* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Selling Genzyme Genetics` Maternal Serum Screening Program
Survey
Document related concepts
Behavioural genetics wikipedia , lookup
Population genetics wikipedia , lookup
Designer baby wikipedia , lookup
Comparative genomic hybridization wikipedia , lookup
Human genetic variation wikipedia , lookup
Genetic engineering wikipedia , lookup
Genealogical DNA test wikipedia , lookup
Microevolution wikipedia , lookup
History of genetic engineering wikipedia , lookup
DNA paternity testing wikipedia , lookup
Genome (book) wikipedia , lookup
Down syndrome wikipedia , lookup
Medical genetics wikipedia , lookup
Public health genomics wikipedia , lookup
Genetic testing wikipedia , lookup
Birth defect wikipedia , lookup
Nutriepigenomics wikipedia , lookup
Transcript
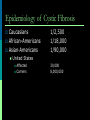
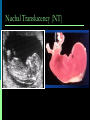
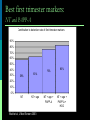
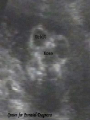
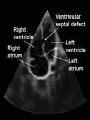
Recommendations for Testing for Fetal Abnormalities Lee P. Shulman MD Northwestern Memorial Hospital Distinguished Physician and Professor and Chief Division of Reproductive Genetics Department of Obstetrics and Gynecology Feinberg School of Medicine, Northwestern University Objectives Describe the major ethical issues surrounding genetic testing for fetal abnormalities. Discuss how health care providers can improve the genetics literacy of their patients to enhance their understanding of the benefits, risks, and limitations of genetic screening and testing for fetal abnormalities. Identify when and how to refer patients seeking genetic testing for fetal abnormalities. Screening is the testing of apparently well persons to identify those who might be at increased risk of having a disease. Diagnosis is the testing of an individual to determine whether or not he a a particular disease or condition. Increased Risk for Detectable Fetal Abnormalities Advanced maternal age (> 35 years-old at estimated date of delivery Family history of detectable Mendelian disorder Parental chromosome rearrangement or aneuploidy Exposure to specific chemical or radiation agents Certain ultrasound findings Positive maternal or genetic screening outcomes Role of Genetic Counseling: Prior to Testing Detailed review of family & medical history Comprehensive pedigree analysis Genetic risk assessment & interpretation Genetic testing options, including risks, benefits & limitations Provide educational materials Facilitate patient informed consent Chorionic Villus Sampling Amniocentesis Efficacy and Safety: CVS and Amniocentesis Similar efficacy Confined placental mosaicism with CVS Cytogenetic success over 99% Similar safety More losses after CVS because it is performed at an earlier gestational age Increased risk of loss with both procedures is approximately 0.5% over baseline Screening Practices Second trimester 15.0 – 20.9 weeks AFP (NTD), hCG, uE3, inhibin A NTD, Down syndrome, trisomy 18 First trimester 10.3 – 13.8 weeks hCG, PAPP-A, Nuchal translucency Down syndrome, trisomy 18 Integrated Screening Combines first and second trimester in a sequential, unified fashion Cannot separate the two components Most effective approach to Down syndrome, trisomy 18 detection Allows for NTD detection Applications - AFP Neural Tube Defects Down Syndrome Trisomy 18 Second Trimester Screening – Fetal Chromosome Abnormalities AFP b – hCG uE3 60% detection rate for Down syndrome, trisomy 18 Inhibin A Detection rate may increase to 80% The highlights of first trimester screening Provides an early answer Requires access to sonographers trained in NT measurement Requires access to CVS Does not provide a risk assessment for ONTD Nuchal Translucency (NT) Nuchal translucency (NT) A critical component What is it? Measurement of the fluid that collects behind the fetus’ neck Measured by ultrasound between 10 and 14 