* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download PIAS-KT Educational Outreach
Survey
Document related concepts
Tuberculosis wikipedia , lookup
Methicillin-resistant Staphylococcus aureus wikipedia , lookup
Gastroenteritis wikipedia , lookup
Whooping cough wikipedia , lookup
Typhoid fever wikipedia , lookup
Oesophagostomum wikipedia , lookup
Anaerobic infection wikipedia , lookup
Staphylococcus aureus wikipedia , lookup
Neonatal infection wikipedia , lookup
Mycoplasma pneumoniae wikipedia , lookup
Carbapenem-resistant enterobacteriaceae wikipedia , lookup
Neisseria meningitidis wikipedia , lookup
Clostridium difficile infection wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Transcript
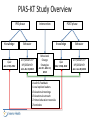
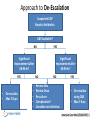
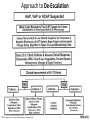
UTI & Pneumonia Translating Knowledge into Practice PIAS-KT Study Sukhjinder Sidhu Sean Gorman Richard Slavik Tasha Ramsey Sarah Murray Nicole Bruchet Attendance • Please email Brenda Flood ([email protected]) if you attended this session • Please email Brenda Flood ([email protected]) if you view this presentation online at a later date THANK YOU! • YOU SURPASSED OUR PROJECTED PARTICIPATION RATE FOR THE PRE-QUIZ! • STAY TUNED FOR A POST-QUIZ THAT WILL BE SENT OUT IN MID-MARCH • THANK YOU TO TASHA RAMSEY FOR HER EXPERT REVIEW OF THIS PRESENTATION Speaker Disclosure • The speakers have no actual or potential conflicts of interest to disclose Outline • • • • • • • PIAS-KT Study Overview Local Opinion Leaders Prevalence and Impact of UTIs & Pneumonia Antimicrobial Stewardship Key Pharmacist Interventions for UTIs & Pneumonia DTP Tracker Data for UTIs & Pneumonia UTIs & Pneumonia Therapeutics – – – – When to treat with antibiotics and When Not to treat? What antibiotics to initiate and Why? When, How, and Why to de-escalate antibiotics? How long to treat with antibiotics? Objectives • To review the pharmaceutical care of patients with UTIs & Pneumonia including: – Key pharmacist interventions – Indications for antibiotic therapy – Initial empiric antibiotic therapy recommendations – Antibiotic de-escalation strategies – IV to PO step-down considerations – Duration of antibiotic therapy PIAS-KT Study Overview PRE phase Knowledge Quiz Jan 17-30, 2014 Intervention POST phase Behavior DTP/DSEM DTP KPI/DSEM KPI Jul 1-Dec 31,2013 Behavioral Change Strategies Jan 30 – Mar 14, 2014 Knowledge Behavior Quiz DTP/DSEM DTP KPI/DSEM KPI Mar 17-28, 2014 1. Audit & Feedback 2. Local opinion leaders 3. Educational meetings 4. Educational outreach 5. Printed education materials 6. Reminders Jan 1-Jun 30, 2014 Local Opinion Leaders • • • • • • • KGH – Dawn Robb RIH – Kim Winters PRH/SOH – Orysya Fetterly VJH – Chelsea Argent SLH/OMH – Ian Petterson KBH/KLH – Michael Conci EKH/GDH – Darren Feere Prevalence & Impact of UTIs Prevalence – Approximately 4,000,000 UTIs/year in Canada – Affects 20% of women between 15-29 yo – Number 1 healthcare-associated infection – 16th most common non-surgical reason for IH admission Impact – – – – 660 cases and 3200 acute bed-days at IH Hospital-acquired UTIs associated with extra day of hospitalization Up to 25% of patients with UTI receive inappropriate therapy Up to 50% of patients with asymptomatic catheter-associated bacteriuria are treated with antibiotics (which is inappropriate) Mayo Clin Proc 2007;82:181-5.; Can J Infect Dis Med Microbiol 2005;16:166-70. Prevalence & Impact of Pneumonia Prevalence – Approximately 170,000 cases of CAP each year in Canada – HAP/VAP is 2nd most common nosocomial infection in Canada – 5th most common non-surgical reason for IH admission Impact – – – – 1300 cases and 7000 acute bed-days at IH each year CAP is the leading infectious cause of