the membrane during the same time. 42 21 9/25/13 The Heart Beat: AP s in the contracting cells The action potential of a myocardial pumping cell. The quick opening of voltagegated sodium channels is responsible for the rapid depolarization phase. 43 The Heart Beat: AP s in the contracting cells The action potential of a myocardial pumping cell. The quick opening of voltagegated sodium channels is responsible for the rapid depolarization phase. The prolonged plateau of depolarization is due to the slow but prolonged opening of voltage-gated calcium channels PLUS closure of potassium channels. 44 22 9/25/13 The Heart Beat: AP s in the contracting cells The action potential of a myocardial pumping cell. Opening of potassium channels and closure of the calcium channels results in the repolarization phase. 45 23