* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download File
Cardiac contractility modulation wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Heart failure wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Artificial heart valve wikipedia , lookup
Electrocardiography wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Jatene procedure wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
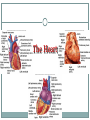
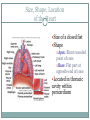
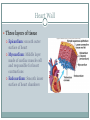
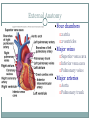
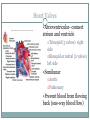
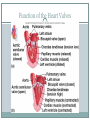
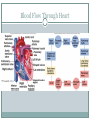
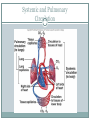
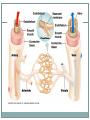
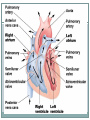
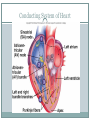
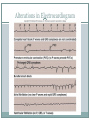
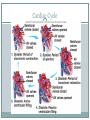
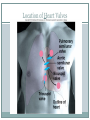
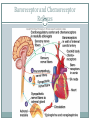
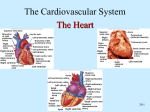
The Heart Functions of the Heart Generate blood pressure Route blood Heart separates pulmonary and systemic circulations Ensure one-way blood flow Heart valves ensure one-way flow Regulate blood supply Changes in contraction rate and force match blood delivery to changing metabolic needs Size, Shape, Location of the Heart Size of a closed fist Shape Apex: Blunt rounded point of cone Base: Flat part at opposite end of cone Located in thoracic cavity within pericardium Heart Wall Three layers of tissue Epicardium: smooth outer surface of heart Myocardium: Middle layer made of cardiac muscle cell and responsible for heart contractions Endocardium: Smooth inner surface of heart chambers External Anatomy Four chambers 2 atria 2 ventricles Major veins Superior vena cava Inferior vena cava Pulmonary veins Major arteries Aorta Pulmonary trunk Heart Valves Atrioventricular- connect atrium and ventricle Tricuspid (3 valves)- right side Bicuspid or mitral (2 valves) left side Semilunar Aortic Pulmonary Prevent blood from flowing back (one-way blood flow) Function of the Heart Valves Blood Flow Through Heart Systemic and Pulmonary Circulation Amazing Heart Facts! An average adult body contains about five quarts of blood. All the blood vessels in the body joined end to end would stretch 62,000 miles or two and a half times around the earth. The heart circulates the body's blood supply about 1,000 times each day. The heart pumps the equivalent of 5,000 to 6,000 quarts of blood each day. Conducting System of Heart Electrical Properties Resting membrane potential (RMP) present Action potentials Rapid depolarization followed by rapid, partial early repolarization. Prolonged period of slow repolarization which is plateau phase and a rapid final repolarization phase Voltage-gated channels Action Potentials in Skeletal and Cardiac Muscle SA Node Action Potential Refractory Period Absolute: Cardiac muscle cell completely insensitive to further stimulation Relative: Cell exhibits reduced sensitivity to additional stimulation Long refractory period prevents tetanic contractions Electrocardiogram Action potentials through myocardium during cardiac cycle produces electric currents than can be measured Pattern P wave QRS complex Atria depolarization Ventricle depolarization Atria repolarization T wave: Ventricle repolarization Cardiac Arrhythmias Tachycardia: Heart rate in excess of 100bpm Bradycardia: Heart rate less than 60 bpm Sinus arrhythmia: Heart rate varies 5% during respiratory cycle and up to 30% during deep respiration Premature atrial contractions: Occasional shortened intervals between one contraction and succeeding, frequently occurs in healthy people Alterations in Electrocardiogram Cardiac Cycle Heart is two pumps that work together, right and left half Repetitive contraction (systole) and relaxation (diastole) of heart chambers Blood moves through circulatory system from areas of higher to lower pressure. Contraction of heart produces the pressure Cardiac Cycle Events during Cardiac Cycle Heart Sounds First heart sound or “lubb” Atrioventricular valves and surrounding fluid vibrations as valves close at beginning of ventricular systole Second heart sound or “dupp” Results from closure of aortic and pulmonary semilunar valves at beginning of ventricular diastole, lasts longer Third heart sound (occasional) Caused by turbulent blood flow into ventricles and detected near end of first one-third of diastole Location of Heart Valves Mean Arterial Pressure (MAP) Average blood pressure in aorta MAP=CO x PR CO is amount of blood pumped by heart per minute CO=SV x HR SV: Stroke volume of blood pumped during each heart beat HR: Heart rate or number of times heart beats per minute Cardiac reserve: Difference between CO at rest and maximum CO PR is total resistance against which blood must be pumped Factors Affecting MAP Regulation of the Heart Intrinsic regulation: Results from normal functional characteristics, not on neural or hormonal regulation Starling’s law of the heart Extrinsic regulation: Involves neural and hormonal control Parasympathetic stimulation Supplied by vagus nerve, decreases heart rate, acetylcholine secreted Sympathetic stimulation Supplied by cardiac nerves, increases heart rate and force of contraction, epinephrine and norepinephrine released Heart Homeostasis Effect of blood pressure Baroreceptors monitor blood pressure Effect of pH, carbon dioxide, oxygen Chemoreceptors monitor Effect of extracellular ion concentration Increase or decrease in extracellular K+ decreases heart rate Effect of body temperature Heart rate increases when body temperature increases, heart rate decreases when body temperature decreases Baroreceptor and Chemoreceptor Reflexes Baroreceptor Reflex Chemoreceptor Reflex-pH Effects of Aging on the Heart Gradual changes in heart function, minor under resting condition, more significant during exercise Hypertrophy of left ventricle Maximum heart rate decreases Increased tendency for valves to function abnormally and arrhythmias to occur Increased oxygen consumption required to pump same amount of blood