death Up to 15% of patients with CAP receive inadequate therapy Up to 75% of patients with HAP/VAP receive inadequate therapy Clin Infect Dis 2005;41:1709-16.; Postgrad Med 2010;122:130-141. Antimicrobial Stewardship Definition • An activity (or activities) that includes – Appropriate antibiotic selection – Appropriate antibiotic dosing – Appropriate antibiotic route selection – Appropriate antibiotic duration of therapy Clin Infect Dis 2007;44:159-77. Antimicrobial Stewardship Goals • Optimize clinical outcomes by ensuring effective antimicrobial therapy • Minimize collateral damage from antimicrobials – Antimicrobial resistance – Antimicrobial toxicity – Costs of inappropriate antimicrobial use – Superinfections (e.g. Clostridium difficile) Clin Infect Dis 2007;44:159-77. Clinical Pharmacists’ Role in Antimicrobial Stewardship PHARMACEUTICAL CARE ANTIMICROBIAL STEWARDSHIP Urinary Tract Infection Key Pharmacist Interventions 1. Initiate appropriate antibiotics for symptomatic UTI 2. Discontinue empiric antibiotics started for UTI that are not indicated 3. De-escalate antibiotics for UTI based on C&S data and clinical response 4. Perform IV to PO step-down of antibiotics for UTI 5. Promote appropriate duration of antibiotic therapy for UTI IH UTI Key Pharmacist Interventions, April 21, 2011 Pneumonia Key Pharmacist Interventions 1. Initiate appropriate antibiotics for pneumonia 2. Discontinue empiric antibiotics started for pneumonia that are not indicated 3. De-escalate antibiotics for pneumonia based on C&S data and clinical response 4. Perform IV to PO step-down of antibiotics for pneumonia 5. Promote appropriate duration of antibiotic therapy for pneumonia IH Pneumonia Key Pharmacist Interventions, April 21, 2011 Project Alignment CPhA “Blue Print” for Pharmacy Practice CSHP “Vision 2015” Canadian Clinical Pharmacy KPI Collaborative Accreditation Canada MOHS KRAs and CCM groups IH SET goals, objectives IH Pharmacy Clinical Priorities DTP Tracker Data - UTI • UTI ranks #6 in disease prevalence for all Rx interventions • UTI ranks #3 in disease prevalence for 8 DSEM interventions • UTI ranks #2 in disease prevalence for key pharmacist interventions DTP Tracker Data - UTI • AIMS study showed a statistically significant, clinically important increase after DSEMs – DSEM DTP/total DTP (27.9% to 31.9%, p<0.05) – KPI/total DTP (21.7% to 25.8%, p<0.05) • In UTI subgroup, AIMS failed to show a statistically significant benefit – DSEM DTP/total DTP (3.91% to 3.93%, p=NS) – KPI/total DTP (3.82% to 4.61%, p=NS) DTP Tracker Data - Pneumonia • Pneumonia ranks #3 in disease prevalence for all Rx interventions • Pneumonia ranks #2 in disease prevalence for 8 DSEM interventions • Pneumonia ranks #3 in disease prevalence for key pharmacist interventions DTP Tracker Data - Pneumonia • In Pneumonia subgroup, AIMS failed to show a statistically significant benefit – DSEM DTP/total DTP (4.75% to 4.90%, p=NS) • However, in Pneumonia subgroup, AIMS demonstrated a statistically significant REDUCTION – KPI/total DTP (5.07% to 3.94%, p=0.016) Pharmaceutical Care of UTI and Pneumonia UTI Pharmaceutical Care Outline • When and When Not to treat with antibiotics? • What antibiotics to initiate and Why? • When, How, and Why to de-escalate antibiotics? • How long to treat with antibiotics? What Makes a UTI ‘Complicated’? • Patients with structural or functional abnormalities of the genitourinary tract – Obstruction – Instrumentation (including catheters) – Impaired voiding – Metabolic abnormalities – Immunocompromised – Men Can J Infect Dis Med Microbiol 2005;16:349-60. UTI “Why should antibiotics be initiated?” • duration of symptoms • abscesses, metastatic infection, septic shock, AKI Clin Infect Dis 2005;40:643-54. UTI “When should