* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download PBL- Case 1: Cardiac Arrhythmias Pre
Remote ischemic conditioning wikipedia , lookup
Heart failure wikipedia , lookup
Coronary artery disease wikipedia , lookup
Rheumatic fever wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Cardiac surgery wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Myocardial infarction wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Electrocardiography wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Atrial fibrillation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
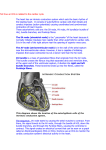
PBL- Case 1: Cardiac Arrhythmias Pre-Meeting Questions 1. Describe how the interaction between the anatomy & physiology of the cardiac conduction system results in generation of the heart beat Myocardial cells have 2 functions: - contraction (myocytes- majority) - initation & conduction of electrical impulses o form ‘conducting system of the heart’, modified myocytes o Generate impulses which are conducted to the myocytes contraction ‘Excitation-coupling’ Rate of impulse/force of contraction modified by ANS & stretch. Conduction of the heart: Sinus node: o Lies b/w junction SVC/RA o Generates impulses automatically via spontaneous depolarisation of its membrane (quicker than other cardiac cells- ‘pacemaker’) o Relies mostly on influx of Na+ ions into the cells o Rate of depolarisation modulated by autonomic tone, stretch, temperature, hypoxia, blood pH and hormonal influences i.e 5HT, T3 Atrial & ventricular myocyte APs o Sinus node depolarisation of atrial & ventricular myocytes o Resting membrane of these cells relies on flow of K+ into cells (Na & Ca channels closed) o Arrival of adjacent APs triggers opening of voltage-gated self-inactivating Na+ channels sharp - depolarisation spike. o This is followed by a partial repolarisation. o Plateau phase (unique to myocytes): result of calcium influx- sustained plateau prevents early reactivation of the myocytes & determines the strength of contraction AV node, Bundle of His, Purkinje fibres o Depolarisation continues AV node (lies beneath right atrial endocardium w/i lower inte-atrial septum). o AV node continues as BoH, which conducts the cardiac impulse rapidly towards the ventricle o BoH divides at crest of interventricular septum Right bundle branch: continues down the right side of the iv septum to the apex. It then radiates & divides to form Purkinje network, which spreads t/o the subendocardial surface of the right ventricle Left bundle branch: short structure, fans out into many strands on the left side of the iv septum Strands can be grouped into anterior hemi-bundle: supps Purkinje network of anterior & superior surfaces of left ventricle o Posterior hemi-bundle: supps inferior & posterior surfaces o AV impulse conduction is slow & dependent on slow trans-membrane Ca flow o In atria, ventricles and His-Purkinje system, conduction is rapid b/c of APs generated by rapid Na diffusion In adults, the normal resting heart rate is 60-80 bpm. Higher in kids (ECG: P wave- SA node; PR interval- AV node/Bundles; QRS complex- Purkinje fibres/ventricular myocardium; T wave- ventricular repolarisation). 2. What are the incidence and prevalence in the community of the most common cardiac arrhythmias, including atrial fibbrilation, atrial flutter, supra-ventricular tachycardia and ventricular tachycardia? Atrial fib: common, 5-10% patients >65 y/o (also occurs paroxysmally in younger patients) Atrial flutter: Supra-ventricular tachycardia: Most common in children, 20-60% ped patients present in 1st year of life Ventricular tachycardia: 3. Discuss the significance of age and underlying cardiac pathology in relation to their impact on the risk of occurrence of specific arrhythmias High prevalence of CAD, CHF and valvular disease and calcification (common in older patients) puts them at higher risk of atrial fibrillation. Cardiac valvular stenosis or regurgitation caused by either rheumatic or age related degenerative changes increases left atrial pressure and results in the enlargement of the left atrium and/or the left ventricle. These changes to cardiac structure and function activate sympathetic nerves and modulate hormones that control ion channels, which might explain the high prevalence of atrial fibrillation in older patients with heart failure and valvular dysfunction. 4. What investigations are routinely used to identify/diagnose common arrhythmias? -ECG: Look for signs of IHD, AF, short PR interval (WPW syndrome), long QT inteval (metabolic imbalance, drugs, congenital), U waves (hypokalaemia) - 24 hr ECG monitoring - exercise ECG - FBC, U & E, glucose, Ca, Mg, TSH - Echo: structural heart disease? (i.e. mitral stenosis)