* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Mycobacterium tuberculosis
Survey
Document related concepts
Transcript
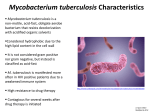
Mycobacterium tuberculosis Introduction:Mycobacteria are Gram-resistant (waxy cell walls), non-motile, pleomorphic rods, related to the Actinomyces. Most Mycobacteria are found in habitats such as water or soil. Tuberculosis , MTB or TB (short for tubercles bacillus However, a few are intracellular pathogens of animals and humans. Mycobacterium tuberculosis, along with M. bovis, M. africanum, and M. microti all cause the disease known as tuberculosis (TB) and are members of the tuberculosis species complex. Each member of the TB complex is pathogenic, but M. tuberculosis is pathogenic for humans while M. bovis is usually pathogenic for animals. Classification:-Kingdom Bacteria. -Phylum Actinobacteria. -Order Actinomycetales. -Suborder Corynebacteriaceae. -Family Mycobacteriaceae. -Genus Mycobacterium. -Species M. tuberculosis approximately (100) species Tuberculosis complex organisms are: Obligate aerobes growing most successfully in tissues with a high oxygen content, such as the lungs. Facultative intracellular pathogens usually infecting mononuclear phagocytes (e.g. macrophages). Slow-growing with a generation time of 12 to 18 hours (c.f. 20-30 minutes for Escherichia coli). So grow sloly in branching chains resembling fungal hyphae. Hydrophobic with a high lipid content in the cell wall. Because the cells are hydrophobic and tend to clump together, they are impermeable to the usual stains, e.g. Gram's stain. Known as "acid-fast bacilli" because of their lipid-rich cell walls, which are relatively impermeable to various basic dyes unless the dyes are combined with phenol. Once stained, the cells resist decolonization with acidified organic solvents and are therefore called "acid-fast". (Other bacteria which also contain mycolic acids, such as Nocardia, can also exhibit this feature.) 1 Symptoms of tuberculosis include: Fever Night-time sweating Loss of weight Persistent cough Constant tiredness Loss of appetite Culture media:1- LOWENSTEIN-jensen (LJ) - Gold standard of tb media - Egg based media - Whole egg (white & yolk), -Potato flour, glycerol - Malachite green. 2- Middlebrook media. 3- ATS media (American Thoracic Society) 2 Identification group for T.B niacin nitrate urease 68c catalase M. tuberculosis + + + 0 M. avium-intra- 0 0 0 + M. bovis v 0 + 0 M. ulcerans 0 0 v + cellular Modern testing:1- Bactec 460 2- GLC & HPLC 3- PCR 4- Nucleic acid probes 5- Restriction fragment length polymorphism Diagnosis:1- positive tuberculin skin test (Mantoux skin test 0.1 ml in 5 tuberculin units of PPD ) 2- An immune reaction to a small quantity of tuberculosis antigens. 3- It can be confirmed by X rays of the chest and microscopic examination of sputum. 4- Detection of significant numbers of acid-fast bacilli (using the Ziehl-Neelsen stain) in sputum or tissue samples is considered a positive diagnosis, 5- Although disease may confirmed by laboratory culture of the bacterium (difficult, dangerous and slow - takes at least 4 weeks). 3 Ziehl-Neelsen acid-fast staining procedure: 1. Heat fix cells on glass microscope slide. 2. Flood the slide with carbol fuchsin stain. 3. Heat the slide gently until it steams (5 min). 4. Pour off the carbol fuchsin. 5. Wash slide thoroughly with water. 6. Decolourize with acid-alcohol (5 min). 7. Wash slide thoroughly with water. 8. Flood slide with methylene blue counterstain for 1 min. 9. Wash with water. 10. Blot excess water and dry in hand over bunsen flame. 4 Transmission: 1-Transmission of TB occurs primarily by the aerosol route. 2- through the gastrointestinal tract. 3- Coughing by people with active TB produces droplet nuclei containing infectious organisms which can remain suspended in the air for several hours. Infection occurs if inhalation of these droplets results in the organism reaching the alveoli of the lungs. Only 10% of immunocompetent people infected with M. tuberculosis develop active disease in their lifetime - the other 90% do not become ill and cannot transmit the organism. However, in some groups such as infants or the immunodeficient (e.g. those with AIDS or malnutrition), the proportion who develop clinical TB is much higher. In the lung, the organism is taken up by alveolar macrophages and carried to lymph nodes, from where it may spread to multiple organs. Two to eight weeks after infection, cell mediated immunity (CMI) and hypersensitivity (DTH) develop leading to the characteristic reaction to the tuberculin test and, in immunocompetent individuals, containment of infection. Inflammatory immune responses eventually result in lung damage. 5 TB treated:TB is currently treated by means of combination therapy, using cocktails of 3-4 drugs with different properties: Antibacterial activity: e.g. isoniazid, rifampin, streptomycin Inhibiting the development of resistance: e.g. isoniazid, rifampin, ethambutol Many countries use Bacillus Calmette-Guérin (BCG) vaccine as part of their TB control programmes, References :^ a b c Ryan KJ, Ray CG (editors) (2004). Sherris Medical Microbiology (4th ed.). McGraw Hill. ISBN 0-8385-8529-9. 2. ^ Cole ST, Brosch R, Parkhill J, et al. (June 1998). "Deciphering the biology of Mycobacterium tuberculosis from the complete genome sequence". Nature 393 (6685): 537–44. doi:10.1038/31159. PMID 9634230. 3. ^ Camus JC, Pryor MJ, Médigue C, Cole ST (October 2002). "Re-annotation of the genome sequence of Mycobacterium tuberculosis H37Rv". Microbiology (Reading, Engl.) 148 (Pt 10): 2967–73. PMID 12368430. http://mic.sgmjournals.org/cgi/pmidlookup?view=long&pmid=12368430. 4. ^ Arnvig KB, Young DB (August 2009). "Identification of small RNAs in Mycobacterium tuberculosis". Mol. Microbiol. 73 (3): 397–408. doi:10.1111/j.13652958.2009.06777.x. PMC 2764107. PMID 19555452. http://www3.interscience.wiley.com/resolve/openurl?genre=article&sid=nlm:pubmed&is sn=0950-382X&date=2009&volume=73&issue=3&spage=397. Retrieved 2010-08-31. 1. Assist-Lecturer Abdul-Karim S. Alyassaree Microbiology department College of veterinary medicine /Babylon university 6