antibiotics be initiated?” – Clinical manifestations of cystitis • Dysuria, frequency, urgency, suprapubic pain, hematuria – Clinical manifestations of pyelonephritis • Above symptoms together with fever (>38°C), chills, flank pain, costovertebral angle tenderness, and nausea/vomiting – Asymptomatic bacteriuria in pregnancy Cystitis at IH “When should antibiotics be initiated?” “If clinically feasible, initiation of antimicrobial therapy should be delayed until results of urine culture are available” Can J Infect Dis Med Microbiol 2005;16:349-60. UTI at Interior Health “What antibiotics should be initiated and why?” Organisms Associated with Urinary Tract Infections Infection 2007;35:150-3. (Calgary Data 2004-5) UTI at Interior Health “What antibiotics should be initiated and why?” PO options IV options Antibiotic Susceptibility (%)* Collateral Damage Risk Nitrofurantoin 94-98 Low Cefixime 92-94 Probable Amox/Clav 84-90 Probable TMP/SMX 80-83 Possible Ciprofloxacin 78-85 Probable Ceftriaxone 94-97 Probable Gentamicin 94-96 Possible Pip/Tazo 94-97 Probable Ampicillin 61-68 Probable *E. coli Susceptibilities at IH 2012 UTI at Interior Health “What antibiotics should be initiated and why?” *Enterococcus Susceptibilities at IH 2012 UTI at Interior Health “What antibiotics should be initiated and why?” • Risk Factors for Antibiotic Resistant UTIs – Abx exposure (especially to TMP/SMX or FQ) in past 3 months – Travel to endemic area – Previous multi-drug resistant UTI Clin Infect Dis 2005;40:643-54. UTI at Interior Health “What antibiotics should be initiated and why?” • Oral Antibiotic Selection – Oral antibiotics are first line for cystitis – Oral antibiotics are first line for uncomplicated pyelonephritis (not acutely ill) • IV Antibiotic Selection – – – – Unable to tolerate oral therapy (nausea/vomiting/ileus) Impaired GI absorption Hemodynamic instability (acutely ill) Infecting organism resistant to available oral options Clin Infect Dis 2005;40:643-54., Can J Infect Dis Med Microbiol 2005;16:349-60. Complicated Cystitis at IH “What antibiotics should be initiated?” “Oral antimicrobial therapy is appropriate for most episodes” Can J Infect Dis Med Microbiol 2005;16:349-60. Uncomplicated Cystitis at IH “What antibiotics should be initiated?” Recommendations for Empiric Therapy 1. Nitrofurantoin 100 mg PO BID x 5 days (CrCl ≥ 40 mL/min) 2. Trimethoprim/Sulfamethoxazole i DS PO BID x 3 days • Cefixime 400 mg PO Daily x 3 days • Amoxicillin/Clavulanate 875 mg PO BID x 3 days • Amoxicillin/Clavulanate 500 mg PO TID x 3 days Complicated Cystitis at IH “What antibiotics should be initiated?” Recommended Empiric Oral Options 1st Line • • • • Cefixime 400 mg PO Daily x 7-14 days Amoxicillin/Clavulanate 875 mg PO BID x 7-14 days Amoxicillin/Clavulanate 500 mg PO TID x 7-14 days Trimethoprim/Sulfamethoxazole i DS PO BID x 7-14 days 2nd Line (high prevalence resistance) • Ciprofloxacin 500 mg PO BID x 7-14 days Complicated Cystitis at IH “What antibiotics should be initiated?” Recommended Empiric IV Options • Ampicillin + Gentamicin • Ampicillin + Ceftriaxone • Piperacillin/Tazobactam +/- Gentamicin Uncomplicated Pyelonephritis at IH “What antibiotics should be initiated and why?” Recommend Empiric Oral Therapy • Same as for uncomplicated cystitis EXCEPT: – No nitrofurantoin – Longer duration of therapy (7-14 days) Uncomplicated Pyelonephritis at IH “What antibiotics should be initiated and why?” Recommended Empiric IV Therapy for Acutely Ill Patients • Gentamicin 5-7 mg/kg/day IV OR • Ceftriaxone 1-2G IV daily Complicated Pyelonephritis at IH “What antibiotics should be initiated and why?” Recommended Empiric Oral Options • Same as for complicated cystitis 1st Line • • • • Cefixime 400 mg PO Daily x 7-14 days