weeks’ gestation Size of fetus is 45 to 84 mm Why is it important? Indication of fetal distress/abnormalities Trisomy 21, Trisomy 18, heart defects More fluid indicates a greater the risk of an abnormality • 10% of fetuses with NT of 3mm have major abnormalities • 90% of fetuses with NT of 6mm have major abnormalities Nicolaides et al The 11-14-week scan 1999 Best first trimester markers: NT and PAPP-A Contribution to detection rate of first trimester markers 90% 80% 70% 60% 50% 40% 30% 76% 58% 63% NT NT + age 83% 20% 10% 0% Wald et al, J Med Screen 2003 NT + age + PAPP-A NT + age + PAPP-A + HCG Screening for Trisomy 21 Sensitivity Procedures needed to detect one case 30% (Age) 100 60% (BC) 55 80% (NT) 40 90% (NT+BC) 35 Ultrasound as a Screening Tool Improved ability to detect an increasing number of fetal anomalies Able to reliably detect fetal anomalies in the first trimester 3-D/4-D Increased ability to provide meaningful information to women and couples Limitations of Ultrasound as a Screening Tool Highly Subjective Operator experience Machine Training Quality Assurance Difficult to Assess Ability to Provide Accurate Diagnosis False Positive False Negative Anomalies Detectable by Ultrasound Craniospinal: (anencephaly; spina bifida; encephalocele; hydrocephalus) G.I.T: (omphalocele; gastroschisis; diaph hernia; duod atresia; colonic obstruction) Urinary tract anomalies: (obstructive uropathy; polycystic kidney; renal agenesis; renal cysts) Limb Deformities (limb reduction; skeletal dysplasia; limb-body wall defect). Cardiac anomalies (ASD; VSD; hypoplastic anomalies; aortic arch; mitral atresia; cardiomyopthy) Fetal tumors: (cystic hygroma; teratoma; neuroblastoma) Ethnicity and Genetic Disease Ethnic/Racial Group Disorder Acadian Tay-Sachs Screening Test African-Americans sickle cell disease presence of sickle cell hemoglobin (sickledex); confirmatory hemoglobin electrophoresis Ashkenazi Jews Tay-Sachs DNA molecular analysis serum hexosaminidase-A DNA molecular analysis DNA molecular analysis Canavan Familial dysautonomia DNA molecular analysis serum hexosaminidase-A Mediterranean people b-thalassemia mean corpuscular volume (MCV) less than 80% from CBC; confirmatory hemoglobin electrophoresis Southeast Asian and Chinese ethnic groups a-thalassemia mean corpuscular volume (MCV) less than 80% from CBC; DNA analysis All ethnic groups cystic fibrosis DNA molecular analysis - should be offered to Caucasians and Ashkenazi Jews, made available to all other groups Epidemiology of Cystic Fibrosis Caucasians African-Americans Asian-Americans 1/2,500 1/18,000 1/90,000 United States Affected Carriers 30,000 8,000,000 CYSTIC FIBROSIS GENE Located 250,000 27 on 7q bp (250kb) exons cDNA Cystic 6,100 bp fibrosis transmembrane regulator; 1,480 amino acids Population Carrier Screening by Ethnic Group Ethnic Background Published Range of Carrier Risk Test Detection* Caucasian 1/25 - 1/29 78-90% Ashkenazi Jewish 1/25 - 1/29 95-97% 1/46 58-85% Hispanic African 1/65 American Asian 1/90 American *varies by laboratory 60-80% 33-38% OFFERED Physician or other health care worker initiates the counseling about CF screening May be supplemented by written materials, videotape, CD, or other modalities Similar to second trimester Maternal Serum Screening RECOMMENDATIONS FOR MAKING CF SCREENING AVAILABLE Low Risk Groups African-Americans Hispanics Asian-Americans No known admixture with higher risk groups MAKE AVAILABLE Written material should be provided to lower risk racial or ethnic group(s) Risk for having a child with CF Sensitivity of CF screening When requested, additional information or counseling should be provided If desired, CF screening should be provided CONCLUSIONS 3 generation family history Disorders, ethnicity, race Counseling Current when appropriate Standards Sickle cell disease, a- and bthalassemia, Jewish genetic disorders including Tay Sachs, Canavan, familial dysautonomia and CF