Amoxicillin/Clavulanate 875 mg PO BID x 7-14 days Amoxicillin/Clavulanate 500 mg PO TID x 7-14 days Trimethoprim/Sulfamethoxazole i DS PO BID x 7-14 days 2nd Line (high prevalence resistance) • Ciprofloxacin 500 mg PO BID x 7-14 days Complicated Pyelonephritis at IH “What antibiotics should be initiated and why?” Recommended Empiric IV Options • Same as for complicated cystitis – Ampicillin + Gentamicin – Ampicillin + Ceftriaxone – Piperacillin/Tazobactam +/- Gentamicin Asymptomatic Bacteriuria in Pregnancy “What antibiotics should be initiated and why?” Recommended Antibiotic Therapy • Wait for results of screening urine C&S • Select narrowest spectrum agent that is safe in pregnancy – – – – – – Amoxicillin/Clavulanate Amoxicillin Cefixime Cephalexin Nitrofurantoin (avoid in 3rd trimester) TMP/SMX (avoid in 1st and 3rd trimesters) UTI Therapeutics “What is antibiotic de-escalation and why is it important?” • Antibiotic De-escalation – Replace empiric broad-spectrum regimen with a more narrow spectrum regimen – Organism identified with susceptibilities – Intended to reduce collateral damage – De-escalation for UTIs is under-performed Infection 2013;41:211-14. UTI Therapeutics “When and How should antibiotics be de-escalated?” • When to de-escalate – Once urine C&S known – No other suspected infections – No patient-limiting factors (e.g. allergy) Infection 2013;41:211-14. UTI Therapeutics “When and How should antibiotics be de-escalated?” • How to de-escalate – Broad spectrum to narrowest spectrum – Narrowest spectrum with collateral damage risk Examples Empiric Step-Down Ciprofloxacin Amoxicillin Cefixime Cephalexin Ceftriaxone TMP/SMX Pip/Tazo Amoxicillin/Clav Ceftriaxone Cefixime Infection 2013;41:211-14. UTI Therapeutics “How should antibiotics be de-escalated?” • IV to PO Step-Down – Tolerates oral intake – No factors affecting absorption – Hemodynamically stable – If acutely ill pyelonephritis and considering PO βlactam, patient should receive at least 1 dose of Ceftriaxone OR Aminoglycoside Infection 2013;41:211-14. Interior Health IV to PO Step-Down Policy • Pharmacists Have IV-PO Step-Down Authority – – – – – Applies to Ciprofloxacin/Moxifloxacin Duration IV antibiotics: ≥ 48 hours Tolerating other PO medications, fluids, or foods x 12 hours No potential problems with absorption Clinically stable (stable BP, resolving fever/afebrile, adequate urine output, absence of encephalopathy, WBC normal or normalizing) • Exclusions • Febrile neutropenia, gram negative bacteremia, CNS infections, septic shock, severe cellulitis InsideNet – Pharmacist managed IV to PO conversion program (2006) UTI Therapeutics “How long to treat with antibiotics?” • Uncomplicated cystitis – 3-7 days (5-7 days for nitrofurantoin) • Complicated cystitis – 7-14 days • Pyelonephritis – 7-14 days Candida-Associated Cystitis • Indications for treatment – Symptomatic cystitis – Asymptomatic, but high risk (neutropenia, planned urologic manipulation) • Recommended treatment – Fluconazole 200-400 mg PO daily x 14 days – Amphotericin 0.3-0.6 mg/kg IV x 7 days (2nd line) Clin Infect Dis 2009;48:503-35. Pneumonia Pharmaceutical Care Outline • When and When Not to treat with antibiotics? • What antibiotics to initiate and Why? • When, How, and Why to de-escalate antibiotics? • How long to treat with antibiotics? IH Pneumonia DSEM Pneumonia When and Why Antibiotic Treatment? • Physician/NP Diagnosis • • • • Varies depending on outpatient/inpatient Chest x-ray infiltrates PLUS Fever, purulent secretions, elevated WBC Other clinical manifestations: dyspnea, pleuritic chest pain • Consequences of Pneumonia – Reduced survival – Increased risk of ICU admission – Prolonged length of hospitalization Clin Infect Dis 2007;44:sS.; Pneumonia DSEM 2008. Community-Acquired Pneumonia • Patients not hospitalized in previous 14 days Clin Infect Dis 2000;31:383-421. Community-Acquired Pneumonia “What antibiotics should be initiated and why?” Microbiologic Etiology Patient Setting Outpatients Organisms Mycoplasma pneumoniae, Streptococcus pneumoniae, Haemophilus influenzae Inpatients (non-ICU) Streptococcus pneumoniae, Mycoplasma pneumoniae, Chlamydia pneumoniae, Haemophilus influenzae, other gram (-) bacilli, Staphylococcus aureus Inpatients (ICU) Streptococcus pneumoniae, various gram (-) bacilli, Legionella pneumophilia, Staphylococcus aureus Clin Infect Dis 2000;31:347-82. Community-Acquired Pneumonia Risk Factors for AROs Drug-Resistant Pneumococci MRSA Pseudomonas aeruginosa Age > 65 yrs Dialysis Structural Lung Dz Abx exposure 90 d* Hospitalization Corticosteroids (> 10 mg Prednisone/day) Alcoholism ICU Admission Immunosuppression Prior/Prolonged Abx > 7 days Broad Abx in past month Comorbidities Previous colonization Malnutrition Exposed to child in daycare *β-Lactam, Fluoroquinolone, Macrolide Can J Infect Dis Med Microbiol 2008;19:19-53., Clin Infect Dis 2007;44:(Suppl 2):S27-72. Community-Acquired Pneumonia “What antibiotics should be initiated and why?” Antibiotic Susceptibility (%) Cost/day S. pneumo H. flu Atypicals Ceftriaxone 99-100 99-100 Ø $2.62 Amox/Clav 99-100 92-97 Ø $0.72 Amoxicillin 99-100 73-80* Ø $0.18-0.36 Moxifloxacin 99 √ √ $4.00 (PO) $17.50 (IV) Doxycycline 81-89 88-92 √ $0.18 Azithromycin 74-89 NR √ $1.28 (PO) $8.32 (IV) NR 91-95 Ø $1.84-3.68 (PO) $31.56 (IV) Cefuroxime *Ampicillin Susceptibility Susceptibilities at IH 2012 Community-Acquired Pneumonia “What antibiotics should be initiated?” Recommendations for Empiric Therapy in Hospital • General Ward 1. Moxifloxacin 400 mg PO/IV daily 2. Ceftriaxone 2 g IV daily + Azithromycin 500 mg IV daily • ICU 1. Ceftriaxone 2 g IV daily + Azithromycin 500 mg IV daily 2. Ceftriaxone 2 g IV daily + Moxifloxacin 400 mg IV daily Clin Infect Dis 2007;44:(Suppl 2):S27-72. Approach to De-Escalation Suspected CAP Empiric Antibiotics C&S Available? NO Significant Improvement after 48-96 hr? • De-escalate • Max 7 Days Significant Improvement after 48-96 hr? NO YES • • • • • YES NO Review Abx Review Dose Re-culture Complication? Consider non-infection YES • De-escalate using C&S • Max 7 days Intensive Care Med 2014;40:92-5. Community-Acquired Pneumonia “Pathogen-Directed Therapy” Organism Preferred Alternatives S. pneumoniae; MIC < 2 mg/L Pen G, amoxicillin Macrolide, cephalosporins, clindamycin, doxycline, respiratory fluoroquinolone S. pneumonia; MIC ≥ 2 mg/L 3rd generation cephalosporin, fluoroquinolone Vancomycin, linezolid, amoxicillin >3 g/day if MIC ≤ 4 mg/L H. influenzae (no betalactamase) Amoxicillin Fluoroquinolone, doxycycline, azithromycin, clarithromycin H. Influenza (beta-lactamase) 2nd or 3rd generation cephalosporin, amoxicillinclavulanate Fluoroquinolone, doxycycline, azithromycin, clarithromycin Enterobacteriacea 3rd generation cephalosporin, e carbapenem P. aeruginosa Antipseudomonal beta-lactam Beta-lactam/beta-lactamase inhibitor, fluoroquinolone Clin Infect Dis 2007;44:(Suppl 2):S27-72. Aminoglycoside PLUS cipro or Community-Acquired Pneumonia “IV to PO Step-down Criteria” • Normal functioning GI tract AND • Able to ingest medications AND • Improving clinically AND • Clinical stability – T < 37.8 0C – HR < 100 bpm – RR < 24 breaths/min – SBP > 90 mm Hg – Arterial O2 sat > 90% – Normal mental status Clin Infect Dis 2007;44:(Suppl 2):S27-72. Interior Health IV to PO Step-Down Policy • Pharmacists Have IV-PO Step-Down Authority – – – – – Applies to Ciprofloxacin/Moxifloxacin Duration IV antibiotics: ≥ 48 hours Tolerating other PO medications, fluids, or foods x 12 hours No potential problems with absorption Clinically stable (stable BP, resolving fever/afebrile, adequate urine output, absence of encephalopathy, WBC normal or normalizing) • Exclusions • Febrile neutropenia, gram negative bacteremia, CNS infections, septic shock, severe cellulitis InsideNet – Pharmacist managed IV to PO conversion program (2006) Community-Acquired Pneumonia “How long to treat?” • Minimum treatment duration 7 days AND • Afebrile (T ≤ 37.8 x 48-72 h) AND • ≤ 1 sign of CAP-related clinical instability • • • • • • • T ≥ 37.8 HR ≥ 100 beats/min RR ≥ 24 breaths/min SBP ≤ 90 mmHg SaO2 ≤ 90% or PaO2 ≤ 60 mm Hg on room air Inability to maintain oral intake Abnormal mental status • Azithromycin 500 mg IV daily x 3 days (with ceftriaxone) Clin Infect Dis 2007;44:(Suppl 2):S27-72. Hospital-Acquired/ Ventilator-Associated Pneumonia • HAP – Pneumonia that occurs > 48 hours after admission • VAP – Pneumonia arising > 48 hours after intubation Clin Infect Dis 2000;31:383-421. HAP/VAP “What antibiotics should be initiated and why?” Microbiologic Etiology Patient Setting Organisms S. pneumoniae, MSSA, H. influenzae, E. coli, Early HAP (≤ 4 days) Klebsiella spp., Enterobacter spp., Proteus spp., Serrratia spp Late HAP (> 4 days) VAP All of the above PLUS: MRSA, P. aeruginosa All of the above PLUS: Late (> 4 days on ventilator): MRSA, P. aeruginosa, Acinetobacter spp., Stenotrophomonas spp. HAP/VAP “What antibiotics should be initiated and why?” Susceptibility (%) Antibiotic E. coli Klebsiella spp. Enterobacter P. aeruginosa Ceftriaxone 94-97 95-99 NR R Moxifloxacin NR NR NR NR Piperacillin/ Tazobactam 94-97 95-99 NR 91-95 Amoxicillin/ Clavulanate 84-90 82-96 R R Meropenem 100 99-100 98-100 96-98 Ciprofloxacin 78-85 92-99 95-100 80-89 Gentamicin 94-96 97-100 99-100 82-89 Ceftazidime NR NR NR 94-96 Susceptibilities at IH 2012 HAP/VAP “What antibiotics should be initiated and why?” MDR Bacteria Risk Factors HAP/VAP “What antibiotics should be initiated and why?” Infect Dis Clin N Am 2004;18:939-962. RSS 2012 HAP/VAP “What antibiotics should be initiated and why?” Reasonable IH Strategy Early HAP/VAP, and no risks for MDR bugs Ceftriaxone Late HAP/VAP, or risks for MDR bugs Piperacillin-tazobactam Piperacillin-tazobactam Ciprofloxacin (?) Moxifloxacin Meropenem* +/- aminoglycoside (PA) +/- vancomycin (?) RSS 2012 Approach to De-Escalation Am J Respir Crit Care Med 2005;171:388-416. RSS 2012 Pneumonia Therapeutics “How long to treat with antibiotics?” Shorter Duration of Therapy Potential Benefits • • • • • Overall antibiotic use Resistance rates Super-infection Drug costs Adverse events Potential Risks • Treatment failures • Relapse rates • Re-infection rates • Complications J Clin Pharmacol Therap 2003;28:123-129. RSS 2012 HAP/VAP “How long to treat?” Diagnosis* Duration HAP/VAP (not caused by MRSA/NLFGNR**) 7-8 days HAP/VAP (caused by MRSA/NLFGNR) 14-15 days *Uncomplicated Pneumonia **Non-lactose fermenting Gram negative rods Am J Respir Crit Care Med 2005;171:388-416. Session Review • • • • • • • • • PIAS-KT overview Local Opinion Leaders UTIs/Pneumonia are highly prevalent and impactful Pharmaceutical care of patients with infections naturally includes antimicrobial stewardship activities UTI/Pneumonia KPIs are antimicrobial stewardship activities When to initiate antibiotics for UTI/Pneumonia What antibiotic to initiate for UTI/Pneumonia When and how to de-escalate antibiotics for UTI/Pneumonia How long to treat with antibiotics for UTI/Pneumonia Attendance • Please email Brenda Flood ([email protected]) if you attended this session • Please email Brenda Flood ([email protected]) if you view this presentation online at a later date Questions? TMP/SMX Resistance Clinical Cure Uncomplicated Cystitis Ann Intern Med 2001:135:41-50